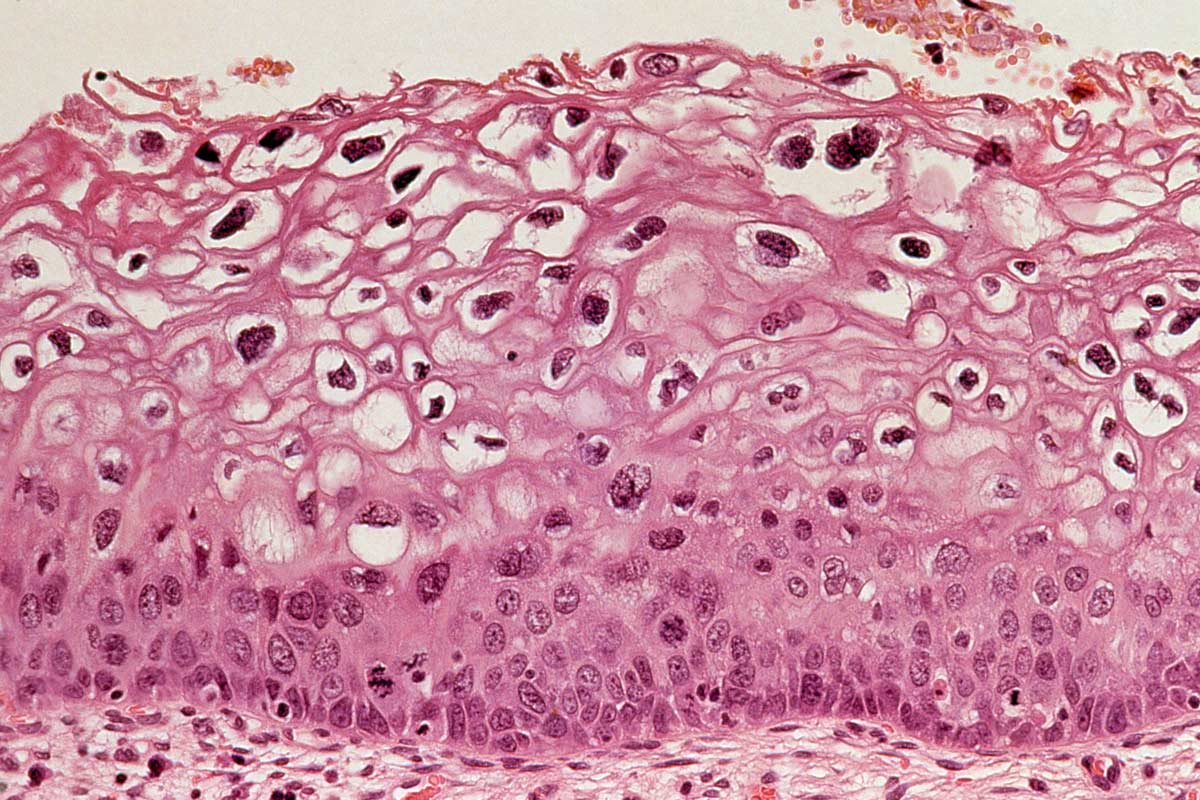
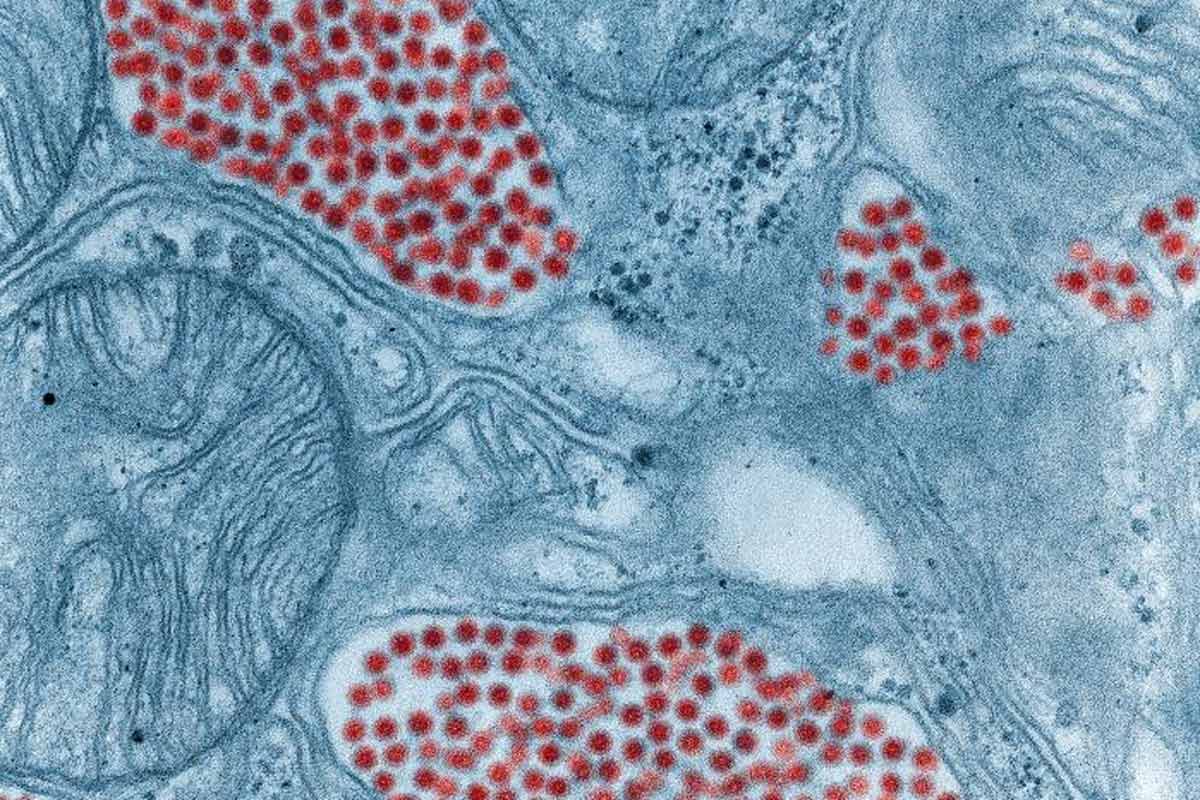
Value of vaccination
In this special series, we show how vaccines save millions of lives a year, allow children to grow and develop, and stop millions more falling into poverty through unaffordable healthcare costs.
- 7 December 2021
- 1 min read
- by Priya Joi
Value of vaccination