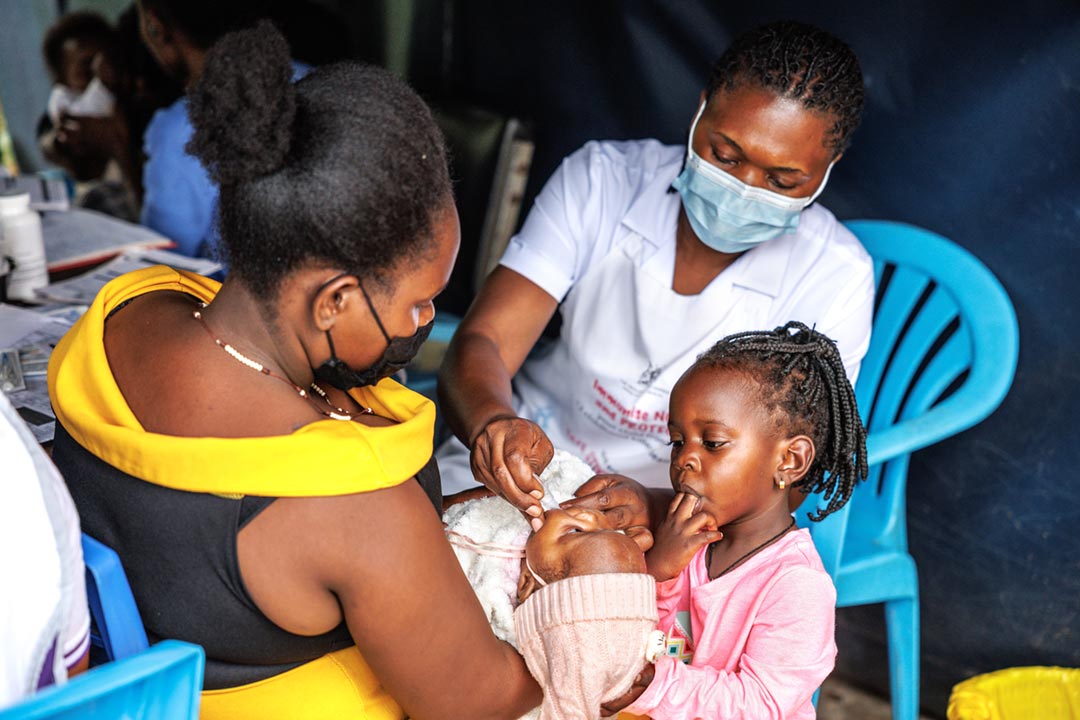
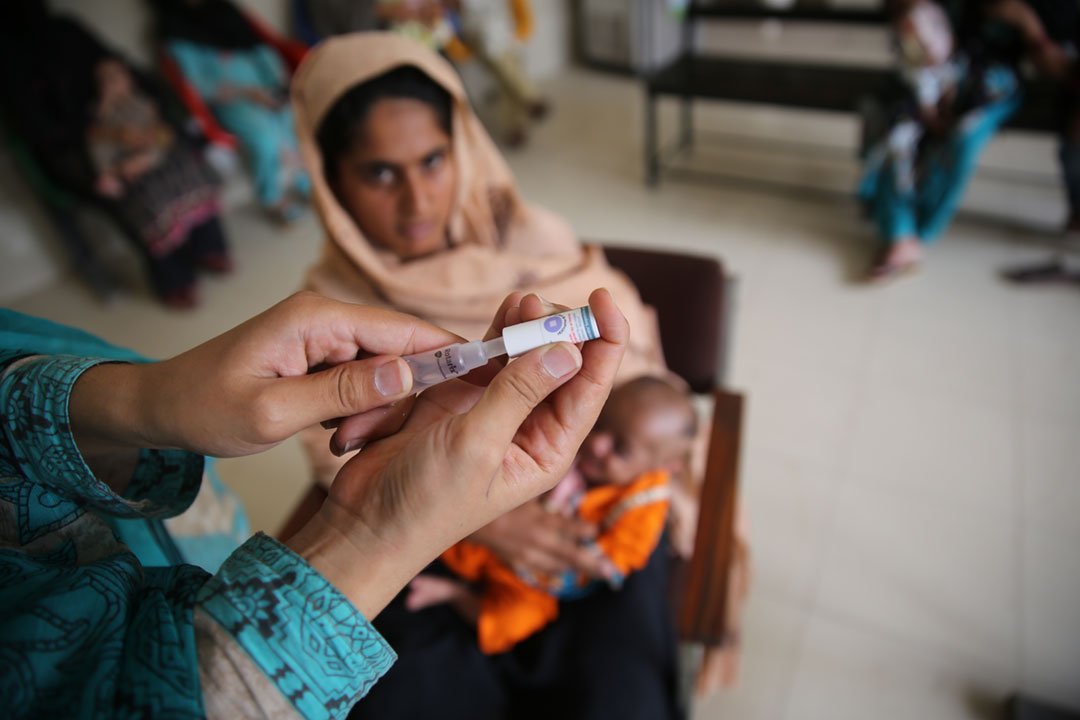
Preventing the next pandemic is vastly cheaper than reacting to it: Study
Humanity's response to pandemics to date is similar to our climate change response: mitigation rather than prevention. A new study says prevention could save trillions of dollars and millions of lives.
- 8 February 2022
- 10 min read
- by Mongabay

- A new study emphasizes the need to stop pandemics before they start, stepping beyond the quest for new vaccines and treatments for zoonotic diseases to also aggressively fund interventions that prevent them from happening in the first place.
- Researchers estimated that based on Earth’s current population and on past pandemics, we can expect 3.3 million deaths from zoonotic diseases each year in future. COVID-19 pushed numbers in 2020-21 even higher. These outbreaks are now happening more frequently, and their cost is calculated in trillions of dollars.
- Addressing the main drivers — deforestation, the wildlife trade and burgeoning agriculture, especially in the tropics — could prevent future pandemics, save lives and catastrophic societal disruptions.
As the novel COVID-19 coronavirus swept the planet in early 2020, researchers scrambled to find effective treatments and vaccines. Within a year, there was a clarion call from heads of state, the World Health Organization (WHO) and other agencies to create an international “pandemic preparedness and response” treaty. WHO noted that COVID-19 offered “a stark and painful reminder that nobody is safe until everyone is safe” from zoonotic disease outbreaks.
While these actions are extremely important, a new study in the journal Science Advances emphasizes the critical, largely overlooked need to prevent disease outbreaks before they occur. The average yearly cost in human lives and lost productivity can be in the trillions. These researchers show, in hard numbers, that boosting surveillance and curbing high risk human activities, such as the destruction of tropical forests, will save many lives and vast sums of money.
“We are grossly underestimating the economic harms [of pandemics], and prevention is far cheaper than a cure,” says lead author Aaron Bernstein, a pediatrician at Boston Children’s Hospital and a researcher at Harvard University’s Center for Climate, Health and the Global Environment.
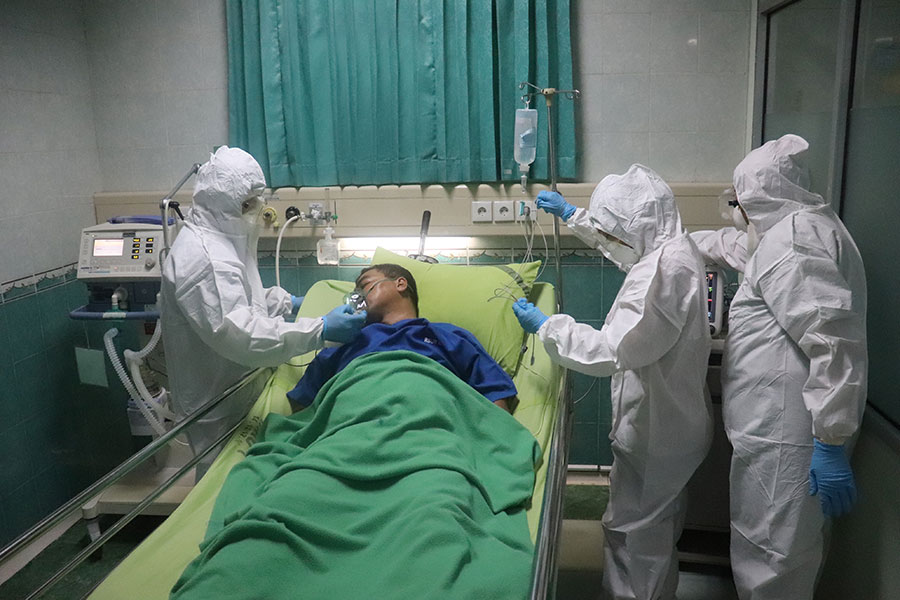
Image by Mufid Majnun at Unsplash.
In this new analysis, an esteemed cadre of doctors, epidemiologists, economists, ecologists, and conservation biologists point out that the current pandemic fight rests squarely on “post-spillover actions.” It’s a reactive approach, with action only after a pathogen has jumped from wild animals, infecting humans with a newly emerged zoonotic disease. COVID-19 is believed to have resulted from a spillover event, as did HIV, Ebola, SARS, avian flu and others — each with astronomical societal costs. But preemptive efforts, Bernstein and his coauthors warn, are severely underfunded, putting the world at grave risk.
Major health initiatives consistently overlook humanity’s key role in aiding pathogens in their quest for new hosts — specifically by razing forests; by enormously expanding agribusiness, especially in the tropics; and by a massive, poorly regulated global trade in wildlife.
“Our alterations to the ecosystem and the environment are what’s causing these outbreaks,” says Colin Chapman, a conservation scientist at George Washington University and public policy fellow at the Wilson Center. COVID-19 wasn’t a surprise, he says. “We knew the pandemic was coming. But we didn’t have the will to do something to slow down the chances of an emergence.”
Have you read?
The new study delves deeply into the economic costs of human deaths and lost productivity. It examines the increasing frequency of major epidemics over the last century and calculates how much it would cost to lower future risks. Protecting forests, wildlife, and limiting contact between wild animals, humans and livestock in regions of concern “could save us innumerable human lives and trillions of dollars, but it also goes hand in hand with fighting climate change and preventing mass extinction,” says Les Kaufman, a conservation biologist at Boston University.
This groundbreaking research answers key questions for humanity, including, “How much should we be spending to prevent disease emergence and reduce pandemic risk,” says Bernstein. “And what are the best things we can do right now?”
The exorbitant human cost of global pandemics
The new analysis contains “disconcerting messages that create a sense of urgency,” says Andrew Dobson, an ecologist who works on wildlife diseases at Princeton University. “Epidemics are happening more often, getting larger and spreading further.”
Up to 75% of all new infectious human diseases are zoonotic. There may be more than 1.6 million unknown viruses in circulation, mostly in the tropics, says zoologist Peter Daszak, president of the nonprofit EcoHealth Alliance.
In a globalized world, spread is rapid. Covid-19’s Omicron variant revealed just how quickly a virus can infect the globe. First detected in South Africa, it traveled across continents in a matter of weeks.
The deaths and economic hardships have been enormous. To calculate the expected number of lives lost each year to viral disease epidemics, economists tallied the human cost of every novel zoonotic virus that has killed 10 or more people since the 1918 influenza pandemic. Based on the Earth’s current population of nearly 8 billion people, they estimate that we can expect about 3.3 million deaths per year from zoonotic epidemics.
But that figure is an average which discounts the surge in deaths from a large global event like the 1918 flu or the current pandemic. The official death toll from COVID-19 has now climbed to more than 5.7 million lives lost over two years, though experts say the true number may be up to four times that. While ongoing mortality from influenza, HIV, Ebola, Zika and other viruses, and total zoonotic disease deaths in 2020 and 2021 surpass the 3.3 million yearly estimate.
“This is a mortality rate that is cataclysmic,” said Duke University conservation scientist Stuart Pimm.

Image by Ehimetalor Akhere Unuabona on Unsplash.
Estimating the economic value of human lives is controversial. As abhorrent as the concept may be, the value varies according to the wealth of the country someone lives in, explains Bernstein. For example, a U.S. life is valued at $10 million by the U.S. Environmental Protection Agency. In 2018, the so-called “value of a statistical life” of a blue-collar male worker in India was $598,116.75; a recent estimate valued a life lost in the Central African Republic at $1,931.
Taking this disparity into account, the team’s economists found that 3.3 million deaths from zoonotic diseases translates to between $350 billion and $21 trillion in yearly economic loss. Preventing just 10% of those deaths could be worth up to $2 trillion.
Estimates of yearly pandemic-caused losses to world gross national income added another $212 billion. These calculations omitted economic loss from unemployment and closed businesses, ongoing medical costs from deferred healthcare, treatment for long COVID, wildlife diseases that infect livestock, and more. Dobson notes that the true cost to the global economy from the current pandemic won’t be clear for at least a decade. To date, estimates range from 15 to 50 trillion dollars.

Photo by roya ann miller on Unsplash
“Primary prevention”
The major pandemic risk factors have been known for decades: deforestation, expanding agriculture and the wildlife trade, all exacerbated by growing human populations and global interconnectivity. “Everything we do that increases contact between wild animals and humans increases the probability we’ll get a spillover event,” says Dobson.
Destroying species-rich tropical forests for mining, agriculture, ranching and other development is of particular concern. Incursions into wild areas brings people, their domestic animals and wildlife — along with the unique, deadly pathogens they may carry — into unnatural proximity, inviting spillover.
But despite this knowledge, funding for prevention of zoonotic disease has been low. “Our investments in these areas pale in comparison to the harms that emergence is causing,” Bernstein says.
The good news, Pimm notes, is that “with relatively inexpensive measures, we can greatly reduce the odds of having another event like this. Prevention is a lot cheaper than a cure.”
Keeping forests intact is key. The researchers estimate that about 2,100 square miles of tropical forest is cut yearly in hotspots of emerging infectious diseases. This brings people into contact with bats, primates, rodents and other wild species known to harbor numerous viruses. Chapman’s research on red colobus, vervet and other monkey species in Kibale National Park in Uganda, for example, discovered 50 previously unknown viruses.

Image by Colin Chapman.
However, it would only cost between $1.5 billion and $9.6 billion a year to reduce deforestation by half in these high-risk areas, according to Jonah Busch, an economist with Conservation International.
Much of these tropical forestlands are felled for agriculture, particularly for soy and palm oil, or for ranching. Bringing pigs, chickens and other domestic animals into contact with wildlife makes them possible intermediary hosts. Pig farms that were built adjacent to forests in Malaysia facilitated transmission of the deadly Nipah virus, which passed from bats to pigs to humans. Poultry has contracted and transmitted avian flu to people.
The new study estimated a price tag of $476 million to $852 million to prevent spillover from wildlife to livestock.
Hunting, eating and trading wildlife also poses a huge disease risk. Both HIV and Ebola, for example, are believed to have originated in primates. “If we butcher chimpanzees, our nearest relatives, it’s not surprising that we contract nasty diseases,” says Pimm.

The ongoing HIV/AIDS pandemic alone offers a tragic example of how much prevention is worth. There is still no cure for HIV, which has plagued humanity since 1980 and killed some 10.7 million people.
Both the legal and illegal wildlife trade offer innumerable opportunities for disease emergence. Caging wild species together, selling them in markets, and shipping them across the globe for food or as exotic pets creates a virtual petri dish for pathogens to mutate and jump the species divide to infect people. The legal wildlife trade dwarfs the $23 billion black market trade, and wildlife farms, particularly in China, also pose serious risk. Mink on farms in both the EU and U.S. have been infected with the COVID-19 coronavirus.
This study estimated that wildlife trade surveillance would cost between $250 million and $750 million annually. Shutting down China’s wildlife farming industry was the highest single cost for primary prevention, at $19 billion.
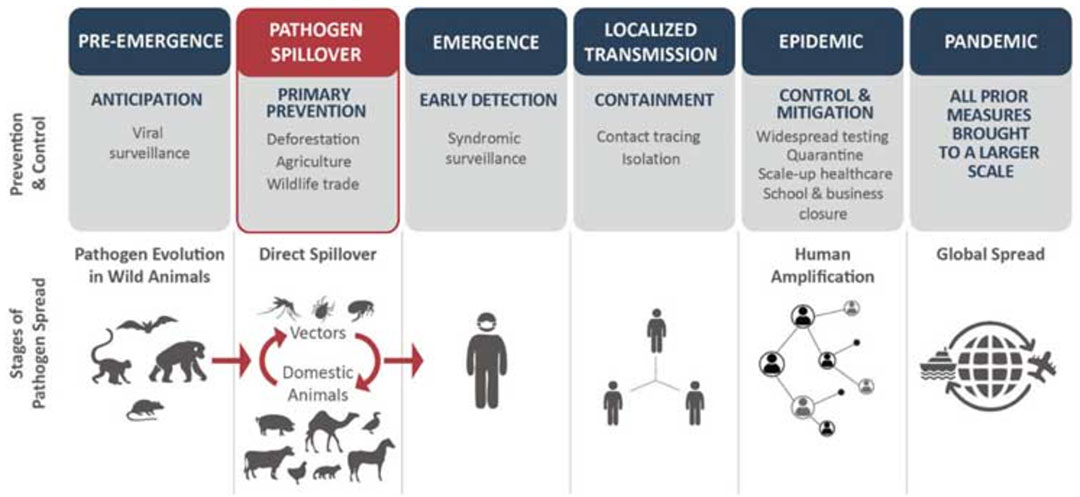
Image courtesy of Aaron S. Bernstein et al.
Viral discovery and surveillance
Viral discovery is the cornerstone of this suite of preventive interventions. Amassing a database of viruses carried by mammals and birds, as well as their genetic makeup and hosts, could one day help researchers predict which viruses are most likely to infect people. But in the near term, such a database could help focus prevention activities: Which forests should remain untouched because the public health risks of cutting them down and bringing humans into these areas are too high? Which animals should not be traded or eaten?
New epidemics will invariably emerge. This viral library would provide a leg up when that occurs, accelerating development of tests and vaccines. Researchers estimate the cost of gathering data and building this library at $120 million to $340 million annually.
The final key piece in this suite of prevention measures is surveillance and early detection, at a cost of $217 million to $279 million. Improving healthcare for underserved communities that border tropical forests would help detect infectious disease outbreaks and curtail them before they can spread. One example of a successful program is a mobile clinic that now provides free medical care to people who neighbor Kibale National Park.

Image by Laura Gil Martinez/IAEA via Flickr (CC BY-NC-ND 2.0).
The new paper also emphasizes the need to monitor wildlife health. That means deploying more field veterinarians and wildlife disease biologists to global hotspots. Veterinarians are the frontline troops in the battle against emerging pathogens, Kaufman says.
Although these interventions may sound costly, if they proved to be just 1% effective in preventing substantial disease outbreaks, they would pay for themselves in lives saved and economic productivity.
But instituting and funding them will require political will and commitments from the wealthiest nations, NGOs and international organizations — along with broad, interdisciplinary collaboration. “A tiny proportion of the Pentagon budget would allow us to stop most new future outbreaks,” says Dobson. That would mean rethinking potential global disease outbreaks not as remote possibilities but as a looming, inevitable national and international security risk.
Human behavior tends to be reactive rather than proactive. But Bernstein believes that “it would be a great victory if we could start understanding that investments in conservation and health systems that focus on spillover risk are investments in pandemic prevention.”
“I think this work makes it abundantly clear that the wisest dollar spent on pandemics is the one dollar spent to make sure they never start in the first place,” he said.