A 4-point checklist for assessing countries' vaccine readiness
As the new COVID-19 vaccines begin to ship out, how ready are health systems to manage delivery? Here are four ways countries should frame that question.
- 15 December 2020
- 6 min read
- by World Economic Forum
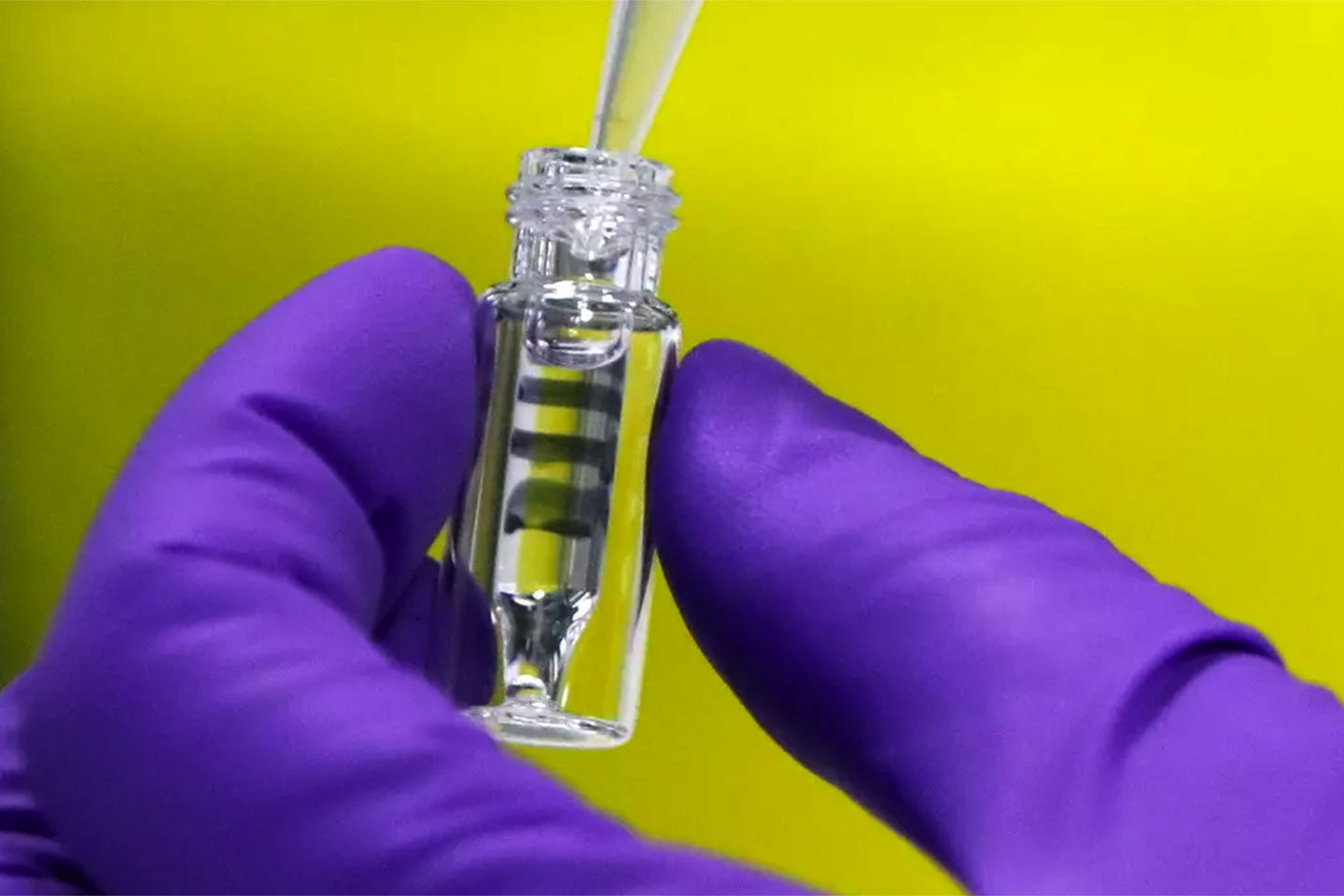
- As the new COVID-19 vaccines begin to ship out, the focus now turns to the readiness of countries' health systems to begin the roll-out.
- Any weakness in countries' ability to store, deliver or prioritize the vaccines must be dealt with now - especially in LMICs.
- Here are four lenses through which countries can assess their preparedness and identify potential problems.
As the world finds itself swinging in and out of lockdowns and restrictions, news of the arrival of three COVID-19 vaccines in quick succession has created a sense of optimism in the fight against the pandemic. However, from a global health perspective, the efforts against COVID-19 have only just shifted into a new gear.
Even before the vaccines begin to arrive in ports around the world, the focus will shift to the preparedness of in-country logistics, especially in low and middle-income countries (LMICs) and to their health systems' ability to deploy and administer the vaccine to their populations. Any weaknesses in health system readiness – in vaccine distribution, storage, refrigeration, prioritization or delivery – will need to be quickly assessed, addressed and resolved at unprecedented speed before any effective immunization campaign can begin.
Here's how countries, and especially LMICs, can assess their readiness along four key dimensions: awareness, acceptance, accessibility and availability.
Have you read?
1. Awareness
Clear, consistent, evidence-based information from trusted authorities is a critical component of creating the appropriate sense of urgency and necessary action (rather than panic). However, in many countries the risk of an 'infodemic' accompanying the pandemic is real. How governments choose to leverage collective communication assets will be critical in a health system response, especially for an immunization campaign. Public health communication campaigns sponsored by the government and leveraging prominent celebrities and personalities were shown to have had a profound impact on India’s polio eradication, particularly in shaping behavior-driven outcomes.
Beyond campaigns themselves, public health authorities must leverage and collaborate, leveraging health information systems, to share knowledge of disease progression, response, critical workflows and redressal, and to analyze and assess facts to combat misinformation up and down the healthcare chain. This remains a major challenge in the context of increasingly divisive and polarized politics, even in some major economies where the COVID-19 disease burden remains high.
2. Acceptance
A study of 149 countries published in The Lancet found an increase in aspects of vaccine hesitancy between 2015-19 in parts of South and South-East Asia, West Africa and Eastern Europe, while remaining a matter of concern in North America and in Western European countries such as France. As the response to the 2014-15 West Africa Ebola outbreak showed, it is essential for health systems to engage local communities in dialogue to accommodate their concerns and to to counter community-level misinformation that inhibits vaccine acceptance. In countries already battling deep-rooted taboos linked to healthcare, acceptance of a new vaccine can be even more challenging. Furthermore, disadvantaged groups suffering from information asymmetry are particularly vulnerable to misinformation campaigns, and even the more digitally privileged population groups are not entirely immune from global social media campaigns that attempt to increase vaccine hesitancy. A recent article in Nature highlights the vast differences that continue to exist in terms of potential acceptance of a COVID-19 vaccine, with China reporting 90% acceptance and Russia, at the lower end, with less than 55%. These differences will impede the process of COVID-19 immunization efforts and an eventual return to normalcy.
3. Accessibility
It is likely that during the initial stages of a COVID-19 immunization drive, sufficient vaccine doses will not be available immediately to cover the entire population.
Regardless, given the global urgency to contain the pandemic, one can imagine that an immunization drive requiring large proportions of populations to be covered would necessarily require mobilizing resources on an unprecedented scale. Target groups, as illustrated in the diagram below, in the context of India’s potential response, would have to be prioritized in a way that would provide the biggest impact in halting the progress of the pandemic in the shortest amount of time with limited resources.

Image: IQVIA
Furthermore, last-mile challenges will remain, and finding the 'missing and most vulnerable millions' will be key for COVID-19 campaigns in LMICs. Outreach approaches spearheaded by community health, leveraging technology and electronic immunization records, and scaling up connectivity and infrastructure could fill coverage and recipient follow-up gaps quickly. The ability to integrate digital vaccination certificates with a national beneficiary identification system would further prevent the duplication or loss of prioritized beneficiaries.
4. Availability
Vaccine characteristics such as shelf life, required dosage and storage specifications will be critical for planning efficient vaccine supply-chain processes. These include technologies that can effectively track and trace inventories, preventing loss or pilferage from the system, thereby protecting public, donor and manufacturer trust. An impending COVID-19 immunization effort is a perfect time to upgrade or create a vaccine intelligence infrastructure to ensure real-time information on stock and temperature controls across cold chain points, and to assess and expand surge capacity as needed.
From a logistical standpoint, one of the biggest challenges to COVID-19 vaccine availability is likely to be the cold supply chain. Vaccines such as those being developed by Pfizer or Moderna – that require ultra-low temperature storage at -70°C and -20°C respectively – are likely to require a different state of cold-chain readiness and investment than ones that can be stored at normal refrigeration temperatures, such as the vaccines being developed by Johnson & Johnson, AstraZeneca and Sanofi-GSK, that can be kept and shipped in an unfrozen state. Thus, any failure in cold chain integrity, especially in LMICs with weaker health systems, could be disastrous leading to a significant wastage of valuable vaccines.
Conclusion
Finally, normalcy itself will be a function of how successfully health systems are able partner for the COVID-19 immunization effort. Partnerships with the private sector, donors, technical partners, and with other sectors (such as agriculture, in the case of cold chains), will be key to success. What LMIC health systems choose to do in the next 3-6 months will be critical for any return to a post-COVID-19 normalcy.
Partner content
This article was first published by the World Economic Forum on 14 December 2020
Authors
Pratik Bhatnagar
Director, Global Public Health, IQVIA
Karan Sagar
Head, Health System and Immunisation Strengthening, GAVI
Lokesh Sharma
Senior Principal & Practice Leader - Public Health, AMESA, IQVIA
Nilesh Maheshwari
Principal and Head, Public Health, South Asia, IQVIA
Deepak Batra
Head - Public Health and Government Solutions, Middle East and Africa, IQVIA
Anurag Saxena
Head of Digital Health, IQVIA Public Health, IQVIA
Vidhi Gupta
Consultant – Public Health, IQVIA
Shyanne Dewan
Public Health and Government Consultant, IQVIA
More from World Economic Forum
Recommended for you









