Community health workers as vaccinators: A pathway to achieving global immunisation goals
A shortage of health workers has made the roll-out of COVID-19 vaccines in many lower-income countries a major challenge. In Malawi, community health workers are helping to fill the gap.
- 6 October 2022
- 4 min read
- by Tafwirapo Chihana , Rebecca Alban
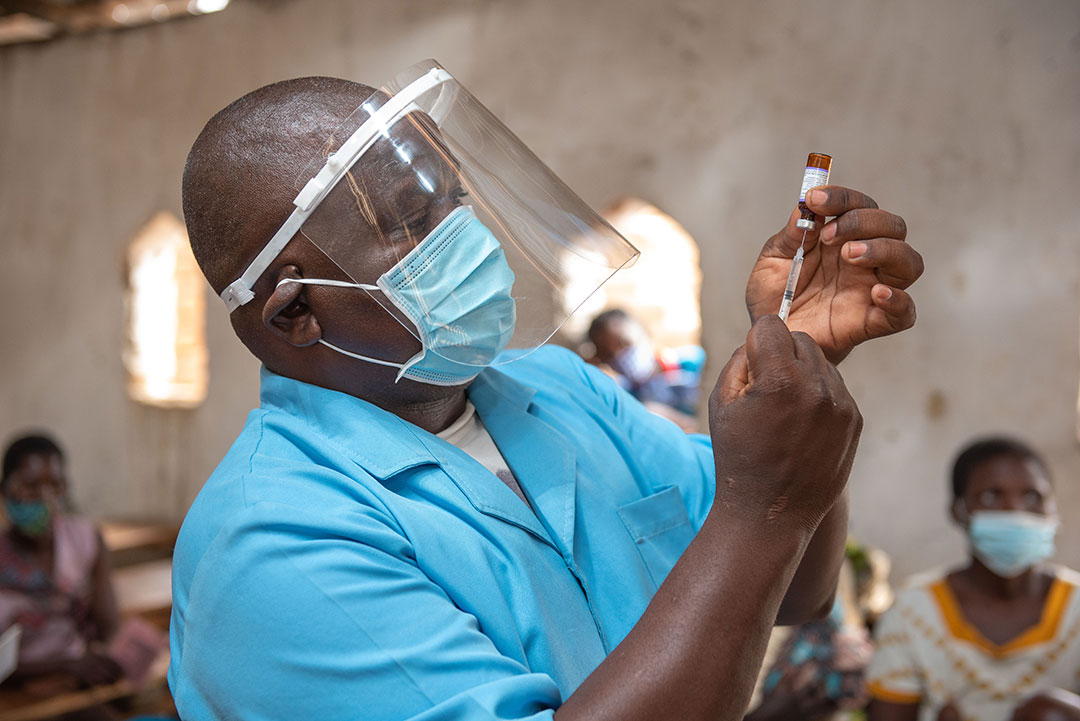
The roll-out of the COVID-19 vaccine has encountered issues with equitable access and vaccine hesitancy globally. In many low- and middle-income countries (LMICs) these challenges are compounded by severe health worker shortages that further hinder achieving the WHO COVID-19 vaccination targets.
However, in Malawi the primary cadre of community health workers (CHWs), known as Health Surveillance Assistants (HSAs), have been meeting these challenges head-on for decades.
"I bring their memories back telling them about the vaccines people had before. They had chicken pox, people got the vaccine for it and the disease disappeared. Vaccines are not a new thing; they came a long time ago. We are living in a world that needs vaccines so once we [get vaccinated], we will be protected.”
HSAs have been administering routine vaccinations since the 1950s, and were formally included in the Malawi national health system in 1998. In fact, Malawi is one of only 20 countries that deploy CHWs to administer vaccines. Therefore, when COVID-19 vaccines came to Malawi, the government quickly organised training for HSAs so they could better serve their communities, not just through COVID-19 outreach and education, but also through COVID-19 vaccine administration.
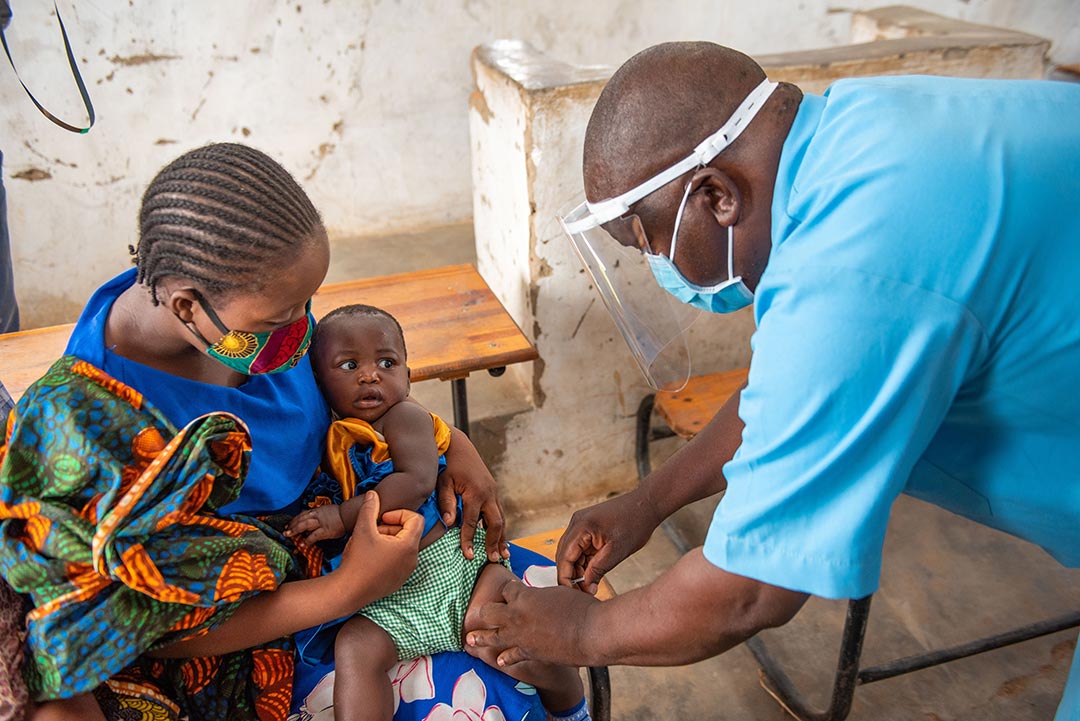
Credit: Homeline Media
A Trusted Source
CHWs have different roles in each country, but in Africa (where VillageReach works) they are often people’s only touch points with the health system (particularly in remote areas). In fact, CHWs serve nearly 400 million people in Africa, and have trusted relationships with community members. CHWs in Africa are also already involved in most public health vaccination campaigns through education and outreach. The only thing they do not do in many countries is administer vaccines.
While HSAs in Malawi were accustomed to administering routine immunisations, the arrival of COVID-19 vaccines meant they now had to reach a large number of adults during a time of increased vaccine hesitancy. One HSA, interviewed by VillageReach as part of qualitative research (with HSAs, HSA supervisors, community members and government officials) explained that vaccine hesitancy for COVID-19 was much higher than for other routine vaccines, but HSAs played a key role in changing community perspectives about the vaccine: “I bring their memories back telling them about the vaccines people had before. They had chicken pox, people got the vaccine for it and the disease disappeared. Vaccines are not a new thing; they came a long time ago. We are living in a world that needs vaccines so once we [get vaccinated], we will be protected.”
Because of this trust, HSAs were able to educate communities and reach more people in remote areas by administering COVID-19 vaccines at both fixed locations and in people’s homes. One HSA noted, “...another person goes [to communities] with the vaccine, people will not receive it but if it is [a] HSA, [communities] say our doctor has arrived.”

Credit: Homeline Media
Have you read?
Increasing Immunisation
The potential for deploying CHWs as vaccinators could both increase COVID-19 vaccination in LMICs, as well as address declines in routine vaccination among children. An estimated 25 million children under the age of one did not receive basic vaccines in 2021, and more than 60% of these children live in 10 LMICs. This highlights inequities in access to vaccines, which was exacerbated during the pandemic, making the goals of the Immunization Agenda 2030 feel further out of reach.
In Malawi, HSAs have successfully administered routine vaccinations for decades and the country boasts high immunisation rates. Around 72.6% of children 12-23 months are vaccinated. While HSAs in Malawi noted room for improvement, Malawi demonstrates that when CHWs are embedded in the national health system, trained, supervised and paid they are critical assets to tackling the COVID-19 pandemic and improving community health. One HSA supervisor interviewed said, “... if you want us to achieve universal health coverage, let us use HSAs as much as possible, because they're always there in the community, and they know their communities better.”
Scaling this Model
Given the persistent challenges of equitable access, vaccine hesitancy and health worker shortages, leveraging CHWs as vaccinators is an important opportunity. One government official from the Malawi Ministry of Health said, “(HSAs) can be the best vehicle we have for accelerating immunisation rollout and improving coverage and acceptance of vaccines.”
While Malawi serves as one example of how this can work on a national scale, more research should be done to look at best practices around using CHWs as vaccinators, and how other countries can adopt and adapt this model. With more information and resources to advocate for embedding CHWs into national health systems, the world can better address immunisation challenges and ensure everyone, everywhere has the health care needed to thrive.
Get involved, contact Hope Ngwira, Senior Manager, Advocacy and Communications at VillageReach hope.ngwira@villagereach.org.
Visit the Center for Health Worker Innovation, and the Community Health Impact Coalition to see how you can support CHWs.





