COVID-19 threatens weak health systems in indigenous Amazonian communities
Indigenous groups face unique health challenges. How do we mitigate these risks in our COVID response?
- 21 April 2020
- 4 min read
- by Partnership for Maternal, Newborn and Child Health (PMNCH)

From 2018 to 2019, I worked as a medical doctor in the San José de Guayusa community in the province of Orellana, Ecuador. This region of the Amazon rainforest is well known for its biodiversity, indigenous communities, unique species of animals and plants, and its abundance of natural resources.
However, this stunning environment is blighted by widespread poverty and pervasive social inequalities. Even though they generate a great deal of income for the state and private sector through oil production, local communities face enormous health risks and challenges, exacerbated by low wages, lack of access to water and sanitation, and poor education.
Layered and overlapping barriers to health care services
A major issue is physical access to health services due to geographical factors. For example, some people can only be reached after many hours by river or walking long distances, and in certain cases may be completely cut-off because the roads are too rough or unsafe.
This experience taught me the meaning of privilege and drove me to keep advocating to reduce health inequalities based on the principle of social justice. Historically, indigenous communities in Latin America have been discriminated against and marginalised, left outside social protection services, and denied their right to health. This has translated into high child mortality, maternal mortality, adolescent pregnancy, and other negative health outcomes.
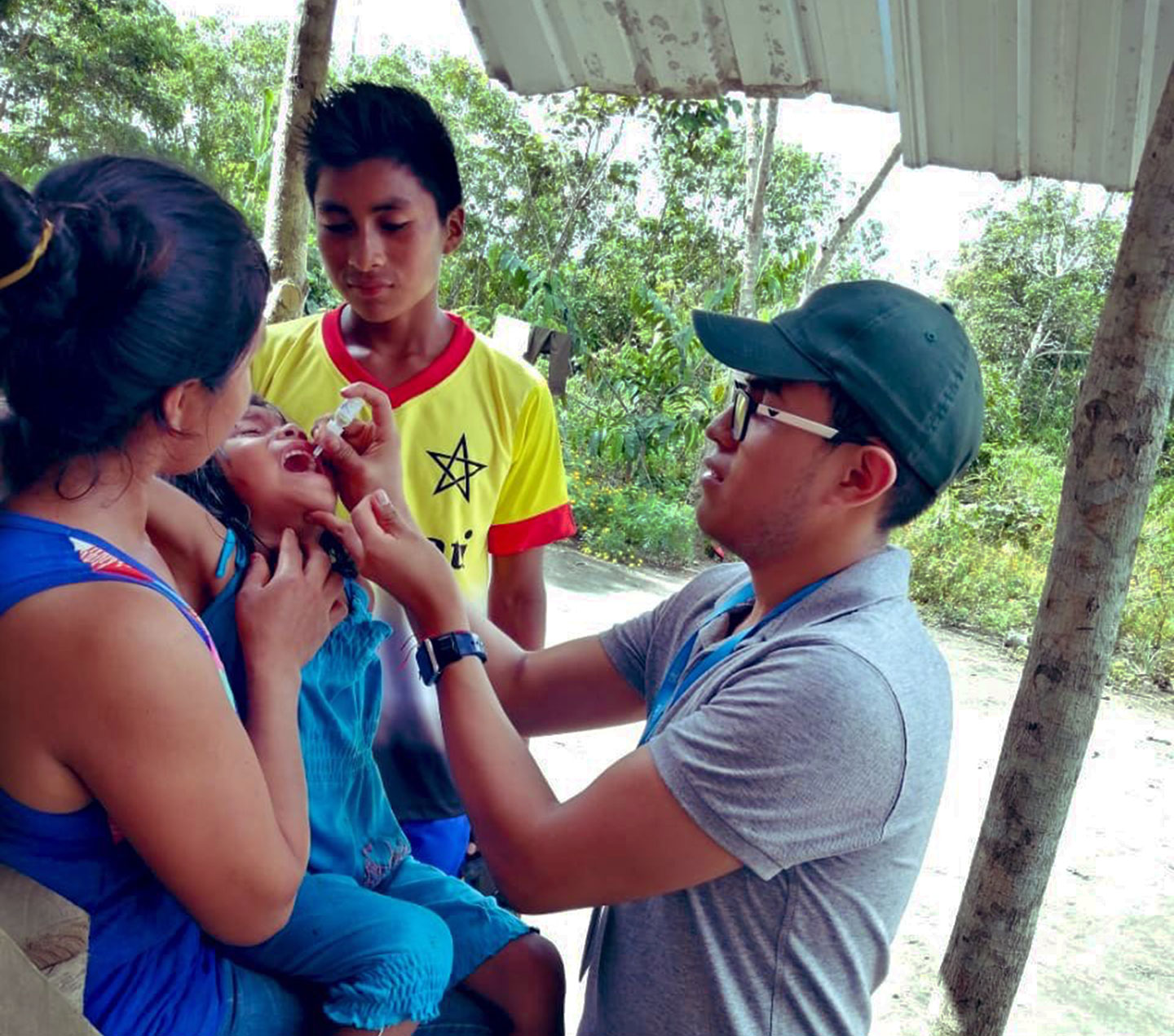
Within this context, I was proud to support a provincial immunisation programme led by nurses at a local health centre. The programme’s success hinged on the support and close collaboration with education officials - school administrators and teachers - to reach all the children and complete their vaccination schedules. It also required us to knock on every single door and visit every school, mapping the location of each child in the community, and ensuring we didn’t leave anyone behind.
It takes more than a village
This ambitious initiative demanded the time and commitment of all health workers, as well as the community. Luckily, we were supported by a member of the community who was also part of the team at the health centre, helping tackle language barriers and building a bridge between the health services and the beneficiaries.
Working with indigenous communities was not an easy task. There are deeply ingrained cultural and traditional obstacles related to health, beliefs that in some cases could be hazardous, including those against the use of vaccines. Local traditional practices advised against seeking medical attention and vaccination. Children were particularly vulnerable in these situations, because they didn’t have a say about their right to access a free and available programme that was developed to protect them from life-threatening, preventable diseases.
I vividly recall the case of a one-year old child who almost died from a severe pneumonia infection, because he did not receive his full schedule of vaccines.
Through it all, the people I worked alongside showed remarkable grit and resolve to get the job done and reach every child. But motivated health workers can only do so much. Overcoming the unique, systemic challenges of healthcare provision in remote communities requires adequate resources and infrastructure including vaccines, drugs, transportation, safety, staff, salaries and institutional support.
Immunisation as a platform for primary healthcare in remote communities
Over the past few years, significant strides have been made to secure political commitment from governments to prioritise Universal Health Coverage. Now is the time for the world to be held accountable and for us to put those resolutions into practice, applying them at the local level and making sure the principles of solidarity, equity, dignity and justice are followed at all levels.
The COVID-19 pandemic is a painful reminder of the importance of strong, resilient health systems. It is absolutely clear that we must invest in immunisation to prevent further outbreaks of other diseases, and protect people’s health. However, marginalised groups, including the indigenous community I worked with in the Amazon, have unique needs and vulnerabilities, and reaching them will require strong collaboration across multiple sectors and significant sustainable funding.
Author
Dr. David Imbago Jácome, Board Member, Partnership for Maternal, Newborn and Child Health (PMNCH) and Vice President, International Youth Health Organization
Website

Visit the PMNCH website