How do you keep pregnant women safe during a pandemic?
Pregnant women can be more exposed to risk during outbreaks. With 200 million pregnant women in the world, is the global pandemic response adequate to protect them, and not just from the coronavirus?
- 21 May 2020
- 5 min read
- by Gavi Staff

During this era of COVID-19, older people and those with underlying health conditions have been considered most at risk of developing severe illness and death. However, there are other exposed populations, including pregnant women, who may also be susceptible to increased medical and social risks, as we have seen with previous disease outbreaks including Zika virus, Lassa fever, Ebola, and other coronaviruses like SARS and MERS. So, as the race to develop COVID-19 vaccines continues, and with approximately 200 million pregnant women in the world, it is imperative that pregnant women are not left behind.
The impact of COVID-19 on pregnant women
In March 2020, despite minimal knowledge about the effect of the new coronavirus on pregnancy, the UK government as a precaution recommended that they self-isolate for 12 weeks. While the aim was to protect them, this default position of placing pregnant women within a similar at-risk category as older people, or those with underlying health conditions, may not in fact do so.
With limited data to either confirm or deny any increased risk, such measures may instead perpetuate a narrative of exclusion. Also, there are different risks for different populations of pregnant women. In the UK, 55% of pregnant women hospitalised with coronavirus were from a black and minority ethnic background (BAME) even though they represent a much smaller proportion of the population. This suggests that COVID-19 has amplified the racial disparities in maternal health within high income countries.
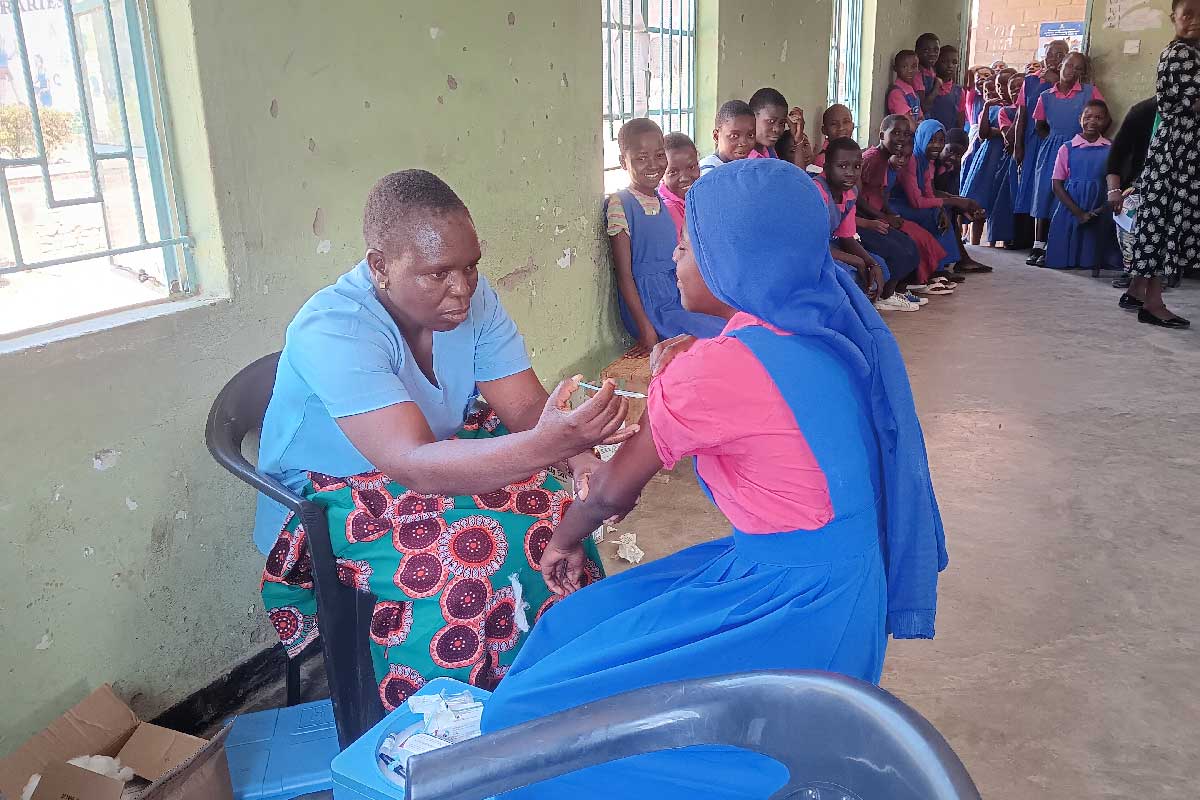
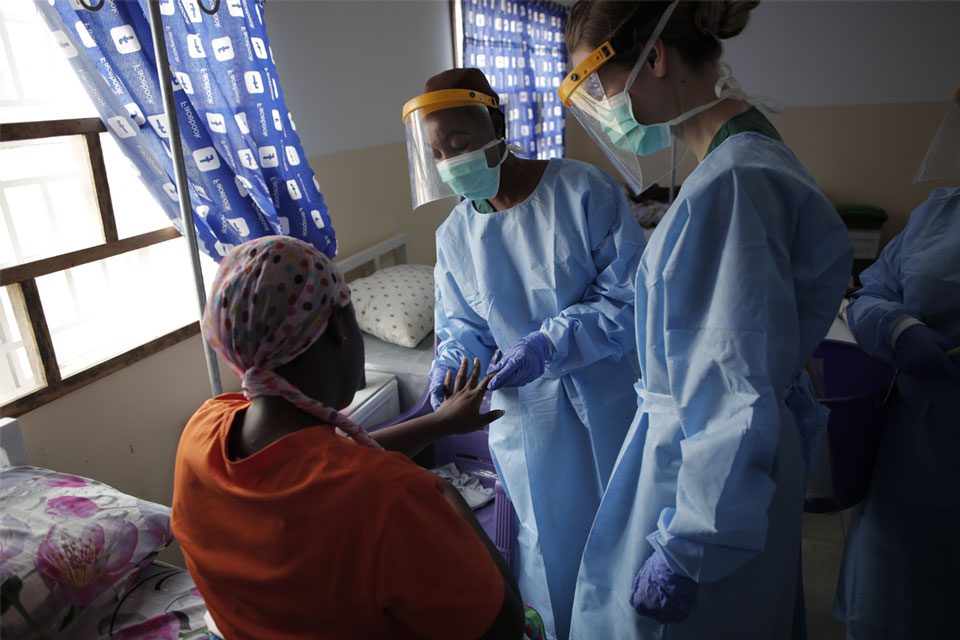
The movement of people has been significantly restricted and health facilities over-burdened, therefore pregnant women may be more at risk when trying to access essential maternal, and ante- and neonatal care. This, combined with economic insecurities and the fear surrounding COVID-19, could inhibit and deter pregnant women from seeking and adopting positive health behaviours, including vaccinations for themselves and their newborns.
Health recommendations for new mothers with COVID-19 have included wearing face masks and washing hands regularly when breastfeeding, which presumes access to basic necessities such as water and sanitation services. Due to global populations being asked to stay at home, the added burden and gendered nature of care work means pregnant women may face added stress and limited time and mobility to access much needed health services. Early modelling has already suggested the tremendous impact this pandemic and its response is having on the utilisation and provision of reproductive, maternal, newborn and child health (RMNCH) services, revealing stark predictions for increases in maternal and early child mortality.
It is also crucial to consider the needs of women who face unwanted pregnancies. As sexual and reproductive health services and resources become harder to access and governments fail to prioritise these services, access could decrease by 10% in low- and middle-income countries, creating 28,000 new maternal deaths. This further translates into a predicted increase of 3 million unsafe abortions and 15 million unwanted pregnancies, simply because 49 million women will be unable to access contraceptives, a fundamental human right.
Furthermore, the ongoing pandemic protection measures and restriction to visitors within hospitals and homes means pregnant women may go through their pregnancies and births alone, increasing vulnerabilities surrounding their mental health. Rather than experiencing support, love and encouragement during an essential healthcare period, pregnant women may instead face loneliness, anxieties and fear, increasing their risk of maternal depression.
This heightened time of COVID-19 and subsequent increased anxieties further reveals the unique mental and psychosocial health effects pregnant women experience. Often the first trimester is a period when some side effects of pregnancy can be the most prevalent, and women often conceal their pregnancy due to the increased risk of miscarriage. This social convention can inadvertently silence and stigmatise miscarriages and pregnant women’s experiences and pain. The pandemic could potentially worsen that experience. This is a time when pregnant women need additional support, and when its absence is compounded by the isolation experienced by the pandemic, there could be detrimental effects on their mental health.
This reflects and is indicative of the wider, holistic evasion of pregnant women’s distinctive needs that are acutely felt now more than ever.
Pregnant women in vaccine research and development
Historically, the needs of pregnant women are rarely considered, represented or researched in biomedical interventions, including the development of vaccines. This has led to pregnant women being denied opportunities to receive vaccines in numerous outbreaks and epidemics that could have protected them. To not consider pregnant women in the development of the COVID-19 vaccine would be more than an oversight, and would ultimately deny their right for equitable health care protection.
To ensure the needs of pregnant women and their children are protected, a generation of evidence is needed by representing them in vaccine research and development (R&D) and vaccine delivery. PREVENT - the pregnancy research ethics for vaccines, epidemics and new technologies - has outlined 22 recommendations to equitably support pregnant women and their babies inclusion within vaccine R&D, naming this proposed change of default, ‘the presumption of inclusion’. Whilst it is noted this undertaking will be more difficult with various ethical, moral and technical complexities, its challenges should not deter but rather inspire the medical research community to include and protect all.
Moving forward
An early preliminary study in China and guidance from the US Centers for Disease Control and Prevention (CDC) suggest pregnant women are not at increased risk of COVID-19. However, with a scarcity of data and parallel studies emphasising pregnant women’s vulnerability to respiratory pathogens, there are gaps in the evidence and in our knowledge.
It is still not known whether viral transmission is possible from mother to baby in the womb, during birth or breastfeeding. Therefore more studies must be conducted to widen and inform health interventions. There is currently a global call from gender and public health advocates for more gender-disaggregated data to improve our understanding of the gender implications of COVID-19. Pregnant women must be included to create a foundation of understanding on the distinct experiences, vulnerabilities and risks they face.
The far-reaching impacts of this pandemic are still playing out, and require action now to protect the most exposed, and ensure the critical progress made in the global fight for gender equality is not undermined.