The longest mile in the COVID-19 vaccine cold chain
Promises of COVID-19 vaccine doses for developing countries will face challenges along the crucial cold chain.
- 24 November 2020
- 6 min read
- by SciDev.Net

Promises of COVID-19 vaccine doses for developing countries will face challenges along the crucial cold chain, writes Inga Vesper.
The world was unprepared for COVID-19 — but it has responded remarkably to the challenge of a pandemic. Nearly one year into the outbreak, 172 countries are involved in researching vaccine candidates for the virus.
On the surface, it looks like a new level of equity in global health has been achieved through the pandemic. But while developing the vaccine is a joint effort, access to it could be stymied by poor health systems and lack of infrastructure.
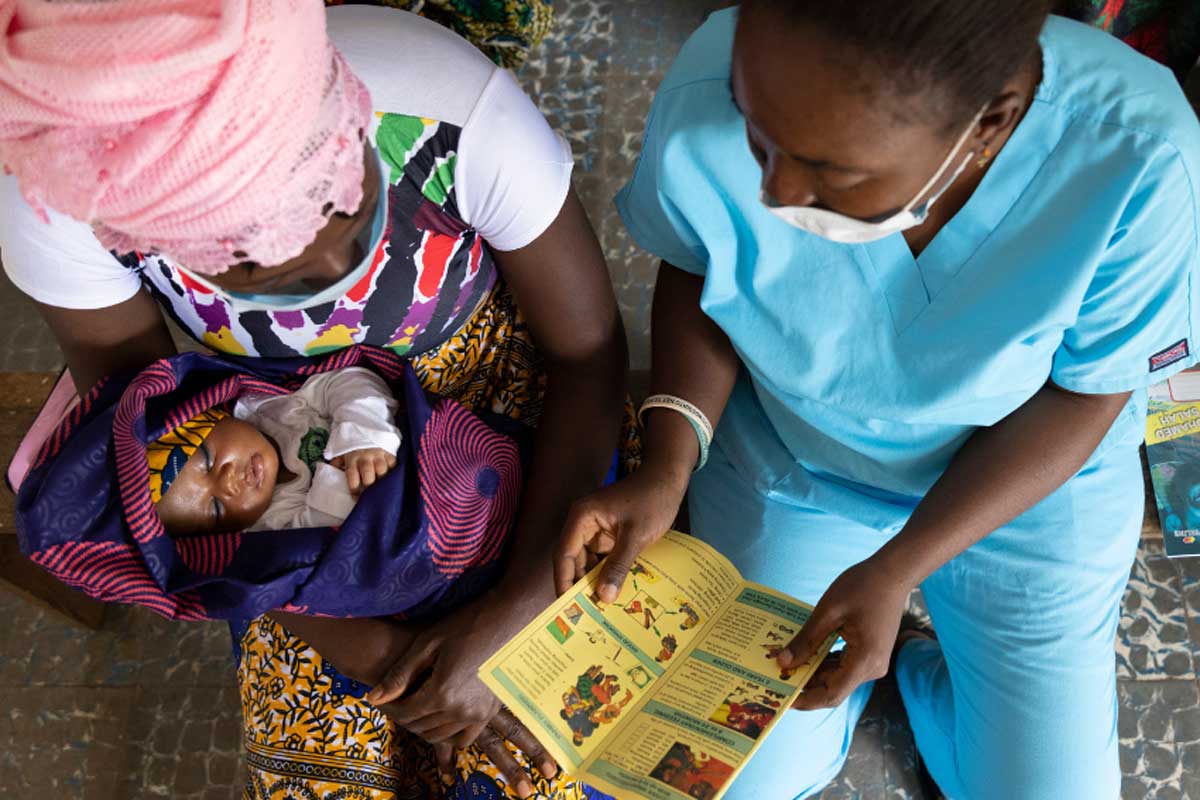
The scale of global vaccination needed to achieve some level of immunity to the virus is unprecedented — and almost unbelievable. India alone will have to vaccinate around 900 million of its people to reach the desired herd immunity threshold. In Africa, the number is pegged at 750 million people, many of who live in rural communities with limited access to healthcare.
The problem is the supply chain. Producing a vaccine, once it is researched, is relatively easy. But getting it to people requires a tangled network of shipping, storage, freezing, communication and healthcare that will be difficult to deliver globally — especially on the last mile of the journey.
“It’s the biggest logistical challenge the world has ever seen,” says Toby Peters, professor of cold economy at the University of Birmingham. “You’ve got a volume of vaccines that has never been tackled before, the speed requirements and the problem of outreach.”
Peters is involved in a research project in Bangladesh to develop a blueprint for future large-scale vaccination programmes in the global South. Supplying rural healthcare centres and remote villages at the end of the “gnarly” last mile is where logistics falter and up to 25 per cent of vaccine doses are lost, he says.
Cold chain
Across Asia and Africa, daytime temperatures hovering around 50 degrees Celsius are not uncommon, while the Middle East and Caribbean are also experiencing episodes of extreme heat and humidity.
It’s the biggest logistical challenge the world has ever seen.”
Toby Peters, University of Birmingham
COVID-19 represents a specific challenge: all vaccine candidates under investigation lose their potency fast at temperatures above ten degrees Celsius, as the antigen — the component that provides the immunisation — degrades quickly if not frozen. Several different protein antigens are currently being trialled around the world, but even the most resilient ones will require cooling.
This means that all current potential vaccine candidates for the disease will require cooling at between two and eight degrees Celsius, while some require freezing at up to minus 80 degrees Celsius throughout transportation.
This is the so-called cold chain: the ability to transfer and transport frozen goods seamlessly from cargo hubs into the smallest, most remote communities.
Infrastructure challenge
Cold chain infrastructure exists in most developing countries, but is insufficient in the last mile. According to Kostadin Fikiin, a professor of refrigeration technology at the Technical University of Sofia in Bulgaria, this makes around 40 per cent of existing vaccines unusable in poor countries.
However, countries with a strong food storage cold chain could easily adapt this to distribute vaccines, Fikiin says. He points to India as an example, which has the world’s fastest growing cold chain thanks to progress in technology.
“The cold chain capacity strongly depends on a country’s digitalisation level and communication technologies, for example for tracking and tracing,” Fikiin tells SciDev.Net. “Many of these technologies are affordable enough and feasible for the developing world, especially given the global coverage of satellite navigation systems.”
In addition, cold chain technology is increasingly better at adapting to developing country settings. Fridges and freezers are becoming smaller and more efficient, and many types can be powered with batteries or solar panels to protect them from power outages. Some of these fridges now weigh just five or ten kilograms, meaning they can be carried on foot into hard-to-reach regions. They also have data connectivity to enable the remote monitoring of the vaccines inside.
Storage times have also increased. Pfizer’s COVID-19 vaccine candidate could be stored for six months at minus 70 degrees Celsius and up to ten days in ice packs. Moderna’s candidate remains stable at minus 20 degrees Celsius for up to six months and can be stored in a fridge for 30 days. Johnson & Johnson’s candidate can be stored for up to three months at between two and eight degrees Celsius, the temperature of a standard fridge.
“This makes the COVID-19 vaccine candidate compatible with standard vaccine distribution channels and would not require new infrastructure to get it to the people who need it,” Luis Roman, vice president of global delivery for Johnson & Johnson subsidiary Janssen, tells SciDev.Net.
In the absence of a thermostable vaccine that can withstand the extreme temperatures experienced in some developing countries, Peters says the fridge stable vaccines will be better-suited for wider distribution in the global South.
“This does not change the need for robust cold-chain and the need to ensure equitable distribution, but it does perhaps make the types of equipment more standard,” he says.
Improvements in last-mile delivery during the coronavirus pandemic could have additional benefits. For example, they could open new, long-term markets for pharmaceutical companies, resulting in better access to other vaccines besides COVID-19.
Vaccine nationalism
But some scientists sound a warning note, saying that fixing the convoluted last-mile problem alone will not be enough to ensure vaccines are distributed everywhere swiftly. Earlier this year Richard Hatchett, chief executive at the Coalition for Epidemic Preparedness Innovations, warned of ‘vaccine nationalism’, a situation in which countries could distribute a vaccine worldwide, but will not do so until their own markets are satisfied.
According to Hilde Stevens, a senior researcher at the Institute for Interdisciplinary Innovation in Healthcare, this risk is particularly high for the COVID-19 vaccine, which is needed globally and immediately.
“The current corona crisis poses particular challenges with respect to unrestricted demand,” she says. “The vaccine-producing countries will face the dilemma to meet national vaccine demand and ensuring export to other countries. The question of price and demand risks leaving the poorest regions without access.”
For Peters, there is another issue that has been rarely discussed—that of sustainability. He hopes that politicians and healthcare organisations spending big on technology to tackle the tricky last mile will ensure that such infrastructure, once created, can be easily maintained and will generate as small an environmental impact as possible.
“We want to come out of the pandemic with a cold chain that covers 100 per cent of the global population,” he says. “Governments must get their heads around this quickly, but create capacity that can be used long-term — beyond COVID-19.”
Original article
This article is republished from the SciDev.Net under a Creative Commons license.