Nourishing roots: Why women’s health matters for all
Investment in locally led-innovation and midwifery can transform child and maternal health, write Nigerian health minister Muhammad Ali Pate and Samba Sow, former minister of health for Mali.
- 17 June 2024
- 5 min read
- by SciDev.Net

In many African cultures, women are often likened to the roots of a tree, providing stability, nourishment and support.
When women are healthy and empowered, they can unleash their full potential, creating a ripple effect of prosperity that strengthens families, communities and societies.
Consider one area where the roots are critical for a family to thrive — ensuring healthy mothers give birth to healthy babies.
“It is sobering to note that as you finish reading this piece, at least two more women will have died of preventable causes related to pregnancy or childbirth.”
Muhammad Ali Pate and Samba Sow
The world has made significant progress in maternal, newborn and child health over the last few decades.
Between 2000 and 2020, the global maternal mortality ratio decreased from 339 to 223 deaths per 100,000 live births. Similarly, the neonatal mortality rate declined by over 50 per cent— from 36.6 to 17.6 deaths per 1,000 live births — between 1990 and 2021.
In low- and middle-income countries (LMICs), 371 million women now use modern family planning methods, representing an increase of 87 million women and girls over the past decade.
The uptick in the use of birth control helps women control the spacing and timing of their pregnancies, preventing high-risk pregnancies, improving maternal health, and contributing to better birth outcomes.
Despite the substantial progress in maternal and newborn health, an estimated 287,000 women still die every year from preventable causes related to pregnancy and childbirth.
With 70 per cent of these deaths occurring in Sub-Saharan Africa, pregnancy and childbirth remain dangerous times for many women, exemplified by the tragic death of renowned Malian journalist Hawa Séméga during childbirth in 2021. Her story underscores the persistent disparities in access to quality maternal healthcare, even for prominent figures.
Globally, every two minutes, a woman dies from pregnancy complications, while in conflict zones that number doubles.
In LMICs, complications related to pregnancy and childbirth are also a leading cause of death among adolescent girls aged 15 to 19, and neonatal mortality rates are drastically higher, with 48 deaths per 1,000 live births compared to four deaths per 1,000 live births in high-income countries. These statistics demand immediate attention and action.
Investing in maternal, newborn and child health saves lives. It not only makes moral sense, it’s also sound economics. Healthy women are more likely to participate in the workforce, increasing productivity and economic growth.
According to a 2024 Report released by the World Economic Forum and McKinsey Health Institute at Davos, addressing the women’s health gap would boost the global economy by US$1 trillion by 2040, resulting in a 1.7 per cent yearly increase in per capita GDP.
Have you read?
One of the most dangerous complications of childbirth is postpartum haemorrhage (PPH). It is also the leading cause of death for mothers during childbirth.
Thankfully, investments in innovations — from cutting-edge technologies to low-cost, high-impact solutions — are making a significant difference.
A simple and affordable tool called a calibrated obstetric drape, which is a part of the WHO-recommended E-MOTIVE package, was tested across 80 secondary level health facilities in Kenya, Tanzania, Nigeria and South Africa.
This drape, together with the WHO recommended treatment bundle, allows trained birth attendants to monitor and measure blood loss in real-time, helping them quickly identify PPH and potentially save lives.
This treatment approach was shown to significantly reduce severe bleeding by approximately 60 per cent. It is a powerful example of how locally-driven innovation can have a global impact.
But innovations alone aren’t enough. Strong primary healthcare systems with well-equipped clinics, staffed by trained professionals, are the backbone of healthy communities.
These systems, with robust referral networks and reliable supply chains, ensure everyone gets the care they need, when they need it.
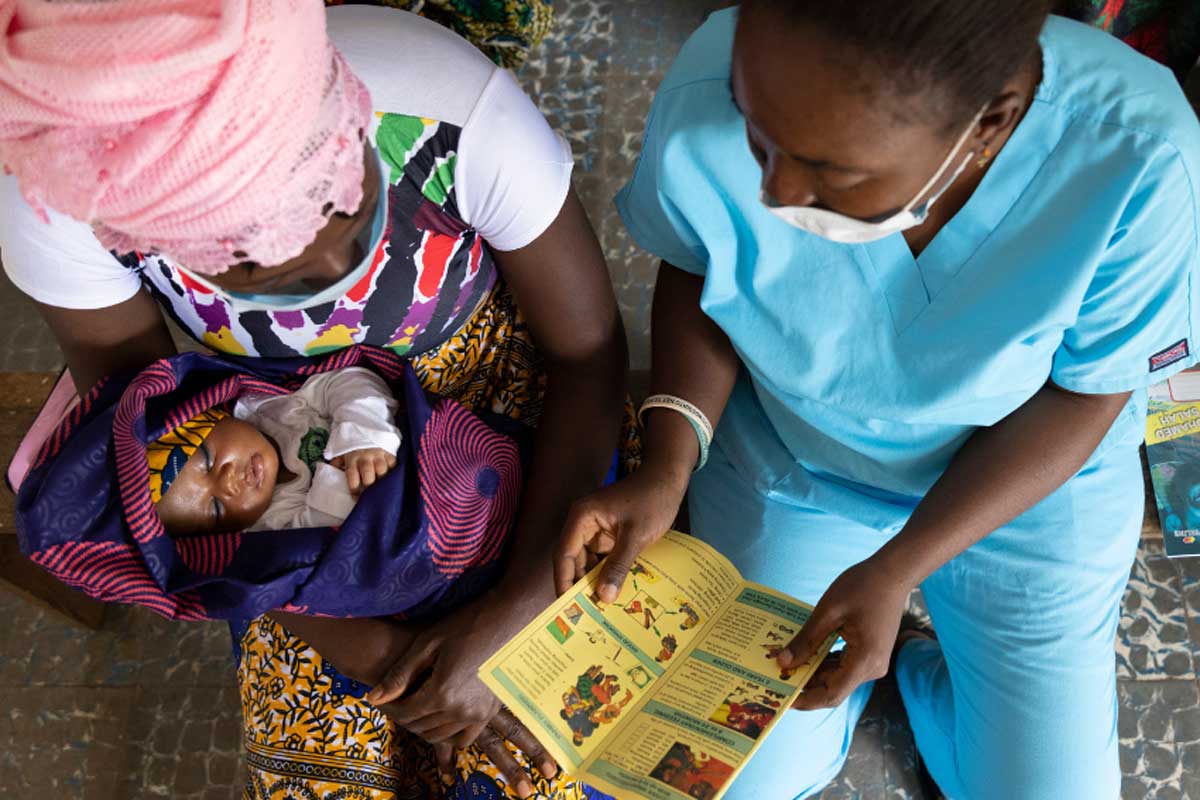
Equally important are the people delivering care. Empowering midwives and community health workers, who are often the first point of contact for mothers and children is critical.
Studies estimate that increased investment in midwives — who can provide up to 90 per cent of essential care for women and newborns — could save an estimated 4.3 million lives annually by 2035.
Today, we have a unique opportunity with the current data and evidence, combined with renewed energy, to reach the SDG goals by 2030.
We must commit now to ensuring that all women and babies, regardless of their socio-economic background or where they live, have access to the quality care they deserve.
This requires a transformation in how we prioritise and support the health of mothers and babies, particularly in Africa.
The good news is that we don’t have to do it alone. We need partners from the private sector, philanthropies and governments to collaborate more than ever to ensure women are healthier, and in turn, their families, communities, and economies thrive.
The moment is now to work collectively across sectors to strengthen primary healthcare systems, empower healthcare workers and accelerate access to these lifesaving tools.
It’s sobering to note that, as you finish reading this piece, at least two more women will have died of preventable causes related to pregnancy or childbirth.
This stark reality underscores the urgent need for investments in the tools and systems to transform maternal and child health realities across our continent.
Muhammad Ali Pate is Nigeria’s minister of health and social welfare. He was formerly the global director of health, nutrition and population global practice at the World Bank. Samba Sow is a former Minister of Health for Mali and currently director general of Mali’s Center for Vaccine Development. In 2020, he was appointed as one of six Special Envoys to the WHO on COVID-19.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.
Written by
Muhammad Ali Pate and Samba Sow
Website
This article was originally published by the SciDev.Net on 6 June 2024.
More from SciDev.Net
Recommended for you