Duncan Graham-Rowe, Gavi
Ten-year-old Princess Ko waits patiently with the other girls until her name is called. As her parents watch on, she enters the small open hut that serves as a community health centre to receive her first shot of human papillomavirus (HPV) vaccine. There is a sense of
anticipation in the air, yet as she feels the scratch of the needle in her upper arm she neither winces nor grimaces. Instead Princess looks down at the small pinprick and smiles with pride, and perhaps just a hint of relief. Having lived through the West African Ebola epidemic and the measles outbreaks that followed, she and her parents understand the importance of vaccination and how
fortunate she is to be among the first in Liberia to receive this potentially life-saving vaccine.
Princess is even more fortunate than she realises. This HPV demonstration project taking place in Bong County, just 200 km outside the capital, Monrovia, is part of a joint roll-out – with rotavirus vaccine. It is also one of the first HPV vaccination sessions that draws on lessons learnt from earlier introductions and targets girls both in and out of school.
Since Gavi started supporting HPV vaccines, demand has been extremely high. While countries recognise the importance of HPV vaccination for reducing cervical cancer rates, the target population – girls aged between 9 and 13 years – is not easily reached through
immunisation programmes more suited to vaccinating infants. The 21 countries that have already introduced the vaccine with Gavi support, including 6 in 2015, do so largely through school-based campaigns. While this approach has successfully reached many girls, it leaves open the question of how to access those who do not attend school.
Princess is one of eight girls attending the vaccination session in Bong who do not go to school. That’s because the nearest school is a five-mile walk away, along a busy highway – a journey that most parents consider too dangerous for their child to make each day.
In order to reach girls like Princess and her friends with HPV, Liberia is raising local awareness of cervical cancer prevention through face-to-face meetings with community leaders. This helps ensure high turnout for HPV vaccination sessions in community health centres, such as the one in Bong.
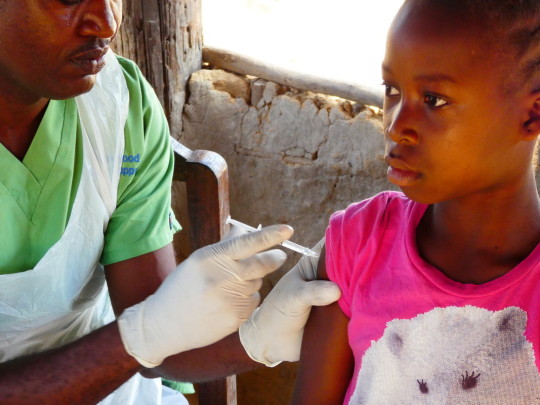
A girl receives her HPV vaccine from a health worker. Photo: D. Graham-Rowe.
Other countries are watching Liberia’s new approach to HPV roll-out with interest. Since most countries have only introduced HPV vaccines in districts with high levels of school attendance, we have very little evidence for what works when this is not the case. However, it is anticipated that when combined with school-based HPV vaccination sessions, social mobilisation projects like the Bong example will help to increase national coverage rates and reduce health inequity by reaching some of the more marginalised members of society.
The Liberia experience will also help to inform efforts to use HPV vaccination as a platform for rolling out broader adolescent health and education interventions, such as nutrition, deworming, body literacy and menstrual hygiene. Finding ways to reach girls like Princess is vital if we want to stop the rise in cervical cancer deaths. Currently around 266,000 women die from this form of cancer every year, equating to roughly one every two minutes. The figure may already exceed the annual number of maternal deaths and,
without intervention, is expected to reach nearly 416,000 by 2035.
For Princess however the good news is that there is talk of building a school in her village, which means she won’t miss out on an education. As for the HPV vaccine, Princess beams as she holds up her vaccination card. She’s got that covered.
This post was originally published as part of Gavi, the Vaccine Alliance’s Annual Progress Report, which you can read here.
For more about our support for HPV vaccines in developing countries, see here.