World Immunization Week: Eradicating cervical cancer through HPV vaccination
UICC’s Director of Special Projects, Dr Julie Torode, highlights the importance of continuing to push forward with the global strategy to eliminate cervical cancer despite the current coronavirus pandemic.
- 30 April 2020
- 4 min read
- by Gavi Staff
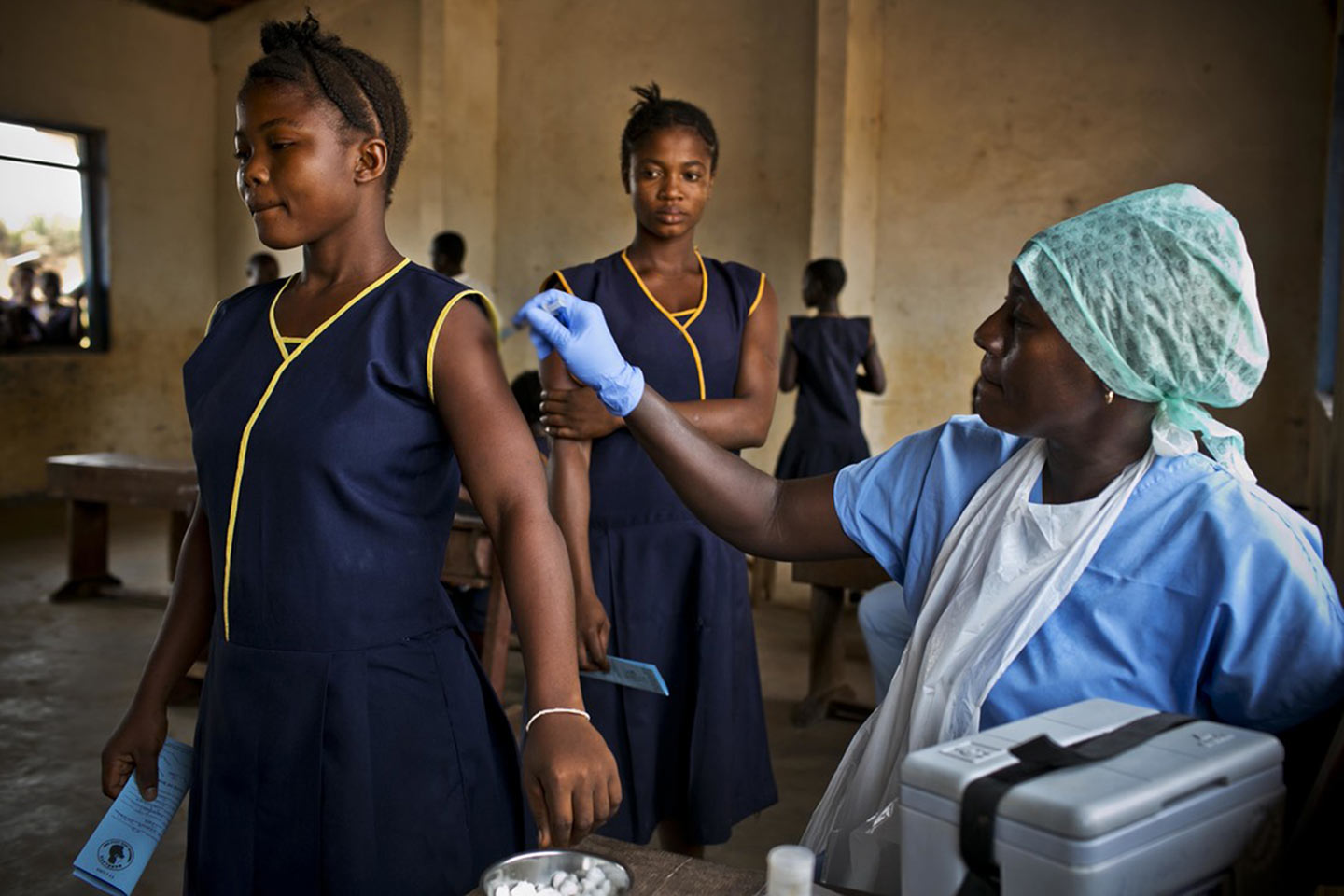
When I joined UICC 12 years ago, one of my first activities was to represent my new organisation at the steering group of Cervical Cancer Action, an advocacy network comprising civil society and academic groups that was established the previous year. Our big focus in 2008 was to urge the board of GAVI, the Vaccine Alliance, to adopt the HPV vaccine as part of its portfolio.
Back then technology was a lot simpler and we relied on a bound set of letters of appeal gathered from cancer organisations, women and community groups as well as governments affirming their readiness to support HPV vaccination programmes where they were needed the most - in countries with the highest burden of cervical cancer, often spurred by HPV-HIV co-infection, but with no affordable access to a vaccine that is both safe and effective in preventing this devastating cancer.
By joining forces with partners such as the American Cancer Society, Jhpiego, PATH and Cancer Research UK, we were able to achieve our aim of submitting a collective call for action to the fall board meeting. A number of board members gave us the informal feedback that the loud thump of the bound letters on the board room table alone was an effective advocacy tool, grabbing the attention of the room.
Unfortunately, what we did not anticipate was the global financial crisis that struck that same year. GAVI board members took the decision to consolidate and ensure they could maintain the existing portfolio of commitments to Member States. GAVI revisited the decision a year later and by the end of 2020, Gavi will have supported the introduction of the HPV vaccination in 24 countries and helped protect 14 million girls by doing so. A new platform was also introduced for countries to build community conversations to address gender-specific health issues like women’s cancers, from childhood.
Women’s empowerment has major potential to facilitate the ambition to eliminate cervical cancer. Stepwise scaling of programmes towards the 2030 target of 90% of girls vaccinated by age 15 can be boosted by improving the status of women in many societies. HPV vaccination is an excellent opportunity to educate girls and their families about vaccines and improve health literacy more broadly, identify and tackle gender barriers and address gender issues that restrict access to health centres.
The irony is not lost on me that in 2020, as the vision of a world free of cervical cancer is on the cusp of being adopted by governments around the world, we are again facing a global crisis. The coronavirus pandemic and looming economic crisis threatens to divert global health and development attention from the unique opportunity to eliminate a cancer.
2020 has seen the World Health Organization (WHO) and partners establish a global commitment. The resolution supporting the elimination of cervical cancer was sponsored by 50 countries from all geographies. I am confident, therefore, that the advocacy community will be able to reach women to build the community demand for the protection they deserve in the post-coronavirus era. Publications in The Lancet report that if 78 of the world’s poorest countries rapidly add HPV vaccines to their routine immunisation, it could help prevent 62 million cervical cancer deaths in the coming decades. World Immunisation Week is a timely milestone to remind ourselves of the potential to #ProtectTheNextGeneration and ensure that #VaccinesWork for All.
 | Dr Julie Torode, Director of Special Projects, Union for International Cancer Control, Geneva, Switzerland |
_Logo.png)
This article is republished from UICC under a Creative Commons license.
Related content
More from Gavi Staff
Recommended for you
















