Coronavirus risks creating a lethal vaccine gap
Could the impact of COVID-19 on routine immunisation be an even bigger threat in low-income countries than the virus itself?
- 3 April 2020
- 3 min read
- by Ciara McCarthy
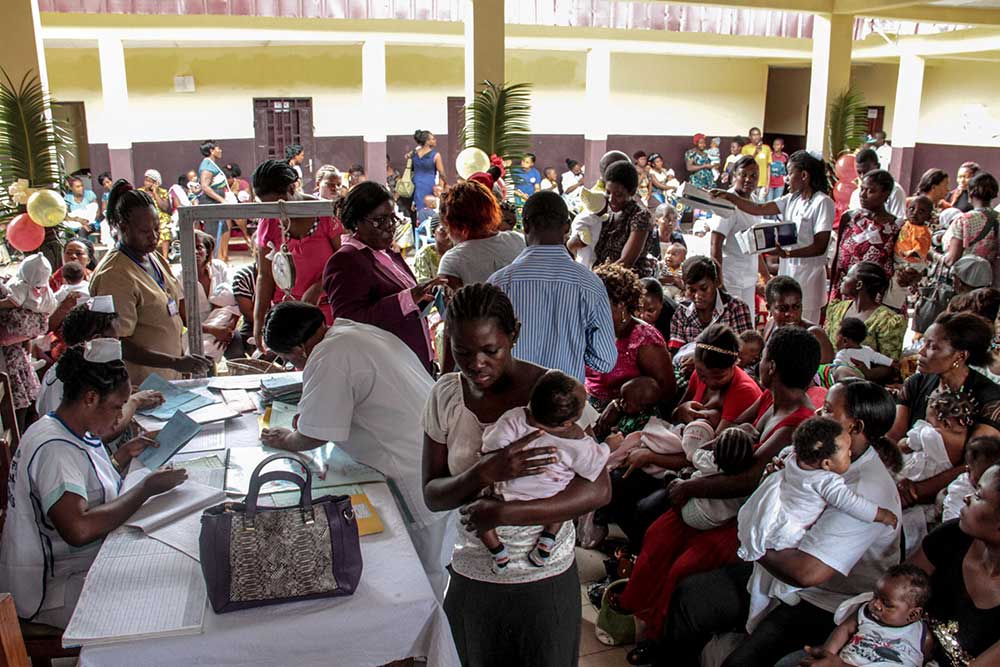
There has been a lot of attention globally on concerns about shortages of masks, testing kits and other medical supplies that are urgently required to respond to the COVID-19 crisis. Yet just outside the limelight, supplies needed to keep basic health services running are also at risk. At least 21 countries globally are already reporting that their stocks of basic vaccines are running low.
Impact of COVID-19 on vaccination
Disruption to scheduled flights and border closures are having an inevitable impact on vaccine supply chains. On top of this, ensuring the vaccines that countries do have access to continue to reach the children who need them poses another challenge.
The World Health Organization’s Strategic Advisory Group of Experts (SAGE) on Immunization has advised that all mass vaccination campaigns, such as measles, yellow fever and cholera, are halted. Increasingly, physical distancing measures could prevent families from getting their children to health centres to receive routine immunisation.
Health workers can be forced to divert their attention to COVID-19, leaving a vacuum in the workforce delivering routine services. Such measures can be necessary to tackle the more pressing health threats posed by COVID-19, but they can create challenges to ensuring that they do not jeopardise the future health of today’s children. Already, 14 Gavi-supported vaccination campaigns and 4 national vaccine introductions have been postponed, meaning that over 13.5 million people in 14 of the world’s poorest countries will miss out on vaccines. This figure is likely to rise in the coming months.
As we saw with the 2014-2016 Ebola epidemic in West Africa, infectious disease outbreaks can have a devastating impact on the ability of health systems to deliver routine health care. An estimated 10,600 lives were lost to HIV, tuberculosis and malaria during the epidemic – that’s almost as many as the number of deaths from Ebola itself. During the most recent outbreak in the Democratic Republic of the Congo, a concurrent outbreak of measles killed twice the number of people as Ebola.
Have you read?
Impact of vaccination on COVID-19
Conversely, maintaining immunisation coverage is important for ensuring health systems are able to respond as effectively as possible to the pandemic. When coverage of a vaccine falls, we often see a rapid resurgence of the disease that it prevents.
If a greater proportion of the population are susceptible to the disease – i.e. not protected by vaccination – then there is more opportunity for the pathogen to spread. In the case of highly infectious diseases like measles, even small drops in vaccine coverage can have a major impact on transmission. Many health systems now facing cases of COVID-19 are already under pressure from outbreaks of vaccine-preventable diseases. In the DRC, cholera, polio and measles are already overloading a fragile health system. Routine immunisation is crucial to keeping these diseases at bay so that health workers have more capacity to focus on COVID-19.
In the short term, the measures put in place in response to the pandemic may themselves go some way to mitigating its impact on vaccination coverage. Physical distancing measures and greater focus on clean water and sanitation could be beneficial in slowing the spread of a whole host of infectious diseases, not just COVID-19. Although often such measures are not feasible. And once measures lift, countries will need to rapidly make up for lost time. Otherwise, the gaps in vaccination created by this outbreak could have an impact on the incidence of infectious diseases for years to come.