
But Prevention Can Save Many Lives at Risk
The hosting of a Health Day at the upcoming 28th Conference of the Parties to the United Nations Framework Convention on Climate Change (COP28 UAE) by the United Arab Emirates Presidency signals a recognition of the multiple impacts of global warming on health.
There is no vaccine for climate change and never will be. There are however multiple readily available health interventions and prevention measures that can help save many lives directly threatened by climate disasters, extreme weather events and more discreet environmental trends.
In 2022 alone, 32.6 million people were displaced within their countries, the highest number ever recorded, driven mainly by weather-related hazards, including floods, storms and droughts. The number includes, for instance, drought in the Horn of Africa, floods in Pakistan and intense cyclones in Bangladesh and the Philippines – which is more than forced migration due to conflict and violence. This also means more people being deprived of essential health services, such as childhood immunisation.
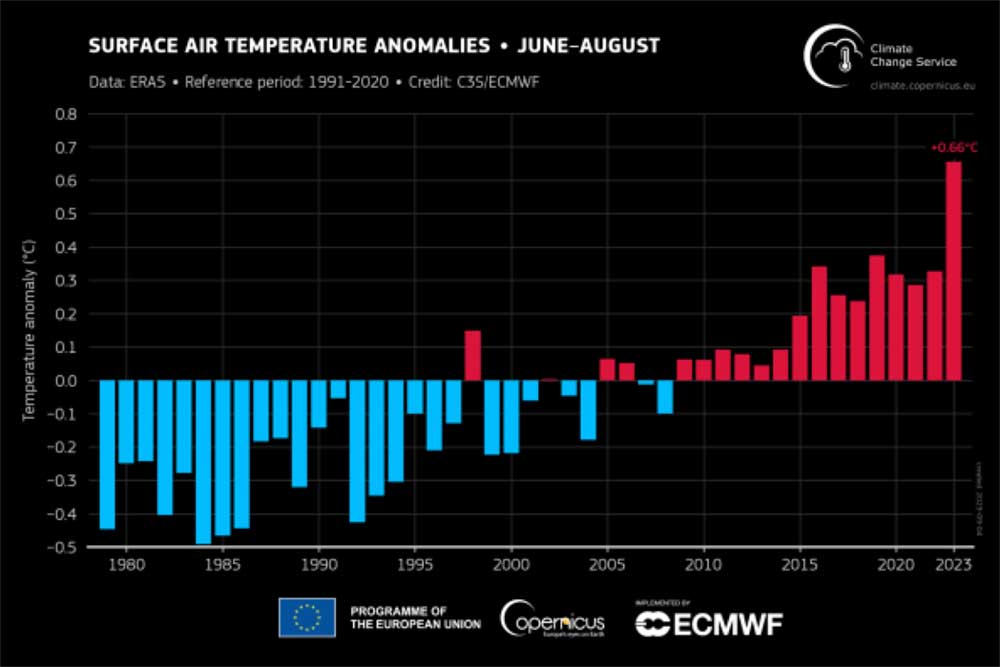
In 2023, the earth had the hottest three-month period on record, with unprecedented sea surface temperatures and much extreme weather. High global temperatures are increasingly impacting the health and survival of people worldwide and projections show that these risks could worsen with further inaction. If we add the associated economic losses to the climate crisis, the people being harmed first and worst are those living in low-income and disadvantaged countries and communities.
Despite this worrying scenario, one out of six countries does not yet have a national adaptation plan to address the impacts of the climate crisis. Underfinanced, countries face even wider gaps when it comes to incorporating public health measures into those plans.
Fortunately, some positive trends are emerging: a recent review shows that 60% of 193 "nationally determined contributions" (NDCs) refer to one or more climate-sensitive health risks or outcomes. However, countries are still far from translating these commitments into preventive health measures in their national adaptation plans.
Have you read?
Projected climate change will impact human health by exacerbating old and new health problems, especially in low-income countries. In addition to risks of increased malnutrition, health impacts include greater likelihood of foodborne, waterborne and vector-borne diseases. Up to 8.4 billion people could be at risk of diseases like dengue and malaria by the end of the century if emissions keep rising at current levels. Even if mitigation and adaptation activities are successful, it would still be 6.1 billion people potentially threatened.

Changes in malaria transmission, for instance, derive from the environmental and climatic requirements of the vector (Anopheles mosquitoes) and Plasmodium parasites. Under a scenario compatible with limiting temperature rise to 2°C, 23% of areas not suitable for malaria transmission between 1995 and 2014 could become suitable in 2041–60. Considering a scenario in which no further mitigation occurs, this figure rises to 26% in 2041–60.
There are vaccines against some of these deadly climate sensitive diseases such as yellow fever or cholera. And more are coming. For instance, earlier in July, Gavi, the Vaccine Alliance, announced that 12 countries in Africa were allocated a total of 18 million doses of the new malaria vaccine RTS,S/AS01 for the 2023–2025 period. And just last month the World Health Organization recommended the world's second malaria vaccine, paving the way for a significant expansion in the global supply of malaria vaccines and increasing the diverse range of tools available to fight malaria.
The other piece of positive news is that health professionals and the organizations they represent are increasingly advocating for the transition to more resilient and low-carbon societies, building on their reputation as trusted partners. This is critical as insufficient adaptation measures are still the norm. Inaction leaves health systems vulnerable to climate-related health hazards, undermining long-term delivery of basic health interventions. It is, therefore, urgent to mobilise the strength of the health community to drive policy change and to build public support for the inclusion and operationalisation of preventative health measures in national adaptation plans.
Strengthening surveillance and vulnerability assessments of climate-sensitive diseases to build associated immunisation programmes must be an integral part of countries' efforts to protect their populations from the health impacts of a warmer planet.
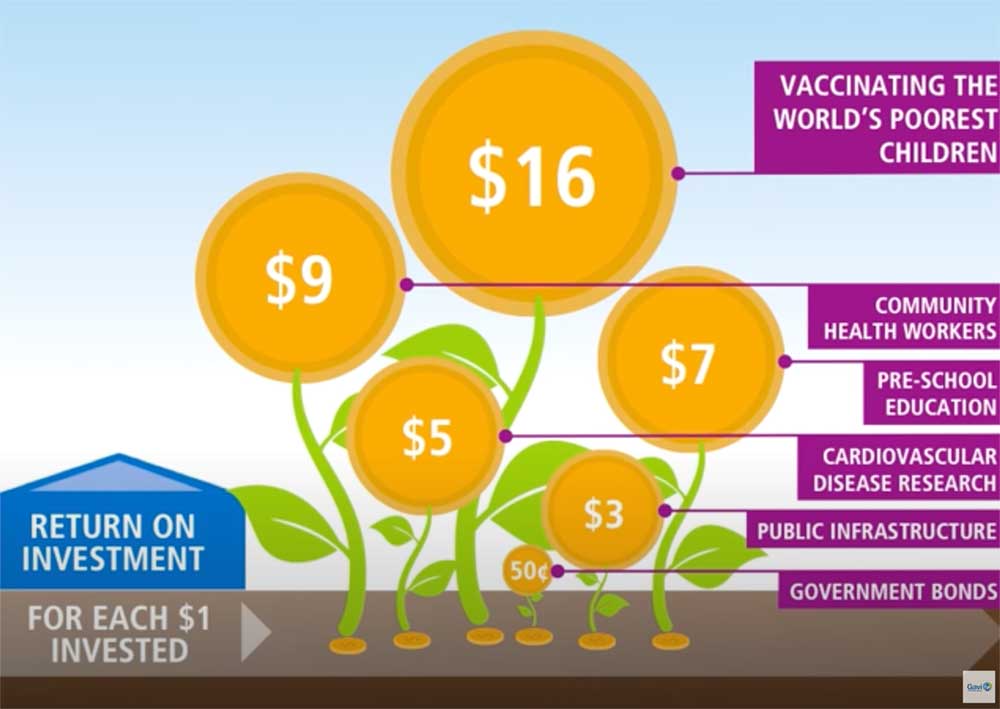
Given that the climate crisis is threatening countries' abilities to deliver essential vaccines, investing in routine immunisation continues to be a "best buy", as it helps communities, particularly the most marginalised, build resilience and mitigate the risk of some of the deadliest diseases, while laying the foundation for health system to prepare for and respond to climate and other health emergencies.
Website
This article was originally published on Pascal's LinkedIn on 22 November 2023.
More from Pascal Barollier
Recommended for you









