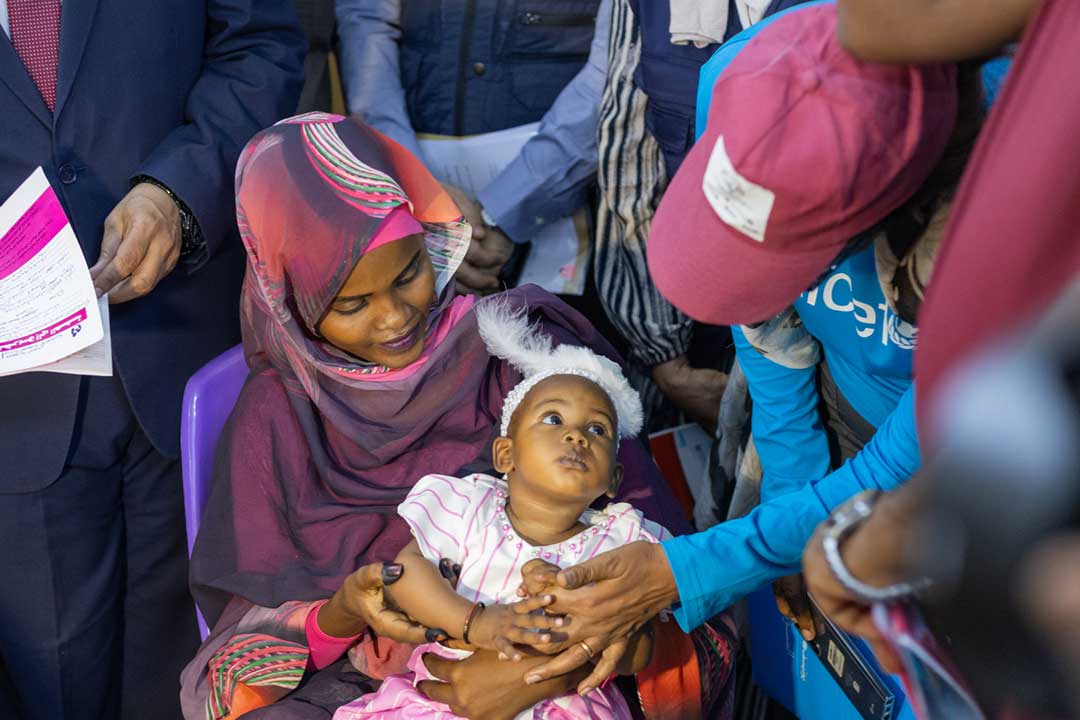
The vaccine back-stop
Checking vaccination status when children visit health facilities can be a highly effective way to catch up those who have missed vaccinations.
- 9 July 2024
- 7 min read
- by Ian Jones

No matter how good immunisation programmes are, some infants fall through the net and do not receive the vaccines they need at the optimal, recommended moment. But when it comes to vaccination, it’s better late than never.
Following drops in immunisation coverage seen during the COVID-19 pandemic, Gavi and other partners are spearheading the “Big Catch-up” initiative. But more generally, “catching up” missed children is an important responsibility of integrated primary health care systems, both during outreaches and at the clinic. Going out into the community to provide care takes time and effort to organise, so it makes sense to provide a bundle of services, including vaccination. Meantime, when caregivers attend health facilities with their child for any reason, their visit is an opportunity to ask about immunisation status, and may offer a chance to provide deliver vaccine doses.
For the immunisation session at Teach to Reach 10, an experience-sharing event that took place on 20 June 2024, drawing participation from more than 21,000 health workers from the Global South, the Geneva Learning Foundation (TGLF) invited attendees to share their experiences of integrating services. Their responses offer insight into the nimble pragmatism of primary health care done right.
In some cases, immunisation catch-up activities piggy-back onto other community-oriented services:
“During family planning activities, routine vaccination was integrated. This made it possible to catch up with several children who had not yet received their first dose of measles vaccine… This activity helped reduce the incidence of measles cases in the community. This strategy also made it possible to reduce the costs of implementing the routine EPI because the agents had the possibility of thinking of several activities in a single outing.”
- Anon, Sanitary Technology Engineer, Ministry of Health, Yamoussoukro Health District, Côte d’Ivoire
Other contributors described how activities had been planned around community events, with services provided for multiple age groups:
“Vaccination days were set as days of intensification of nutritional activities. Every month in some of my health facilities, we choose the fair days as health fairs. A child can receive the care they need, such as screening for malnutrition and its management, vaccination or catch-up, deworming, nutritional advice. For adults, they can receive screening for diabetes or its control, control of blood pressure. Everyone welcomes the time-saving, money-saving benefits of integrating primary health care services.”
- Fousseyni Dembele, Public Health Physician (MPH), Mali
The benefits can also work in reverse, with routine vaccination activities in the community providing an opportunity to deliver additional services:
“The most memorable story of child vaccination is when we went for community outreach for child immunisation. A little girl was brought for immunisation and what she needed was a vitamin A supplement. When we asked the mother to bring her the vitamin, the little girl refused, with tears gushing out from her eyes. We had to get some sweets to give her in order to get her trust. After giving her the sweets with a smile on her face then we presented the vitamins and she received them happily.”
- Esther Yusuf Yakubu, Public Health Specialist (MPH), NGO, Plateau State, Nigeria
A highly effective catch-up strategy is avoiding “missed opportunities for vaccination” (MOV) – contacts with health services that do not lead to identification and vaccination of under-immunised infants. In many countries this is a national policy and formal part of daily practice:
“This vaccination practice is common here in Côte d’Ivoire. During daily consultations, if a child presents to our services, whatever the cause for which they came and their state of health allows it, we vaccinate them. This practice makes it possible to catch up with those who are not up to date in the schedule and also improve vaccination coverage.”
- Sopi Sess Michel, Sanitary Engineering Engineer, Ministry of Health, San Pedro, Côte d’Ivoire
While the strategy can be written into national or institutional policies, it is vital that it is adopted in practice. Several respondents described how, as well as providing care for a sick child, they have also taken the time to enquire about immunisation status:
“One day a woman came to our health facility who was having a fever and cough. The woman had a five-month-old baby also. We attended to her complaint and gave her the medicine she deserved. After that, we asked her about the immunszation status of her baby but surprisingly, she said that the baby did not have any vaccine. She said that there was no nearby health facility providing vaccinations. On hearing that, the health worker in charge of vaccination counselled her on the need to have her baby vaccinated and that she could come to the facility on an appointed date for her baby to complete her immunisation schedule. After convincing her, the baby was administered the vaccines appropriate to her age schedule. The woman was happy and showed her appreciation.”
- Abdulrahman Umar Pella, Community Health Practitioner, Gombi Local Government Area, Nigeria
This personal approach enables the causes of missed vaccinations to be approached. In the context of caregiving, people may be more receptive to messaging around vaccination:
“A baby was rushed to my facility sometimes last year around Christmas. The baby was convulsed and the mother was crying thinking that the baby will not survive it as the baby is the only survivor child for her. Myself and the hospital tried to stabilise the child and when the mother calmed down to see her child had come around, I called the mother to my office confidentially to ask some vital questions about immunisation, when I got to know that the child had never been given immunisation. I asked the mother further the reason why she didn’t take her child for immunisation. She confided in me that, due to a still birth, a herbalist warned her not to immunise her child. I asked her to bring her husband to convince both together and tell them about the importance of immunisation. Up till now the child is doing well because we asked her to give the child immunisation, which she did after several pleading. The procedure that made this work for me is confidentiality and trust.”
- Eegunjobi Anifat Omowumi, Public Health Specialist (MPH), Ministry of Health, Ladoke Akintola University of Technology Teaching Hospital, Ogbomoso, Oyo State, Nigeria
Have you read?
A failure to have a child vaccinated is not always a sign of antipathy to vaccination. Sometimes other priorities intercede, so vaccination at another contact with the health service can provide a more convenient opportunity for caregivers:
“One such memorable experience involved a mother who brought her young daughter to our facility for a routine check-up due to a mild respiratory infection. As I conducted the check-up, I engaged the mother in a conversation about her child’s overall health and vaccination status. Through our discussion, I discovered that her daughter had missed several key vaccinations due to the family’s recent relocation and the disruptions caused by it. The mother was unaware of the importance of staying on schedule with the immunisation plan and the potential risks of missing vaccinations. Recognising the opportunity, I explained the benefits of vaccinations and addressed her concerns about vaccine safety. I informed her about the policies in place at our facility that allow for the integration of immunisation services with other health visits. Our health facility operates under a policy that promotes a holistic approach to health care, ensuring that every patient encounter is maximised for comprehensive health promotion. With the mother’s consent, I was able to administer the necessary vaccines during the same visit. This not only saved her an additional trip to the facility, but also ensured that her child was up to date with her immunisation schedule.”
- Fatima Ado Garba, Nurse, Gashua, Nigeria
Several respondents noted that these valuable activities are not always easy in practice – but the potential benefits are great:
“Integrating immunisation with other services wasn’t always straightforward. I faced several challenges, such as time constraints during busy clinic hours, limited vaccine supplies, and occasional resistance from parents who were sceptical about vaccines. Additionally, the health facility’s electronic health record system, though useful, sometimes had issues with updating and retrieving vaccination histories promptly… I believe that continuous training for health care staff on integrating immunisation with other health services, coupled with community outreach programmes to build trust in vaccines, could significantly reduce missed vaccination opportunities and improve overall public health outcomes.”
- Claudius Mbuya, Social Worker, NGO, Kisumu, Kenya
Note: Contributor quotes in this article are their own and do not necessarily represent their employers.
Request your invitation for Teach to Reach 11 https://www.learning.foundation/teachtoreach
View recorded Teach to Reach sessions https://www.youtube.com/playlist?list=PLti7k0eaN3gQM1Vnie2tjar6rih9FqTfk
Get access to peer learning resources from the IA2030 Knowledge to Action Hub https://www.learning.foundation/ia2030-knowledge-action-hub