What kind of tests are there for COVID-19?
Large-scale testing for COVID-19 could help solve some of the mysteries surrounding the virus that are still puzzling scientists.
- 1 April 2020
- 3 min read
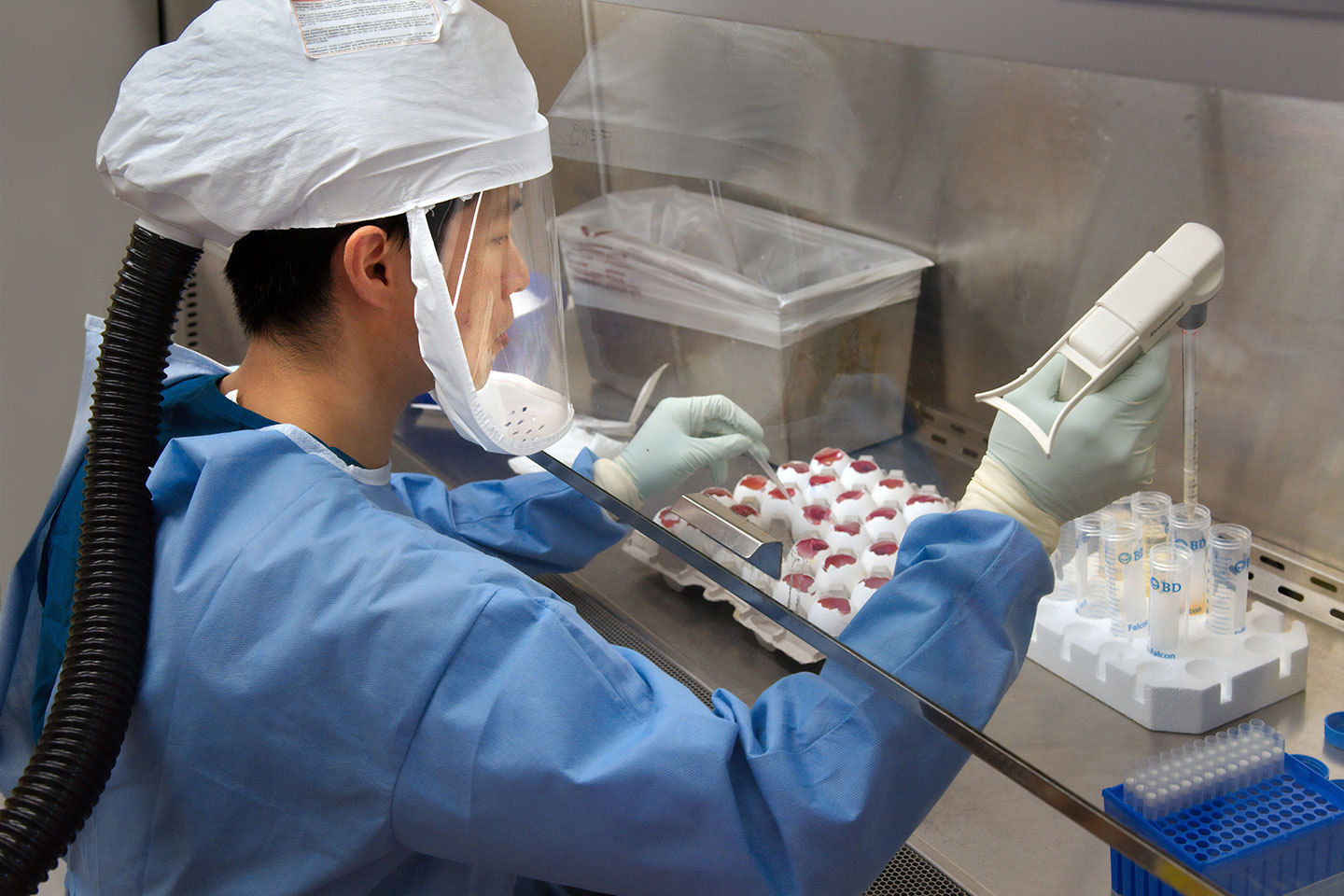
Diagnostic tests are a key part of the response to any outbreak. They are not only essential in correctly diagnosing patients, but can also help establish who has been infected in the past.
This can play a critical role in ensuring people get the treatment they need and in the response to the pandemic, by helping to improve contact tracing to prevent the further spread of the virus. At the moment, thousands of people are being tested worldwide every day to identify those infected with SARS-CoV-2, the virus behind COVID-19. Yet depending on the type of test we use, their value can go beyond case management. Large-scale testing, even of people without symptoms, could give valuable insight into how the pandemic will progress.
Testing for the virus
Current tests involve collecting nose and throat swabs from patients with suspected COVID-19. If the virus is present in the cells collected from these patients, viral genes can be detected using a technique called polymerase chain reaction (PCR). This selectively amplifies a sequence of DNA, in this case from a SARS-CoV-2 gene. This offers a highly specific way of detecting the presence of the virus, even from a very small sample. PCR-based tests are being used to varying degrees by countries across the world to identify patients with active infection.
Testing for immunity
But there are also growing calls for serological testing. Rather than looking for the virus itself, these detect antibodies specific to SARS-CoV-2. When a person becomes infected with a pathogen like the virus behind COVID-19 – whether they show symptoms or not – the immune system usually produces antibodies specifically targeting the virus. It can take a week or more for the body to produce these antibodies, and so the test can be less useful for detecting recent infection. Yet antibodies remain in the blood after the virus itself has been cleared, and therefore their presence can indicate that a person has previously been infected with the virus and recovered.
This in itself can be useful and has important implications for our response to the pandemic. If health workers who have previously contracted the virus are immune, they could treat COVID-19 patients without putting themselves at risk. This logic could be extended to other key workers: Germany is even considering issuing “immunity certificates,” allowing people who are immune to leave lockdown early. Monitoring antibody levels in people who have recovered can also give us insight into how long immunity lasts, which could be important for how we use future vaccines.
Beyond its impact on individual patients, large-scale use of antibody testing could help solve some of the mysteries about this virus that are still puzzling scientists. It could determine whether the small number of cases reported in children are down to fewer infections or milder symptoms. It could also help establish a more accurate infection fatality rate by revealing a truer picture of how widespread the virus actually is. And ultimately, by giving us a better estimate what proportion of the population are already immune to the virus, it will help predict how quickly the virus will continue to spread. This could provide a key piece of evidence in determining how and when physical distancing measures can be relaxed and economies re-opened.





