Why mothers and babies will suffer more as Africa grows hotter
As Africa gets hotter, mothers and babies are most at risk. Why is this and what can be done about it? Matthew Chersich, a specialist in climate change and maternal health, explains the reasons to health editor Nadine Dreyer.
- 13 September 2023
- 5 min read
- by The Conversation
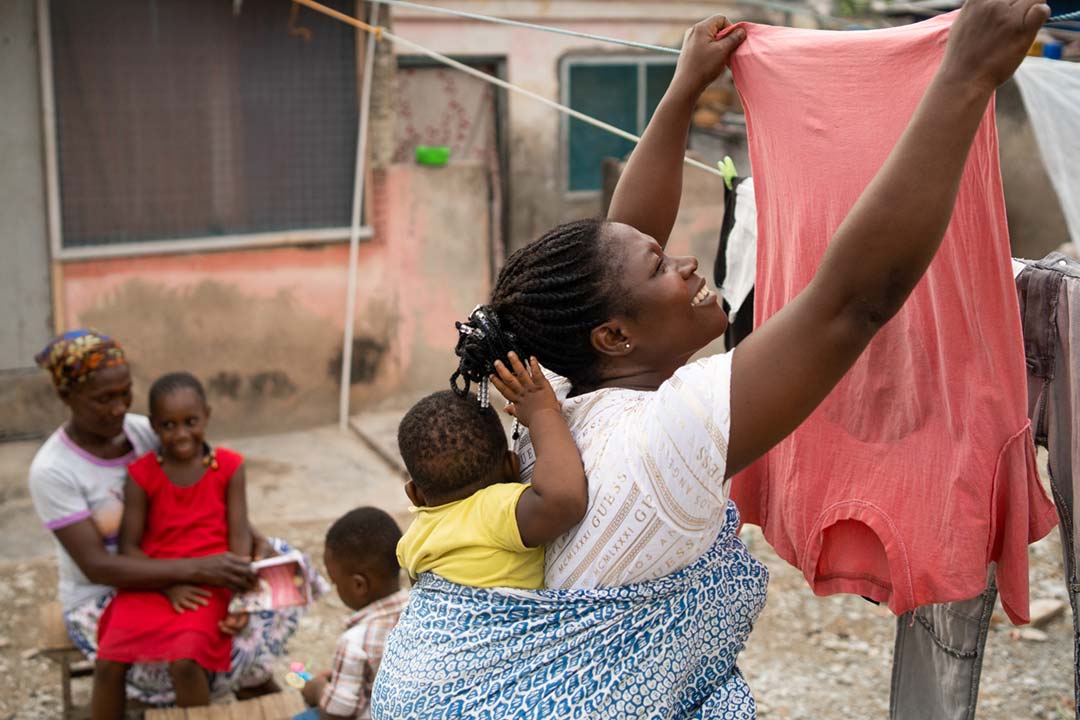
What makes pregnant women particularly vulnerable to extreme heat?
Many women in Africa have little or no protection against extreme heat events, with pregnancy being an particularly vulnerable period. High ambient temperatures may overwhelm the capacity of the maternal thermoregulatory mechanisms to dissipate heat in pregnancy.
Foetal metabolism generates considerable heat in the mother’s body. Then there is the strain from additional weight gain in pregnancy, fat deposits that retain heat, and the major exertion of labour and childbirth.
The foetus remains around 0.5℃ warmer than the mother and thus if a mother has heat stress or a fever, the foetal temperature quickly reaches dangerous levels.
The most dangerous period is likely during childbirth, when women generate remarkable levels of heat from the labour process. If this occurs during a heatwave it can increase complications, such as prolonged labour, increased emergency caesarean sections and maternal haemorrhage.
What makes babies particularly vulnerable?
Infants are dependent on their carers for protecting them against heat exposure. Some practices, such as over-swaddling, pose considerable risks as global temperatures rise.
Dehydration is also a major concern for young children, due to water loss through sweating or from gastroenteritis, which increases as food- and water-borne pathogens replicate more frequently and survive longer during warm weather.
Mothers may also supplement breastfeeding with water. In many areas, water is unsafe because of poor infrastructure.
Infants may breastfeed for shorter periods during hot weather as feeding can be uncomfortable for baby and mother in the heat.
In one of our studies in Burkina Faso, breastfeeding duration was about 25 minutes shorter on hot days compared to cold days.
It is possible to quantify the effect of climate change on pregnant women and newborn babies?
We are able to calculate the relative risk of adverse birth outcomes, such as preterm birth, which increases about 1.15 fold during heatwaves. The key gap in the field is quantifying the absolute number of additional adverse outcomes that are occurring because of climate change.
Those figures would help people to appreciate the implications of climate change for maternal and child health. There are real concerns that extreme heat may reverse the previous gains made in maternal and child health, from childhood vaccines, for example.
Have you read?
In some of our work we estimated how many additional child deaths occurred in Africa from heat exposure. We showed that there were between 7,000 and 11,000 deaths from heat exposure in children in Africa annually that could be attributed to climate change. Unless we curb carbon emissions dramatically, heat-related child mortality in Africa may reach over 38,000 a year in 2049.
A study of pregnant women in Johannesburg showed that rates of severe hypertensive disorders in pregnancy increase by as much as 80% when temperatures exceed 23℃ in early pregnancy.
Do different health issues affect mothers and children?
While the harms of exposure to extreme heat in pregnancy are well known, we do not yet have easy ways of calculating how much of that additional burden of disease is due to climate change, as opposed to natural variations in temperature. The methods for doing so are improving rapidly, however.
What is clear is that if South Africa experiences the kinds of temperatures that were seen in Europe and North America in 2023, there will be many thousands of additional pregnancy complications, all of which will be directly attributable to climate change.
What are some practical solutions?
There are a number of relatively simple, low cost “cooling” interventions which could be implemented at scale if countries in the global north kept to their funding commitments.
Each year high-income countries make major promises about climate financing, but have yet to deliver. They committed US$100 billion a year in the 2015 Paris Agreement and have delivered only a tiny fraction of that amount.
Low-cost interventions include painting roofs of houses or health facilities with white reflective paint, fans with evaporative cooling, providing cool water for women during labour and making “cooling centres” where women could go during a heatwave.
What can pregnant women and communities do to reduce risks?
On a local level there are behavioural changes that can benefit maternal health. Many pregnant women continue physical work even late in pregnancy, including walking long distances to collect water and firewood. A project in Burkina Faso and Kenya tested a community-mobilisation intervention that aimed to reduce heavy workloads during pregnancy and early motherhood. Results of the project are promising.
Major changes must be made to built environments. The temperatures in many informal settlements are higher indoors than they are outdoors, which can be devastating for expectant mothers. Higher night-time temperatures are especially concerning. Many healthcare facilities are similarly ill-equipped to provide pregnant women with cooler environments.
All the interventions mentioned above can provide some degree of protection against the current level of heat exposure women face, but will be poorly effective against the kinds of temperatures that we will experience in five to 10 years’ time.
We know almost nothing about what could be done to prevent mass mortality events at temperatures around 50-55℃ in settings where air conditioning is not feasible and the population is not accustomed to those temperatures.
Authors
Matthew Cherisch, Associate Professor at the Wits Reproductive Health & HIV Institute, University of the Witwatersrand

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Matthew Chersich receives funding from the Wellcome Trust, US National Institutes of Health and the European Union.
Partners
University of the Witwatersrand provides support as a hosting partner of The Conversation AFRICA.








