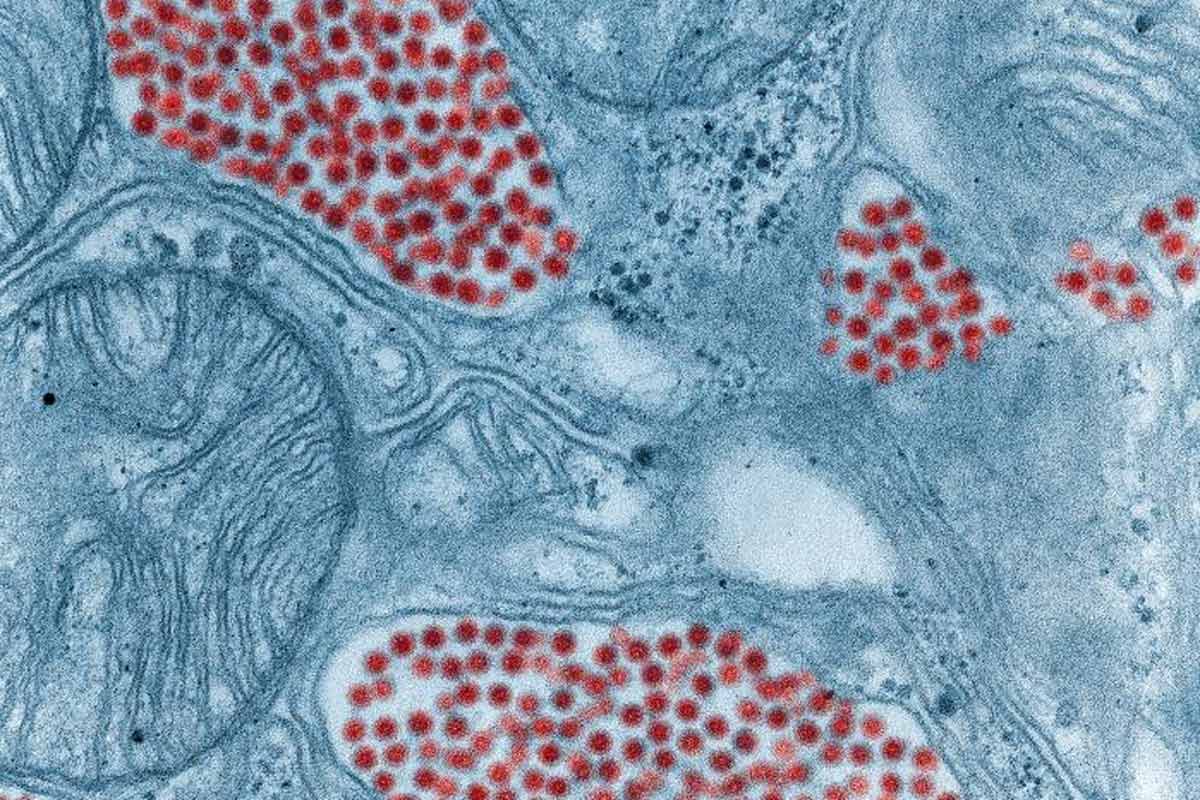
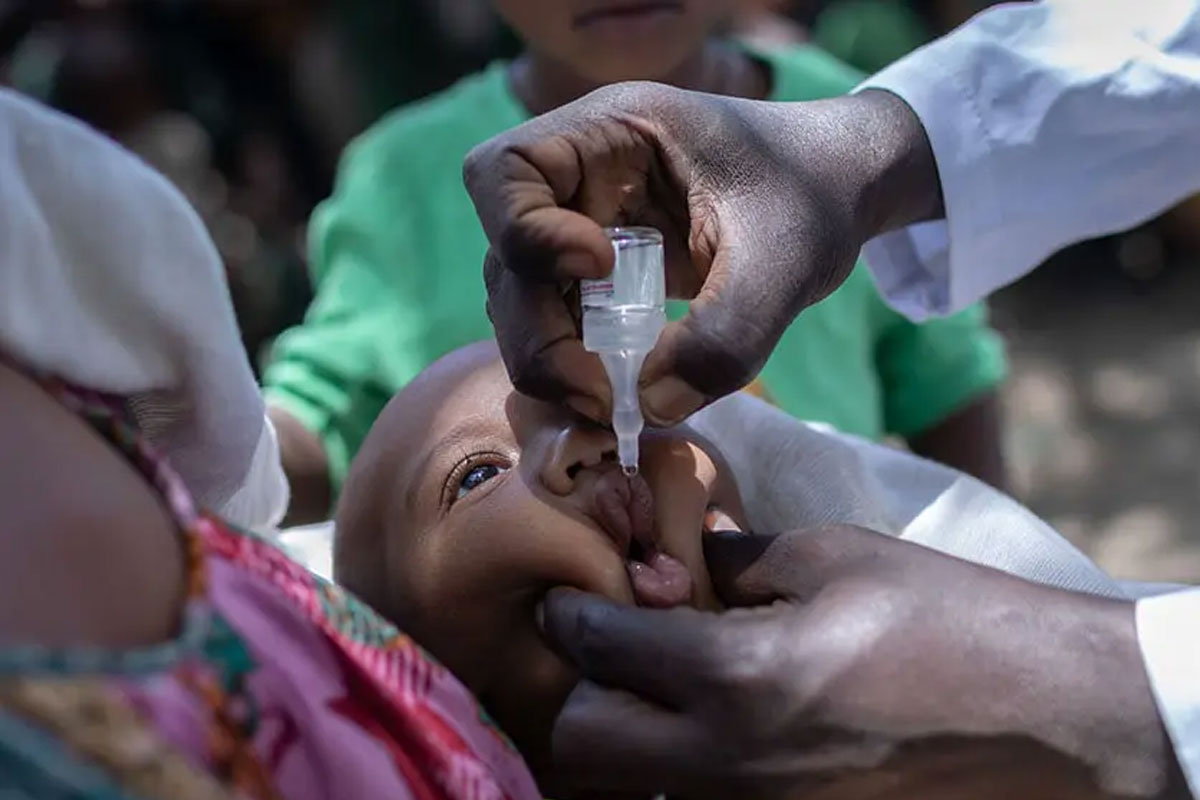
Is altering the dosing strategy of COVID-19 vaccines a good idea?
Uncertainty in the availability of vaccine doses is prompting some countries to consider altering dosing schedules, or mixing different vaccine types. How could this impact the effectiveness of vaccines?
- 7 January 2021
- 6 min read
- by Linda Geddes
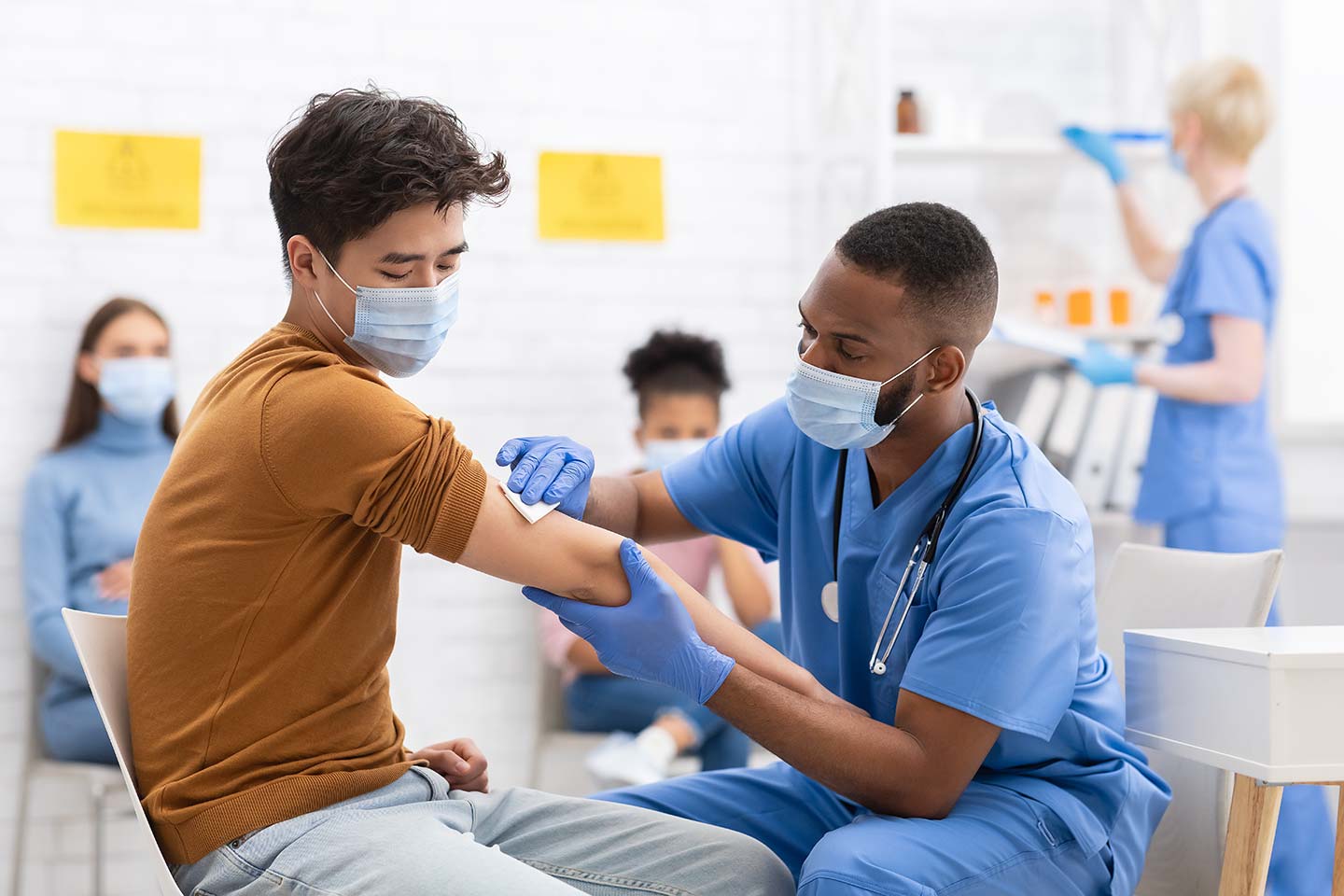
In an ideal world, vaccines would be administered using the same dosing regimen as used in the clinical trials; this is the best way of ensuring that their real-word protection matches the levels observed experimentally. However, until there is adequate global supply of COVID-19 vaccines, the pressing need to vaccinate as many people as possible in the shortest possible time – particularly in countries currently experiencing high rates of infection – means that some countries are considering extending the period between first and second doses, or using a different vaccine to provide the second shot. Already, the UK has decided to stretch the period between the first and second doses of the Pfizer/BioNTech and Oxford/AstraZeneca vaccines to twelve weeks, while Germany and Canada are currently investigating this option.
The UK’s emergency use authorisation for the Oxford/AstraZeneca vaccine allows for this, with the second dose to be administered up to 12 weeks after the first. However, in the US authorisation by the Food & Drug Administration has less flexibility, placing a limit of 28 days for the second dose of the Pfizer/BioNTech vaccine. This position was echoed by the World Health Organization, although it also stated that countries should have leeway to spread doses out over six weeks or so. The UK has also announced that it plans to go even further by mixing and matching vaccine doses from different manufacturers, but only in extremely rare situations, such as if a second dose of the original vaccine isn’t available.
The impact of these strategies hasn’t yet been tested in clinical trials, so it is impossible to say whether it will decrease – or even increase – the effectiveness of those vaccines which have so far only been approved for emergency use. However, given the high level of protection afforded by the first dose of these vaccines, it is possible that vaccinating a greater number of people with a one initial dose will prevent more deaths and hospitalisations than vaccinating a smaller number of people with two doses, provided everyone receives a second dose after 12 weeks.
Two doses are more effective than one.
One thing everyone agrees on is that receiving two doses of the currently available COVID-19 vaccines is likely to be better than receiving just one. For instance, in the case of the Pfizer/BioNTech vaccine, although antibodies against the virus were detected 12 days after the first ‘priming’ dose, the response was stronger after the second dose. The published vaccine efficacy, which shows what proportion of people were protected against COVID-19 disease under trial conditions, was also higher. After the first dose, this was estimated to be 52.4%, compared to around 95% after the second dose – although the efficacy following the first dose appeared to increase as time wore on, hitting 89% after 15 days. Similar patterns were observed with the Moderna and AstraZeneca vaccines.
Have you read?
Vaccines against many other diseases also require more than one dose, including the pneumococcal conjugate vaccine (PCV), which involves a primary series given to infants between six weeks and six months of age, followed by a booster dose at around age 12 months. This is because although the primary series teaches the immune system to recognise the pathogen and leads to the generation of ‘memory cells’ which will rapidly respond if the body encounters the pathogen again, the booster dose strengthens and optimises the duration of that immune response.
Lengthening the period of time between doses
Pfizer has cautioned that its efficacy studies are based on giving two doses of its vaccine 21 days apart – significantly less than the twelve weeks the British government is recommending. The main risk is that people’s level of immunity to the virus declines in the period before receiving their second dose. However, it’s likely that they would maintain some level of protection, which would be boosted when they finally did receive their second shot. Delaying this second ‘booster’ dose by eight weeks is unlikely to have a negative effect on the overall immune response post-boost, according to a consensus statement by the British Society for Immunology (BSI): “We also would not expect any specific safety issues to arise for the individual due to delaying the second dose, other than an increased potential risk of disease during the extended period due to lowered protection,” it added.
For the Oxford/AstraZeneca vaccine, the UK’s Joint Committee of Vaccination and Immunisation (JCVI) pointed to an exploratory analysis which included participants who received a single dose of the vaccine, and found that protective immunity likely lasts for at least twelve weeks – with limited data beyond this point. “With most vaccines, an extended interval between the prime and booster doses leads to a better immune response to the booster dose,” the JCVI said. “There is evidence that a longer interval between the first and second doses promotes a stronger immune response with the AstraZeneca vaccine.”
Mixing and matching vaccines
The UK Government has also stated that a patient’s first and second doses of COVID-19 vaccine could come from different manufacturers and be based on different vaccine types in exceptional circumstances – such as if an additional dose of the first vaccine isn’t available. From an immunological perspective, this should still trigger an effective response, since almost all of the COVID-19 vaccines in development are based on triggering an immune response to the spike protein that the virus uses to gain entry to our cells – even if this antigen is delivered into our bodies using different vaccine platforms. And this strategy of combining different vaccines against the same antigen – known as heterologous prime-boost vaccination – has been deliberately used to boost the immune response against some other pathogens, including the Ebola virus.
Desperate times
Ideally, all of these strategies would first be tested in clinical trials, but the emergence of a highly transmissible coronavirus variant, combined with extremely high case and fatality numbers, and initially limited vaccine supplies in some countries, are far from ideal. The JCVI pointed out that any risks from these actions must be balanced against the risks of allowing the virus to spread through communities at current rates. Even so, it will be important to closely monitor how altering the dosing schedule of these vaccines impacts their efficacy, and to adjust the schedules if necessary.