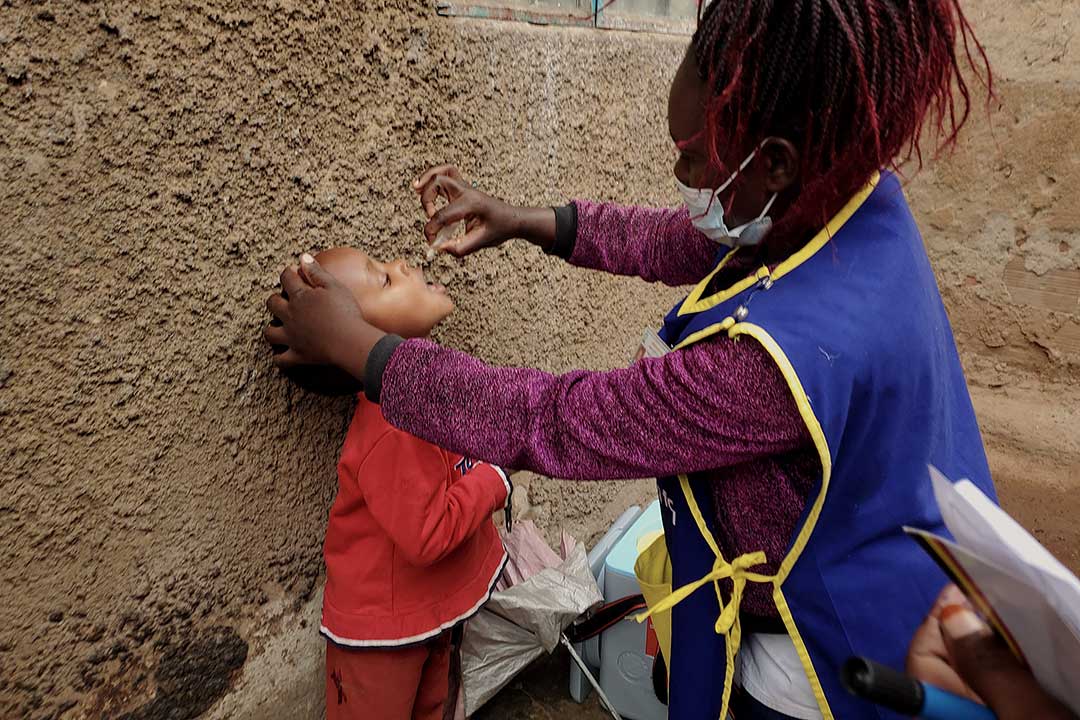
The community health workers getting people vaccinated in Uganda
As Community Health Workers, Harriet Nankwanzi and Yusuf Maganda have built personal relationships with people in their communities who have over the years relied on their services to access vital health information.
- 20 May 2021
- 4 min read
- by Evelyn Lirri

It is a sunny Tuesday morning in Namalumba village, Kamuli District in Eastern Uganda, and Harriet Nankwanzi and Yusuf Maganda have started their day. They move from house to house to give health talks to residents. These days, their talks are mostly about how to prevent COVID-19 and good hygiene practices, as well as offering encouragement to those who are eligible for the vaccine to take the shot.
“My role is to assure the community that the vaccines are safe. And because they trust the information that we give them, they are now willing to be vaccinated,” says 48-year-old Nankwanzi, who has been a community health worker since 2010.
Credit: Evelyn Lirri
As community health workers, Nankwanzi and Maganda have built personal relationships with the people in their communities who have, over the years, relied on their services to access vital health information, including treatment and management of common childhood illnesses such as malaria, diarrhoea, and pneumonia. They also distribute health commodities such as treated bed nets and contraceptives.
With the COVID-19 pandemic, community health workers in Uganda are now playing an additional role, helping the government mobilise the public to get vaccinated.
“I treat children under the age of five for common illnesses and when there are complications, I refer them to the health facilities. I also mobilise parents to take children for immunisation and ensure pregnant mothers attend all their antenatal visits,” explains Nankwanzi.
For many people living in rural Uganda, community health workers are often the first point of contact for health care, serving as a critical link between the healthcare facilities and the communities. They are often selected by members of their community and the role is voluntary.
Have you read?
In Uganda, each village is mandated to have four community health workers, at least two of whom provide integrated case management of childhood diseases. These community health workers are attached to and work closely with the nearest health facilities within their areas of jurisdiction.
“Many people live far away from the facilities, so we have become their first point of care. We have been trained to screen for many of these diseases. I can now easily tell when a child is suffering from pneumonia or malaria. We also have the necessary tools to carry out tests,” says Maganda who has been a community health worker since 2003.
Credit: Evelyn Lirri
But, with the COVID-19 pandemic, community health workers in Uganda are now playing an additional role, helping the government mobilise the public to get vaccinated. Since the first batch of vaccines arrived in the country in March, community health workers like Maganda have been mobilising people in places such as markets, schools, and mosques.
“We are reaching people everywhere with the message. In fact, when people see me with a megaphone these days, they almost know what I am going to tell them,” says Maganda.
Janet Namukwaya, who heads the immunisation programme at Nankadulo Health Centre IV, to which Maganda and Nankwanzi are attached, says community health workers have not only helped in mobilising the public to come for the COVID-19 vaccine, they have also contributed to getting more children immunised against childhood diseases.
“We used to carry out general immunisation once a week, on Thursdays. These days we do it daily, although because most parents are still used to the Thursday schedule they still generally come on that day. We immunise about 50 children on that day, which is still about the same number we used to immunise before the pandemic,” she says.
According to Namukwaya, although the immunisation schedule was affected briefly by the nationwide lockdown imposed at the start of the pandemic in March 2020, they were able to pick up and get all children who were affected to complete their schedules.
“The community health workers helped us to trace these children because they know every child in the village who has been immunised and who has not,” Namukwaya explains.