How Can I Spot A Fake COVID-19 Vaccine?
Fake COVID-19 vaccines erode public trust in much-needed jabs and encourage vaccine hesitancy.
- 2 July 2021
- 8 min read
- by Global Citizen
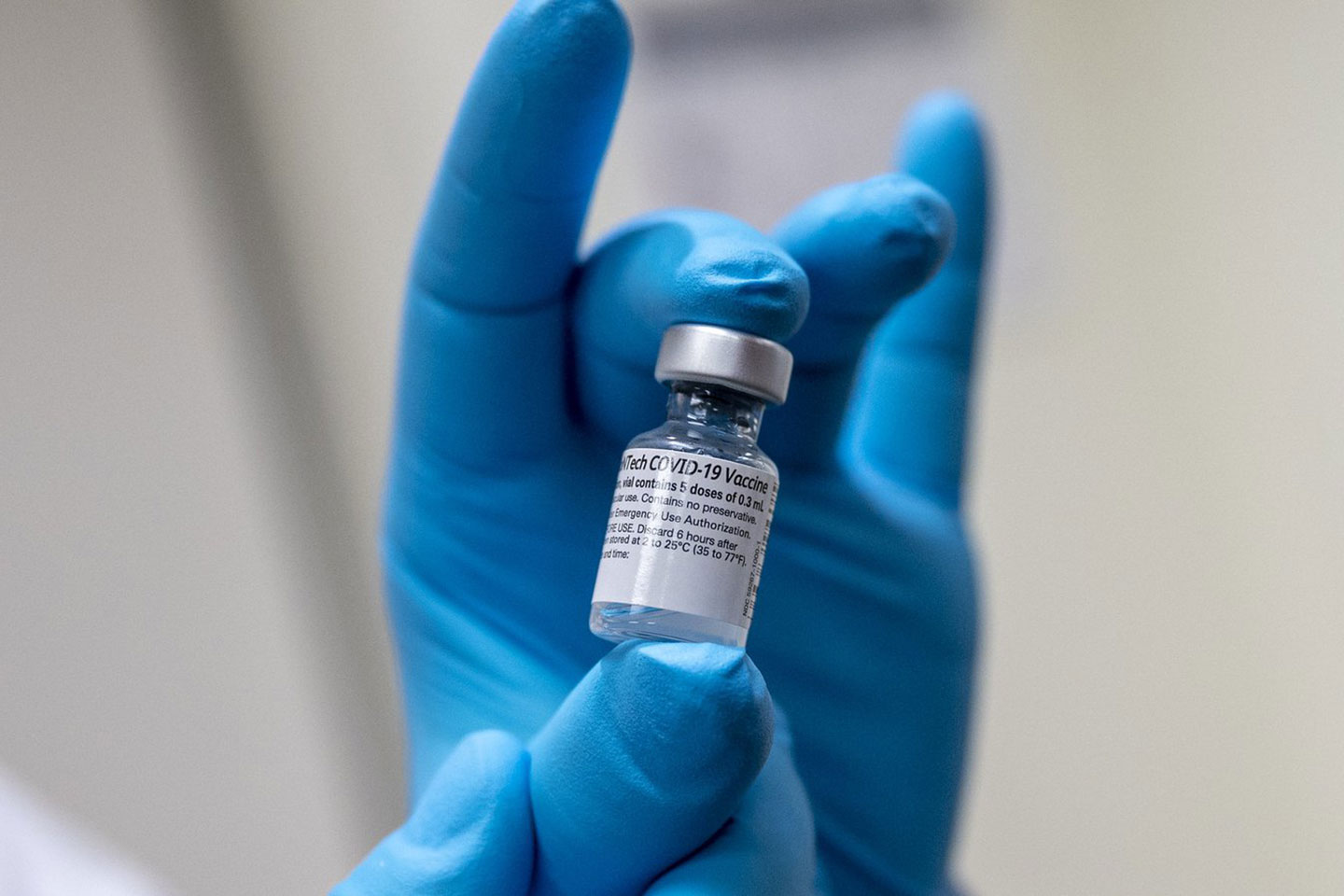
No one likes to be scammed — but fake medication takes that uneasy feeling to another level because counterfeit medicines can kill or cause terrible complications and disabilities.
That is why basically every country in the world has a drug regulation agency to ensure drugs are safe and effective. With medicines, there is no room for error — everything has to be precise and accurate or it could have any number of unintended results.
And while counterfeit medicines are an ongoing problem worldwide, we’ve taken a deep-dive look into the COVID-19 vaccine so you don’t have to. The biggest issue facing COVID-19 and veracity is through the lucrative PPِِِِِِِE market — but we've looked into the drugs themselves.
Thankfully, when it comes to the critical COVID-19 vaccine, only governments and multilateral agencies have access to the limit number of closely monitored suppliers meaning there is little room for bad actors to exploit.
But that can change very quickly if we do not pay attention to the issue of fake medical products and take urgent action — bad actors have already tried to take advantage of the worldwide public health crisis to peddle fake vaccines and PPE materials: more than 80 people have been arrested in China and South Africa with over 5,000 fake COVID-19 vaccine doses seized.
While this is alarming, it is important to put these incidents into perspective, as according to the World Health Organisation (WHO), “...As long as vaccines are supplied through regulated (legal) supply chains, there is very low risk of falsified vaccines and people can be confident they are receiving quality products.”
Counterfeit medicines are not unique to any one region of the world. The WHO says it has received reports of fake drugs in every region of the world and estimates that hundreds of thousands of people die every year from using fake medicines globally.
“Of course, risks do remain, and we continue to monitor the situation, including ensuring that used vials are securely disposed of to prevent them being refilled with fake products. We currently assess the prevalence of fake vaccines to be higher in private and unregulated markets because relatively few vaccines have been supplied to the private sector as yet," Paul Catchick, Head of Investigations and Counter-Fraud at Gavi, the Vaccine Alliance, told Global Citizen.
Have you read?
"The highest risks will likely be in those countries where governments have not secured enough vaccines to meet demand, or where stock mismanagement has created shortages and where people turn to the private sector to protect themselves,” he continued.
4 key facts you should know about fake medicines
- The counterfeit drug trade is worth at least $200 billion worldwide.
- WHO estimates that 1-in-10 medical products in low and middle-income countries are either substandard or falsified.
- Up to two billion people globally do not have access to necessary medicines, vaccines, medical devices and other health products.
- Around 122,000 children die each year on the continent from fake antimalarial drugs, according to an estimate from the Brazzaville Foundation.
How many people does it affect?
Every one of the two billion people worldwide who do not have access to quality and safe medical products, either for social or economic reasons, are at risk of falling prey to the fake medicines trade, says WHO.
Who is most affected, and why?
“No countries remain untouched by this issue — from North America and Europe through to sub-Saharan Africa, South East Asia, and Latin America. What was once considered a problem limited to developing and low-income countries has now become an issue for all,” according to WHO.
However, the body also emphasizes that low and middle income countries (e.g Senegal, Togo, Mexico); people in areas of civil unrest, high insecurity or war (e.g Syria, Yemen, Gaza); and people living in places with weak or non-existent health systems (e.g Nigeria, Benin), suffer the biggest impact of this issue.
WHO estimates that 42% of the world's reported cases of fake pharmaceuticals were found in Africa between 2013 and 2017. Also, it is illegal to sell medicines outside a pharmacy or medical institution in many countries, although these laws are rarely enforced.
High poverty rates, insecurity and inability to access safe and affordable medical services are among the leading causes that drive people in these areas toward counterfeit medicines which, by nature, are designed to look like approved medicines.
What impact is it having on people’s lives?
When it does happen, being given fake medication can have a devastating toll on people’s lives.
Amele Louise Assogba, a 49-year old Togolese cook and mother of four, told The Washington Post in January 2020 she ended up in a hospital and needed blood transfusion after purchasing a substandard remedy for a flu. She explained that drugs at pharmacies cost three times more.
“I needed to save money for my children,” Assogba said.
Apart from the hundreds of thousands of people who die every year, many other people suffer varying complications and the diseases they are taking medication for might also not be taken care of.
In the climate of COVID-19, where some place an even higher significance on the vaccine, international authorities are working even harder to ensure doses are verified.
“Fake vaccines pose a danger to people's health. They may even contain harmful ingredients which can directly cause illness or death. Even if they are not contaminated, fake COVID-19 vaccines may give people a false sense of security whereby they assume they are protected when in fact they remain at heightened risk of getting and spreading the virus,” said Catchick.
“Furthermore, it can take a while to realize a fake vaccine has been administered, which can increase the risk of someone with asymptomatic COVID spreading the virus. Fake vaccines also erode trust in legitimate vaccines and vaccination programmes, and place an additional burden on health systems which are already stretched by the pandemic.”
But tracking and stopping fake medicines is not the most straightforward thing and requires huge effort amongst countries and global bodies alike.
“Assessing the harm caused by substandard and falsified (SF) medical products is complex and difficult. In the case of falsified vaccines, the socio-economic and public health harm includes loss of trust in public organizations. It is important to stress that any harm caused by a falsified vaccine does not reflect any safety failure of an authentic / genuine version. Genuine vaccines which have been subject to regulatory approval are considered to be safe, efficacious, and quality assured,” says WHO.
How does it impact on the mission to end extreme poverty and systemic causes of extreme poverty?
The global counterfeit drug trade is worth $200 billion and has been linked to funding all kinds of nefarious activities including terrorism. In 2017, Interpol seized more than 41 million fake pills worth more than $21 million at the time.
Also, when people are having complications from using fake medicine or illnesses they are trying to cure remain, their quality of life is reduced and their ability to fend for themselves or their loved ones is compromised.
This problem has considerable socio-economic impact by contributing to losses in productivity, wasted resources and increased expenses for individual and national health systems.
Who are the key players in tackling the issue?
“In an increasingly globalized world, no one country has sufficient resources and capacity to deal with this issue in isolation,” says WHO, as part of its effort to build momentum behind the required global strategy to tackle sham medicines.
The global health body also launched the Global Surveillance & Monitoring System for Substandard & Falsified (SF) medical products in July 2013. “It’s objective is to work with WHO Member States in improving the quantity, quality and analysis of accurate data concerning SF medical products, and to use that data in the better prevention, detection and response to those products, in order to protect public health,” according to WHO.
Interpol also works with the police in many countries to track and dismantle illegal drug-making operations across the world. The United Nations and many other global bodies also work together to tackle the issue as well as journalists, activists, social welfare organizations and other individuals.
What action can we all take against it?
Education is the first action towards tackling counterfeit medicines that anyone anywhere in the world can take. When you know what to look out for and how to spot fake medical products, you can teach other people and so on.
A good start is the “six Ps” of identifying fake medicine, according to Interpol:
- Place: Do not buy medicines from unknown websites or in a marketplace, for any reason. Buy medicines only from licensed suppliers whose authenticity is verifiable.
- Prescriptions: Only buy medicine that has been prescribed by your doctor or healthcare professional.
- Promises: Watch out for false promises like “cures all types” of a major illness, “money-back guarantee”, “no risk” or “limited supply – buy in advance”.
- Price: Compare the price with products you usually buy. If it is much cheaper, it is likely to be a fake.
- Privacy: Interpol says the trade in fake medical products has also been linked to credit card fraud and identity theft. Do not reveal any personal information beyond appropriate medical details.
- Product: A medicine is fake if: it contains too much, too little or any different ingredients; claims to have different properties or side-effects; is not correctly labelled or not labelled at all; has an out-of-date or missing expiry date; does not contain information on how to store the medicine; the packaging looks poorly made or looks tampered with; there are spelling or grammatical errors on the packaging or instructions.
PARTNER CONTENT
Originally published by Global Citizen on 24 June 2022
Fake medical products have been described by WHO as “one of the urgent health challenges for the next decade” so it is important that we all do our part. You can also join Global Citizen to take action toward ending the pandemic here.