How COVID-19 led to devastating rises in malaria
The fight against the killer disease has nearly halved malaria deaths since 2000, but now that hard-won progress could be lost because of the pandemic.
- 7 December 2021
- 3 min read
- by Priya Joi
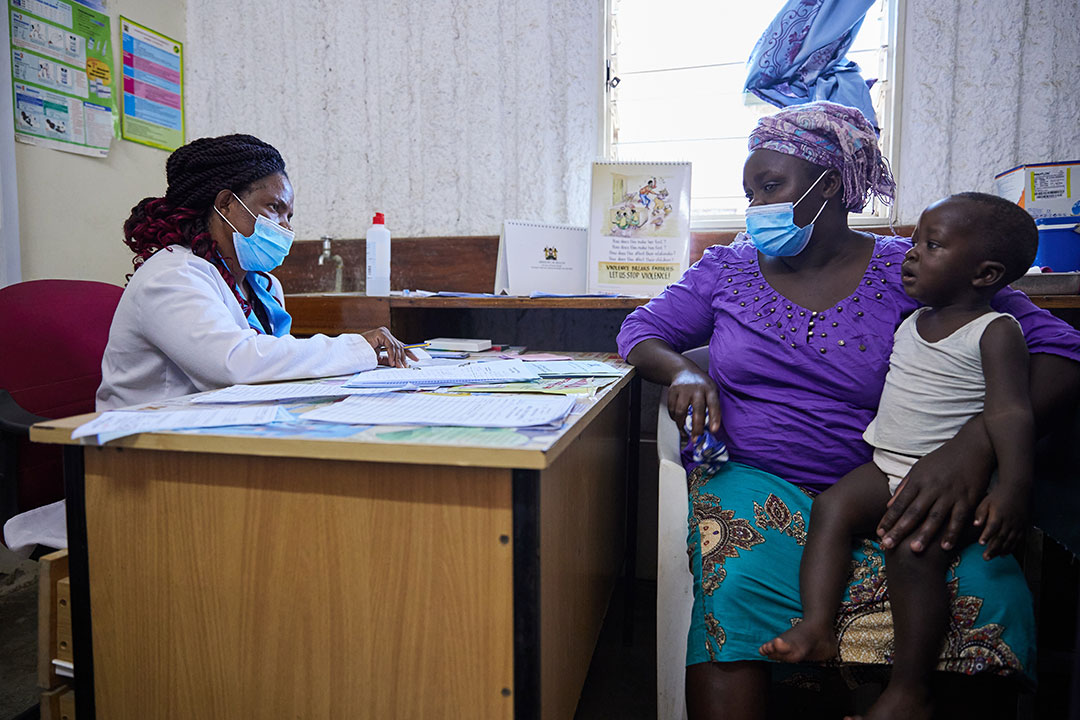
The COVID-19 pandemic has caused significant collateral damage in many other areas of health, from emergency surgery to disease prevention. Lockdowns and supply chain issues disrupted routine immunisation and cases of infectious diseases such as malaria, HIV/AIDS and TB have gone up significantly.
Ultimately, to resurrect the fight against malaria in lower-income countries, COVID-19 also needs to be quelled.
The world had made significant progress against these major killers over the past few decades, yet these gains could be lost unless the global focus is brought back from solely COVID-19, warn experts. In some countries “the knock-on effects on HIV, TB and malaria could exceed the direct impact of COVID-19”, said the Global Fund’s chief Peter Sands.
Of the three diseases, malaria services continue to experience the highest level of disruption according to data from the Global Fund. The World Health Organization (WHO) 2021 World Malaria Report published this week (1 December) demonstrates how cases have soared since the COVID-19 pandemic started in early 2020 and calls for efforts against malaria to be reinvigorated.
In 2000, nearly 900,000 people died of malaria. By 2019 this had fallen to 558,000. But there was a significant jump in 2020, when 627,000 died. WHO says that around two thirds of the additional deaths (around 47,000) were linked to disruptions in the provision of malaria prevention, diagnosis and treatment during the pandemic.
Disruptions to malaria prevention and care
Reporting earlier this year on progress in eliminating malaria, WHO said that from the start of the pandemic “governments diverted human and financial resources away from national malaria programmes to tackle COVID-19; in some cases, nearly all national malaria programme staff were detailed to the pandemic”.
Many countries responded to the pandemic by introducing lockdowns, mobility restrictions and stopping the movement of goods. This meant that health workers were unable to carry out malaria measures such as the provision of insecticide-treated bednets and the spraying of insecticides in homes, and people were unable to travel to health centres for preventive antimalarial treatment, or for diagnosis and treatment when they suspected they had malaria. Sometimes, even when people were able to travel to clinics, they were unwilling to for fear of becoming infected with COVID-19.
In countries like Botswana, sharp spikes in malaria cases were seen in 2020 as people moved en masse from urban to rural areas in anticipation of lockdowns.
Have you read?
Adapting malaria elimination approaches
Some countries managed to adapt malaria prevention strategies to respond to the disease in the midst of crisis, including Eswatini, which began conducting malaria case investigations by telephone after mobility restrictions stopped teams from going to the field.
Meanwhile, Benin adapted its insecticide-treated nets mass distribution campaign to one with a ‘no touch’ payment for campaign workers. The national strategy switched from a fixed-point collection to a door-to-door-distribution procedure. This outreach approach allowed health workers to offer community health education on COVID-19 as well.
Tackling COVID-19 to be able to fight malaria
Getting on top of malaria and other major killers will mean thinking in new ways to ensure the services continue to reach the millions of people who need them. The rollout of the new malaria vaccine that Gavi’s board has just approved funding for will help to save lives. But it still needs to be accompanied by other interventions, such as bed nets and chemoprevention. Ultimately, to resurrect the fight against malaria in lower-income countries, COVID-19 also needs to be quelled.









