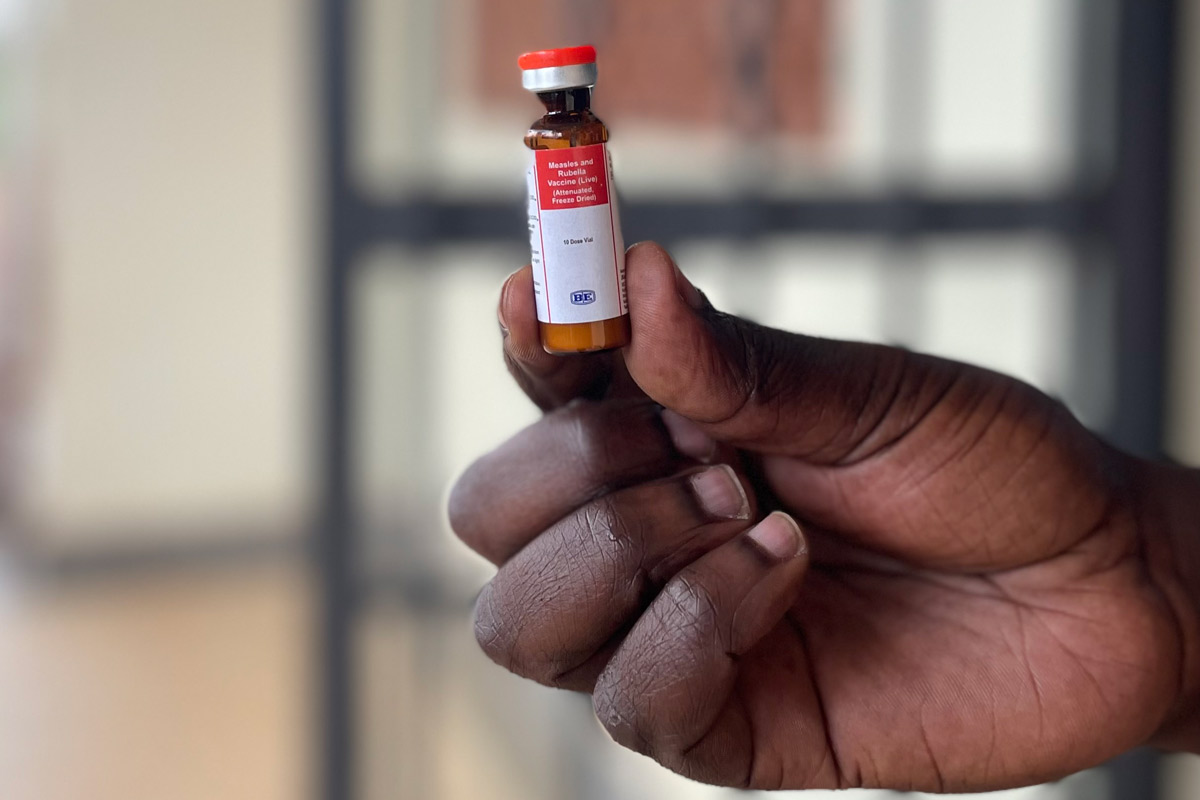
How Uganda’s immunisation programme helped reduce child mortality
In Uganda in 2011, 90 children out of every 1,000 live births died before their fifth birthday. Today, that figure has dropped to 52 – and health leaders say vaccination has been key to the change.
- 5 January 2024
- 8 min read
- by John Agaba
Stella Nanyonga slipped on a pair of blue nitrile medical gloves and opened the vaccine carrier – a small, insulated container lined with coolant packs to keep drugs and diluents cold.
She picked up a vial containing a vaccine against diphtheria, pertussis, tetanus, hepatitis B and haemophilus influenzae type B out of the container, and shook it methodically before drawing the drug into a syringe. She turned to a waiting mother and child, and swiftly, smoothly, injected the baby.
“While we have many other factors (that have contributed to falling child mortality), vaccines have been key… vaccines, and our robust immunisation programme.”
– Dr Diana Atwine, permanent secretary at Uganda’s Ministry of Health
Nanyonga – who is an enrolled nurse at the Mulago Specialised Women and Neonatal Hospital in Kampala – further inoculated the baby against polio, rotavirus diarrhoea and pneumococcal pneumonia.
She issued some advice to the mother: should the baby develop a temperature later, undress the child and wipe it with a wet towel. Then it was the next child's turn.
At another health facility, about 10 kilometres west of Kampala, enrolled midwife Lonette Kiconco snapped on her gloves and inoculated newborns with BCG vaccine, to help protect them from deadly tuberculosis.
These health workers number among the approximately 7,000 nurses who help to vaccinate children and protect them from several vaccine-preventable diseases (VPDs) at 6,937 health centres across Uganda's 135 districts. They constitute a nationwide safety net.
"Vaccines have helped us to stop some of the deadliest childhood diseases," Kiconco told VaccinesWork. "They have helped us to reduce child mortality."
More survivors
A new report by the Uganda Bureau of Statistics shows the East African country has reduced child deaths among under-fives from 90 per 1,000 live births in 2011, to 52 per 1,000 live births today, in significant part due to expanding vaccine coverage.
In the same period, the number of children dying before their first birthday dropped from 54 per 1,000 live births to 36 per 1,000 live births.
"While we have many other factors (that have contributed to falling child mortality), vaccines have been key… vaccines, and our robust immunisation programme," said Dr Diana Atwine, permanent secretary at Uganda's Ministry of Health, in an interview with VaccinesWork.

Credit: Emmanuel Ainebyoona
Despite pandemic setbacks, between 2011 and 2022, official statistics show a gentle increase in the number of 12- to 23-month-old children fully vaccinated with >all of the recommended routine immunisations. In the same period, coverage for >DTP3, given to protect against diphtheria, tetanus and pertussis, increased from 82% to 89%, according to WHO and UNICEF data.
Dr Atwine singles out rotavirus immunisation as a strong example of life-saving impact. The vaccine, which protects against the leading cause of severe infectious diarrhoea in children, began rolling out in 2018. By 2023, Uganda had achieved 85% coverage with the second dose of the vaccine. The effect on mortality was evident: where 465 children were recorded as having died of severe diarrhoea in 2015, that number had dropped to 284 in 2022. In the first 10 months of 2023, diarrhoea had claimed 172 lives.
Ramping up vaccination
In 1987, when Uganda re-launched and ramped up its immunisation programme, coverage rates across the country stood at an estimated 34%.
Over time, not only coverage rates, >but the number of disease Uganda vaccinated has grown. In 1987, the number of vaccines on offer was six. Today, Uganda vaccinates against 13 diseases, including polio, measles, pertussis, tetanus, diarrhoea and diphtheria, plus tuberculosis and haemophilus influenzae type B. Further antigens in its arsenal of protection include rabies, meningitis, hepatitis B, yellow fever and cervical cancer.
"Vaccines support the body's immunity to fight off diseases," Atwine told VaccinesWork. "So, (by increasing the number of VPDs) we wanted to protect as many children (and adults) as we could from these VPDs."
"Our target is to vaccinate every child who is born in Uganda to give them protection," said Atwine, "but we also know that when sufficient percentages of the population are vaccinated, the few children who, for one reason or another miss out on immunisation, are somehow protected."
This ultimately reduces the rate of these VPDs circulating in the population, said Atwine. "It is the reason you don't hear of diseases like polio, diphtheria or whooping cough in Uganda today."
Dr Alfred Driwale, an immunisation consultant in Kampala, has said that Uganda's vaccination programme has halved child mortality from VPDs, crediting a committed leadership that understands the importance of immunisation.
That has required pushing against the tide. To expand its proportional reach, the immunisation programme has needed to outpace one of the world's fastest growing populations.
"This has enabled us to improve our DTP3 coverage from about 70% to over 90% in the last decade," said Dr Rita Atugonza from the Vaccines and Immunization Division at the Ministry of Health.
Filling gaps
Uganda had been one of the first countries on the African continent to eradicate smallpox, and the Uganda National Expanded Program on Immunisation (UNEPI) was created in 1983. But challenges remained. Political and civil conflict in the early 1980s saw the vaccination programme stall and coverage rates drop. 1987's relaunch was a shot in the arm for the programme, but funding was still scarce, human resources lacking, and the cold chain remained patchy.
Uganda's porous borders with the Democratic Republic of Congo, South Sudan and Kenya also exposed the country to circulating vaccine-preventable diseases.
To address persistent gaps, the Ministry of Health developed the comprehensive immunisation policy in 2012.
"The policy aimed at reducing childhood and maternal mortality and disability rates due to VPDs," said Atwine. "It aimed at improving safety and effectiveness of vaccines in procurement, transportation, storage and administration." It also aimed at improving research, surveillance and community involvement in immunisation services in the country.
"We started by engaging political leaders at national and district levels to mobilise resources and rallied village health teams, religious and cultural leaders and other community-based organisations to improve immunisation services," Atugonza said.
"We worked with partners to establish a sub-national logistics management information system and expand our cold chain system at national, district and health facility levels to reach services to communities."
The ministry also developed a communications strategy, including tools like emails, social media and bulk small messaging to create awareness and address myths, rumours and negative attitudes towards immunisation.
Have you read?
It rolled out preventive and responsive mass vaccination campaigns and implemented Integrated Child Health Days – usually in the months of April and October – to inoculate children who may have missed out on immunisation, she said.
These initiatives have enabled Uganda to improve its routine immunisation coverage and lower its child mortality.
Eyes on "zero-dose" kids
Ministry of Health records show that as of October 2023 coverage rates with the third dose of DTP3 stand at more than 90%. This is the same for the first dose of measles rubella vaccine, the inactivated polio jab, the third (and final) dose of pneumococcal conjugate vaccine, and the third dose of oral polio vaccine. Coverage rates for BCG and rotavirus 2 each stand at more than 80%.
But the country can do more. The programme means to reduce the number of totally unvaccinated children – currently estimated to be about 3% of the total – by 50% in the next five years.
That calls for a close review of health facility immunisation data to identify and prioritise areas with the highest numbers of so-called "zero-dose children".
"Each situation is different," said Atugonza, when asked why pockets of undervaccinated kids persist. "We have myths and misconceptions about vaccines fuelled by social media that are causing vaccine hesitancy (in towns, for instance) and then we have emerging resistance (to vaccines) by religious sects and certain communities.
“Our target is to vaccinate every child who is born in Uganda to give them protection, but we also know that when sufficient percentages of the population are vaccinated, the few children who, for one reason or another miss out on immunisation, are somehow protected.”
– Dr Diana Atwine, permanent secretary at Uganda’s Ministry of Health
"We have upped our advocacy campaigns to address these misconceptions and want to address the specific reasons some parents do not take their children for immunisation," she said.
She said the programme is supporting village health teams, local councils and other local leaders who are the "frontline mobilisers for routine immunisation" to create awareness about the importance of immunisation.
"We want to put all our efforts into reaching these children," Dr Michael Baganizi, UNEPI's programme manager, said earlier this year. "We want to understand what is stopping them from seeking immunisation, and the barriers stopping us from reaching them."
"We have a lot of hard-to-reach areas, gender-based violence issues, and other challenges," said Baganizi. "But we will come up with customised interventions. We need to reach every child."
Next chapter
The planned introduction of a malaria vaccine will reduce child mortality even further, said Baganizi. Malaria is one of the leading killers of under-five children in the country.
Immunisation against VPDs remains a crucial contributor to the reduction and maintenance of low infant and child mortality in Uganda, said Atwine.
"With the current total fertility rate at 5.2, we have lots of children born every year who will require immunisation, to ensure their survival and to maintain the gains made in our overall health indicators," she said.
"Our vision is a population free of VPDs," said Atwine. "We want to ensure that every child and high-risk group is fully vaccinated with high quality and effective vaccines against the target diseases."