Ivermectin: why a potential COVID treatment isn’t recommended for use
The antiparasitic drug was thought to be a potential treatment for COVID-19, but there isn't sufficient evidence to recommend its use, despite widespread support online.
- 22 April 2021
- 5 min read
- by The Conversation
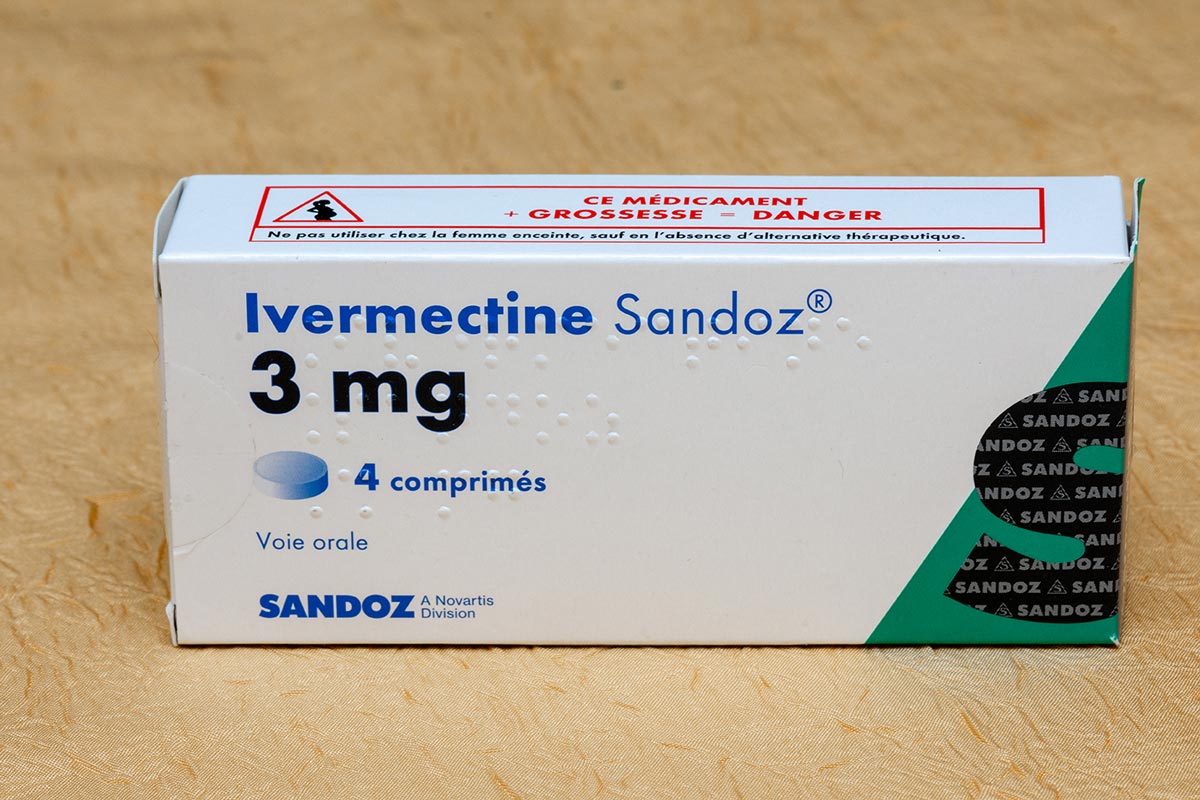
As the search continues for treatments for COVID-19, the results from a number of studies have led to changes in the advice on which drugs to give people who are suffering from the disease.
The European Medicines Agency and the United States National Institutes of Health have recently stated that one previously promising treatment – the antiparasitic drug, ivermectin – is not recommended for use in routine management of COVID-19 patients.
Despite these decisions, support for ivermectin has been circulating on social media and in WhatsApp groups, with rumours abounding that the drug is being blocked on purpose. Some have dubbed it the “new hydroxycholoroquine”, after a treatment that received a significant amount of online support but was found in trials to be ineffective against COVID-19.
So what is ivermectin, and why have national agencies ruled against it?
What is ivermectin?
Ivermectin was first developed in the 1970s from a bacterium in a soil sample collected from woods alongside a Japanese golf course (no other source has ever been found).
In the intervening years, the effectiveness of ivermectin and its derivatives in treating parasitic worm infections transformed human and veterinary medicine, leading to a Nobel Prize for its discoverers, William C Campbell and Satoshi Ömura.
In humans, ivermectin is currently prescribed in tablet form to treat certain roundworm infections that cause illnesses such as river blindness. It may also be applied as a cream to control the common inflammatory skin condition papulopustular rosacea.
But ivermectin is most commonly used for veterinary parasitic diseases, especially gastrointestinal worm infestations. Consequently, it is readily available and relatively inexpensive.
Have you read?
As ivermectin is more extensively used in veterinary than human medicine, however, the US Food and Drug Administration found it necessary to issue a warning in April 2020 against use of veterinary preparations in human patients with COVID-19.
Why might it be used to treat COVID?
How did a drug mainly used to treat intestinal parasites in cows come to be of interest to doctors treating humans with COVID-19?
In early 2020, a paper was made public (before it was reviewed by other scientists) which showed ivermectin suppresses the replication of the SARS-CoV-2 virus, which causes COVID-19, under laboratory conditions. This was one of many studies over the past 50 years to show that the antiparisitic drug could also have antiviral uses.
There appear to be two key ways in which the drug could prevent coronavirus replication. First, it could prevent the virus from suppressing our cells’ natural antiviral responses. Second, it’s possible the drug prevents the “spike” protein on the surface of the virus from binding to the receptors that allow it to enter our cells. Along with the anti-inflammatory actions apparent from ivermectin’s efficacy in rosacea, these may point towards useful effects in a viral disease that causes significant inflammation.
These initial findings were used as the basis of numerous recommendations for ivermectin’s use to treat COVID-19, particularly in Latin America, which were later retracted.
Why is it controversial?
Since then, there have been numerous studies into ivermectin as a potential treatment for COVID-19.
In late 2020, a research group in India was able to summarise the results of four small studies of ivermectin as an add-on treatment in COVID-19 patients. This review showed a statistically significant improvement in survival among patients who received ivermectin in addition to other treatments.
But the authors stated clearly that the quality of the evidence was low and that the findings should be treated with caution. As is frequently the case for reviews of multiple small studies, the paper suggested that further trials were needed to determine whether ivermectin was indeed clinically effective.
A controversy subsequently blew up over an article by the Front Line COVID-19 Critical Care Alliance, a group of doctors and researchers that lobbies for the use of ivermectin.
This article, summarising multiple small studies of the effects of ivermectin on COVID-19 patients, was provisionally accepted for publication in the journal Frontiers in Pharmacology in January 2021 but then rejected and removed from the journal’s website in March. The journal’s editor stated that the standard of evidence in the paper was insufficient and that the authors were inappropriately promoting their own ivermectin-based treatment.
One larger randomised clinical trial was published in March 2021. This showed no effect of ivermectin on duration of symptoms of adults with mild COVID-19. The authors stated that the findings did not support the use of ivermectin in these patients, but again highlighted that larger trials were needed to determine whether the drug had other benefits.
Why isn’t it recommended?
While some other studies did appear to show benefits of ivermectin, many did not. These were summarised by the National Institutes of Health, showing severe limitations arising from small sample sizes and problems with study design.
Both the National Institutes of Health and the European Medicines Agency judged, on the basis of these studies, that there is currently insufficient evidence to support the use of ivermectin in treatment of COVID-19.
More studies are underway. A large, multicentre trial began in February to determine the effectiveness of ivermectin as well as metformin (an anti-diabetes medication) and fluvoxamine (an antidepressant) in preventing COVID-19 disease progression.
It would therefore be premature to conclude absolutely that ivermectin has no place in COVID-19 treatment. On the basis of current evidence, however, its use cannot be recommended.
Authors
Gordon Dent
Senior Lecturer in Pharmacology, Keele University

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Gordon Dent does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
Partners

Keele University provides funding as a member of The Conversation UK.








