Primary health care: a postcard from 2030
What would a future in which we’ve achieved Universal Health Coverage look like, and how do we get there?
- 19 January 2023
- 5 min read
- by Juan Pablo Uribe , Daniel Dulitzky
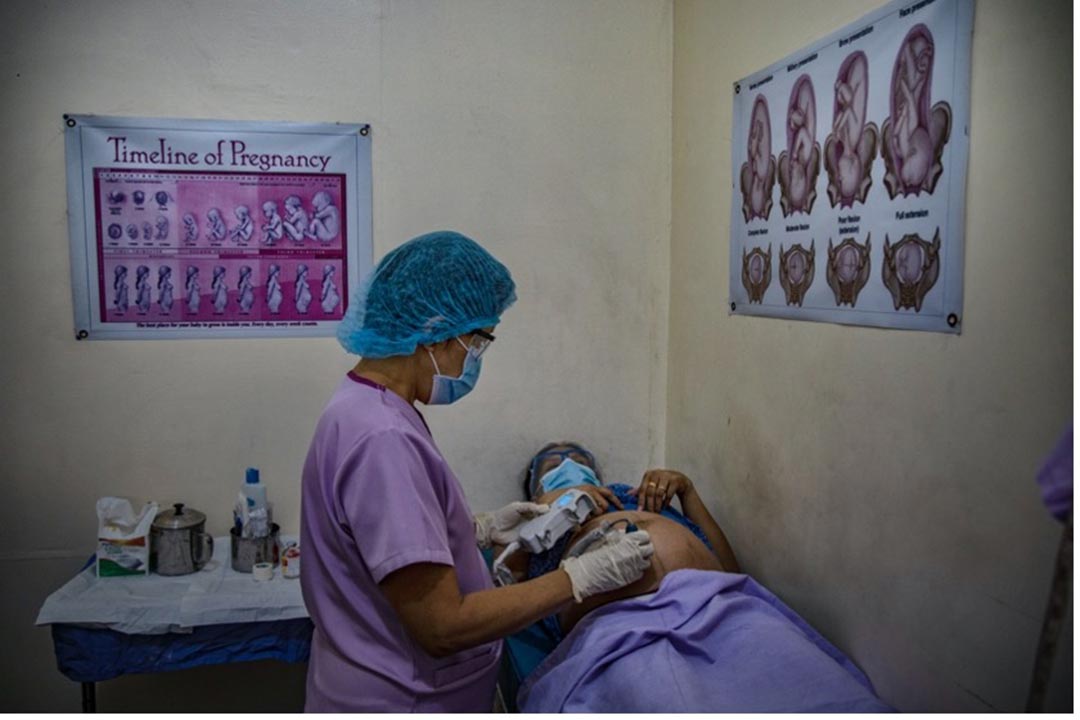
Picture this: it is the year 2030, and leaders at the the United Nations are discussing progress against the Sustainable Development Goals. A standout success is Goal 3 – Health.
Despite the major social and economic setbacks facing governments following the COVID-19 pandemic between 2020 and 2023, almost all countries report that they have reached Universal Health Coverage. This is, unmistakably, a monumental achievement.
We designed health financing around people’s immediate health needs and we prioritised addressing inequalities. To support this, we not only mobilised additional public funding, we also allocated funding more efficiently.
For the first time, every person on the planet can get the health services they need, no matter where they live, and without being put into financial hardship. The benefits will reverberate throughout humanity for generations.
Smiling, the UN Secretary-General approaches the dais, and she begins to outline a few of the notable challenges that were overcome to bring the world to this moment. Here are some of her reflections:
Putting people at the centre
It seems obvious now, but perhaps the most profound thing we did was put people at the centre of primary health care.
Not enough resources were going to community-based health providers and people had stopped using them. This affected the availability and quality of human resources, medicines and medical supplies. It was a vicious cycle: underfunded health services were poor quality health services. Fewer people used them and so governments stopped funding them, pushing resources to higher levels of care where service delivery was generally not cost-effective. In the end, people were not receiving the right care at the right time.
We were able to reset and rebuild a system with a people-centred focus. We prioritised people's experience with health services so that the care provided to them was the care they needed at that moment. This fundamental shift led to a more comprehensive, fully resolutive, primary health care system that earned confidence, trust and support from communities who recognised that it addressed most of their health needs.
Investing in primary health care
Another crucial step was to change the way primary health care was funded, particularly given that many countries did not have enough money to properly fund community health services. We knew we had to invest more and we had to invest better.

Credit: World Bank
We designed health financing around people's immediate health needs and we prioritised addressing inequalities. To support this, we not only mobilised additional public funding, we also allocated funding more efficiently. This way, we were able to ensure there was sufficient money available for people to receive primary health care services equitably and free at the point of use. We also incentivised health providers to focus on continuity of care for the populations they serve.
Focusing all stakeholders on primary health care
Finally, we championed an approach that made effective primary health care delivery the focus of stakeholders across government, public service, civil society, the private sector and donors.
When all the key health actors collaborated on the design and implementation of the new system it was inherently more focused on the people it was set up to help. Each stakeholder brought valuable expertise and perspectives to the process, and together formed a powerful and much needed support network for the community health workforce who continued providing for their patients every day.
Have you read?
We embraced health service delivery and financing as a political exercise that could benefit from long term commitment and leadership, even when fiscal space was challenged due to the double burden of the pandemic. The ministries of health and finance worked collaboratively to ensure a higher share of government spending went to health services, and particularly to primary health care. Technical agencies and academics played an important role in researching, collecting and reporting health care output and expenditure data, which encouraged evidence-based policymaking.
The importance of primary health care has been recognised since the 1970s and its scope has evolved considerably over the last 50 years. Recently, our team brought together health officials from 19 countries for The Asia and Pacific Health Financing Forum a valuable opportunity to learn more about the innovations being implemented by countries across the region and develop a deeper understanding of the challenges being faced.
The World Bank has long been committed to helping low and middle-income countries build stronger, more resilient health systems and provide quality, affordable health services to everyone. Our $34 billion global health portfolio includes over 240 projects that help countries take a comprehensive approach to improving health outcomes, especially for poor and vulnerable people, by strengthening primary care and key public health functions. This includes investment in quality service delivery models that are fit for remote areas, expanded accountability mechanisms, and deploying strategies that encourage equity, efficiency, and financial protection.
If this 2030 future is to be possible, we need to make sure the foundational role primary health care plays in our health systems is acknowledged and appropriately financed.
Let's get moving.
The Asia & The Pacific Health Financing Forum was co-hosted by the World Bank, Australia's Department of Foreign Affairs & Trade, the Global Financing Facility, and the US Agency for International Development with support from the Advance UHC multi donor trust fund, Global Fund, the Joint Learning Network, the Global Alliance for Vaccines & Immunization, and the Bill & Melinda Gates Foundation.
Daniel Dulitzky is the Regional Director, Human Development, East Asia and the Pacific Region at the World Bank.
Juan Pablo Uribe, MD, is the Global Director for Health Nutrition and Population at the World Bank and Director of the Global Financing Facility for Women Children and Adolescents (GFF).
More from Juan Pablo Uribe
Recommended for you





