Seven things countries have done right in the fight against COVID-19
There has been a huge variation in how countries have responded to COVID-19. Whilst some have imposed strict lockdown measures, others have avoided tight restrictions. But what works best?
- 22 June 2020
- 5 min read
- by Ciara McCarthy
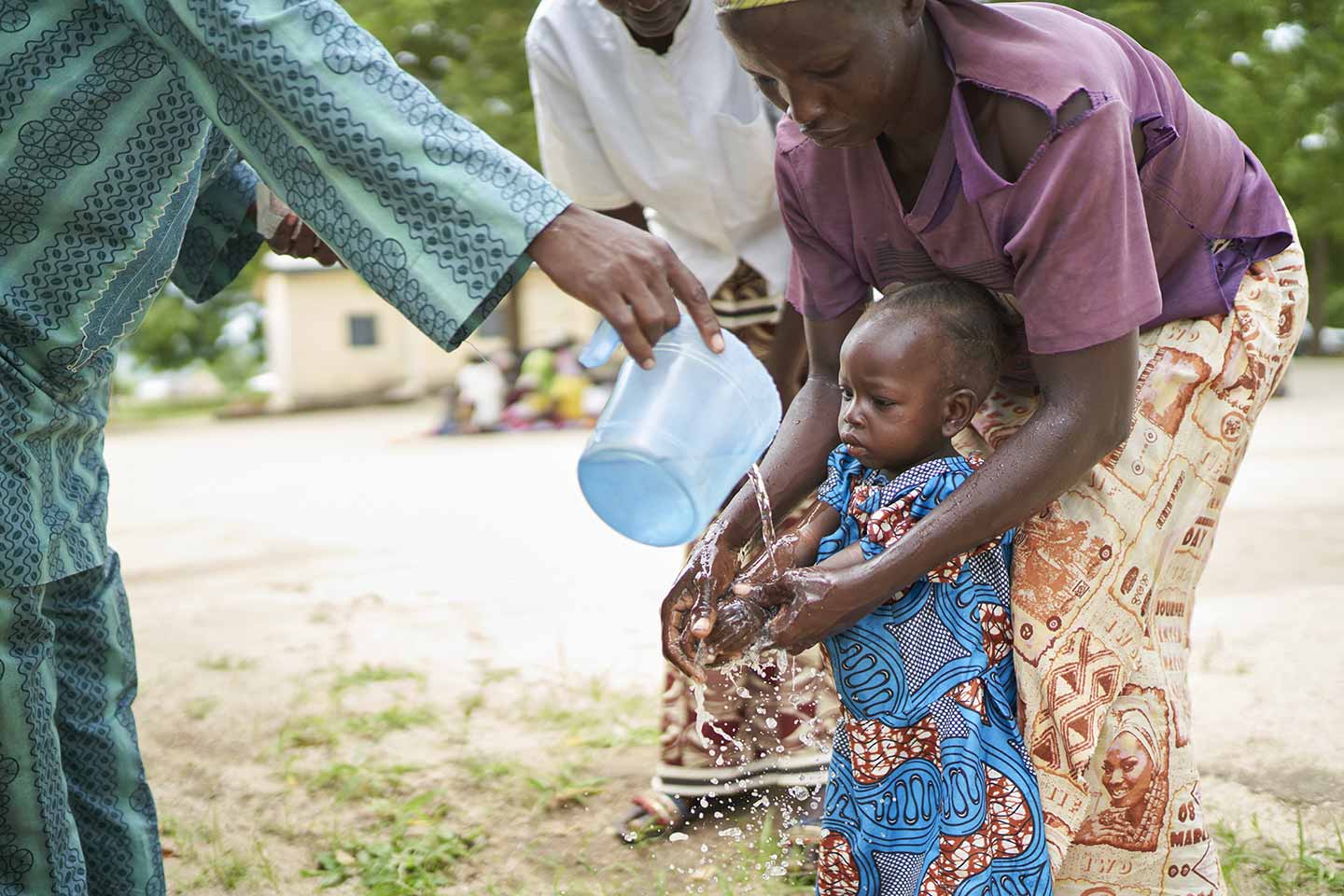
Analysing the varied global response to the COVID-19 pandemic and identifying measures that have worked best will no doubt occupy scientists from years to come, but there are a few strategies that already seem to be coming out on top.
1. PHYSICAL DISTANCING
One of the main strategies used worldwide has been physical distancing, either through advising people to keep a distance of 1-2 metres from people they don’t share a home with and the cancellation of large events, to the closure of shops and restaurants, and asking everyone to stay at home. There is increasing evidence that these measures do work and have saved thousands of lives. It is critical though that they are used in conjunction with hygiene and sanitation measures, such as handwashing and disinfection. However, others argue that lockdowns are not the solution in themselves but a means of buying time so that other measures can be scaled-up. The vast majority of people remain at risk of contracting the virus when the social and economic restrictions start to ease.
2. CONTACT TRACING
Contact tracing is a targeted approach to finding cases of COVID-19 in communities by tracing people who have come into contact with an infected person. It’s an approach that has been at the heart of outbreak response for decades: it helped eradicate smallpox in the 1970s and in the past few years has been used in the Democratic Republic of the Congo in response to Ebola, where contacts were tracked down and vaccinated with the new Ebola vaccine. The countries that are faring the best against COVID-19 now include many that invested in contact tracing from the start, with the aim of containing the outbreak. Some countries are using smartphone apps to alert people who could have been exposed to the coronavirus, but there seems to be no substitute for a strong contact tracing network of local people who can identify those at risk through interviewing cases.
3. TESTING
A strategy such as contact tracing relies on a robust testing capacity. South Korea began open public testing as early as the beginning of February, even for people who were not showing symptoms. Germany followed their lead: from as early as 20 March, laboratories in Germany had the collective capacity to carry out 160,000 tests a week. Using widespread testing, these countries were not only able to gain a more accurate picture of the extent of transmission of the virus in their communities, but more reliably identify those who could have been exposed and ensure that they went into isolation.
4. HOSPITAL SURGE CAPACITY
Many of the countries that implemented strict lockdown measures, such as the UK, did so out of concerns that the healthcare system would not be able to cope with rapidly rising numbers of cases. However, many of the countries that had previous experience from the 2003 SARS outbreak had already built surge capacity into their healthcare systems. Post-SARS, Singapore expanded isolation capacity in all public hospitals and even built a 330-bed isolation hospital, which provided a buffer when COVID-19 hit.
5. PPE SUPPLY
In March the World Health Organization (WHO) warned that shortages of Personal Protective Equipment (PPE), such as gloves, masks and gowns, posed a major risk to the safety of health workers around the world. They estimated that manufacturing of such equipment may need to increase by 40%. Whilst governments were focussing on scaling-up healthcare capacity through increasing numbers of ventilators and beds, fewer countries were giving enough attention to protecting the health system’s most valuable resource: its workers. Countries like Singapore, who already had a stockpile of PPE as part of their outbreak preparedness infrastructure, have been able to prevent healthcare-associated transmission of the virus.
6. CLEAR MESSAGING
Countries such as New Zealand have been marked out for their clear communication to the public about the risks posed by the coronavirus and the rationale behind the response. Prime Minister, Jacinda Ardern, has been praised for her clear but kind messages on response measures, asking the country to “Unite against COVID-19.” It’s a contrast to the images of war and messages about fighting the virus that have been evoked by some governments.
Whilst war analogies can sound compelling, they have received widespread criticism for promoting panic and encouraging an inward-looking approach to responding to the virus. Messaging around simple protection methods such as hand hygiene and mask-wearing could also have an important impact on transmission, particularly in communities where physical distancing is more challenging.
7. ACT FAST
In a WHO COVID-19 briefing, Dr Michael Ryan said of emergency response that “the greatest error is not to move.” Countries that implemented control strategies rapidly seem to be faring the best, whether that is by introducing early lockdown measures or rapidly scaling-up their capacity to test and trace. It is crucial that rapid response is based on evidence, as the urge to act without enough data and analysis can lead to misinformed health policy. Many of those are countries who had already experienced an outbreak of a serious respiratory disease in the form of SARS and MERS, but this is not a rule. With strong political leadership, other countries across the world, such as New Zealand, Germany, Switzerland and Japan, have stood out for their clear strategy and clear communication from the start.
For many countries, facing an outbreak like COVID-19 has been an entirely new challenge, and the evidence around the effectiveness of control measures has been scarce. Capitalising on the vast amounts of data becoming increasing available on what works best will be important for informing the ongoing response to COVID-19, and in preparation for future pandemics.