Vaccine hesitancy in South Africa: COVID experience highlights conspiracies, mistrust and the role of the media
Curbing vaccine hesitancy is as much a matter of acknowledging its social, historical, and cultural roots as it is of addressing its clinical dimensions.
- 27 January 2023
- 5 min read
- by The Conversation
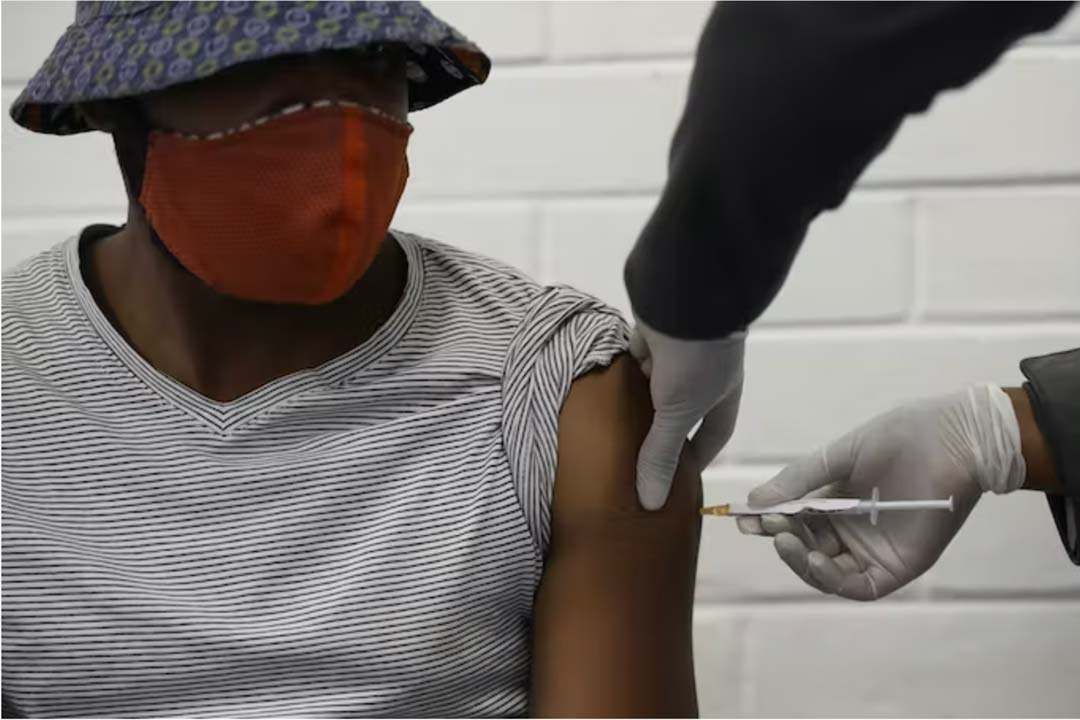
In recent weeks, China has reported a spike in new cases of COVID and related deaths. Some countries have imposed travel restrictions as a result. But most – including South Africa – have not.
Instead, the South African government’s approach is to increase testing, boost surveillance, and, most importantly, breathe new life into its COVID vaccination campaign.
South Africa first introduced COVID vaccines in February 2021. It set an ambitious target of fully vaccinating 67% of the population (40 million people) by the end of that year. By mid-January 2023, almost two years down the road, only 35% (21 million people) had been fully vaccinated.
One area that’s seen a troublingly low turnout is Soweto. The area is a massive cluster of some 30 townships – underdeveloped, racially segregated urban areas – in the south of Johannesburg. Soweto has about 1.7 million inhabitants; most are black. Only about 20% have gone to a vaccine site to finish their inoculation.
This vaccination rate is in stark contrast to what Sowetans told us as part of a study we undertook back in August 2020, before vaccines became available nationwide. The study was done at Chris Hani Baragwanath Academic Hospital in Soweto – Africa’s largest hospital. More than half of everyone we interviewed said they would accept a vaccine. This was still much lower than national surveys at the time, which estimated a hypothetical acceptance rate of about 75% on average.
This clearly shows that hypothetical intent to vaccinate cannot be used to predict uptake. To plan an effective rollout, it’s paramount to understand the social underpinnings of vaccine hesitancy in Soweto. Such insights would likely be transferable to places with similar demographics and socioeconomic profiles throughout South Africa.
What drives hesitancy?
There is always a certain “field of suspicion” in perceptions and attitudes towards illness and inoculation. People may have uncertainties and doubts concerning, for instance, adverse side effects, symptoms, or outcomes of disease. This is especially true in the case of a novel, rapidly spreading and potentially deadly virus like COVID-19.
In Soweto, we identified a host of factors amplifying this field of suspicion.
The haphazard way in which the media reported on the disease was one such factor. There were conflicting messages coming from health and government authorities. Wild speculation, rumours, “fake news” and whispers about COVID-19’s nature and true origins spread via local social media networks and in some parts of the press. Some concepts weren’t explained in a way non-expert audiences could engage with (or in languages that the vast majority of people in Soweto speak).
Have you read?
Mistrust of the institutions involved was another factor. Suspicion and uncertainty opens a space in society for stubborn false or incorrect claims and conspiracy theories. Some people were saying that COVID-19 fatalities had been deliberately exaggerated and that it was a scheme concocted by “Big Pharma”. Some believed that the virus did not exist. Others claimed that Bill Gates had put a microchip in the vaccine to “control” the masses, or that the 5G network was somehow causing it.
In Soweto, various Africanised counterfactual claims circulated. For instance, some warned that COVID-19 was a man-made virus purposefully created to destroy black African populations. Or, in a contradictory version, black people were immune and COVID-19 only infected white people.
When such misinformation flourishes, people become even more anxious, doubtful and hesitant about getting vaccinated.
Structural, social, economic and political factors together decrease uptake in immunisation programmes. This is particularly evident in townships such as Soweto because of histories of colonisation, marginalisation and racism. For instance, during apartheid, the white government displaced thousands of people and decreased funding for social services such as education and healthcare for non-whites. This resulted in a lack of medical coverage for and discrimination against black people both economically and in terms of healthcare. These historical and structural health disparities continue to have an impact on the broader healthcare picture in South Africa even today.
Another factor was related and, in some ways, similar to the issue of mistrust. The pandemic triggered a social mechanism that medical anthropologists refer to as “othering”, just as it did and still does in the ongoing HIV pandemic. This time, othering presented in its more sinister form – racialisation.
Othering can be viewed as scapegoating and stigmatisation – believing, for instance, that the virus affects only the rich, white people or foreigners.
Othering and racialisation also reinforce false divisions: the mkhukhu (shack) dweller against the wealthy, black people against white people, those who are pro-vaccination against those who mistrust vaccines. All of these tensions combined can destabilise the authorities’ credibility as they try to roll out immunisation programmes.
Way forward
It remains paramount during vaccination rollouts to explore and address factors that influence vaccine confidence and selectivity.
Appropriate media coverage of vaccination and debunking of wrong “information” is crucial in driving forward immunisation.
Curbing vaccine hesitancy is as much a matter of acknowledging its social, historical and cultural roots as it is of addressing its clinical dimensions. These are lessons best remembered for future outbreaks – and they are even more important to unravel now as South Africa’s government encourages more people to line up for the COVID-19 jabs.![]()
Authors
Bent Steenberg, Medical Anthropologist, Vaccines and Infectious Diseases Analytics Research Unit, South African Medical Research Council

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Bent Steenberg has received funding from the Danish International Development Agency (Danida), the European Commission, the Mellon Foundation, and the Bill & Melinda Gates Foundation.








