How good quality data is vital to saving lives
Throughout the 2016–2020 strategic period, the Vaccine Alliance has worked with countries to improve data quality. From GIS to SMS, new tech and tools aim to reach more people with life-saving immunisation.
- 2 October 2020
- 4 min read
- by Gavi Staff

The saying “What gets measured, gets managed” applies across Gavi’s work. Without consistent, accurate data, Expanded Programme on Immunization (EPI) managers cannot run their programmes, and funds cannot be allocated to meet the most vital needs. The Vaccine Alliance has worked with countries throughout this strategic period to improve data quality, availability and use. The overall quality of data, as measured by the difference between administrative and survey estimates, has been stable since 2017, and countries have increasingly met the Alliance’s requirements for best practice in data gathering and use, and survey quality. Almost two thirds of Gavi-supported countries are now improving their use and analysis of data, to correct the course of their programmes as needed.
"What gets measured, gets managed"
applies across all of Gavi’s work.
Alliance-supported activities in 2019 included: the WHO Scholar Series on data quality, survey design and implementation, bringing together some 1,150 country staff (many of them working at subnational or facility level); development and roll-out of the DHIS2 data quality module to help identify inaccurate or implausible data inputs to health management information systems (HMIS); working with Kenya and Myanmar to pilot geographic information system (GIS) tools with geospatial data, and technologies to improve microplanning (and to map subnational coverage and equity); and, in Chad and Mozambique, developing and piloting satellite imagery, triangulation and statistical methods to estimate local target populations for immunisation at subdistrict levels.
Examples of countries where support from the extended Alliance partnership for improved data quality is making a difference include: Chad, where support from Acasus has helped build real-time data into informed decision-making; Angola, where an initiative from 2017 INFUSE Pacesetter Logistimo has supported vaccine management; Indonesia, where Gavi has supported the use of SMS-based RapidPro technology for vaccination campaign monitoring and data collection; Afghanistan, where a data quality improvement plan and provincial-level staff with analytical capacity are helping to improve data analysis and use at subnational level; and Pakistan, where an electronic immunisation registry supported with Gavi funding is helping build a picture of who has been vaccinated and who has been missed.

Measuring progress in DRC
Throughout 2019, outbreaks of infectious diseases (including measles and polio) in several countries supported by the Vaccine Alliance increased pressure on health systems, while also highlighting areas where populations are under-immunised.
Some countries with the greatest challenges nonetheless made progress on immunisation coverage. The Democratic Republic of the Congo (DRC) is home to a significant number of under-immunised and "zero-dose" children, evinced by the world’s worst measles epidemic and a decline in routine coverage (according to the latest WHO/UNICEF Estimates of National Immunization Coverage). With Gavi support and high-level political commitment, DRC is implementing the Mashako Plan (also known as the Emergency Plan for Revitalisation of Routine Immunisation in the DRC). Even while fighting Ebola and measles, DRC initiated a recovery trend in immunisation coverage – including an impressive 50% increase in 2019 in the number of monthly immunisation sessions held across the nine most vulnerable provinces (from 16,000 to 24,000). One feature of the plan is the use of detailed quarterly micro surveys to confirm where progress is being made.
Planning for success in South Sudan
In South Sudan, one of the world’s most acutely fragile countries, Gavi provided US$ 17.5 million of funding under Gavi’s Fragility, Emergencies and Refugees Policy, focused on strengthening service delivery, expanding cold chain capacity and improving data gathering for decision-making and planning. In eight of ten states, the third phase of the Health Pooled Fund (HPF3) – a collaboration of the UK Department for International Development (DFID), Government of Canada, Swedish International Development Cooperation Agency (Sida), United States Agency for International Development (USAID) and Gavi – with technical assistance by Crown Agents, helped expand immunisation delivery by complementing the country’s primary health care priorities.
Gavi also partnered with International Organization for Migration (IOM) to deliver an integrated package of health services, including immunisation, to refugee camps, migrants and other mobile populations. At 49%, South Sudan’s coverage with the third dose of diphtheria-pertussis-tetanus-containing vaccine was among the lowest in the world in 2019; yet this is 4 percentage points higher than 2016 – suggesting these efforts are starting to bear fruit.
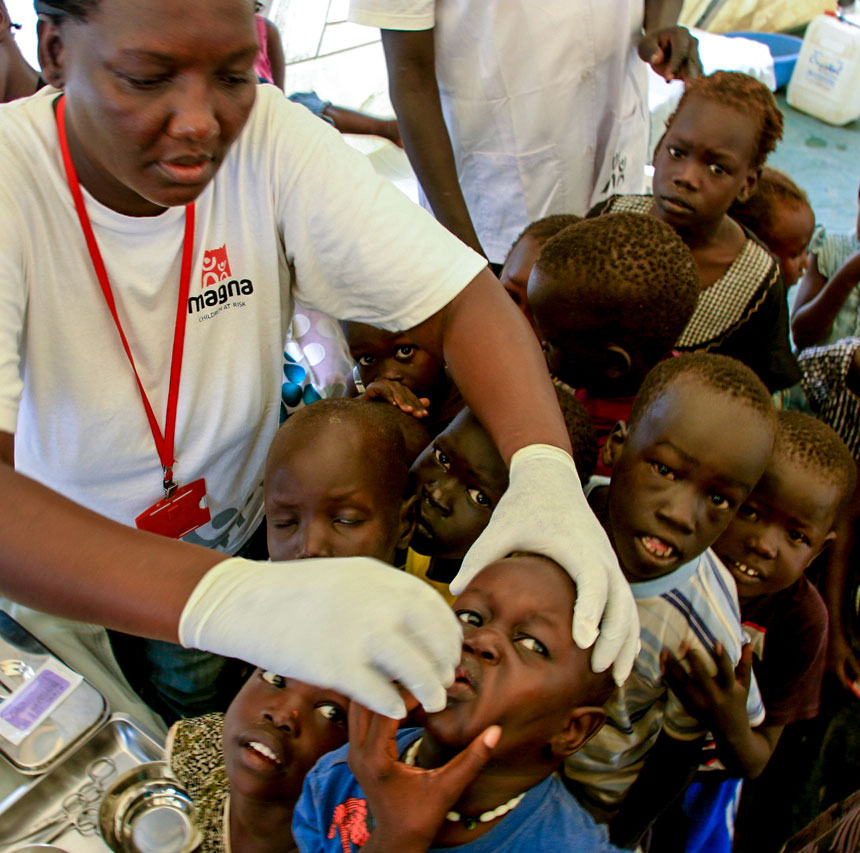
Read more about how Gavi has accelerated equitable uptake and coverage of vaccines in Gavi’s 2019 Annual Progress Report.










