Why get vaccinated when the flu vaccine doesn’t work well?
The best way we can prevent flu infection is by getting vaccinated. The problem with the flu vaccine is that in some years it doesn’t work as well as others.
- 16 December 2020
- 7 min read
- by Gavi Staff

Authors: Sarah A. Galvani-Townsend and Pratha Sah
Associate Editors: Tanya Dimitrova
Have you ever had the flu? Most people recover from it pretty fast. However, the flu still kills thousands of children and adults each year. This makes it a big health problem across the world. The best way we can prevent flu infection is by getting vaccinated. The problem with the flu vaccine is that in some years it doesn’t work as well as others.
For example, in 2017-2018 the flu vaccine was less effective in preventing infection among vaccinated people compared to previous years. We wanted to study the impact of less effective vaccines in preventing flu-related infections, hospitalizations and deaths. We found that even when the flu vaccines don’t work well, they prevent a large number of people from getting infected or hospitalized and save thousands of lives. We also learned that when vaccines are less effective, it is most important for school-age children, young adults, and the elderly to be vaccinated.
Introduction
Influenza (flu) is a serious infection that is caused by viruses spreading from one person to another. Common symptoms of the flu include chills, sore throat, runny or stuffy nose, headache, muscle or body aches, tiredness, and fever. We see flu outbreaks in the US every year during the winter. In these outbreaks, about 5% to 20% of all Americans get sick from flu infections and many get hospitalized and die.
The Centers for Disease Control and Prevention (CDC) recommends everyone above the age of 6 months to be vaccinated. Because the flu virus keeps changing, the flu vaccine is modified each year. Still, the most common way that the flu vaccine is made hasn’t changed in over seventy years! Because of this old and unreliable technology, the flu vaccines don’t work well for some years (Figure 1).
That is also one of the reasons why many people don’t get vaccinated. In this study, we looked at the impact of a low efficacy vaccine in reducing health burden due to a flu outbreak. We also wanted to find out which age groups are especially important to vaccinate when the vaccine efficacy is low.
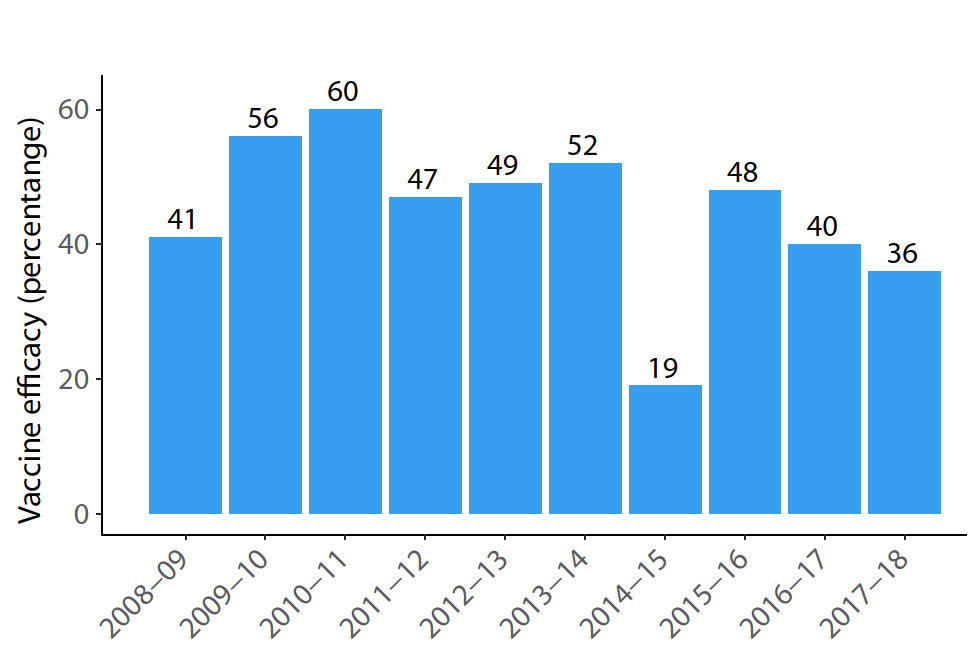
Figure 1:
Efficacy of influenza vaccines in the United States over the last 10 years.
Source: CDC
For the curious:
The traditional way to produce flu vaccines involves injecting live viruses into a fertilized chicken egg, then allowing the viruses to grow in numbers within the egg. Afterwards, the liquid from the egg is removed, and the influenza virus is killed so that it is incapable of causing an infection but can still stimulate the immune response that protects vaccinated people from future infections. This method of influenza vaccine preparation was first used during World War II to protect American troops. Since then, the method to produce the influenza vaccine has largely remained the same.

Lab workers deal with chicken eggs that are being used to develop a flu vaccine at Shanghai Institute of Biological Products (Photo credit: AP/CTV News, August 2009)
Methods
We created a computer model of flu outbreaks using flu data in the US for the past 5 years. In the model, we divided the people in the United States into seven age groups:
- 0 - 4 years old
- 5 - 19 y.o. (school age children)
- 20 - 29 y.o.
- 30 - 39 y.o.
- 40 - 49 y.o.
- 50 - 64 y.o.
- 65 years and older (elderly).
We used this model to predict flu outbreaks when vaccine efficacy was low. Our model allowed us to compare how many influenza cases, hospitalizations, and deaths can be prevented even with a low efficacy vaccine. Next, we found out which age groups needed to be vaccinated the most to minimize health burden due to flu outbreaks.
Results
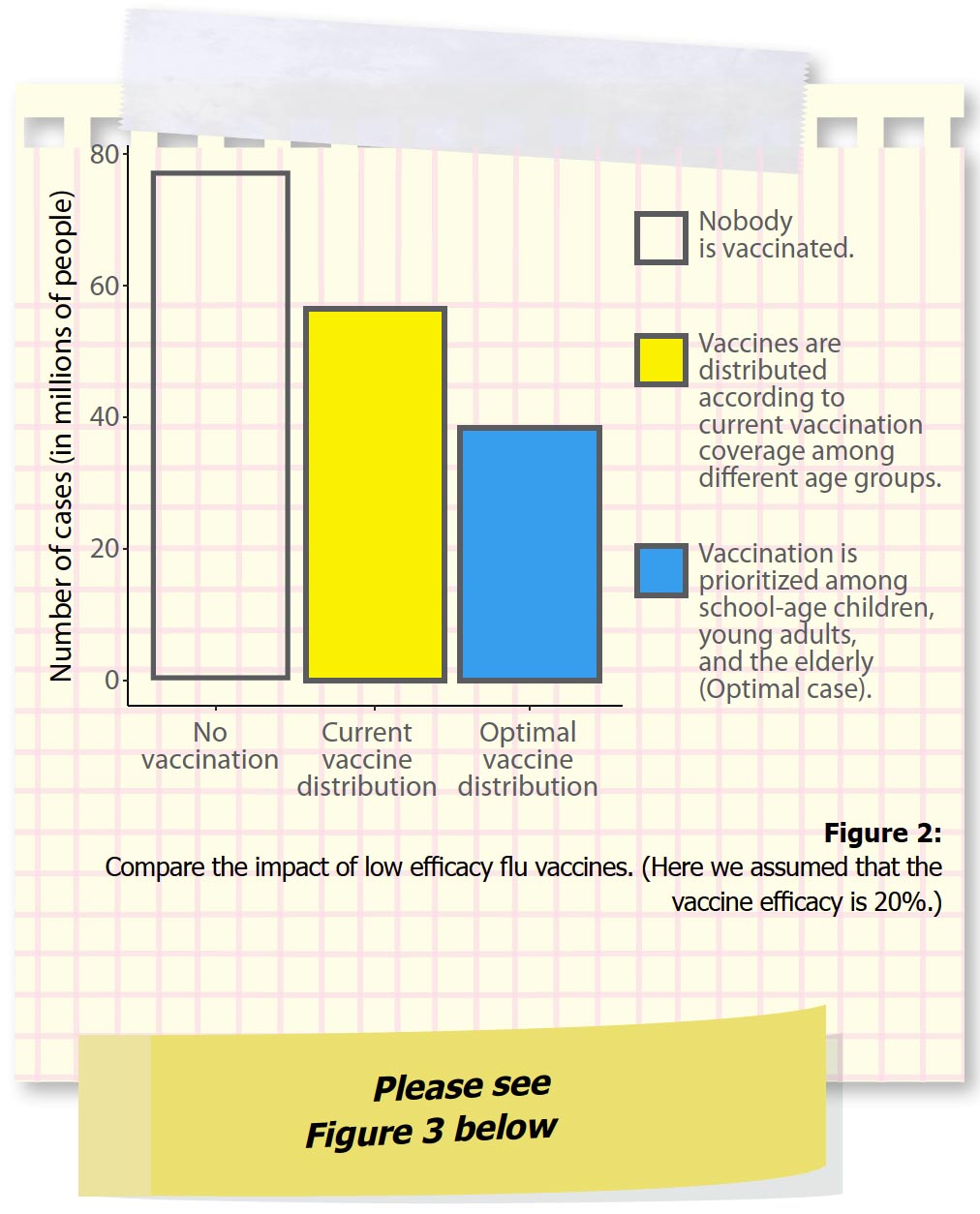
We found that low efficacy flu vaccines can still prevent many infections, hospitalizations and deaths compared to when no one gets vaccinated (Figure 2). Getting vaccinated - even when the flu vaccine doesn’t work well - is therefore much better than not getting vaccinated at all.
In our model, we compared two conditions:
| 1. fewer people getting vaccinated with typical flu vaccine (40% efficacy) - we call this low vaccination coverage | vs. | 2. more people getting vaccinated but with low efficacy flu vaccine (20% efficacy). |
...and found that the first case led to larger flu outbreaks. That’s why low vaccination coverage is a bigger danger than low vaccine efficacy.
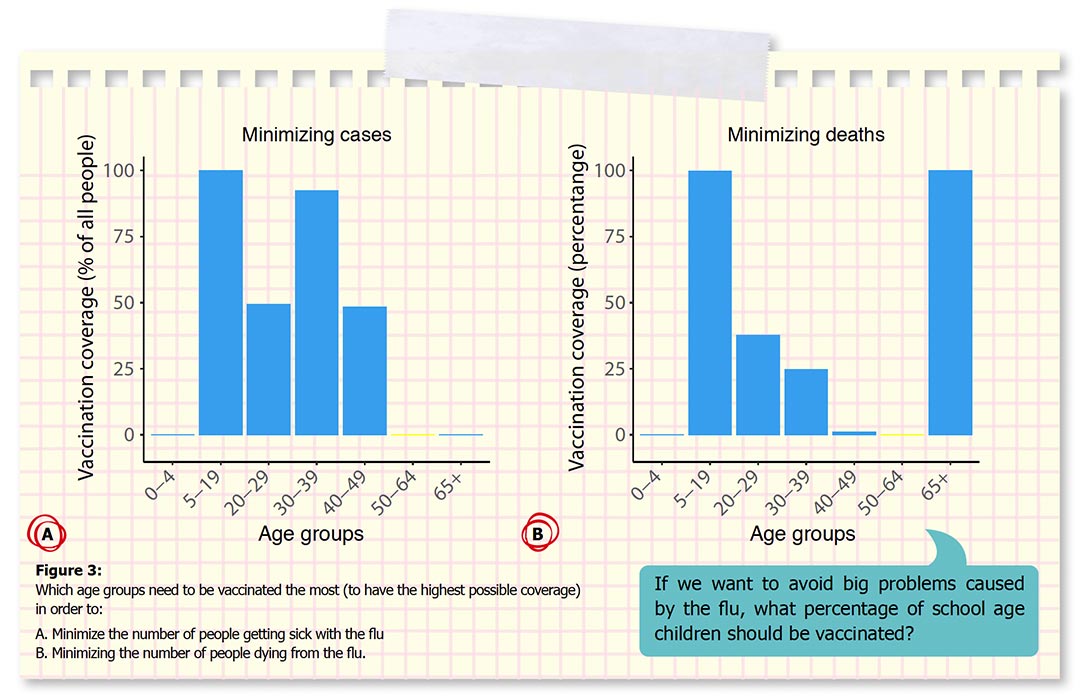
We also identified that prioritizing vaccination of school-age children, young adults, and the elderly is most important to minimize the number of flu-related infections, hospitalizations, and deaths (Figure 3). The elderly are especially important to prioritize when the vaccine doesn’t work as well.
Discussion
The efficacy of flu vaccine changes from year to year. In our study, we found that even a low efficacy vaccine can prevent a lot of flu-related infections, hospitalizations, and deaths.
Our results also prove that it is important to vaccinate as many people as possible, even when the vaccine efficacy is low.
Out of all age groups, it is important to prioritize vaccination of school-age children, young adults and the elderly. Vaccinating school-age children is important because they interact more with others than the adults, and therefore spread the flu more easily. Young adults should be vaccinated because they can easily spread flu to their young children and elderly parents, both of whom are at a higher risk of developing complications from a flu infection. We also found that the elderly are important to vaccinate because they are more likely to be hospitalized or even die from a flu infection. Vaccinating these three age groups would make the health burden of flu outbreaks a lot smaller when the flu vaccine does not work well.
Conclusion
When did you have your last flu shot? The shot may hurt your arm at the time but it is likely to save you from much more serious trouble. Even if the flu vaccine is not very effective, it is still safer to get vaccinated. This is especially important for school-age children and the elderly. You can teach your parents and grandparents about the safety and importance of flu vaccines. In many places, the shot is easily available at pharmacies, retail stores, and nursing homes. Be smart and protect your family from the next flu outbreak.
Check your understanding
1 Why is a new flu vaccine made every year?
2 According to the CDC, people of which ages should get flu shots every year?
3 Should everyone get vaccinated when the flu vaccine isn’t very effective? Why?
4 Is it more important to have a very effective influenza vaccine or to vaccinate everybody?
5 Which age groups are most important to vaccinate?
Glossary of Key Terms
Influenza – Influenza (or the flu) is an illness caused by a virus that infects the nose, throat, and sometimes the lungs. The virus can spread when a sick person coughs or sneezes. It can also be spread by touching surfaces that have the virus. Severe illness can lead to hospitalization and even death in some cases.
Outbreak – A sudden increase in the number of disease cases in a particular season and place.
Virus – A very small organism that usually makes you sick. Viruses need living cells of another being in order to multiply
Hospitalization – Being so sick that you have to be admitted to the hospital for treatment.
Centers for Disease Control and Prevention (CDC) – A national agency in the United States that protects human health and improves the quality of life.
Efficacy – A measure of how well flu vaccines work. For example, 40% vaccine efficacy means that people who received the vaccine are 40% less likely to be sick and need to see a doctor. The flu vaccine efficacy is calculated in the end of the flu season.
Health burden – A measure of how many people get infected, hospitalized and die from a disease.
Age group – All people who are of certain age. For example, “school age children” are all children between 5 and 19 years old.
Computer model – A computer program which attempts to simulate a real world system and to test how the system would behave in different conditions.
Vaccination coverage – Vaccination coverage is the percentage of people in a population that get vaccinated.
References
- Pratha Sah, Jan Medlock, Meagan C. Fitzpatrick, Burton H. Singer, and Alison P. Galvani (2018).
Optimizing the impact of low-efficacy influenza vaccines. PNAS
http://www.pnas.org/content/115/20/5151.short - CDC: About Influenza (Flu)
https://www.cdc.gov/flu/about/index.html










