Ask an Expert: Why Are There So Many COVID-19 Vaccines — and Is It Better to Have More?
Vaccines have been approved – so why are we still developing others?
- 17 December 2020
- 4 min read
- by Global Citizen

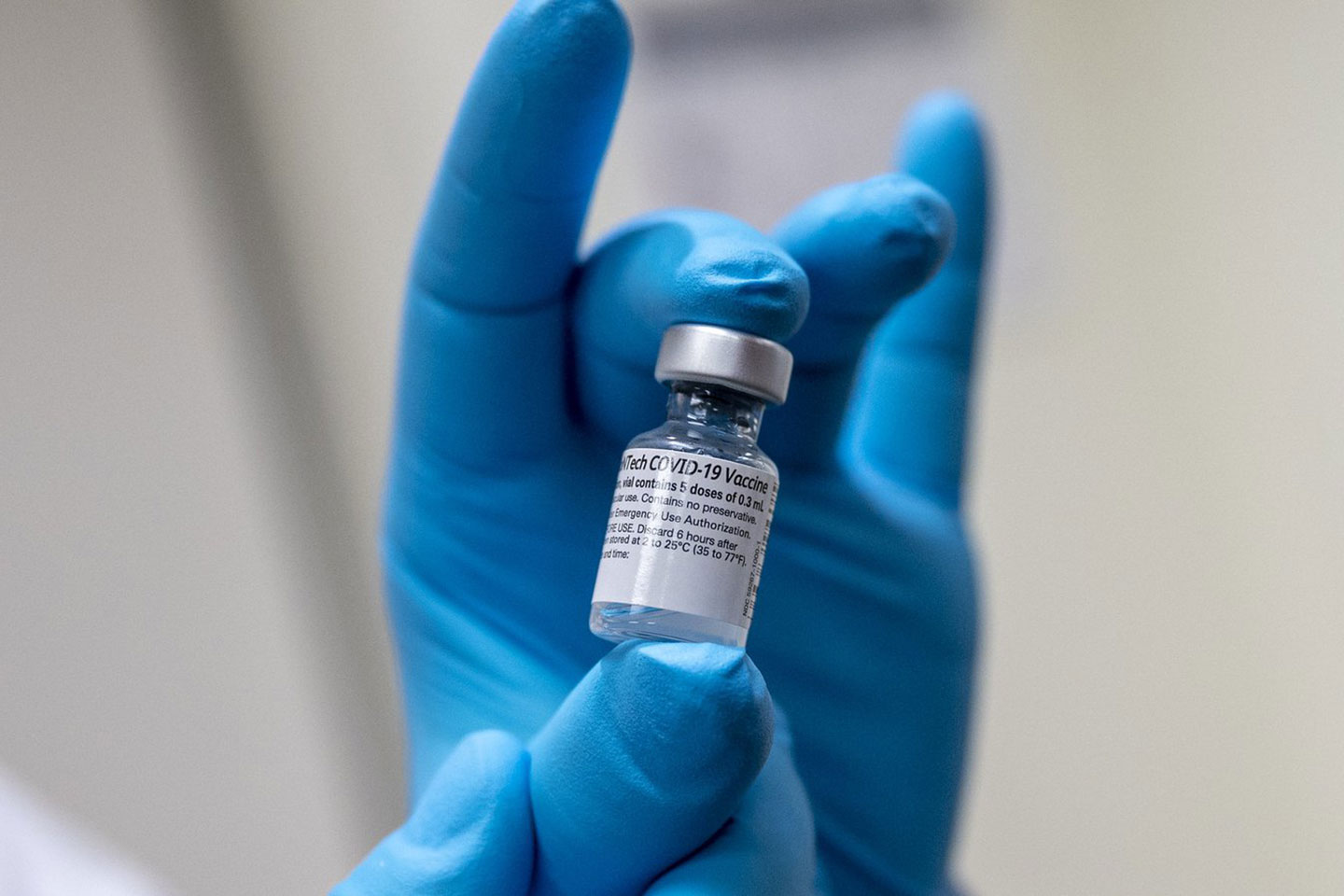
Pfizer-BioNTech, Moderna, and Oxford-AstraZeneca have all announced that their vaccine candidates are effective in protecting against COVID-19. Bahrain, the UK, Canada, the US, and Mexico have already approved the use of the Pfizer vaccine in their countries, and the Moderna vaccine seems sure to soon follow suit.
While this is all welcome news in the global health community as the world looks to bring an end to the COVID-19 pandemic, it also raises the question: Why are there so many vaccines in development? And is it better to have more?
Aurélia Nguyen, managing director of the COVID-19 Vaccine Global Access Facility (COVAX), has the answers.
“At an early stage during this pandemic, it quickly became apparent that to end this global crisis we don’t just need COVID-19 vaccines, we also need to ensure that everyone in the world has access to them,” Nguyen told Global Citizen.
The solution, according to her, is COVAX, a vaccine initiative co-led by Gavi, the Vaccine Alliance, the World Health Organization (WHO), and the Coalition for Epidemic Preparedness Innovation (CEPI).
Prior to working for the COVAX Facility, Nguyen was Gavi’s managing director for vaccines and sustainability, where she worked to find ways to support financially sustainable vaccine programs and markets — and essentially increase the delivery of life-saving vaccines.
Before that, she worked for GlaxoSmithKline (GSK), where she led the development of GSK’s policies on access to medications and vaccines in the developing world. She’s also done research for the WHO on medical policies and holds a master’s degree in health policy, planning, and financing from the London School of Hygiene and Tropical Medicine and the London School of Economics.
Have you read?
In short — she’s the perfect person for the job of ensuring equitable access to the COVID-19 vaccine.
“COVAX has the world’s largest and most diverse portfolio of COVID-19 vaccines, and as such represents the world’s best hope of bringing the acute phase of this pandemic to a swift end,” Nguyen said, adding that COVAX involves almost 90% of the world’s governments.
As of right now, COVAX has secured three promising vaccine candidates, but Nguyen says the goal is to have more in their portfolio.
“To achieve our goal of ending the acute stage of the pandemic by the end of 2021, we will need as many vaccine candidates as possible for use across a range of populations and settings,” she said.
The ideal situation for COVAX would be to have various types of vaccines secured through different manufacturers and supply chains.
“This will also require global manufacturers to step up and commit to this vision of equitable access. The dangers of not doing so — for the entire world, and the effect of this pandemic on public health, economies, trade, travel, communities, and individuals — are clear,” she added.
Given the huge demand for the vaccine around the world, Nguyen says that COVAX will need varied types of vaccines.
“Not all of these will have the same storage requirements,” she said. “In fact, most of the vaccines in development, if successful, will require regular cold chain infrastructure, which Gavi has spent the past two decades expanding and updating in lower-income countries.”
The cold chain entails storing and transporting temperature-specific vaccines, which can become ineffective if they get too warm, across a supply chain — this requires intense logistical planning on top of thermal and refrigerated packaging methods.
“Delivering a vaccine that needs to be transported and stored in extremely cold temperatures, or ultra-cold chain, presents challenges in terms of additional costs and infrastructure to ensure it can be distributed effectively. This is especially the case for low- and middle-income economies,” Nguyen said.
But she says that COVAX is ready to help countries should they need it.
And while that presents a pretty big challenge, it’s not without precedent — Nguyen notes that the Ebola vaccine, which requires cold chain infrastructure, was successfully rolled out in 2018 in the Democratic Republic of Congo (DRC).
“The country, with Gavi support, was still able to vaccinate over 300,000 people during the recent Ebola outbreak in the eastern part of the country, helping to bring an end to the second worst Ebola epidemic in history,” she explained.
That's why Nguyen says this kind of mass delivery is feasible, but she warns that it is hugely complex and will require international teams to work together with new technology, like cold storage devices that can keep vaccines at ultra-cold temperatures, without the need for electricity.