Three experts explain how we can support the health worker of the future
COVID-19 put health systems across the world under unprecedented pressure. Three experts discuss how to better support healthcare workers for the future.
- 3 May 2023
- 5 min read
- by World Economic Forum
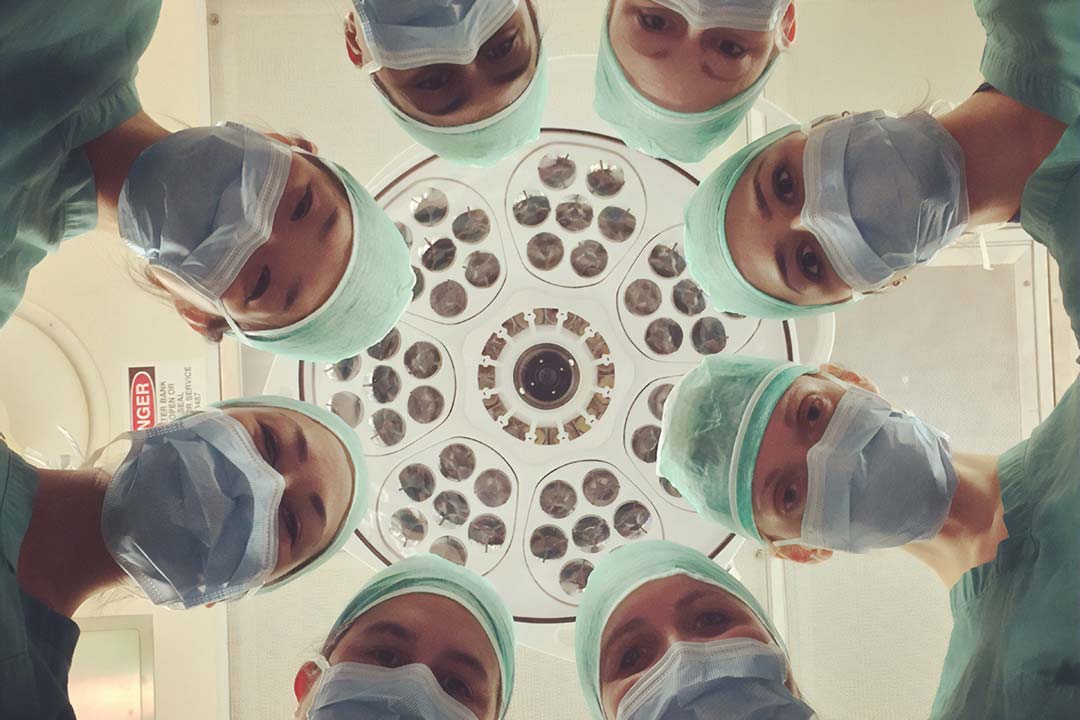
COVID-19 put health systems across the world under stresses unprecedented in the modern era. With an estimated shortfall of 10 million workers in the sector by 2030, we need policies and strategies to transform the health and care economy for the better.
Healthcare systems in many parts of the world were badly hit by the pandemic, which exacerbated stress, fatigue and burnout; put healthcare workers on the frontlines often without personal protective equipment; and led to a higher risk of infection or even death.
Adding to the challenges facing the healthcare sector is that many also consider the sector to be undervalued and underfunded, prompting many workers to leave.
Healthcare workers in high-income countries are quitting their posts due to low wages, while their counterparts from low- and middle-income countries increasingly migrate to seek better pay and conditions, leading to global shortages.
These issues were a topic of discussion at the World Economic Forum's Growth Summit 2023, which took place on 2-3 May at the Forum's headquarters in Geneva, Switzerland.
In a session titled "Future of Work: Health and Care", three experts explored how best to address the challenges. Here's what they had to say:
'Listen to healthcare workers'
Portuguese lawmaker Ricardo Baptista Leita argued that we need to listen to healthcare workers in order to address their concerns and improve retention rates.
This is a particular challenge in Portugal, which exports more nurses than it trains. Between 2015 and 2022, 13,000 nurses were trained but 15,000 left Portugal over the same period.
"We're seeing a transition from the public sector, mainly to the private sector because the public sector is unable to pay what people are expecting. And many of those in the private and/or the public sector are leaving the country – so going from domestic to international careers because they have better opportunities elsewhere," Leita explained.
Expectations of healthcare workers have also changed dramatically, with the idea of a balanced personal life top of list for many after the pandemic. Treated as heroes for their role on the frontline at the time, many now feel they are underappreciated.
"We need to address this challenge by listening to the healthcare workers. We can't continue doing what we've done until now, which is a top-down approach from governments telling healthcare systems what they're going to provide," Leita stated.
"We need to listen to healthcare workers. What do healthcare workers expect from the organization? Is it a balanced personal life? Opportunities in terms of research and life-long learning and so forth?"
Have you read?
Leita also argued that digitization should be seen as an opportunity in the health and care economy – "not to make healthcare less humane, but exactly the opposite".
"So that nurses, doctors, pharmacists and other healthcare workers have more time to be with the patient, to have more connection with the patient from a human perspective, so we can leave those repetitive basic tasks to machines," he said.
Howard Catton, Chief Executive Officer of the International Council of Nurses, argued that the 10 million shortfall of healthcare workers is actually an underestimate. Prior to the pandemic, there was a global shortage of 6 million nurses alone and there is now an ageing nursing workforce, accounting for another 4 million.
"The COVID effect we think could add a deficit of 2-3 million nurses. We're seeing the evidence already of people leaving early. So, just from a nursing perspective, we're looking at a number higher than 10 million – 12-13 million," he warned.
Countries need to invest in educating more nurses to address this growing deficit and change the dynamic whereby countries, often richer ones, end up looking to recruit from places that can least afford to lose them.
Future of Work: Health and Care with @RBaptistaLeite, @anjalibhagramd (@MayoClinic), @HowardCatton (@ICNurses) and @biancarothier (@GloboNews). #GrowthSummit23 https://t.co/f5cN8Vkvpp
— World Economic Forum (@wef) May 2, 2023
Catton also argued that nurses, in particular, need to have a place at the table when it comes to designing, planning and implementing healthcare systems.
"With nurses and all health professionals, because they know delivery, they know where the problems are, they know when care isn't patient-centred, where it is not safe," he said. "They have ideas about how we can improve. Seeing more nursing voices in leadership positions, government policy, and in health institutions as well, is really important."
'Create a better work experience'
The future workforce needs a better work experience and value proposition to address the deficit in healthcare workers, warned Anjali Bhagra, Professor of Medicine and Medical Director, Office of Equity, Inclusion and Diversity at Mayo Clinic.
"On the topic of equity, wellbeing, resilient systems, I think it is time that we prioritise the humane nature of our culture. We've got to infuse the healthcare culture with joy, with focus on humanity – and for that we need leadership, we need commitment," she said.
Some 23% of jobs are expected to be disrupted over the next five years, according to the World Economic Forum's Future of Jobs report. "So we cannot recruit a future workforce that is not upskilled," warned Bhagra.

"I think that fundamentally healthcare has relied heavily in the past on a physical pipeline model for healthcare delivery and at Mayo we are pushing that to a platform model, where there is a seamless integration of physical and digital healthcare provision. And what do we need to do for that? We need to get the workforce ready.
"Incoming students and learners can be skilled in a way they feel confident and competent while dealing with changing landscapes within the healthcare sector. However, many within the existing workforce will need to be upskilled - with the advent of technologies such as artificial intelligence (AI) - to create more future-ready healthcare systems," she added.
"Certainly it has been highlighted that training, governance, regulation, and incentives for integrating our enhanced AI capabilities will be the way that we are going to build a workforce that is more resilient, and we can do it collectively with a future-back approach."
Written by
Website
This article was originally published by the World Economic Forum on 3 May 2023.









