Keeping routine immunisation going during Uganda’s second lockdown
Despite a second lockdown, outreach initiatives ensure continuation of Uganda’s routine child immunisation.
- 19 July 2021
- 4 min read
- by Dicta Asiimwe
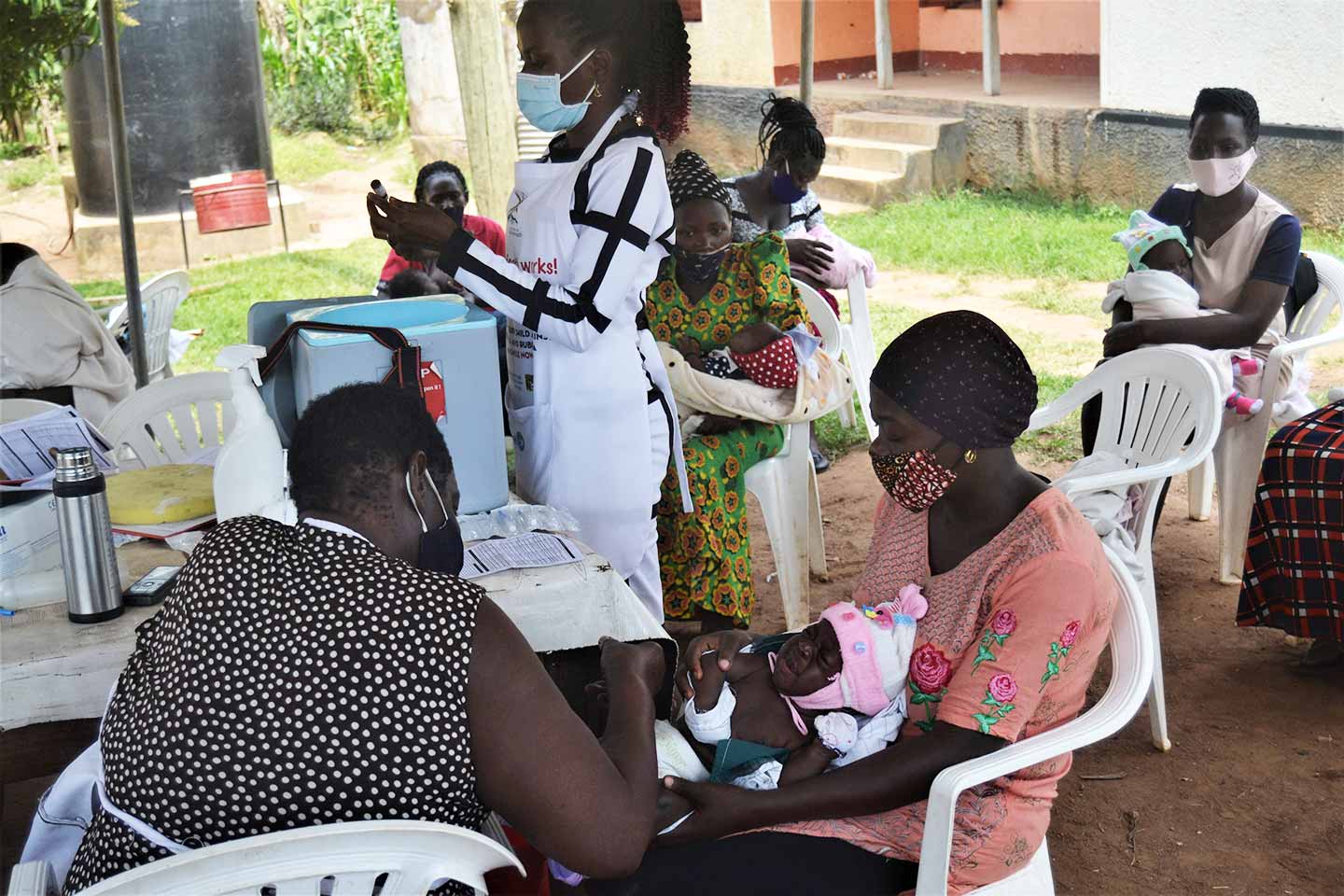
On June 18th, Ugandan President Yoweri Museveni announced the start of a second 42-day lockdown. Public transport is barred and citizens’ movement restricted, only allowing for the movement of essential service providers.
There have been concerns around the impact of this second lockdown, considering what happened in the first lockdown between March and June 2020. Back then the lockdown and widespread fear of contracting COVID-19 meant people stayed away from health facilities. Immunisation is among the services that were affected, with many parents not taking their children to get routine vaccines.
The outreach initiatives are funded by the Ugandan government, alongside other interventions from institutions, such as Gavi, the Vaccine Alliance and Save the Children, to take services closer to the people.
A Makerere University School of Public Health study on the impact of COVID-19 on essential health services suggested that Uganda suffered a drastic reduction in the number of children accessing all three necessary doses of their diphtheria, tetanus and pertussis-containing vaccine (DTP3) in April 2020, when the first lockdown was in place.
The same study shows that access to DTP3 had, by June 2020, recovered to levels beyond what was registered in 2018 and 2019. The June recovery prompted the Ministry of Health to hail the resilience of Uganda’s immunisation system. But the Makerere School study also shows that, on average, the number of children getting their DTP3 shots was lower in 2020 than in the two previous years.
Have you read?
This research is backed up by newly-released data from WHO and UNICEF, which shows DTP3 coverage in Uganda fell from 93% of children receiving these basic, routine vaccines in 2019 to 89% in 2020.
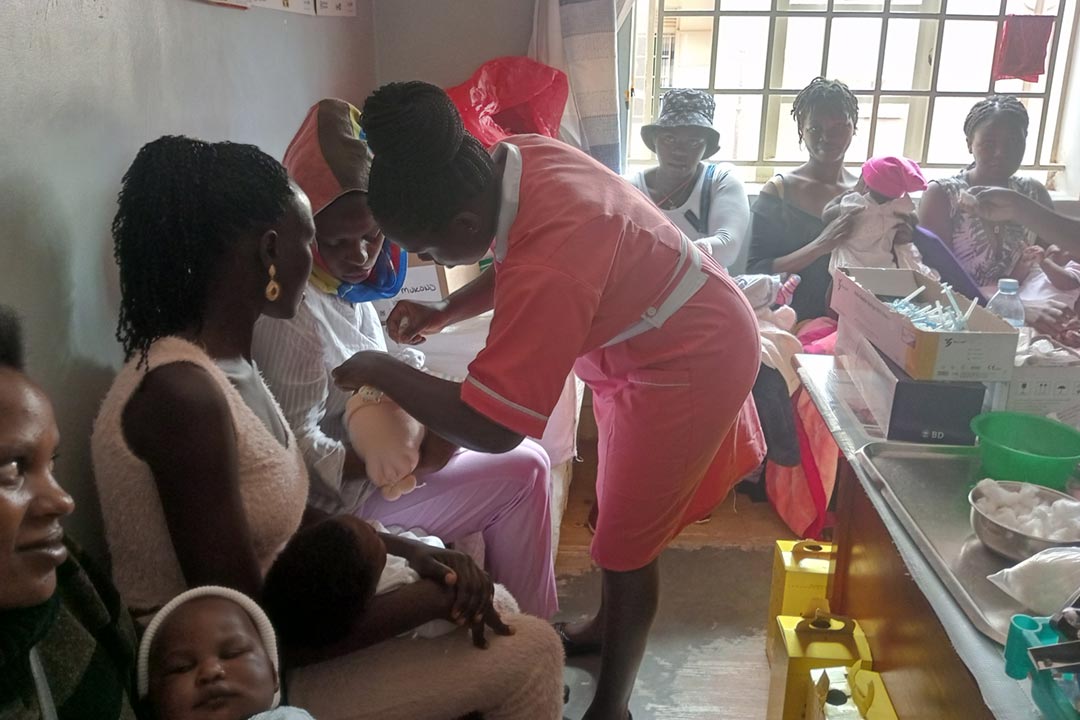
To help stop the same scenario playing out during this new lockdown, new outreach initiatives have been launched which Mary Nabuyondo, a nurse at Kakiri Health Centre III, believes will ensure that routine immunisation rates in her area do not decline.
The outreach initiatives are funded by the Ugandan government, alongside other interventions from institutions, such as Gavi, the Vaccine Alliance and Save the Children, to take services closer to the people.
Dr Mathias Mangeni, the District Health Officer for Namayingo district, says the grants have made it possible for Uganda to expand the reach of health services, especially in places such as Namayingo, which is part of the islands on Lake Victoria.
“Without the outreach, some members of our population could only reach a health facility by taking boats. This is difficult in normal times, but even harder under the current circumstances when there is a ban on non-emergency movement,” he says.
“Even for areas such as Kakiri, which is a semi urban area, these services are important. We do eight integrated outreaches every month during which we average 20 children,” adds Ms Nabuyondo.
This also enables health centres like Kakiri to access would-be zero-dose children. As Ms Nabuyondo says: “mothers will have most likely gone to the village to give birth, only to return and skip immunisation against childhood diseases.”
One reason is that, in Uganda, it is common practice for pregnant women to leave their partner’s home in the last trimester to give birth at their mother’s place. This is so that the pregnant woman is guided by her mother during the birthing process. The newborn also gets to be watched over and taken care of by their grandmother for the first few weeks.
However, the travel between two homes for new mothers can lead them to miss out on important services like immunisation. In addition to providing services to these potential zero-dose children, Dr Lorna Muhirwe, Head of Health at Save the Children Uganda, says that these outreach activities were important immunisation service points during Uganda’s first lockdown.
Officials at Save the Children Uganda highlighted Kakiri Health Centre as one centre that managed to keep immunisation going during the 2020 lockdown. The continued outreach is critical, as it allows people who would otherwise require transport to receive immunisation for their children within walking distance of their homes.