Monkeypox decision a shot in the arm for African health
WHO says countries must target intervention in communities with high transmission rate. Monkeypox has now been discovered in 75 countries and 11 are in Africa. Africa accounts for approximately 12 per cent of all reported cases.
- 23 August 2022
- 5 min read
- by SciDev.Net
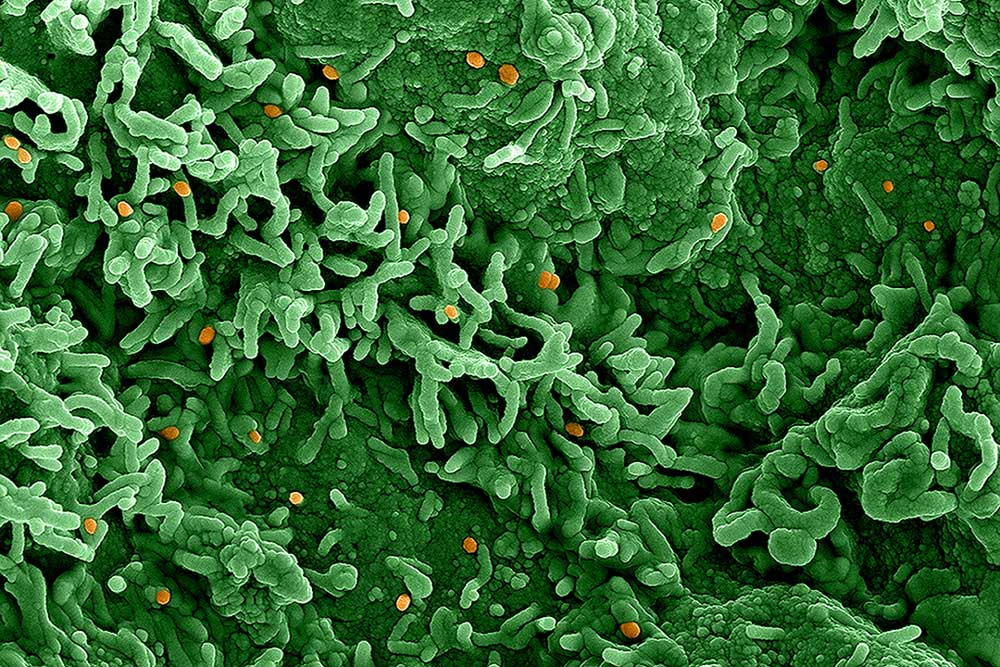
The decision to designate monkeypox a global health emergency will provide the much-needed stimulus for health institutions in the region to combat the virus, infectious disease experts in developing countries have said.
In July, the World Health Organization declared monkeypox a public health emergency of international concern (PHEIC), outlining a set of recommendations to implement a coordinated response to stop transmission of the virus and protect vulnerable groups.
“We have an outbreak that has spread around the world rapidly, through new modes of transmission, about which we understand too little, and which meets the criteria in the International Health Regulations,” WHO chief Tedros Adhanom Gbebreyesus, had said after the emergency committee meeting last month (23 July).
“It’s therefore essential that all countries work closely with communities of men who have sex with men, to design and deliver effective information and services, and to adopt measures that protect the health, human rights, and dignity of affected communities.”
Tedros Adhanom Gbebreyesus, WHO
“WHO’s assessment is that the risk of monkeypox is moderate globally and in all regions, except in the European region where we assess the risk as high. There is also a clear risk of further international spread, although the risk of interference with international traffic remains low for the moment,” Tedros had said.
Dimie Ogoina, member of the international health regulation committee on monkeypox response and a professor of medicine at Niger Delta University in southern Nigeria, believes the WHO’s declaration would create global solidarity and collaboration beneficial for developing countries.
“I can tell you that since it was declared, I’ve gotten calls from different people across the globe requesting for collaboration in order to deepen the understanding of human monkeypox in Nigeria,” he said.
Ogoina said the declaration would also improve the political will to invest in monkeypox amongst government at all levels both national and sub-national governments.
“If WHO has declared something a public health emergency of international concern and for instance, you have monkeypox in Nigeria, states and federal government will be more willing to invest in monkeypox surveillance and treatment.”
Increased awareness
Ogoina tells SciDev.net that the declaration has increased awareness and clinical suspicion among clinicians and in turn, caused increase case detection in Nigeria because of improved surveillance and awareness.
He also says drugs and vaccine that were hitherto unavailable in Africa would be made available.
“We are yet to see therapeutics or vaccines in Nigeria, for instance. But the Nigeria Centre for Disease Control is making efforts to ensure that they are able to tap into the global supply and leverage the connections they have to get the vaccines into Nigeria.”
Monkeypox, once a neglected disease
In May, epidemiologists in the region worried about the lack of investments in surveillance and infrastructuture to manage monkeyypox in Africa.
Oyewale Tomori, in an earlier report, had told SciDev.Net that the region does not have to wait for WHO or the global community to take strong actions over an outbreak endemic in Africa.
Have you read?
“We have had monkeypox since 1970, why are we waiting ‘til now to show concern or take appropriate prevention and control action?”
Ogoina says while it might not have been necessary to declare monkeypox a public health emergency of international concern when the disease only spread in Africa, there were several other channels that the world could have supported Africa in order to deepen the knowledge on the disease.
“Because it is happening in the global north now, that why everyone wants to conduct research. I would argue that in 2017, there was a need for global solidarity because infectious pathogens have no borders,” he said as he made a case for collaboration and investment in infectious disease regardless of its origin.
While health experts say the WHO’s decision is the right step in the right direction, some worry that the spread of the disease could stretch the already exhausted health systems in developing countries, which are yet to recover from the devastating impact of coronavirus.
Mohammed Yerima, a professor of microbiology, said viral diseases would always pose serious challenges to the health infrastructure of developing countries because of the sophistication needed for their detection.
“Unless and until governments of developing countries wake up to improve health infrastructure, these emerging and re-emerging diseases, especially viral diseases, will continue to be a threat to the economy,” said Yerima, a lecturer at Nigeria’s Sokoto State University.
Stigma
Monkeypox is transmitted to humans primarily through close contact with an infected person, animal, or material contaminated with the virus.
Of the 75 countries where monkeypox has been reported, 11 are in Africa, accounting for approximately 12 per cent of all reported cases. Since the beginning of 2022, more than 2,000 monkeypox cases have been reported on the continent from nine endemic and two non-endemic countries, according to the Africa CDC.
Large outbreaks have been recorded in Brazil – where 592 cases were reported as of 25 July – and Peru, with less than ten cases so far reported in India, Lebanon and Thailand, according to the US Centers for Disease Control and Prevention monkeypox outbreak global map.
A study by an international collaborative group of clinicians published in the New England Journal of Medicine last month (21 July) examined monkeypox infections between April and June across 16 countries. It found that 98 per cent of people with infection were men who have sex with men.
The clinicians warned against stigmatizing communities, saying: “Although the current outbreak is disproportionately affecting gay or bisexual men and other men who have sex with men, monkeypox is no more a ‘gay disease’ than it is an ‘African disease’.
“It can affect anyone.”
Tedros called for strategies to protect affected communities and stop the spread of the outbreak. “This is an outbreak that can be stopped with the right strategies in the right groups,” he said.
“It’s therefore essential that all countries work closely with communities of men who have sex with men, to design and deliver effective information and services, and to adopt measures that protect the health, human rights, and dignity of affected communities.
“Stigma and discrimination can be as dangerous as any virus.”
Author
Website
This article is republished from SciDev.Net under a Creative Commons license.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.