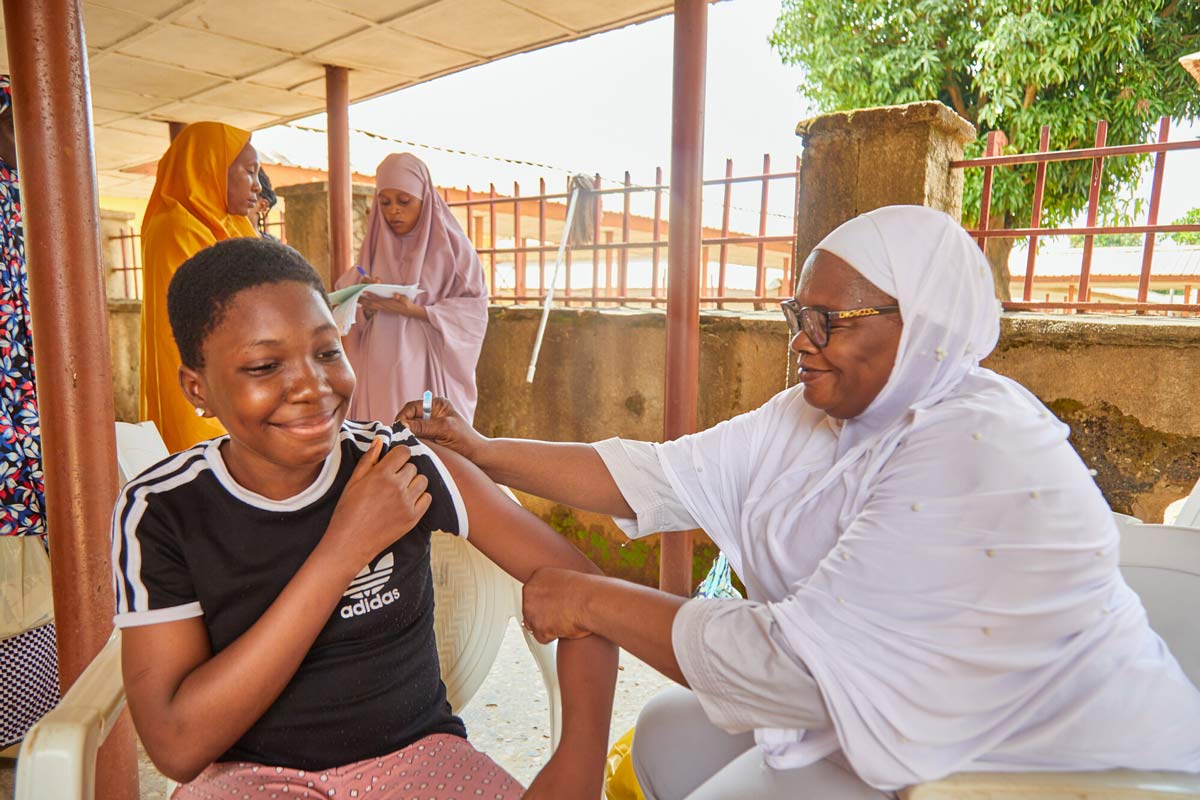Nigeria’s new initiative to boost routine immunisation
To improve routine immunisation, Nigeria is implementing the Accelerated Action for Impact (AAI) initiative.
- 12 August 2021
- 4 min read
- by Royal Ibeh
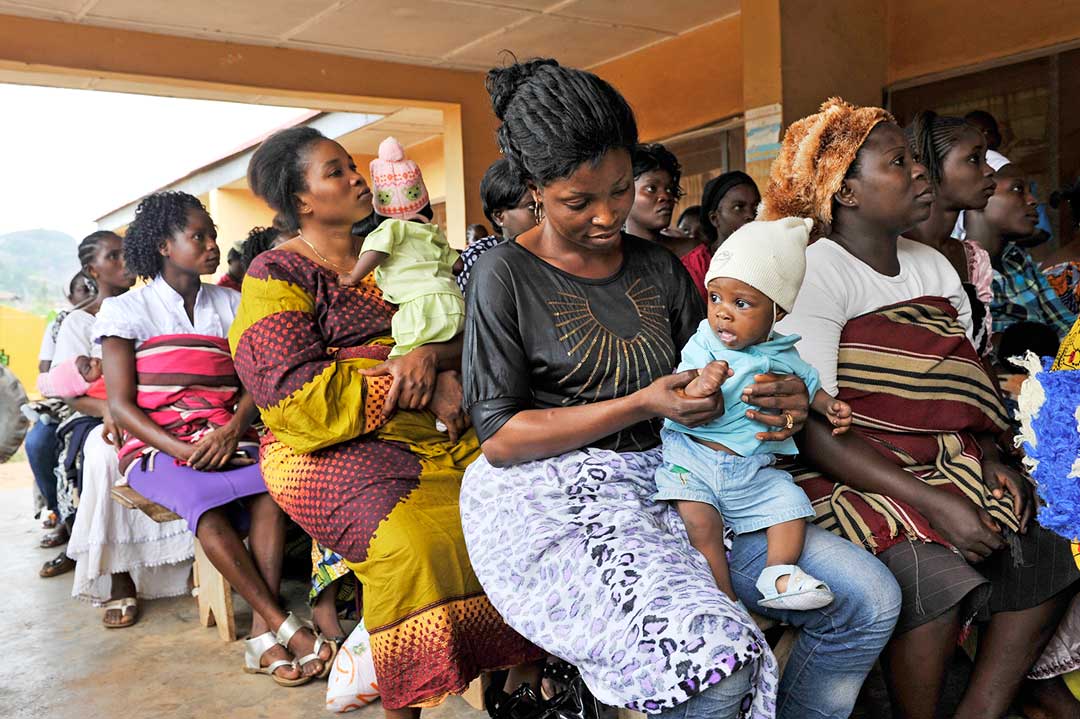
Nigeria’s routine immunisation coverage decreased by close to 20% in the period 2014 to 2016, placing more children at risk of preventable diseases. This made the achievement of the Sustainable Development Goal target of fully vaccinating 90% of children by 2030 a pipe dream for Nigeria - unless major changes were made fast.
Enter the Accelerated Action for Impact (AAI) initiative. Aimed at reducing preventable maternal and child deaths across Nigeria, the AAI is collaboration between the Nigerian government and organisations such as UNICEF, the European Union, the Gates Foundation, the Global Fund and Gavi, the Vaccine Alliance, among others. Focusing first and foremost on the data, the AAI process analyses gaps and bottlenecks in terms of both supply and demand across the maternal and child health life-cycle.
Even while COVID-19 was disrupting the healthcare system, with the AAI structures in place immunisation campaigns were launched immediately after the easing of movement restrictions in Oyo state.
“By triangulating available data, the four states of Kebbi, Bauchi, Niger and Oyo - which have the highest maternal and infant mortality - were prioritised with focused support to the poorest performing local government areas (LGAs) in each of the states,” says Khalilu Muhammad, Health Specialist at UNICEF in Abuja.
“Available survey and programme data were analysed at the most granular level, and the challenges of each specific community were considered in developing appropriate and tailored innovative solutions, together with health workers and community members,” he adds. “By revealing clearly where and what the most critical problems are, AAI rallies all stakeholders, from political leaders to health care workers to communities, around the urgent need to improve maternal and child health and survival in the four states."
Have you read?
In Niger state, Mariga and Mashegu were identified as the poorest performing LGAs in terms of maternal and child health. Muhammad says, “a rapid assessment was conducted which revealed that nine health facilities in these two areas lacked adequate manpower, and that there was low community understanding of the need for immunisation. Focusing on quick wins to drive action and improvement, 18 midwives and 40 health extension workers were allocated to these nine priority facilities, and targeted training of health workers based on gaps also commenced immediately."
He goes on to say, “there was inclusive engagement with community leaders and health care workers from the bottom up to jointly identify bottlenecks and develop solutions to tackle them. Teams for integrated outreach into remote areas were deployed to complement facility-based health care services.”
With the introduction of AAI, Muhammad says coverage for three doses of pentavalent vaccine increased to 33.3% (2018 SMART Survey) from 20% in 2016.
“One of the nurses at Beri Comprehensive Health Centre in Mariga LGA narrated how the initiative helped them increase their routine immunisation coverage, noting that she felt proud and elated seeing the way clients were rushing to the facility. She explained that prior to AAI introduction, it was difficult to record up to 20 antenatal care visits in a month, but with AAI implementation, anti-natal care visits jumped to between 100 and 200 in a month,’ he explains.
In Ondo state, Dr Ijeoma Agbo, a health specialist with UNICEF, says that prior to the AAI initiative approximately 38 babies were dying each day, primarily from sepsis and birth asphyxia, and fewer than four in ten children were fully immunised with routine childhood vaccines.
The AAI improved coordination between officials working in health including the Ministry of Health, Primary Health Care Board, National Orientation Agency (NOA), WHO and the private sector.
Former State Director of the NOA, Mr Moshood Olaleye says, “Members of the three communities complained of what they described as the hostile attitude of health workers, while several women said they gave birth at home because of alleged extortion at health facilities and poor attitude of health workers.”
Dr Agbo adds: “The existing structures in the communities and health facilities were, however, strengthened and utilised in delivery of routine immunisation and other essential Primary Healthcare Centre (PHC) services. NOA community dialogue activities were held which assisted in diagnosing bottlenecks and gaps in primary healthcare centers. The Ward Development Committees were also revitalised to strengthen community and Facility linkages.”
“With the AAI intervention, there has been increased awareness at the grassroots level on immunisation and practices promoting elimination of deaths of under one-month olds. Nursing mothers and pregnant women are now promptly referred to approved health facilities for immunisation and other child health services,” he adds.
Even while COVID-19 was disrupting the healthcare system, with the AAI structures in place immunisation campaigns were launched immediately after the easing of movement restrictions in Oyo state, according to Grace Olukun, a local government monitoring and evaluation officer.
“Presently, mothers bring their children to health facilities every Tuesdays and Thursdays for vaccination. They don’t miss it,” she says.