Noma is a truly devastating tropical disease – more people need to know about it
The World Health Organization recently recognised noma as a ‘neglected tropical disease’.
- 10 April 2024
- 4 min read
- by The Conversation
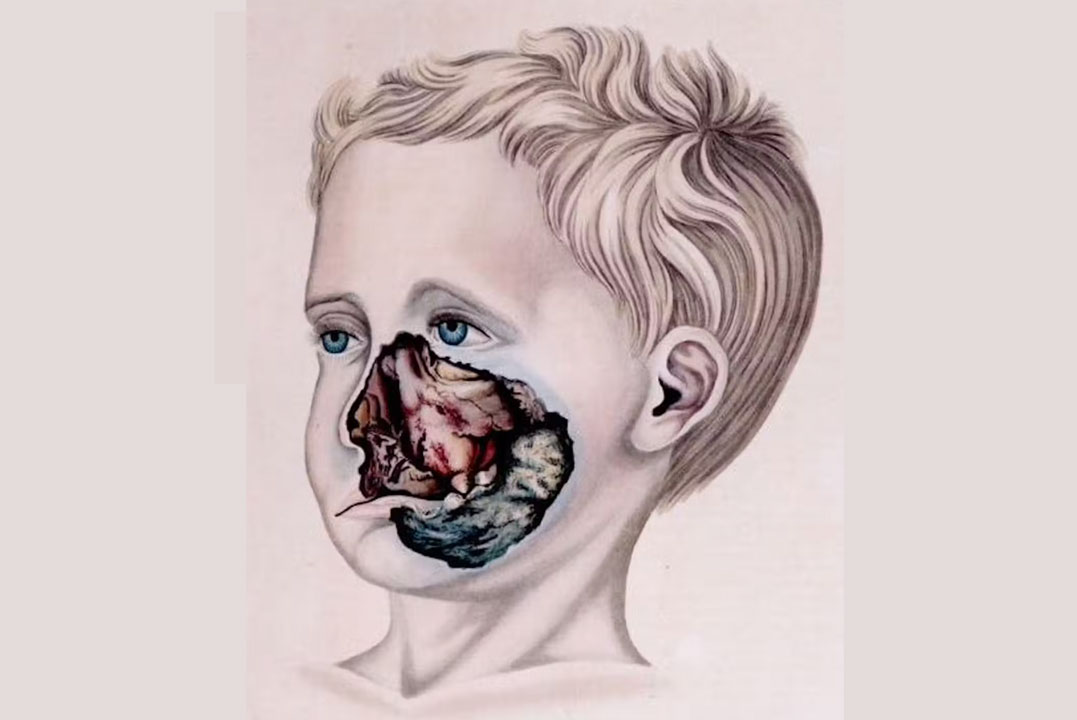
Noma is a rapidly progressing and often deadly gangrenous infection of the face. Horrifically, it mainly affects very young children living in extreme poverty. Despite this, few know of noma’s existence.
In December 2023, after years of advocacy, noma was finally included on the World Health Organization’s list of “neglected tropical diseases”. This is a significant achievement as it increases opportunities for funding and research into the disease, and will ultimately be an important step in helping to eradicate it, globally.
Mone is a noma survivor from Laos, and her experience of noma is typical of so many who have suffered from this disease. When Mone was 16, she met my colleague Dr Leila Srour, a paediatrician who happened to be working in her remote village in Laos, who was able to document Mone’s story.
When Mone was four years old, she developed a sore in her mouth, followed by swelling in her cheek, accompanied by a bad smell. The family treated her with leaves from the jungle. Quickly, her cheek skin fell away and teeth and bones started coming out of the sore in her cheek.
Her parents took her to the hospital, where the dead tissue was removed and she received antibiotics. Thanks to this treatment, Mone survived the early, often deadly, stages of the disease.
Her father carried her on his back to her village with her cheek and part of her nose and lips missing. One of her eyes was lower than the other because the bone beneath it was eaten away. She could not move her jaw to chew or to talk. Mone learned to eat by pushing food against her teeth with her fingers.
Throughout her childhood and teenage years, she suffered from stigma, social isolation, and difficulty with speaking and eating. The healthcare workers, her family and the villagers did not know why Mone suffered and suspected that ghosts were punishing her.
When Dr Srour met Mone, she had never met a noma survivor before, and noma had not been reported in Laos previously. After several years of trying, Srour finally found a way for Mone to receive surgical treatment. Mone travelled to Singapore where she underwent several procedures including a 19-hour surgery. She spent three months in Singapore recovering. Years after returning to Laos, she got married and had three children.
Despite the hardships in her life, Mone is happy she had surgery. She can eat and speak clearly. She is the first reported case of noma in Laos.
A further 50 noma survivors have been identified in Laos who subsequently received care. These few patients are extremely lucky, as the vast majority of noma patients do not survive, and those who do rarely receive the complex surgical care needed to enable them to live a life as close to normal as possible.
Have you read?
Noma starts as a small mouth ulcer and within weeks, leads to the swelling and then falling away of the cheek, and in some cases the nose or the eye – or both.
Most patients die within the first few weeks of infection. However, if they are given widely available antibiotics in these early stages, the infection can be halted, and the patient saved. For those who survive, many are left with lifelong physical health issues, such as trouble eating, drinking and talking, as well as mental health issues due to stigmatisation.
Much remains a mystery
Noma is an ancient disease, with the earliest description being found in a medical textbook from the first century.
It was often seen in Europe up until the 1800s, but has all but disappeared due to better access to food, water and healthcare. Now noma only affects the very poorest communities in the world.
Despite noma’s age, we know extremely little about the disease. We know it is bacterial in nature, but we haven’t been able to identify the causative organisms. We know it’s not infectious, but do not understand why some children get it while other children living in the same conditions do not.
The vast majority of our data on noma comes from Nigeria, which has two dedicated noma hospitals, but for many other regions of the world, all we have are sporadic case reports and anecdotal evidence. Our current best guess is that 110,000 people die from noma each year, but this needs to be treated with caution because we simply do not have the data to be confident of the numbers.
This is why the inclusion of noma on the WHO list of neglected tropical diseases is a significant step in tackling the disease. It has and will continue to raise awareness about the disease. And will provide a much-needed impetus for governments and health agencies to work together to help patients and survivors.
Authors
Stuart Ainsworth, Senior Lecture and UKRI Future Leader Fellow, University of Liverpool

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Stuart Ainsworth is currently lead researcher on a noma project funded by Médecins Sans Frontières, and is affiliated with The International Noma Network.
Partners
University of Liverpool provides funding as a founding partner of The Conversation UK.








