The Pandemic Within the Pandemic
Globally, antibiotic use in hospitals has surged since the start of the COVID-19 pandemic, and over-the-counter sales, legal in many countries, have soared. This is further fueling the global crisis of antimicrobial resistance, as bacteria evolve and become immune to these drugs.
- 30 April 2021
- 5 min read
- by Project Syndicate
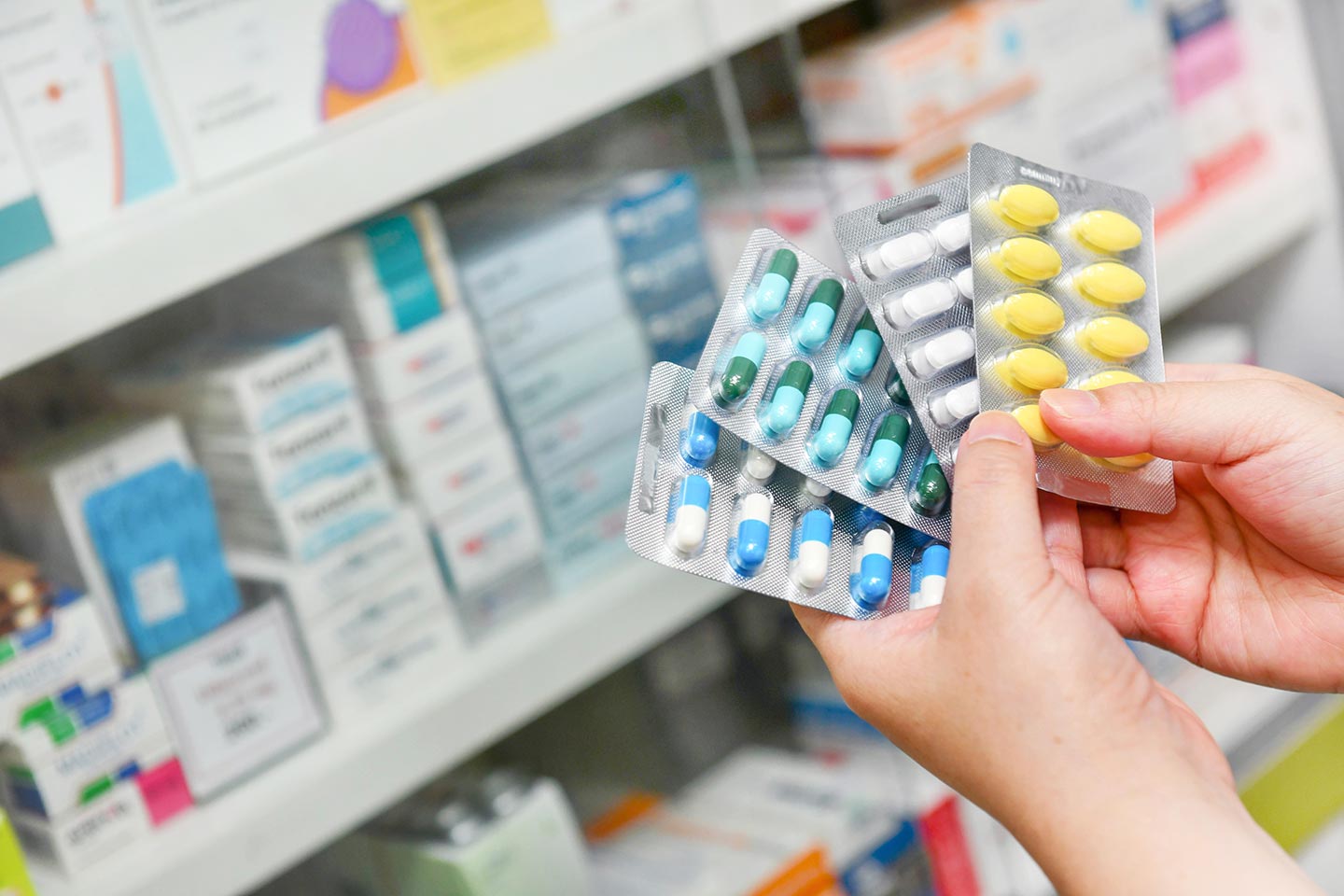
Fear of COVID-19 is driving increased over-the-counter (OTC) sales and in-hospital prescriptions of antibiotics – and fueling a silent pandemic in its wake.
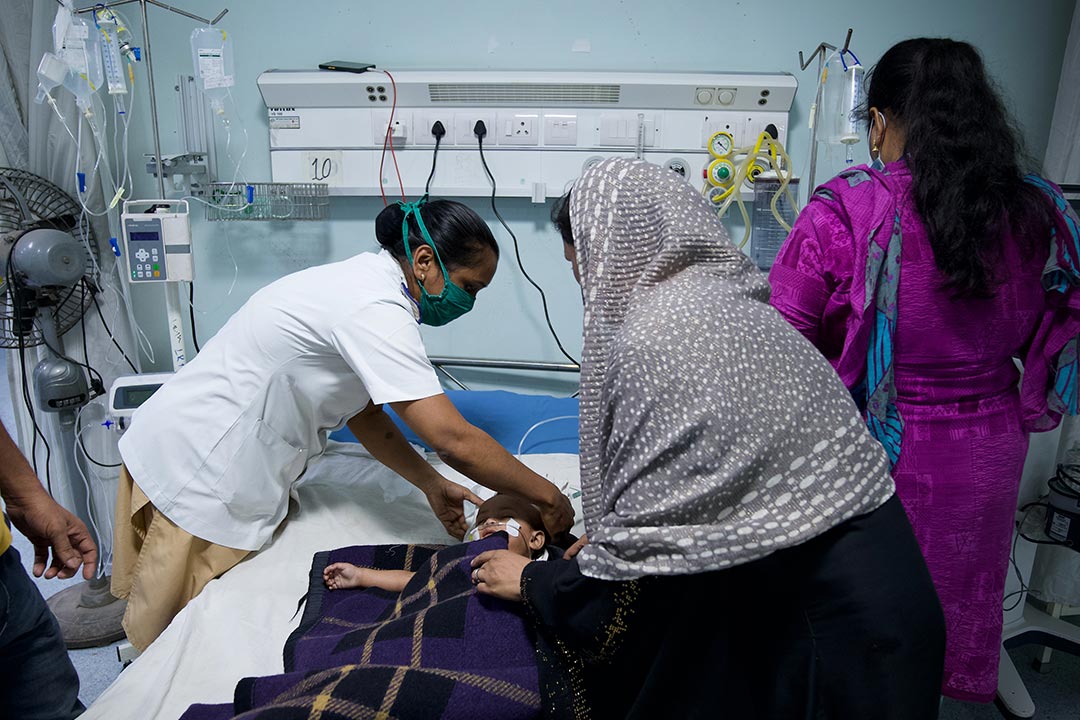
Globally, antibiotic use in hospitals has surged since the start of the COVID-19 pandemic. Even though studies show that only 8% of patients admitted to hospital with COVID-19 also have an infection requiring antibiotics, more than 70% receive them. In addition, many people worried about possible or actual COVID-19 symptoms, and alarmed by global reports about the pandemic, have turned to buying antibiotics without seeing a health-care worker.
This is further fueling the global crisis of antibiotic resistance, as bacteria evolve and become immune to these drugs. We must move quickly – with international policy, national laws, and local action – to control what the World Health Organization has identified as one of the ten leading health threats to humanity.
Antibiotics treat infections caused by bacteria, and have no impact on a virus such as SARS-CoV-2, which causes COVID-19. Overusing them merely accelerates the emergence of antibiotic resistance, which will undercut our ability to treat common diseases. Simple infections such as pneumonia or urinary tract infections, which currently can be quickly cleared by common antibiotics, may prove impossible to treat and become deadly.
This is particularly true in many African, South American, and Asian countries, where access to health-care workers is limited and there are no restrictions on antibiotic sales. In India, antibiotic sales have risen astronomically in recent years, largely driven by unregulated OTC purchases, including of unapproved drugs. Likewise, in Kenya, all antibiotics can be purchased without a prescription.
Bacteria that develop resistance to multiple antibiotics are responsible for causing difficult-to-treat infections, which are up to three times more likely to kill people than infections caused by non-resistant bacteria. And data from several countries – including China and Egypt – indicate that up to 50% of bacteria-causing infections in critical-care units are resistant to several antibiotics. In the United States, it is estimated that close to three million people get an antibiotic-resistant infection each year, leading to more than 35,000 deaths annually.
Drug-resistant bacteria are also more likely to spread from person to person, and have been known to cause large disease outbreaks in hospitals. Many COVID-19 treatment wards around the world are currently grappling with this problem.
As an infectious-disease specialist working on the COVID-19 management front line and also leading the treatment of drug-resistant infections in Kenya, I have often struggled to treat patients with severe bacterial infections that had developed resistance to all available antibiotics. Many of the recently developed drugs that could potentially treat resistant bacteria are often extremely expensive and not available in many countries. A ten-day course of one such antibiotic in Kenya, for example, costs almost $10,000, putting it beyond the reach of most patients.
In fact, many patients entering the hospital for COVID-19 treatment say that they have already taken one or more antibiotics at home in an attempt to address some of their symptoms. Often, using these drugs had made them feel that they were being treated, so they delayed going to the hospital.
Some may argue that allowing unrestricted use of antibiotics can enable access to treatment for those unlikely to be able to see a doctor, and may be cheaper for the poor. But the resulting antibiotic resistance is expensive to treat and potentially costs lives.
What must we do to forestall this next pandemic? For starters, the WHO and other global agencies must speak out much more strongly and explicitly against the use of antibiotics in cases of COVID-19, unless these drugs are specifically indicated for another bacterial infection.
In addition, national governments must tighten restrictions on OTC antibiotic purchases. Evidence suggests that introducing and enforcing laws to limit such sales can be effective if these efforts are sustained over time. Requiring pharmacies to display a notice stating that it is illegal to sell antibiotics to customers without a doctor’s prescription also has been associated with reduced antibiotic sales.
Hospitals should adopt so-called antibiotic stewardship strategies to reduce unnecessary prescriptions. These measures can lead to reduced antibiotic use and cost, and decrease the risk of antibiotic-resistant infections in hospitals. Effective strategies could include developing guidelines for managing common infections, restricting antibiotic use in viral infections, strengthening laboratory capacity – especially in low- and middle-income countries – to help clinicians identify the correct bacteria to treat, and providing continuing education for all clinicians.
Finally, individuals – despite their understandable fears of COVID-19 – should not risk harming themselves by using antibiotics unnecessarily.
The message is clear: if we do not act now to curb antibiotic use, we will invite a new pandemic. And, unlike COVID-19, no vaccine will save us.
Author
Loice Achieng Ombajo is an infectious-disease specialist at the University of Nairobi and a 2021 New Voices Fellow at the Aspen Institute.
ORIGINAL ARTICLE
This article was first published by Project Syndicate on 26 April 2021. Copyright: Project Syndicate, 2019. www.project-syndicate.org