
1. Make families aware of vaccines
Remarkably mothers who lost everything either as a result of civil conflict in the north-east or the 2005 tsunami which devastated the south, still possessed their children’s immunisation cards. “It shows their recognition for immunisation as a guarantee of a better future for their children,” says Dr Ananda.
It also demonstrates the importance of Sri Lanka’s high literacy rates with mothers and fathers highly aware of the benefits of preventive care. For example, hospitals are preferred to home deliveries. When the 5-in-1 vaccine roll-out was suspended in 2008, following reports of adverse reaction to the vaccine, the Health Ministry was rapidly able to reassure families about the vaccine’s safety. “Mothers temporarily questioned pentavalent but they never lost their faith in immunisation,” says Dr Ananda.
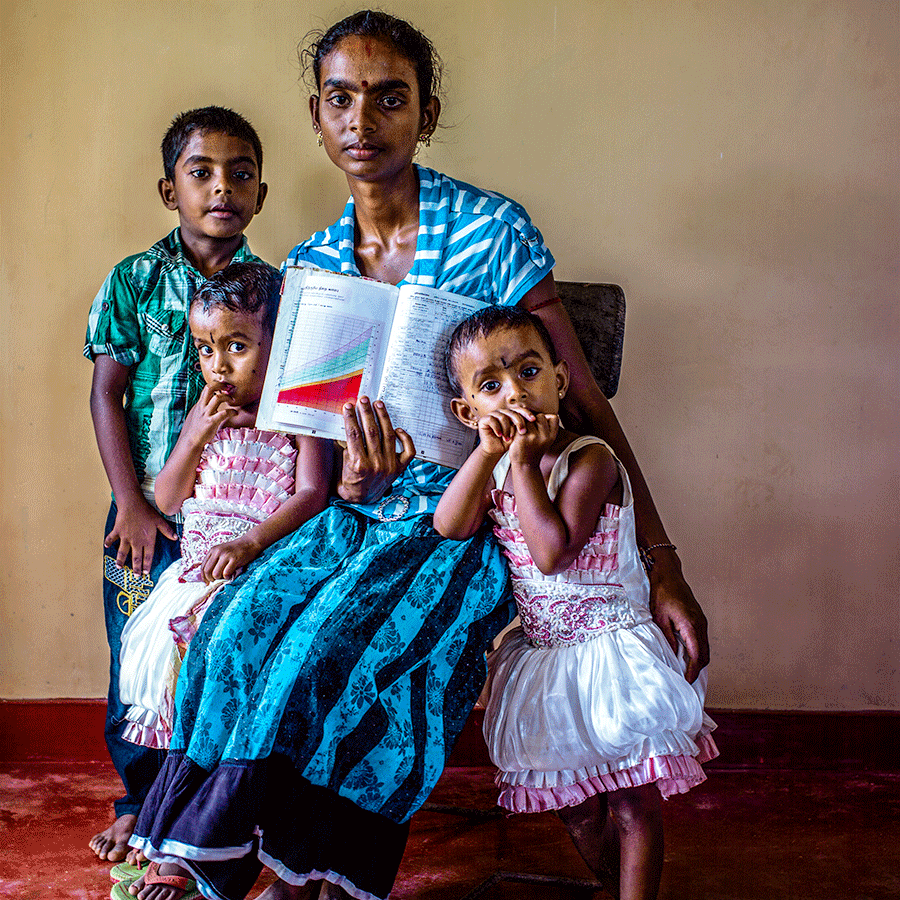
Remarkably mothers who lost everything either as a result of civil conflict in the north-east or the 2005 tsunami which devastated the south, still possessed their children’s immunisation cards. “It shows their recognition for immunisation as a guarantee of a better future for their children,” says Dr Ananda.
It also demonstrates the importance of Sri Lanka’s high literacy rates with mothers and fathers highly aware of the benefits of preventive care. For example, hospitals are preferred to home deliveries. When the 5-in-1 vaccine roll-out was suspended in 2008, following reports of adverse reaction to the vaccine, the Health Ministry was rapidly able to reassure families about the vaccine’s safety. “Mothers temporarily questioned pentavalent but they never lost their faith in immunisation,” says Dr Ananda.
2. Connect with communities
Sri Lanka’s stratospheric immunisation coverage rate owes much to a nationwide network of 4,000 community-based healthcare workers. There is approximately one health worker for every 5,000 Sri Lankans. Regular door-to-door visits, usually by bike or scooter, mean each is always up to date on their patients’ state of health.
The health workers hold regular outreach clinics raising awareness of antenatal care, immunisation and maternal and child health – and also registering every newborn child. If a mother or father fails to bring their child to a vaccination session, the health worker visits their home and, in some cases, personally accompanies the child to her clinic for immunisation.

Sri Lanka’s stratospheric immunisation coverage rate owes much to a nationwide network of 4,000 community-based healthcare workers. There is approximately one health worker for every 5,000 Sri Lankans. Regular door-to-door visits, usually by bike or scooter, mean each is always up to date on their patients’ state of health.
The health workers hold regular outreach clinics raising awareness of antenatal care, immunisation and maternal and child health – and also registering every newborn child. If a mother or father fails to bring their child to a vaccination session, the health worker visits their home and, in some cases, personally accompanies the child to her clinic for immunisation.
3. Build a top to bottom health system
Sri Lanka’s public health system, which dates back to the 1920s and the time of British rule, provides a mix of curative and preventive services at national, district and divisional levels. “Our colonial masters established a good foundation,” says Dr Ananda. It ensures a steady flow of information from grassroots communities to the Health Ministry for monitoring and evaluation. Regular updates on local immunisation coverage rates are delivered to Colombo and are often available online thanks to a new online registration system.
The system works both ways. When launching the five-in-one vaccine in 2008, the Ministry enforced a new open vial policy by meeting with 26 district immunisation managers, who, in turn, informed the 330 divisional offices. “We told them if some doses remain, don’t discard them,” says Dr Ananda. Instead of 10% wastage, the Health Ministry registered less than 1% – enough vials to provide for one month of vaccinations.

Sri Lanka’s public health system, which dates back to the 1920s and the time of British rule, provides a mix of curative and preventive services at national, district and divisional levels. “Our colonial masters established a good foundation,” says Dr Ananda. It ensures a steady flow of information from grassroots communities to the Health Ministry for monitoring and evaluation. Regular updates on local immunisation coverage rates are delivered to Colombo and are often available online thanks to a new online registration system.
The system works both ways. When launching the five-in-one vaccine in 2008, the Ministry enforced a new open vial policy by meeting with 26 district immunisation managers, who, in turn, informed the 330 divisional offices. “We told them if some doses remain, don’t discard them,” says Dr Ananda. Instead of 10% wastage, the Health Ministry registered less than 1% – enough vials to provide for one month of vaccinations.
4. Secure political support
Even during the civil conflict, temporary ceasefires allowed hospitals and clinics to deliver immunisation and other basic health services. Successive Sri Lankan administrations have also prioritised free health and education.
In 2014, the Government introduced a national immunisation policy guaranteeing every citizen the right to vaccination. There is a separate line in the national budget for immunisation ensuring continuity in the delivery of vaccines and virtually no stock-outs. “It is the responsibility of our people to get vaccinated so the Government guarantees the availability of vaccines,” says Dr Ananda.

5. Invest in long term training
To ensure the long-term sustainability of its immunisation programme, the Health Ministry invests in training future generations of public health inspectors and health workers at six regional training centres and one national centre. “No matter how many clinics you build, you can’t provide services without trained resources,” says Dr Ananda, “We want our successors to do even better than us.” Since the end of the civil conflict in 2009, the training centre at Vavuniya in the north of Sri Lanka has trained over 600 health workers to help rebuild the health system in the former conflict zone.
Under the colonial administrative system, all government officers learnt their trade in rural areas before moving to the major cities. Today, Sri Lanka’s public health staff must also gain extensive experience working at divisional then district levels before moving to the Ministry in Colombo. “Before we come to the centre, we need to know the reality on the periphery,” says Dr Ananda.
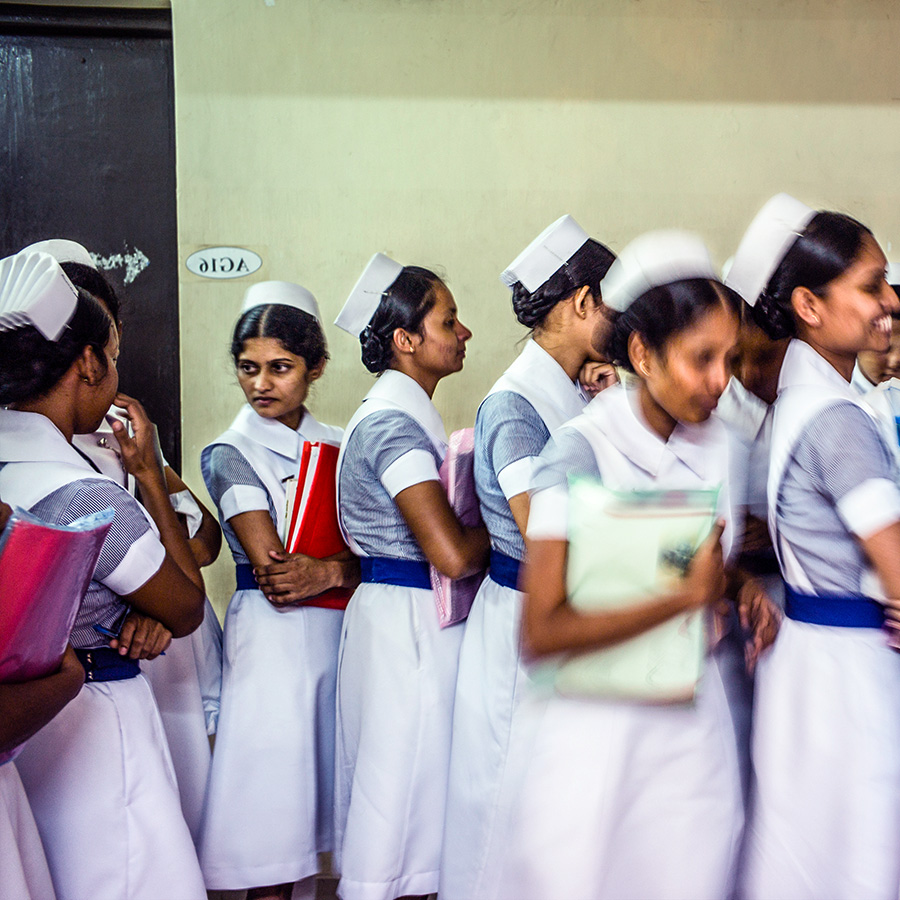
To ensure the long-term sustainability of its immunisation programme, the Health Ministry invests in training future generations of public health inspectors and health workers at six regional training centres and one national centre. “No matter how many clinics you build, you can’t provide services without trained resources,” says Dr Ananda, “We want our successors to do even better than us.” Since the end of the civil conflict in 2009, the training centre at Vavuniya in the north of Sri Lanka has trained over 600 health workers to help rebuild the health system in the former conflict zone.
Under the colonial administrative system, all government officers learnt their trade in rural areas before moving to the major cities. Today, Sri Lanka’s public health staff must also gain extensive experience working at divisional then district levels before moving to the Ministry in Colombo. “Before we come to the centre, we need to know the reality on the periphery,” says Dr Ananda.
The Health Ministry knows what to do to make vaccines work for their citizens – their challenge now is maintain success by keeping prices fair for future vaccine purchases. “That is where Gavi can help,” says Dr Ananda, “We wish to rely on ourselves – we have the money and can procure the vaccine. But with our small population, we are not in a position to bargain with the manufacturers. That is what we now ask of international organisations: can you help as a negotiator?”





