All photos: Sam Phillips/Gavi.

As one of the first countries in south east Asia to introduce the pneumococcal vaccine, Nepal’s immunisation system is under the microscope with many countries hoping to learn from their neighbour’s experience.
Scientists at Patan Hospital’s Academy of Health Science in Kathmandu (above) are conducting a series of surveillance studies which will not only shape how pneumococcal vaccine is delivered in Nepal but across the rest of southeast Asia.

“Nepal is one of the first countries to introduce pneumococcal vaccine in south east Asia, so our studies could be very useful to our neighbours,” says Shrijana Shrestha, Dean of the Academy of Health Science.

Nepal has introduced two vaccines into its routine immunisation schedule to protect children from the primary causes of severe pneumonia: in 2008, Haemophilus influenzae type b (Hib) vaccine and, this year, the pneumococcal vaccine.

Pneumonia is the biggest killer of children under-five in Nepal, especially in winter when children inhale soot from wood-burning stoves used to heat cramped living quarters. High levels of air pollution also aggravate respiratory infections.

Patan’s chief paediatrician, Dr Imran Ansari, explains that some children on his ward have required intensive care to survive severe pneumonia. “This is a very bad experience for a doctor, both as a professional and as a person.”
“Pneumococcal disease has not been studied in our population before” he continues. “It is important to know what bugs are more common in this part of the world, so we can have vaccines that prevent these bugs.”
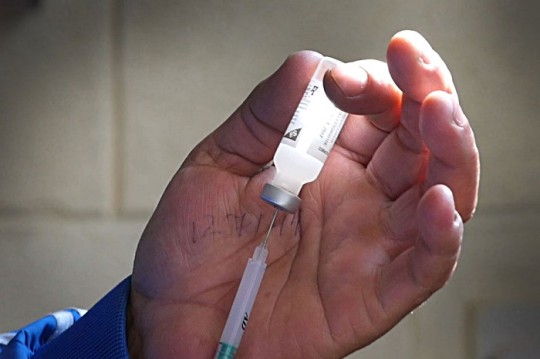
On average, Patan Hospital’s paediatric wards treat 500 cases of severe pneumonia every year – 25-30 percent of all children admitted to the hospital every year.
In most developing countries, pneumococcal vaccine’s three doses are given after six, 10 and 14 weeks of a child’s life. Patan surveillance showed delivering the third dose as a booster after nine months gave Nepalese children better protection through to the age of five. “This encouraged the Nepalese Government to change pneumococcal vaccine’s introduction schedule,” says Shrestha.

With collaboration from the University of Oxford in the UK and New Zealand’s Otago University, as well as funding from Gavi, Patan Hospital has also started studying the impact of pneumococcal vaccine on children’s health.
Another study will assess the long-term economic value of reducing the number of hospitalisation cases. When children in low-income countries are admitted to hospital, family members often lose income to look after them.

While a study on the impact of Nepal’s introduction of Hib vaccine has yet to be published, Dr Ansari has already reached his own conclusion. “It’s our impression that in the last few years probably after the introduction of Hib vaccine, such cases of severe pneumonia are in decline.”
This gallery was originally posted on the Gavi website.






