Cervical cancer can be beaten - the key is vaccinating young girls
Cervical cancer is one of the most common cancers in women. Mortality rates in sub-Saharan Africa are three times higher than the global average.
- 11 April 2023
- 6 min read
- by The Conversation
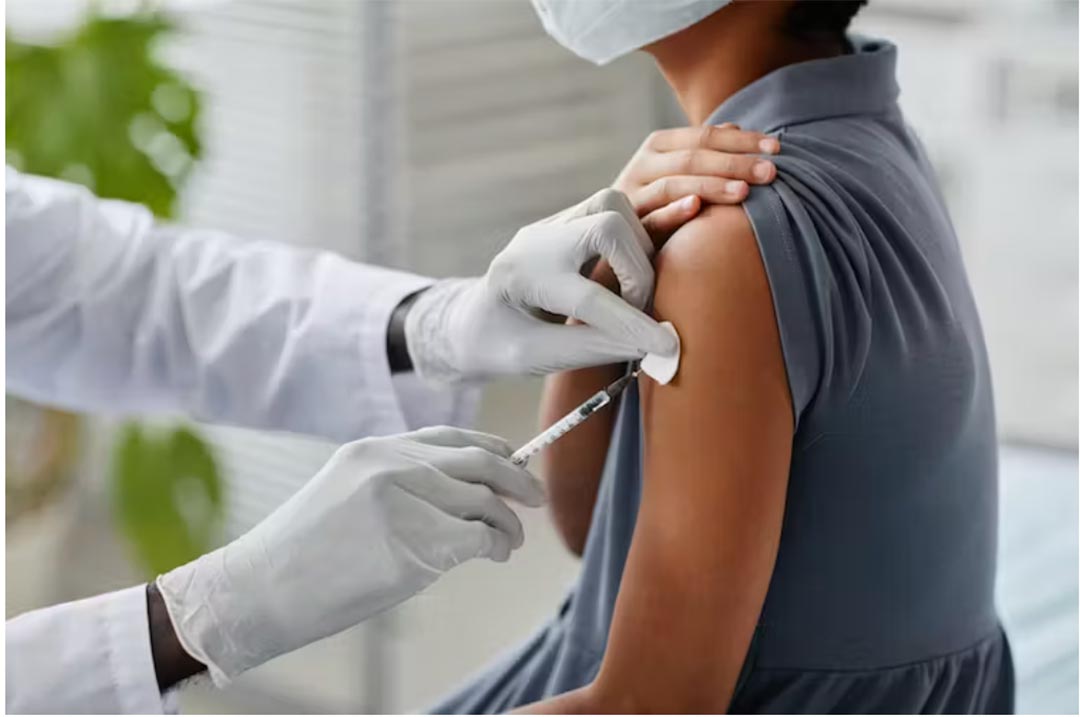
In 2020 the World Health Organization introduced a plan to eliminate cervical cancer as a public health threat by 2030. The first step towards this goal is to have 90% of girls fully vaccinated against human papillomavirus (HPV) by the age of 15 years. Gynaecological oncologist Lynette Denny spells out how much progress still needs to be made, and what hurdles need to be overcome.
How big a threat is cervical cancer in sub-Saharan Africa?
Cervical cancer is one of the most common cancers in women. Sub-Saharan Africa has the highest cervical cancer diagnoses worldwide. Cervical cancer mortality rates in the region are three times higher than the global average. The burden of HIV in sub-Saharan Africa contributes to the disparity. In 2021, in southern Africa, 63.8% of women with cervical cancer were living with HIV, as were 27.4% of women in eastern Africa.
Most cases of cervical cancer are caused by the human papillomavirus (HPV), which is transmitted through skin to skin contact, including sexual activity.
How do countries compare in meeting the WHO target?
By June 2020, more than half of the WHO member states – that’s 107 out of 194 – had introduced HPV vaccination nationwide or partially.
The numbers showed a wide variation in coverage in different geographic regions. High-income countries such as Australia and New Zealand had the highest complete coverage with HPV vaccination at 77%. Low- and middle-income countries lagged far behind – only 41% had introduced HPV vaccination by the end of 2019. Only 20% of the eligible population in sub-Saharan Africa has been vaccinated.
Levels of vaccination matter because, with wide coverage of the appropriate age group, over time it is theoretically possible to eliminate HPV as a human pathogen. This was the case with smallpox.
Most (90%) of low- and middle-income countries deliver vaccination through schools and facility-based vaccination. The two-dose schedule is the most common. When the HPV vaccine was initially approved for use, it was given to girls aged 9-13 in three doses. Dose one intially; dose two at one or two months after the first dose; and a third dose six months later.
It later became evident that two doses gave the same level of immunity as three doses.
It is now recognised that one dose is as good as three doses in preventing HPV infection in the general population. In April 2022 the WHO Strategic Advisory Group of Experts on Immunisation concluded that a single-dose HPV vaccine delivers “solid protection against HPV, that is comparable to two-dose schedules”. However, they recommended that people living with HIV continue to receive three doses where feasible, and if not, at least two doses, due to the limited evidence.
The lower number of doses has important cost and logistical implications. Administering one dose may be a game changer in widening the coverage of eligible girls. In South Africa, the dropout rate from the vaccination programme after the first vaccination in 2014 was 18% and it increased to 26% in 2018 and 2019. The equivalent dropout rate in high-income countries averages 11%.
Have you read?
In 2019, 33 of the 107 HPV vaccination programmes were gender neutral – both girls and boys were being vaccinated. Vaccinating both boys and girls will increase what is known as herd immunity, which means that the prevalence of HPV in the population will decrease. In addition, boys will be protected from HPV associated anal, penile and oro-pharyngeal cancers. However, including boys in vaccination programmes when most girls aren’t vaccinated is not cost-effective.
Globally, it was estimated in 2019 that 15% of girls and 4% of boys were vaccinated.
What’s the surest way of achieving the WHO goal?
There are many important steps.
A critical starting point is to gain political support for HPV vaccination. There needs to be high level collaboration between the ministries of health, education, social development and existing immunisation programmes.
The most successful programmes have used school-based facilities for vaccination. But this excludes adolescents who are not in the school system, hence the need to create facility-based programmes.
Widespread information and population education is critical - education campaigns should include parents, the general population, teachers and healthcare workers.
An adequate supply of vaccine is crucial and the vaccine administration infrastructure must be robust. All the logistics of vaccine implementation, such as distribution, cold chain management, waste control and clinical care must be attended to. Good statistics and information should be maintained and monitored regularly.
Anti-vaccination programmes need to be monitored and their allegations responded to promptly and with cultural sensitivity.
What are the hold-ups?
COVID has had a major impact on many HPV vaccination programmes. Low- and middle-income countries were particularly hard hit. As an example, the South African programme coverage reduced from 85% when introduced in 2014 to 3% in 2020. The programme is still trying to recover.
Along with the impact of COVID on immunisation practices, the recommendation to include boys and older women in vaccination programmes resulted in a worldwide shortage of HPV vaccines. The shortage was recognised in 2020 and was predicted to last three to five years. A statement released by the International Papillomavirus Society recommended that gender neutral vaccination as well as that of older women be temporarily suspended. And that, during the supply constraint, HPV vaccination should be reserved for girls aged 9 to 14.
What should countries be focused on?
Current commercially available HPV vaccines are prophylactic. They will protect individuals who have never been exposed to HPV infection from being infected, and prevent 70%-90% of all cervical cancers. (No vaccine is 100% effective.)
I have spent the past 30 years researching safe, feasible and effective alternatives to the Pap smear for the prevention of cervical cancer. When I began this work in 1995, the HPV vaccine had not yet been produced. Its arrival made the possibility of ending cancer associated with HPV infection a reality.
Who gets vaccinated should depend on age, gender and resources. Girls aged 9-14 years should be prioritised. As resources increase, girls aged 15-18 years should be included. Thereafter, women aged 19-26 years should be included. Vaccinating boys should go ahead only once at least 90% coverage has been achieved in girls aged 9-14 years.
Vaccinating older women, most of whom would already have been exposed to HPV infection (even if subsequently cleared) should be reserved for high resource settings that have reached widespread vaccination coverage.
There are many advantages to vaccinating boys, particularly in preventing HPV-associated cancers in men and in men who have sex with men, as well as increasing herd immunity. However, expanding the programme to include men has implications for resource distribution and possible exclusion of other vulnerable groups.![]()
Authors
Lynette Denny, Professor, Special Projects, Obstetrics & Gynaecology, University of Cape Town

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Lynette Denny receives funding from National Institutes of Health, USA
Partners
University of Cape Town provides funding as a partner of The Conversation AFRICA.








