COVID-19: Q&A
With zero cases of COVID-19 in Mozambique so far, Dr Rosa Marlene, National Director of Public Health of Mozambique, discusses a potential impact that a pandemic of this magnitude could have on the country’s health system.
- 19 March 2020
- 4 min read
- by Gavi Staff

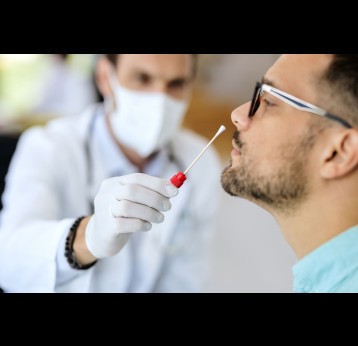
Mozambique hasn’t yet had a case of COVID-19 in the country: how prepared are you?
We are closely monitoring the situation in Italy, South Korea, China and other countries where the outbreak is currently hitting the hardest. Even though we haven’t yet had a case of COVID-19 in Mozambique, we want to be ready if it does eventually reach our country.
This is a very serious public health concern for Mozambique authorities. The outbreak is currently mainly in countries that have strong health systems and the resources to respond, as well as the means to identify cases and treat people infected. One of our greatest challenges will be ensuring the protocols and tools are in place here to help us contain and manage it if the virus does reach here.
What are you doing in terms of public health measures to prevent the pandemic in Mozambique?
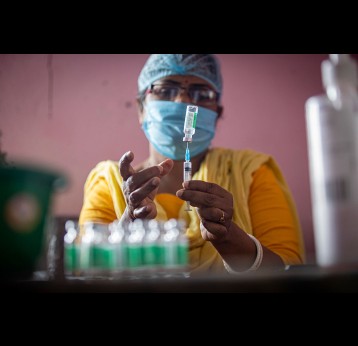
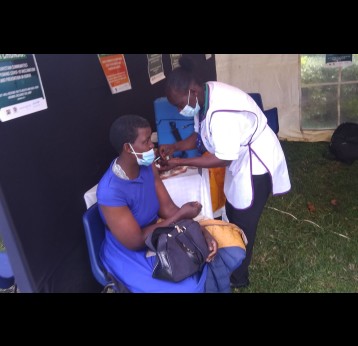
All points of entry to the country are now operating a screening process. Additional screening is given to travelers from affected areas. It is important to note that Mozambique and other countries in Africa have had to deal with pandemics for as long as I can remember, and, while COVID-19 is extremely worrying, we cannot lose sight of other issues in our country, such as cholera, pneumococcal disease and measles. It is absolutely essential therefore that we ensure that routine immunisation services continue and that people in Mozambique, and other countries, are protected from diseases that can be prevented by vaccines.
What, in your opinion, would be the biggest challenges for Mozambique to address the COVID-19 outbreak?
Our overall response capacity is not the same as that of the countries in Europe, therefore one of the biggest challenges for Mozambique would be the capacity of our health systems to cope with the influx of sick people to hospitals and clinics. Not only that, but our health workers have demonstrated incredible heroism and resilience when addressing the cholera outbreak following Cyclone Idai in March last year, and they will be the first ones at risk of COVID-19 as frontline responders to the outbreak. We must keep that in mind. While the number of health workers has increased in Mozambique over the last decade, we will not be able to deliver treatment and services, should they be affected by the virus.
Geography is also a challenge. There are communities that do not have access to a clinic or where the nearest health facility is 20km away. For these communities, even a small outbreak can have a devastating impact. People in these areas are usually the most vulnerable and so we must prioritise reaching them with support.
How can the leaders of countries that are currently experiencing the pandemic help you prepare?
The biggest help we need, and what is already being done, is information sharing. This has been unprecedented; we are able to monitor the situation as it develops in countries in Europe and Asia. The hope is that if the outbreak hits Mozambique severely, there will already be clinical information on transmission and best treatment, which we can use here to contain the spread of the virus.
What can the global health community do to support countries like Mozambique in addressing the coronavirus outbreak should it severely hit countries in Africa?
If COVID-19 teaches us anything, it is that a major outbreak in a country with a weak health system can be a real disaster, and we must all work together to prevent the virus from spreading further. Countries like Mozambique do not have the same resources as wealthier countries in Europe and Asia to tackle the outbreak, therefore funding and technical support for the health systems strengthening from the global health community must continue.
Is there anything the countries hit hardest by coronavirus can learn from Mozambique, given your experience in combatting outbreaks?
When an outbreak hits, we must do everything possible to contain it – that should be our priority. However, we are a small country with a very stretched health system at the best of times. Often, we have to deal with more than one serious disease outbreak. Despite the challenges this presents, we have learned that we must find ways to continue to provide routine health services to the population, making sure that people get the necessary treatment and children are protected against vaccine-preventable diseases through immunisation. We know that should those services stop, we might be facing an even greater toll due to the collateral damage wrought on our already strained health infrastructure.