Fading from global headlines, mpox continues to trouble its ‘cradle’ – DRC
“The fear of mpox looms over us daily,” health workers in Kinshasa say.
- 13 November 2023
- 4 min read
- by Larissa Diakanua
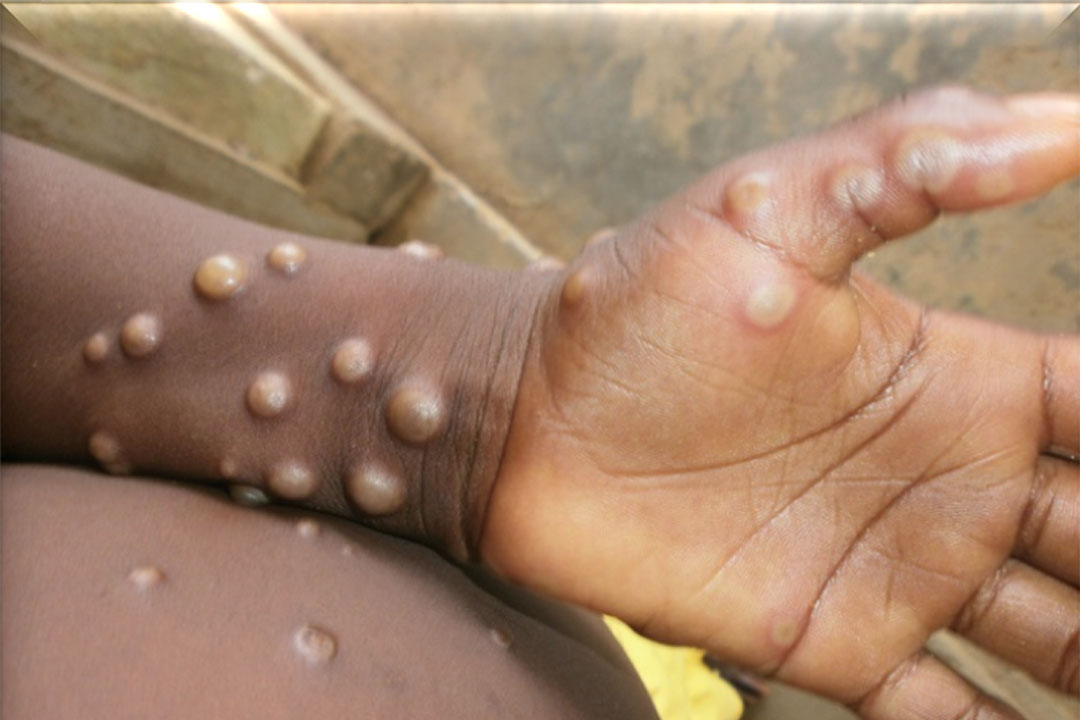
Mpox, formerly known as “monkey pox” , was first identified in humans in the Democratic Republic of the Congo (DRC) in 1970, and until 1986, 95% of mpox cases reported globally came from the central African country. That pattern has changed over the last three decades, with outbreaks cropping up elsewhere in Africa and further afield, and with the viral infection most dramatically bursting its habitual boundaries during the 2022 to 2023 global outbreak.
“The fear and stigma associated with mpox have hindered our efforts. People are hesitant to seek medical attention, and misinformation spreads rapidly.”
Unnamed health worker and mpox survivor, Kinshasa
That global outbreak has pulled focus from mpox-endemic countries, but DRC continues to struggle with a hefty mpox burden.
This year alone, the disease has spread to various provinces, reaching 159 out of 519 health zones in the country. On 25 August 2023, Dr Robert Shongo, Director of the Program for the Fight against Monkeypox and Endemic Viral Fevers, told reporters that the DRC has recorded 6,914 cases of mpox disease including 328 deaths (4.7%) since the start of the year. The most affected provinces have been Equateur, Mai Ndombe, Tshopo, Sankuru, and Maniema provinces, he said.
Ripples of anxiety
Behind those figures are communities struggling under a complex social and epidemiological pressure.
Mpox, which causes fevers and scabbing rashes, progressing to death in a minority among severe cases, is a visible and consequently easily stigmatised viral disease.
Local community members and health workers who have witnessed the disease’s devastating effects have been psychologically affected. A health worker in Kinshasa who has been hospitalised with the disease explained, “The fear of mpox looms over us daily. We've heard stories about people dying across the country and it was emotionally hard to handle.”
He continued: “The fear and stigma associated with mpox have hindered our efforts. People are hesitant to seek medical attention, and misinformation spreads rapidly.”
“Hospitals in some of the most affected areas are at capacity due to the presence of other epidemics, and medical professionals are working tirelessly to provide care.”
Dr Roy Ndenge, surveillance agent with the DRC mpox programme
Overlapping health challenges
Meeting the challenges presented by the mpox epidemic in DRC is not easy. For one, the viral infection is just one among several large-scale health emergencies, including recurrent epidemics of measles, yellow fever and other life-threatening illnesses.
Insecurity, health system limitations and logistical constraints limit access to care for the population. The country extends over a vast territory, and its geography imposes challenges to the work of humanitarian and health teams. It sometimes takes several days to reach remote villages in certain regions. While WHO recommends a ratio of 1 doctor per 1,000 people, DRC has only about 0.09 doctors per 1,000 inhabitants.
Have you read?
With limited resources, the system struggles to meet the demands of an escalating crisis. Dr Roy Ndenge, a surveillance agent with the national programme tasked with curtailing mpox, told VaccinesWork, over the phone in October: “Hospitals in some of the most affected areas are at capacity due to the presence of other epidemics, and medical professionals are working tirelessly to provide care.”
Containment efforts
In Kinshasa, where a few cases were reported in August, five mpox patients had been recently released from hospital, Ndenge said. Those cases included three people who had been transferred to hospital in the capital from Maindombe province in August, and two “contacts” that had fallen sick in Kinshasa.
The response to mpox has evolved over time. Early in 2023, containment efforts were met with logistical challenges, including vaccine distribution and healthcare infrastructure limitations. In the beginning, health staff faced shortages of essential supplies and vaccines. However, current efforts have seen improvements, with international organisations and NGOs stepping in to provide crucial support. Said Dr Ndenge, “The assistance from NGOs like Médecins Sans Frontières (MSF) has been instrumental. We now have better access to supplies, and our teams are more equipped to handle cases.”
Dr Thomas Holebanga, Medical Activity Manager at MSF’s Congo Emergency Pool (PUC) said before the arrival of MSF teams in August 2023, the health zone of Bolomba in the Equateur province recorded the most cases of illness, and many deaths. That was due in part, he explained, to technical, logistical, financial limitations, as well as to socio-economic factors among the affected communities, including poverty, promiscuity or ignorance of the disease.
Beyond putting in place infection prevention and control measures in health structures, MSF also implemented a home isolation strategy, he said, which allowed patients without complications to be treated in their houses. A hygiene kit was provided to them and their loved ones with advice on the use of these kits in order to cut the chain of transmission.
Regular monitoring of these cases was carried out by MSF teams with the support of community workers. “All of these strategies have made it possible to significantly reduce the number of cases and deaths”, said Dr Holebanga. “From 1,781 cases and 216 deaths reported as of August 2023, the number of cases went to 891 and 4 deaths in October.”
Meanwhile, the World Health Organization (WHO) is raising awareness and mobilising resources for the response as part of the “One Health” approach.








