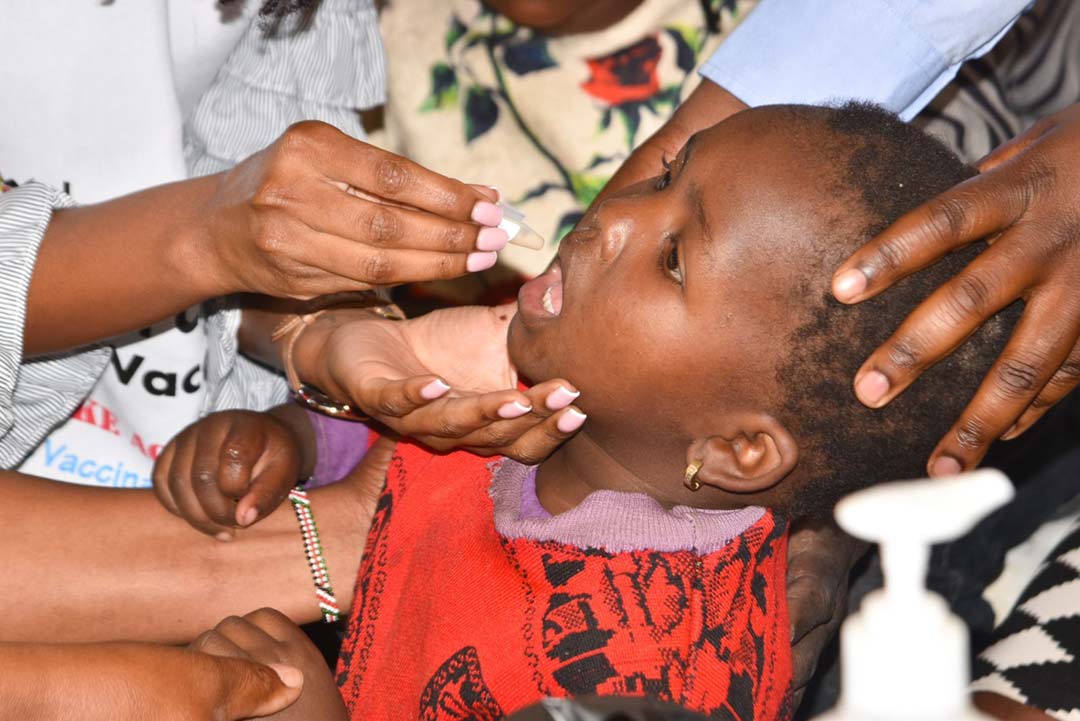
Hope spreads as 18 million doses of the first malaria vaccine are allocated to 12 African countries
Following a landmark announcement by Gavi, UNICEF and the WHO this week, 12 African countries will begin to roll out the RTS,S/AS01 vaccine as part of their routine immunisation schedules. Tens of thousands of children are expected to be saved each year.
- 7 July 2023
- 6 min read
- by Mike Mwaniki , Maya Prabhu
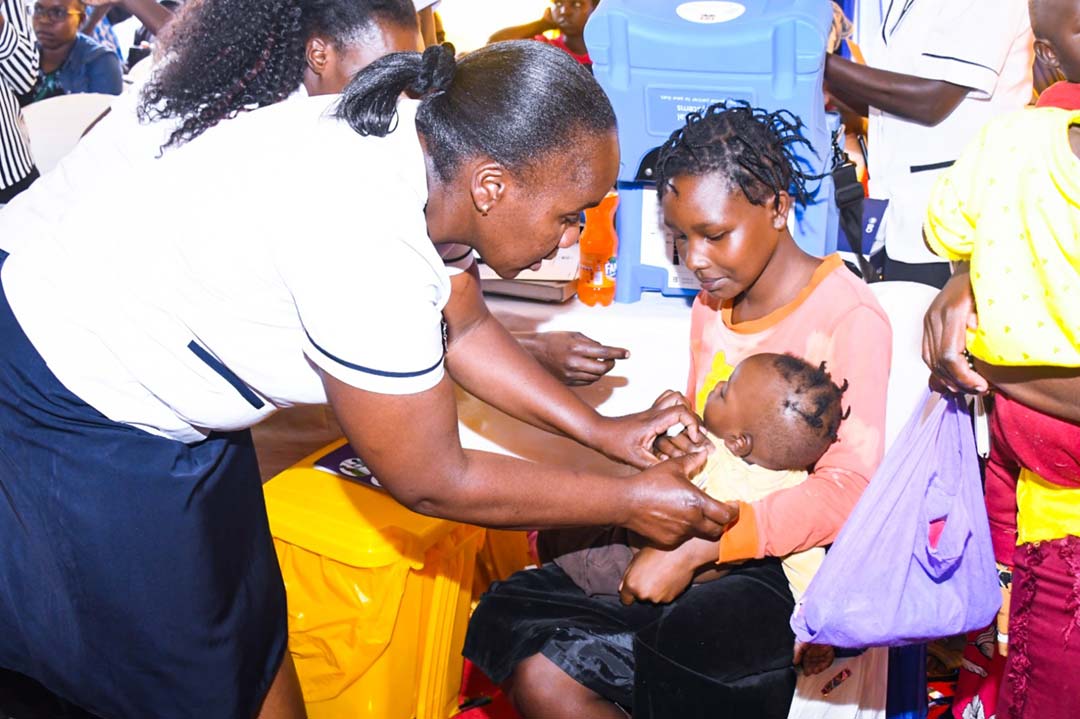
Irene Mideva from Vihiga County in western Kenya lost two children in the space of three months in 2004. The cause of death in both cases was malaria, a mosquito-transmitted parasitic infection that killed 1.8 million people worldwide that year, and an estimated 619,000 people in 2021.
The vast majority of malaria deaths occur among African children aged under five. In Vihiga County, part of the so-called "Lake endemic region" – a wet and mosquito-thronged zone surrounding Lake Victoria – the threat of malaria has historically been feverishly high. "Previously, most of our hospital beds in this county had a high number of patients, a majority suffering from malaria," recalled health worker Janet Atieno.
Rolled out widely and used well, the vaccine is expected to prevent tens of thousands of deaths every year.
But that risk profile has shifted since the world's first malaria vaccine began to roll out here as part of a pilot programme run in Kenya, Malawi and Ghana since 2019. "Since we introduced the vaccinations, we are now experiencing a drastic reduction of malaria in-patients, especially among children in this region," Atieno said.
"The Lake endemic region has particularly seen a drop in malaria prevalence from 27% in 2015 to 19% in 2020, showing that our efforts in malaria prevention and control are bearing fruit," confirmed Dr Patrick Amoth, the Health Ministry's Acting Director General, in March.

Credit: Mike Mwaniki
He was speaking at an event that marked the expansion of Kenya's malaria vaccination drive to 25 additional sub-counties in the Lake endemic region, good news that was greeted with a mixture of hope and regret by Mideva, whose thoughts turned back to her losses of nearly 20 years ago. "I wish the malaria vaccine had been introduced then," she said. "I believe their young lives could have been saved."
A mother of four today, Mideva was resolved that her surviving children should benefit from the RTS,S/AS01 jab: "I will ensure all my children complete the four doses as recommended by health officials."
Following an announcement this week by Gavi, UNICEF and WHO, families not just in Kenya, but in 12 African countries – the three pilot countries and nine more nations – will gain access to the same revolutionary shot at life, as the breakthrough malaria vaccine enters routine immunisation programmes for the very first time.
Who gets malaria vaccines?
These 18 million first doses will provide for the shift into the routine immunisation schedule of the RTS,S/AS01 malaria vaccine in 12 highly at-risk African countries.
A total of 6.9 million doses have been earmarked for Ghana, Kenya and Malawi, where the vaccine has been piloted since 2019, for the period 2023-2025.
A further 10.5 million doses will furnish the needs of Benin, Burkina Faso, Burundi, Cameroon, Democratic Republic of the Congo, Liberia, Sierra Leone and Uganda in the same period. Niger has been offered a partial allocation of 565,000 doses.
The 18 million doses allocated in this first volley are expected to start arriving in countries in the final quarter of this year, and roll-outs are anticipated to kick off in early 2024.
Have you read?
This highly sought-after first tranche of RTS,S/AS01 vaccines have been allocated following a two-stage principle: firstly, that the vaccines should go where the risk is gravest, and secondly, where the health system is best able to ensure their effective delivery.
"While we work with manufacturers to help ramp up supply, we need to make sure the doses that we do have are used as effectively as possible, which means applying all the learnings from our pilot programmes as we broaden out to a new total of 12 countries," said Thabani Maphosa, Managing Director of Country Programmes Delivery at Gavi.
Why those 12 countries?
In an ideal world – one which Gavi is working towards – everyone who is at risk gets access to the vaccine. But unfortunately, demand currently outstrips supply by a hefty margin, which means the available doses have needed to be triaged.
That triaging was conducted by a group of experts that included representatives from the Africa Centres for Disease Control and Prevention (Africa CDC), UNICEF, WHO and the Gavi Secretariat, as well as voices from civil society and independent advisors. They applied ethical priority principles articulated in the "Framework for the allocation of limited malaria vaccine supply" as they assessed applications.
The aim was that the vaccines would:
- Go where the need is greatest: in other words, where the malaria burden and risk of death from malaria are highest
- Maximise health impact: RTS,S/AS01 is given on a four-dose schedule, with little protection expected from just one or two doses. That means a key consideration for allocation was that the vaccine should go to countries who were likely to reliably get all four doses to the target population. A proxy measure for that ability to deliver for maximum impact was the drop-out rate between the third dose of diphtheria, tetanus and pertussis containing vaccine (DTP3) and the first dose of measles-virus containing vaccine (MCV1), which is usually given at nine months – i.e. the point at which the third dose of the malaria jab is expected to be administered.
The first two principles being satisfied, the Framework says that vaccines should:
- Be distributed equitably: priority goes to countries that commit to fairness and inclusion
- All else being equal, go to countries with a prior contribution to the vaccine's development.
NB: The three countries that were part of the MVIP pilot were given priority access under the Framework "to ensure continuity of services, sustained trust in the EPI and fairness for communities who are participating in the pilot evaluation". MVIP areas are covered through 31 December 2023 with doses donated by GSK .
The vaccine is safe, and effective against Plasmodium falciparum, the most dangerous malaria parasite in the world, which is responsible for more than 90% of deaths from the disease annually. As the world's first protective anti-parasite vaccine, RTS,S was a scientific leap forward before it ever rolled out.
But it's not a perfect shield. Phase three clinical trial data showed that when the vaccine was administered among children aged 5–17 months at first vaccination, it resulted in a 36% drop in clinical cases. Administered in four doses – at six months, seven months, nine months and two years, it's estimated to save one life for every 200 children vaccinated.
That means the vaccine needs to be deployed at scale, and in concert with other anti-malaria interventions to deliver on its world-changing potential. Explained Dr Deen Omar, Division Head for Kenya's National Malaria Programme, "we are cognisant of the fact that a combination of tools, including long-lasting insecticide-treated nets, indoor residual spraying and malaria chemoprevention strategies are needed, along with the malaria vaccine to combat malaria."

Credit: Mike Mwaniki
Kenya has so far administered more than 1.1 million doses of the vaccine to close to 400,000 children under five, and is targeting more than 134,000 children annually in the Lake endemic region. "We will continue to expand availability of the vaccine beyond 2023 by applying – along with other countries – for support from Gavi, for subnational use of the vaccine in areas of greatest need," said Dr Lucy Mecca, the Health Ministry's Head of National Vaccines and Immunisations at a media breakfast in Nairobi in March.
Rolled out widely and used well, the vaccine is expected to prevent tens of thousands of deaths every year. Demand for malaria vaccines is estimated to reach 40–60 million doses for the year 2026, rising to as many as 100 million doses a year by 2030.