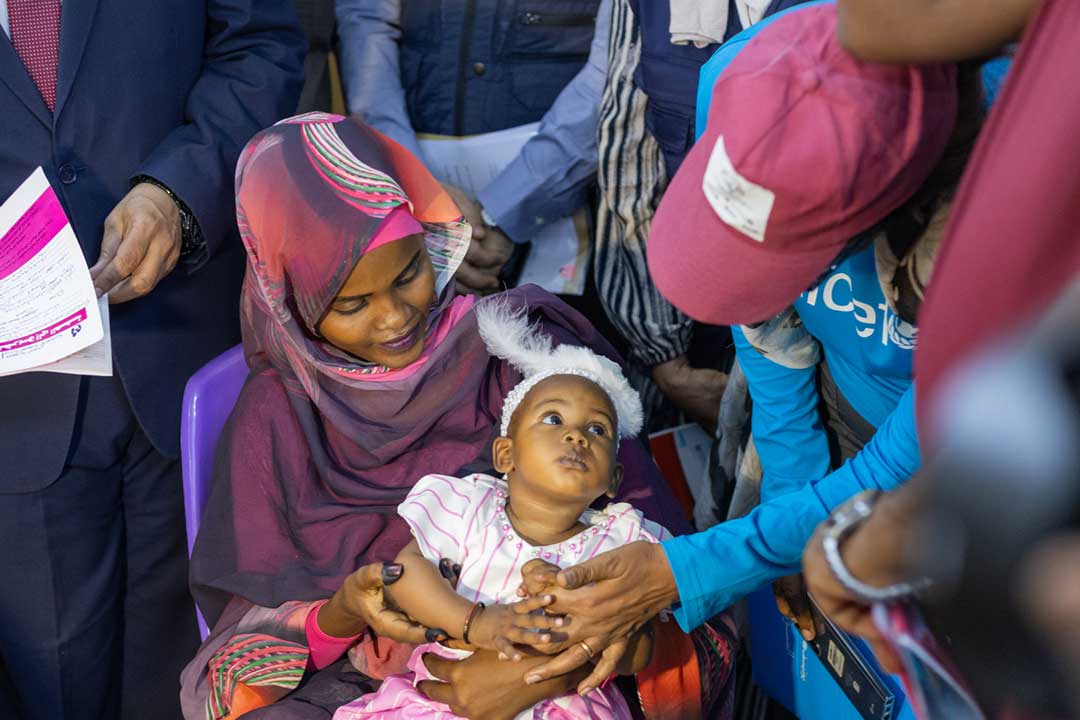
Malaria bites: health workers in 80 countries share their experiences
As two malaria vaccines begins to roll out in many countries, health workers reflect on their experiences of the parasitic killer.
- 12 June 2024
- 8 min read
- by Ian Jones

Great swathes of the world are affected by malaria, with the severest impacts felt in sub-Saharan Africa. It's an often repeated statistic: malaria kills nearly half a million children a year. As sobering as that fact is, such blunt figures do little to give insight into the remorseless toll that malaria takes on families.
In advance of Teach to Reach 10, the peer-learning event being held by the Geneva Learning Foundation (TGLF) on 20–21 June 2024, over 21,000 registrants were invited to share how malaria had affected their lives and local communities, and the challenges they face dealing with it.
The participants in question are health workers, primarily from districts and facilities in over 80 countries across Africa, Asia and Latin America. Half are government employees, the other half from civil society.
Many described how family members – young children, and older people alike – had been lost to malaria.
"As a community health worker in a rural area in Nigeria, I've seen first-hand the devastating impact of malaria on individuals, families, and communities. Unfortunately, I have experienced the pain of losing children to malaria. Despite my best efforts to protect them, they succumbed to the disease. Since then, I've dedicated my life to fighting malaria and ensuring that no other parent goes through what I went through."
– Lucy Pam Dangyang, Public health professional, Bokkos LGA, Plateau State, Nigeria
"Malaria almost took the life of my husband and two kids. I suffered in nursing them at the hospital – from February to April this year was tough for me and my family. I was the only strong person that was not infected with Plasmodium [falciparum]."
– Rebecca Bello, Public Health Scientist, Dobi community Gwagwalada Abuja, Nigeria
In their responses, health workers recalled childhoods punctuated by episodes of the disease.
"Growing up in a malaria-endemic region, malaria has had a profound impact on my life and my family. I have witnessed first-hand the debilitating effects of the disease. When I was a child, my younger brother contracted malaria multiple times, leading to numerous hospital visits and long periods of missed school. These experiences were not only distressing but also financially draining for my family, as medical costs piled up and my parents had to take time off work to care for him."
– Joseph Mbari Ngugi, Public health specialist, Ministry of Health, Kenol, Murang'a County, Kenya
"Malaria has ravaged my community, affecting my family, friends, and neighbours. I've lost count of how many loved ones I've lost to this disease. Growing up, I saw my mother struggle to access health care during her pregnancies. She contracted malaria multiple times, which led to complications and even miscarriages."
– Ibrahim Lawan, Public health specialist, Red Cross Red Crescent Movement, Zakalio/Babale, Nigeria
Respondents also shared vivid details of what a bout of malaria actually feels like.
"Malaria has greatly affected myself and my family. I don't often get infected with malaria, but the few times I was down with malaria, I couldn't go to work, I couldn't cook for my children, I was weak and vomiting profusely."
– Rachel Aniniwaa Addo, Public health specialist, Ministry of Health, Yilo Krobo Municipality, Ghana
"As a child, I vividly remember the panic that would set in whenever someone in our community fell ill with the tell-tale symptoms – the relentless fever, the chills, the excruciating headaches. My own grandmother was one of the many victims claimed by malaria. I can still picture her frail body wracked with the infection, as my family scrambled to find the limited antimalarial drugs available at the time. Tragically, despite our efforts, she succumbed to the disease when I was just ten years old."
– Bwango Benjamin Mukaapa, Public health specialist, NGO, Fort Portal City, Uganda
For many households, malaria is an omnipresent threat. Sickness is not only deeply unpleasant for those affected, but also robs children of time in school, delaying their educational and physical development, and can have severe economic consequences for adults, who may be unable to work because they are too ill or are looking after sick children or relatives.
"The economic toll has been staggering. Time and time again, my parents and other relatives have had to miss work or scale back their small businesses when struck by malaria. The medical expenses, coupled with lost wages, have pushed our family deeper into poverty, making it even harder to access the prevention and treatment resources we so desperately need."
– Bwango Benjamin Mukaapa
Even during periods without sickness, the fear of malaria can be debilitating.
"Even today, as an adult, the threat of malaria looms large. I worry constantly about contracting the disease and passing it on to my own children. The thought of them suffering as I did is a constant source of anxiety."
– Bwango Benjamin Mukaapa
Participants highlighted a range of other issues. Paying for medicines is another source of economic strife, but antimalarial drugs may be difficult to source. Some suggested that antimalarial combination therapies are becoming less effective. Drug resistance is a very real concern, though there are other reasons that the treatment could fail to elicit a response, such as use of poor quality or counterfeit drugs.
"When medicines run low, it's a disaster. People resort to using unapproved drugs or traditional remedies, which can be ineffective or even harmful."
– Lucy Pam Dangyang, Public health professional, Bokkos LGA, Plateau State, Nigeria
"In Uganda, antimalarials (ACT) are very scarce from public health facilities and too expensive from private facilities. People are used to self-medicating whenever they feel uncomfortable, so they just buy painkillers to treat themselves, which is a risk to their lives as in the case of malaria it is given chance to develop further as malaria progresses from mild to severe."
– Kiwalabye Dan Rogers, Public health specialist, Greater Mukono Region, Uganda
Many contributions also highlighted how climate change is driving an upsurge in malaria. Higher temperatures are changing the distribution of the mosquitoes that transmit the disease, their biting habits and the multiplication of malarial parasites. Extreme weather events and flooding are creating more environments in which mosquitoes can multiply.
Have you read?
There are already ways to reduce the burden of malaria. Insecticide-treated bed-nets, for example, can prevent mosquito bites at night. However, although demonstrated to reduce infection, bed-nets are often not popular and take-up in many areas is low.
"The mosquito nets given are not in good size so that it can cover the bed. The mosquito nets are very small enough to protect the people from malaria."
– Anonymous, Community health worker, NGO, Tanzania
"In Uganda, free nets are supplied to communities. But unfortunately treated nets are diverted to different uses, such as making local brew, fishing activities, harvesting coffee, trapping grasshoppers and others use them as mattresses."
– Kiwalabye Dan Rogers
"Some people complain of feeling hot, others complain of a burning sensation on their face and skin when they sleep under the mosquito net; that's why they don't feel like using it."
– Lawrencia Caesar, Nurse, Ministry of Health, Asikuma Odoben Brakwa District, Ghana
Spraying with insecticides is also not an ideal solution and drives the emergence and spread of insecticide resistance in mosquitoes. Use of antimalarials to prevent infection is highly effective but is generally reserved for special populations such as pregnant women, who are at particular risk from malaria, or children in areas where malaria is highly seasonal (seasonal malaria chemoprevention, SMC).
Respondents also highlighted how they and their local communities have been taking steps to respond to the resurgence of malaria.
"Our effort is to kick malaria out of Uganda and save lives by ensuring that our people take the basic prevention measures, such as draining stagnant water and clearing bushes as laid out by Ministry of Health and WHO. So, in that respect, we mobilised the community and engaged them to join the fight against malaria by sensitising them to stop misusing the nets for other activities, allow residential spray strategy and to plant mosquito repellents at their homes."
– Kiwalabye Dan Rogers
"Tragically, I've witnessed many of my neighbours, including young children, succumb to the disease due to lack of timely access to proper treatment. In response to this growing crisis, my community has banded together to take action. We've organised regular clean-up efforts to drain stagnant water sources and eliminate mosquito breeding sites around our homes and public spaces. Many of us have also invested in securing reliable supplies of insecticide-treated bed-nets, ensuring our families have a critical line of defence against mosquito bites."
– Bwango Benjamin Mukaapa
The fact that two effective malaria vaccines, RTS,S/AS01 and R21/Matrix-M, are now available is a major step forward for malaria prevention. More than 20 countries have applied to Gavi for support to introduce malaria vaccination and the first countries began to roll out the vaccine in early 2024 (following in the footsteps of Ghana, Kenya, and Malawi, three countries that began administering the RTS,S vaccine in 2019 as part of a WHO-led pilot programme).
The vaccines will not be enough on their own. They will need to be used alongside other antimalarial measures, such as insecticide-treated bednets and chemoprevention, to achieve optimal protection. There will also be operational challenges to overcome and the need to ensure community acceptance – although the experience to date suggests that the burden of malaria is a strong motivator stimulating high community demand.
"As our country begins to roll out the new malaria vaccine, I am actively involved in educating the community about its benefits. We anticipate challenges such as vaccine hesitancy, logistical issues, and ensuring equitable access. To overcome these, we are focusing on building strong partnerships between health care providers, community leaders, and local organisations. Effective communication and trust-building will be key to the vaccine's acceptance and success."
– Joseph Mbari Ngugi
2024 could therefore be a landmark year for malaria prevention. That figure of 500,000 deaths may soon begin to drop – and fewer households may have to live with constant anxiety that malaria could strike at any moment.
Request your invitation for Teach to Reach 10 at https://www.learning.foundation/teachtoreach
Note: Contributor quotes in this article are their own and do not necessarily represent their employers.