Reaching zero-dose children in Malawi’s cities
In Malawi urban areas have more unimmunised zero-dose children than rural regions. The government is working hard to close the immunisation gap.
- 20 September 2021
- 4 min read
- by Josephine Chinele

It’s a warm and sunny Tuesday morning and all is set for under-five clinic sessions at Mbayani Health Centre. The clinic is located within Blantyre’s high density, slum township of Mbayani. Mothers from all walks of life come here with their toddlers tightly strapped to their backs with a cloth, shading them from the sun with an umbrella carried in one hand, and a nappy bag hanging from the other hand.
“I know the importance of immunisation; that’s why I had to bring the child today."
Most of these children are set to receive at least one routine vaccine while a couple are there just to be weighed and get vitamin A and deworming tablets. Several of the mothers attending had missed their original immunisation date. When asked for the reasons, there is general silence.
Cecelia, a Mbayani resident, however, admits, “I chose to miss my baby’s vaccine but it’s because of the situation I was in. We literally had no food in the house and I had secured well-paying piece work for a few days which included the scheduled immunisation day for my child. I know the importance of immunisation; that’s why I had to bring the child today.”
“Such has been the trend at this clinic and many other urban clinics,” says James Nyirenda, the supervisor for the Mbayani Health Centre. “Most women are very busy with their businesses or careers, so much that bringing a child on the scheduled date is difficult for them. Some give up just looking at the queue.”

Credit UNICEF Malawi
He also explains that sometimes women don’t come back to the same clinic and, for those with the means, go to a private health facility which costs, on average, 2000 Kenyan shillings ($0.25).
“This is okay and their choice but, because most private facilities do not track and share data, which would be used for government reporting, it creates gaps,” Nyirenda says.
Have you read?
A 2019/20 UNICEF brief, Upscaling investments in child immunisation: A Step towards targets by 2021, indicates that although Malawi is doing well in child immunisation, there are disparities in immunisation outcomes between urban and rural populations. The Expanded Programme on Immunisation (EPI) recently indicated that across all antigens, Malawi is missing approximately 10% of children, with a significant portion of these zero-dose children in urban areas.
The trend at Mbayani Health Centre partly explains this but, according to the District Environmental Health Officer (DEHO), Penjani Chunda, there are no designated outreach clinics that are close to the people as is the case with the rural areas, where health workers bring immunisation services to hard-to-reach places through an established clinic schedule.
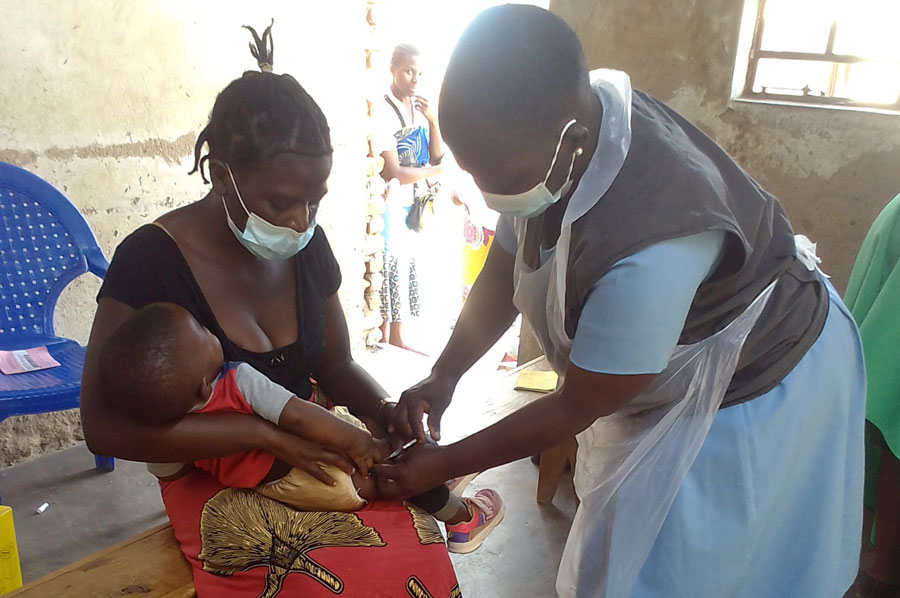
Credit UNICEF Malawi
There are various initiatives being developed to reach these missed urban children. For example, the Blantyre District Health Office is working towards empowering private clinics with adequate staff to provide information on immunisation.
“Among other interventions, we are establishing key focal immunisation points in the urban areas, besides the designated health facilities, to bring the service closer to the people through scheduled programmes. We are also reopening weekend immunisation services and have scheduled to do sensitisation of the block leaders and other urban political structures,” Chunda says.
Professor Adamson Muula, Head of Public Health at Kamuzu University of Health Sciences (KUHES), says that while there are disparities in terms of urban versus rural child immunisation coverage rates, it is important to note that Malawi has made excellent progress in achieving high rates of vaccine coverage.
“Many countries in the world can only dream of achieving such high rates. The rural-urban difference can easily be attributed to the community health infrastructure that is almost always well developed in rural districts,” he notes.
Professor Muula highlights that the backbone of under-five child immunisation is the environmental health staff being trained by the government’s health system.
“Malawi has invested heavily in this group, who live in the community, organise mobile vaccination clinics and can undertake door to door vaccinations, They have the numbers, the experience and the distribution. Each rural community has at least one such cadre. Contrast that with urban areas, where the system is broken with fewer mobile clinics and door to door vaccinations.”
Malawi’s EPI, in partnership with UNICEF and other partners, is implementing equity-focused programming in low-performing districts to develop micro plans for addressing identified bottlenecks. This includes mapping the location of un-immunised or underserved children, understanding reasons for non-vaccination and their root causes.
“Currently UNICEF is working with the government to develop urban immunisation and zero-dose strategies aimed at providing a clear roadmap for reaching under-immunised children,” says Steve Macheso, UNICEF Malawi Health Specialist. “UNICEF broadly supports training of health workers, procurement of vaccines and supplies, cold chain management and demand generation.”









