Amid pandemic chaos, measles – the “canary in the coalmine” of vaccine-preventable diseases – is spiking
What does a 79% bump in global measles cases really mean?
- 4 May 2022
- 5 min read
- by Maya Prabhu
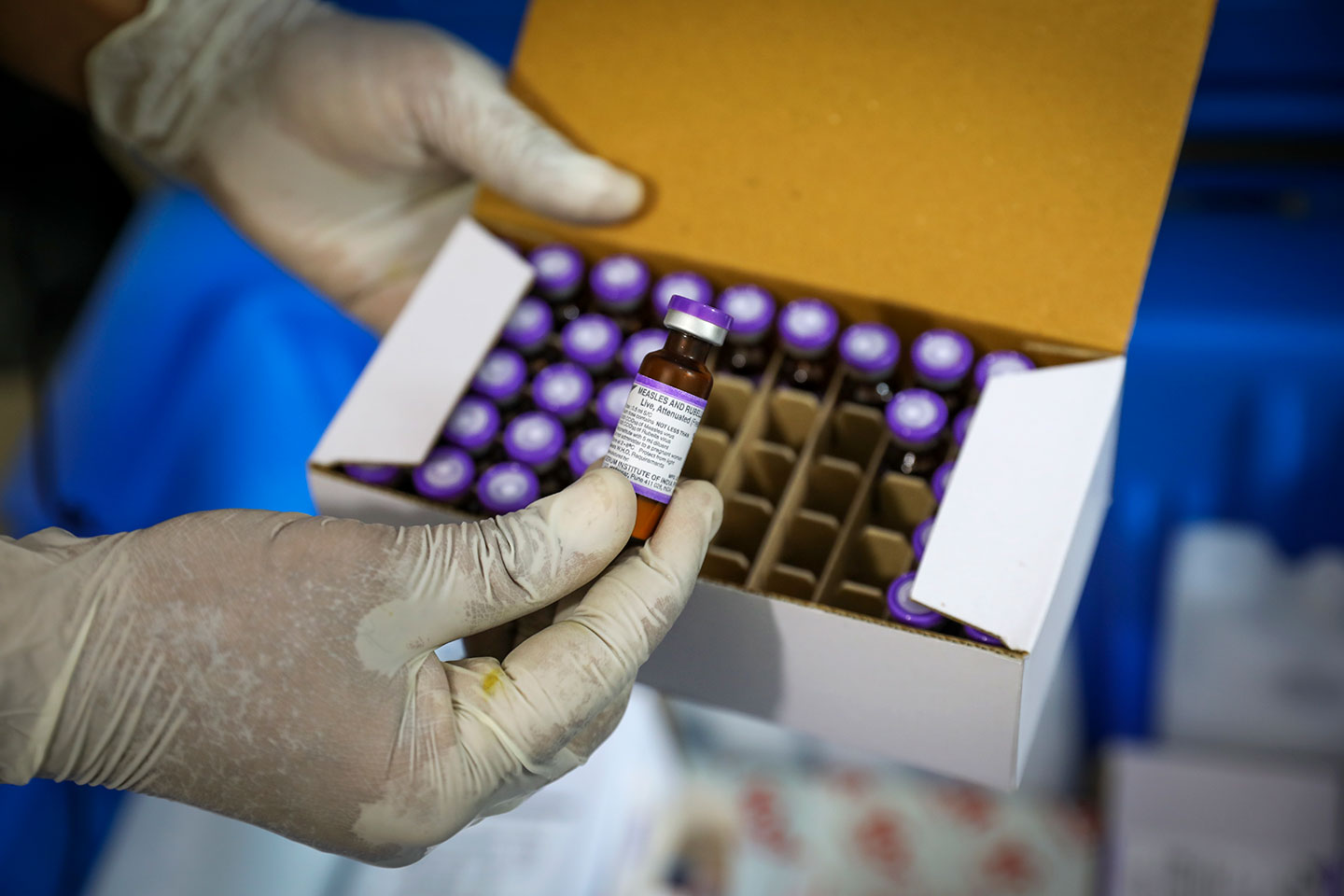
Cases of measles spiked by nearly 80% globally in the early part of this year – a result, according to WHO and UNICEF, of pandemic-related upheavals to health systems, including the diversion of resources and attention away from routine childhood immunisation.
As the most contagious and fast-moving of the vaccine-preventable diseases, measles is often described as the “canary in the coalmine” for other disease outbreaks that might spring up where there are gaps in vaccination coverage.
A total of 17,338 measles infections were reported in January and February of 2022, a startling jump from the 9,665 cases reported in the equivalent period of 2021. On its own, that’s alarming: in the absence of vaccination, measles is a potentially deadly childhood infection, which can also cause blindness, encephalitis and pneumonia.
But that surge in cases also represents a worrying portent. As the most contagious and fast-moving of the vaccine-preventable diseases, measles is often described as the “canary in the coalmine” for other disease outbreaks that might spring up where there are gaps in vaccination coverage.
“It’s a marker for weak health systems because it’s so infectious and easy to recognise,” explains Dr Peter Strebel, a disease-control expert who works on Gavi’s Measles and Rubella portfolio. “From a disease-control point of view, we say, you know, measles will find communities that have low vaccination coverage, or susceptible persons.” In other words, the mid-pandemic uptick in measles cases is a spotlight on health systems compromised by COVID-19, vulnerable, now, to other disease outbreaks too.
Before the measles vaccine was introduced in the 1960s, Strebel says, 95% children could expect to be infected with the virus before mid-adolescence. For most, that meant fevers and rashes and then recovery. But one in a thousand among even healthy, well-nourished children in the industrialised West were expected to die with the disease – most commonly as a consequence of secondary infections like pneumococcal bacterial infection and pneumonia. In poor socio-economic settings, outcomes are far graver, with measles outbreaks killing up to 15% of its victims in developing countries.
Treatment options remain few. There is no specific antiviral medication, so even today, measles patients are offered only supportive care to prevent dehydration, mitigate nutritional deficits, and spot and tackle dangerous secondary bacterial infections like pneumonia. That means that the likelihood that a case of measles will turn fatal is pretty much unchanged – one in a thousand if the patient belongs to a wealthier society, often far higher if the patient lives in a lower-income setting.
Have you read?
“Measles is still a very different disease among well-nourished versus malnourished children, particularly if they are Vitamin A deficient,” says Strebel. On top of nutritional status, children in developing countries often live in crowded settings, which can impact the viral-load dose, with potential ramifications for disease severity. Strebel sketches the hypothetical: “If you’re in a big family, you know, seven or eight kids, and the kids are playing on top of each other, and they’re malnourished, you get a whopping great infectious dose and basically, the virus overwhelms the immune system.” This scenario is often compounded by lack of access to health care.
But widespread vaccination has meant that during the last decades, relatively few children have had to run that gauntlet: between 2000 and 2017, measles vaccination is estimated to have averted 21.1 million deaths.
Somalia, Yemen, Afghanistan, Nigeria and Ethiopia recorded the highest infection figure, a roll-call which underlines the compound ways in which measles both magnifies and highlights global health inequities.
Then came COVID-19. In 2020 alone, WHO and UNICEF say, a massive 23 million children missed out on basic immunisations, creating the largest vaccination gap the world has seen since 2009. In April 2022, a total of 57 vaccine-preventable disease campaigns in 43 countries that had been postponed as a consequence of COVID-19 remained in suspension. Nineteen of them were measles campaigns, leaving 73 million children at risk.
The impact of that thinned coverage will reveal itself on a delay. Early 2021’s official measles tally was strikingly low, probably in part due to under-reporting – surveillance systems in many places were diverted to COVID-19 management. But the mysterious new coronavirus also ushered in a paradoxical kind of collateral protection. Measles is a respiratory virus transmitted, like COVID-19, through the air, and so measures aimed at curtailing COVID-19’s spread – the lockdowns, social distancing and mask-wearing – were likely also insulating the vulnerable from contracting measles.
Now that those preventive norms are relaxing in large portions of the world, the exposure risk for measles is again increasing – presenting the gravest threat where the protective web of vaccine coverage has grown most threadbare.
In the year to April 2022, a period of time probably still characterised by disrupted reporting – and consequently artificially low figures – 21 “large and disruptive” measles outbreaks were reported. Somalia, Yemen, Afghanistan, Nigeria and Ethiopia recorded the highest infection figures, a roll-call of countries that underlines the compound ways in which measles both magnifies and highlights global health inequities.
And the threat of measles isn’t over when the outbreak blows past, or the infection is cleared from a child’s body. Measles is understood to precipitate lasting “immune amnesia”, meaning that the immune system “forgets” its defences to previously-encountered pathogens. “It explains why you often see increased childhood mortality following measles outbreaks,” Strebel says. The children who recover from measles infection this year will remain at greater risk from other infections for possibly two to three years to come.









