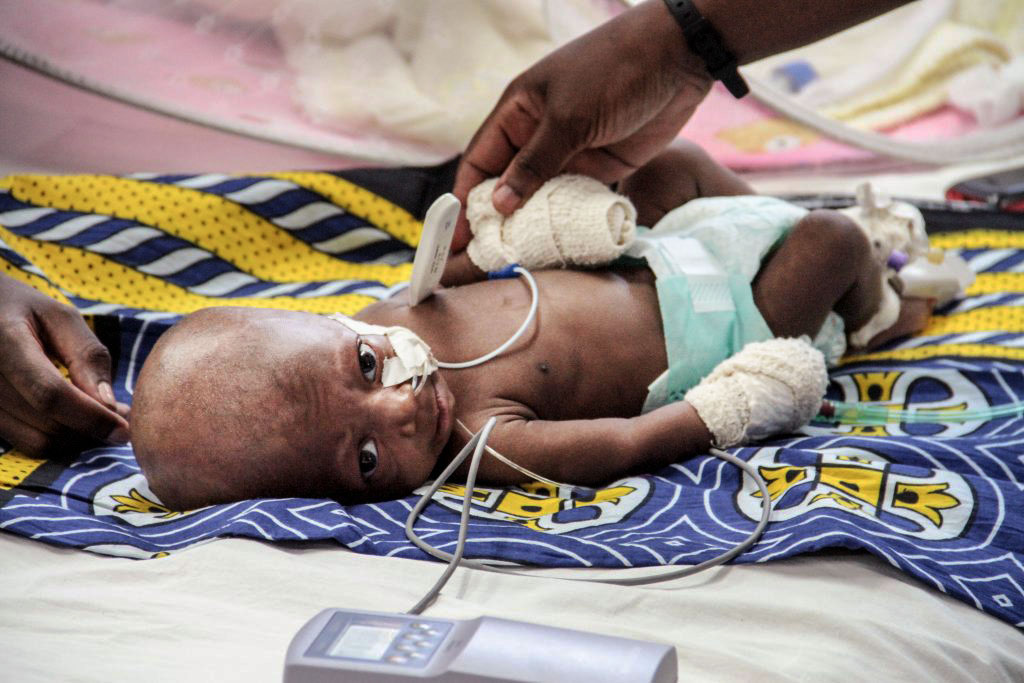
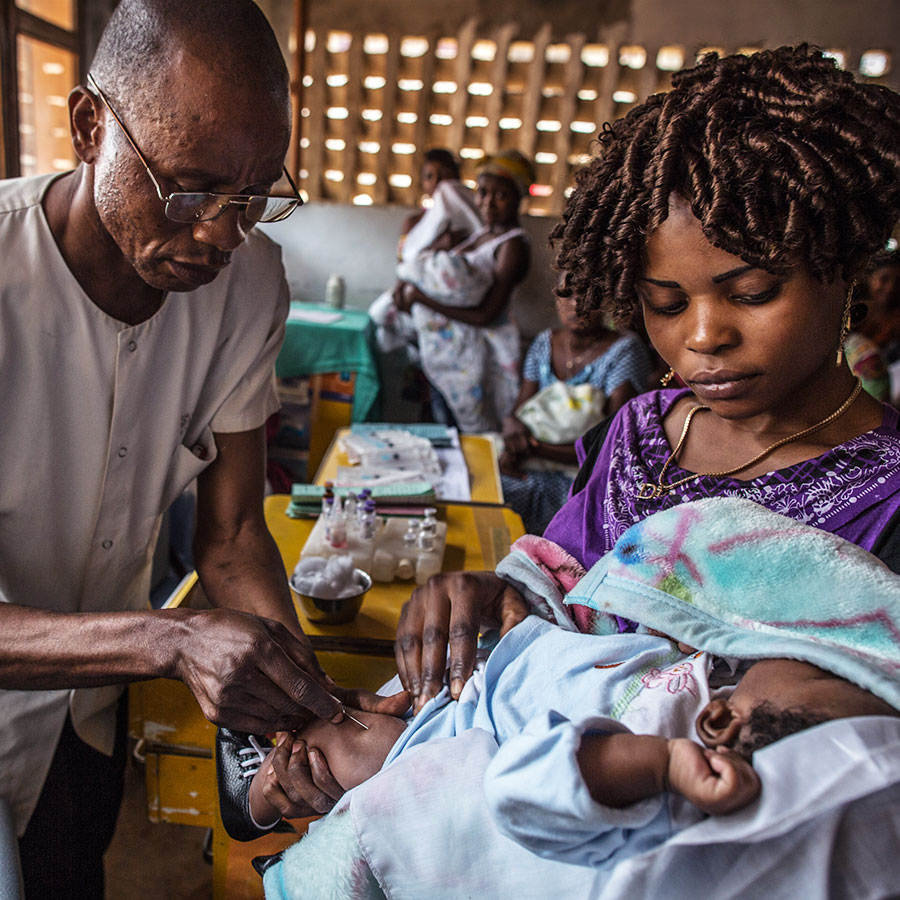
Risks for inadequate care during an illness
We have highly effective and affordable tools to protect, prevent, and even treat pneumonia, but there are major inequities in deployment and delivery of these tools. Many families experience serious impediments to accessing care, and health systems in many districts are not yet able to provide the quality of care children need for recovery from their illness.
The ability to access life-saving treatments is disproportionately influenced by factors like poverty, living in rural areas and low education levels among parents. In five countries with some of the highest numbers of pneumonia deaths in children, treatment for pneumonia by an appropriate healthcare provider was nearly 15 to 30 percentage points lower among children in rural areas than children in urban areas. Similarly, treatment was between 10 and 38 percentage points lower in children of the poorest 20% of the population than in the wealthiest 20%.We also see that costs of care and treatment can be a major barrier to accessing care. For example, the cost of pneumonia treatment for families in the Gambia can be up to 10 times their daily budget, including direct medical costs and indirect costs like meals and transportation, further threatening the entire family.
On average, severe pneumonia kills one in 50 children who receive treatment at a hospital, yet it kills one in seven children who don’t access care at a hospital. It’s also estimated that nearly 40% of children with severe pneumonia don’t reach a hospital for treatment. Poor access to care and inadequate care-seeking behavior are seen in many countries, driven in part by rural location, cost and cultural factors which stop many families from access to life-saving hospital care.
Inadequate health systems have a direct impact on childhood mortality. District level facilities very often do not have oxygen or other treatment supplies for care of children with pneumonia. Referral hospitals are not intended to cope withthe burden of community-acquired pneumonia that they could be expected to take on if community facilities are not in a position to care for these children. A health facility visit for basic assessment, pulse oximetry monitoring to detect oxygen levels and antibiotics to treat a case of pneumonia is quickly impeded by one obstacle after another, making timely treatment an unreliable reality for many. Families and community health workers, where available, are therefore forced to handle severe – and difficult-to-treat – cases. In some cases, this means a preventable and treatable infection can escalate into a critical situation.
Even for those who can reach a hospital setting, the outcome is not always positive. One in four children who were taken to a large pediatric hospital in Bangladesh were refused admission to the hospital because all beds were full, resulting in a substantial proportion of those with symptoms of pneumonia being turned away. It is staggering to know that this situation is repeated in many low- and middle-income country facilities around the globe with health systems that are not adequate to provide the necessary care.
Although it is estimated that about 60% of children with severe pneumonia are treated in hospitals, 80% of pneumonia deaths happen outside hospitals. This shines a bright light on the imperative for pneumonia prevention as the foremost strategy – most children who die of pneumonia do not have medical care for their illness. We cannot ‘doctor’ our way out of this pneumonia burden problem. Vaccination is a proven tool to prevent many cases of pneumonia – and may further shield children from the many risks that are stacked against them.