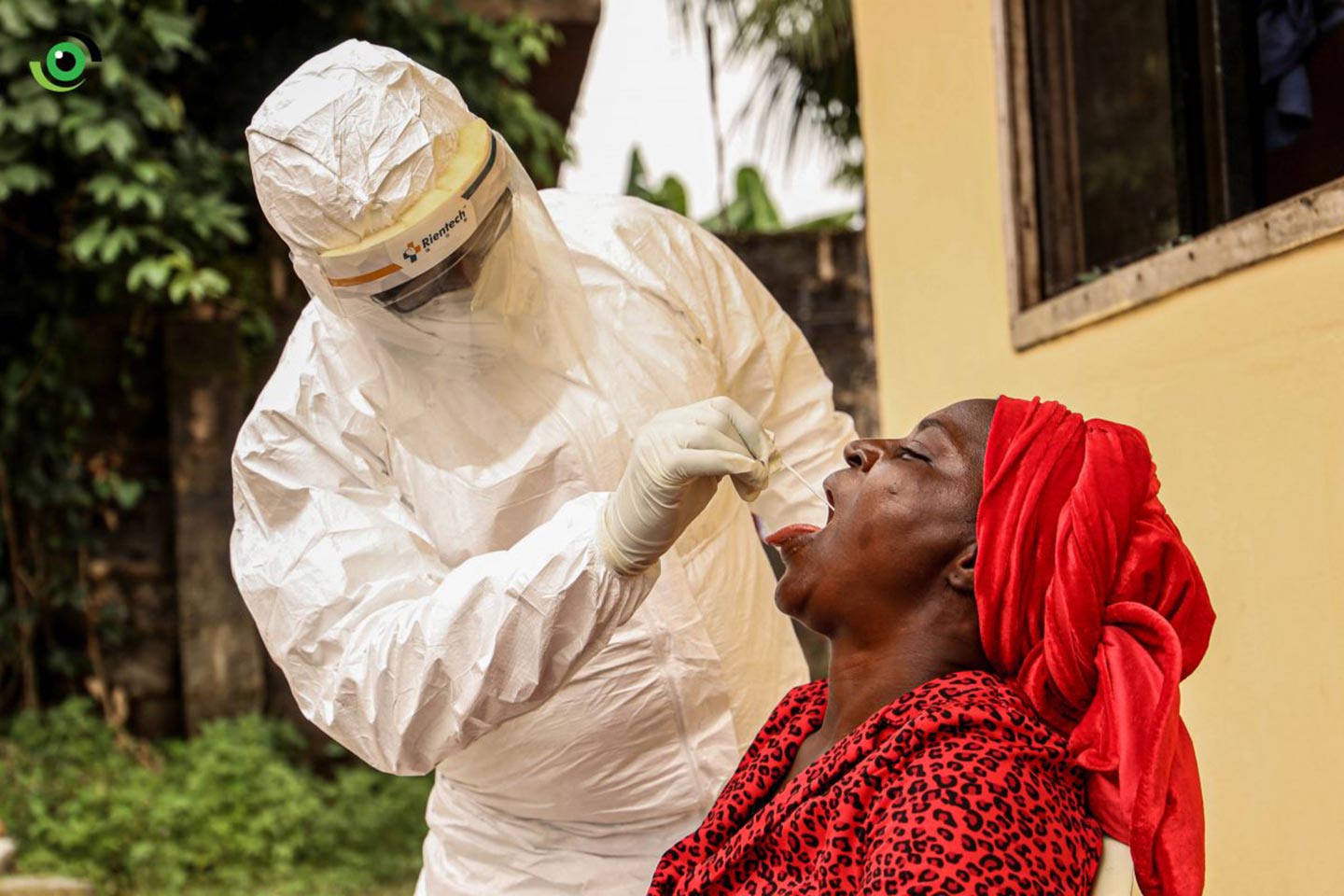
Friendship Bench: Zimbabwe’s Community-based Talk-Therapy Supporting Communities during the COVID-19 Pandemic
In Zimbabwe, Friendship Bench, a community-based approach is providing solutions to people struggling with their mental health during this pandemic.
- 27 January 2021
- 7 min read
- by Nigeria Health Watch

The COVID-19 pandemic has brought a lot of challenges and disruptions to our lives. The livelihood of people has been affected and the pandemic has taken a toll on people’s mental and psychological health. In Zimbabwe, Friendship Bench, a community-based approach is providing solutions to people struggling with their mental health during this pandemic.
Friendship Bench is a community project which trains grandmothers and other volunteers in cognitive behaviour therapy using evidence-based talk therapy in their communities. The grandmothers are custodians of local wisdom and culture across Zimbabwe. They sit on a bench while offering counselling and mental illness services to support community members through issues like depression and anxiety.
The project, an intervention developed to bridge the mental health treatment gap, has been running since 2005 and has helped more than 40,000 people receive care in 2018 alone.

“The Friendship Bench is an evidence-based mental health intervention and it has been running in communities and has continued even with the onset of the pandemic,” says Kelly Muzariri, a team member of Friendship Bench. “Certainly, the pandemic has worsened mental health issues around the world because of loss of jobs and livelihoods. It affected everyone and not just those in the employment sector. Young children have been put out of their circle and have been unable to go to school, or have the routine they were once familiar with.”
The model has now been replicated in Malawi, Botswana, Zanzibar, and as far as New York City, USA. More countries especially in sub-Saharan Africa are ready to adopt it in solving mental health issues among their population.
Mental disorder is an escalating global challenge, especially in low- and middle-income countries where numbers are rising fastest, but services lag far behind due to low numbers of mental health professionals. This has, however, worsened amid the coronavirus pandemic.

Photo source: Friendship Bench
According to the World Health Organization (WHO), more than three quarters of the people with mental challenges in low and middle income countries receive no treatment. The WHO’s Mental Health Action Plan 2013–2020, endorsed by the World Health Assembly in 2013, recognizes the essential role of mental health in achieving health for all people.
Mental illness is accounts for 39 percent of healthy life lost from non-communicable diseases and it is estimated that it will cost the global economy $16 trillion by 2030 in lost productivity and health costs, according to a 2011 report by the World Economic Forum and the Harvard School of Public Health.
Unfortunately, in some African countries, less than 1 percent of national health spending is allocated to mental health and there is only one psychiatrist for every 1 million people, a 2017 study showed.
Have you read?
But solutions for this are emerging, including the use of lay health workers — specifically trained specialists who use WhatsApp to provide therapeutic treatment to those suffering from mental health disorders in Zimbabwe as a result of loss of job or extended lockdown.

During the pandemic, there have been increases in reported cases of mental illness due to COVID-19 restrictions and instead of the normal face-to-face counseling for mental health patients, Friendship Bench has gone online and introduced the use of trained specialists called “open-liners” to provide free counseling sessions for patients via WhatsApp.
A dedicated WhatsApp line is provided where clients who need the free counseling service, can book sessions and call at certain times of the day. The service runs from Monday to Friday from 8 a.m., to 5 p.m. with a session lasting between 30 minutes to one hour.
“Before the pandemic, we had an open house where people can come and have free counselling sessions. But because of the pandemic, we had to switch from our face-to-face problem-solving therapy to an online based therapy called an “open-line talk therapy,” Muzariri said.
More than 600 mental health patients have been reached and have received counseling since the pandemic started, and the numbers are increasing each day.
![Dixon Chibanda [Middle] says the goal of Friendship Bench is to go beyond Zimbabwe to every country around the world. Photo source: Friendship Bench](/sites/default/files/vaccineswork/2021/Thumb/1_tF7mB1pSZqsdEfc48pdWXw_h2.jpg)
Photo source: Friendship Bench
“All that is needed for a counseling session to take place is a digital device like a mobile phone which can be used to contact Friendship Bench specialists who offer this service at no cost,” Muzariri says, adding that this new channel has helped to keep the patients safe as there is no physical contact.
Muzariri says that the COVID-19 pandemic has shone a spotlight on a lot of mental health issues. “People are now beginning to realize the problem at hand and are speaking out. So, I believe that as much as the problem has increased, it is also good in the sense that it has brought a spotlight to the need for mental health services and the demand for people to know what depression really is and that they could be victims of depression or anxiety” she said.
Muzariri added that cases of domestic violence increased during the lockdown because people are now confined in one space with their abusers. “So, there are a whole lot of issues that have come up and contributed to mental health challenges,” she said.
In the last ten years, Zimbabwe has seen a growing interest in the use of lay health workers to reduce the treatment gap for common mental disorders, according to Dr. Dixon Chibanda, the founder of Friendship Bench and the director of the African Mental Health Research Initiative.
Supported by the City Health Department, the Friendship Bench has been accepted by communities in Zimbabwe with over 7,000 patients utilizing the services in three pilot clinics between 2006 and 2011, Chibanda says, adding that more than 70,000 people have received the mental health therapy from grandmothers over a ten-year period.

The Friendship Bench project is presently the most established initiative, providing problem-solving therapy with components of behavior activation.
Chibanda, is also an Associate Professor of Global Mental Health at London School of Hygiene & Tropical Medicine and says the real solution to mental health issues has to be delivered from the bottom-up by “integrating our culture in the way we address challenges that society is facing.”
He continues: “I think one of the successes of Friendship Bench is really because these grandmothers are rooted in local culture. They use a language which the community can resonate with. So, I think the solution is to focus more on communities; to identify community leaders, people who can drive change at community level.
As with any initiative, there are challenges, one of which is with the awareness level of mental health challenges at community level. Additionally, internet connectivity is an issue as service disruptions sometimes prevents the counselors from reaching patients needing counseling, especially in rural communities.

Going forward, Muzariri says that the primary goal is to have a Friendship Bench within walking distance in every community in Zimbabwe.
Chibanda is rather ambitious. He says the goal is making evidence-based treatment like Friendship Bench accessible in communities around the world.
“That is really what I want to try and achieve, and it may sound very ambitious, but I would like to achieve this. It might not happen in my lifetime, but I certainly think it is achievable. We can train ordinary people in communities to make a difference and reach out to other people in the community to help those who need support for their mental health.”
To address and solve a problem, you need data and in many African countries, there is inadequate research and data on mental health to ensure that targeted interventions are put in place. The continent also suffers from a low level of mental health workers compared to global averages.
In Nigeria, mental health issues are largely neglected with outdated policies and legislation. The Mental Health policy currently in place in the country was formulated in 1991 with the first mental health legislation enacted in 1916, called the Lunacy Ordinance, with subsequent amendments in 1958 renaming it the Lunacy Act. A first reading was held in the Nigerian Senate in January 2020 for the Mental Health and Substance Abuse Bill and the bill is now still in consultation with lawmakers. It is evident that urgent action is needed to put in place legislation to protect people suffering from mental illness. This would ensure that they have the necessary support structures in place, access to care when they need it and there is guaranteed budgetary allocation to support the training of relevant mental health workers and adequate service provision.
While we wait for improved access to mental health services, Friendship Bench in Zimbabwe has been a laudable and agile service, bridging the gap in access to mental health services, adapting to meet the needs of communities looking for support, as they navigate the complexities that the COVID-19 pandemic has thrown up. At this time, more than ever, people are looking for an empathic ear and voice that “listens” and “speaks” to them. The ability of digital technology to transcend borders, will now enable Friendship Bench to expand its reach.