How will COVID vaccines work on compromised immune systems? Here’s what we know
Being immunocompromised appears to affect the vaccine response, but this seems to vary depending on the causes of the person's low immunity.
- 11 August 2021
- 5 min read
- by The Conversation

In many cases, vulnerability to COVID-19 exists because a person’s immune system is unable to mount a good response against the coronavirus. Such people are said to be immunocompromised.
It’s possible that these people won’t respond as well to COVID-19 vaccines either. At the moment, though, we’re still finding out to what extent this is the case. Different studies are producing different results, which underlines the difficulty of getting to the bottom of this issue. Immunocompromised people aren’t a uniform group, and so may respond to vaccines differently.
For instance, one US study has found that people taking drugs that suppress their immune systems (after having had an organ transplant, to stop the organ being rejected) appear to be hampered in their ability to generate antibodies after being vaccinated. The study found that over half of the immunocompromised people it looked at had generated no antibodies even after receiving two vaccine doses.
The results of other studies, though, aren’t quite so disheartening. Another piece of research found that immunosuppressed kidney transplant patients did respond somewhat to being given a dose of a COVID-19 vaccine, but that they had weaker antibody responses than those with fully functioning immune systems.
And a recent UK preprint (an early piece of research still awaiting review by other scientists) aimed to provide more information on how well the Pfizer/BioNTech and Oxford/AstraZeneca COVID-19 vaccines work in different at-risk groups. These included patients with diabetes, chronic heart disease, chronic kidney disease, chronic liver disease, neurological conditions as well as those who are immunocompromised.
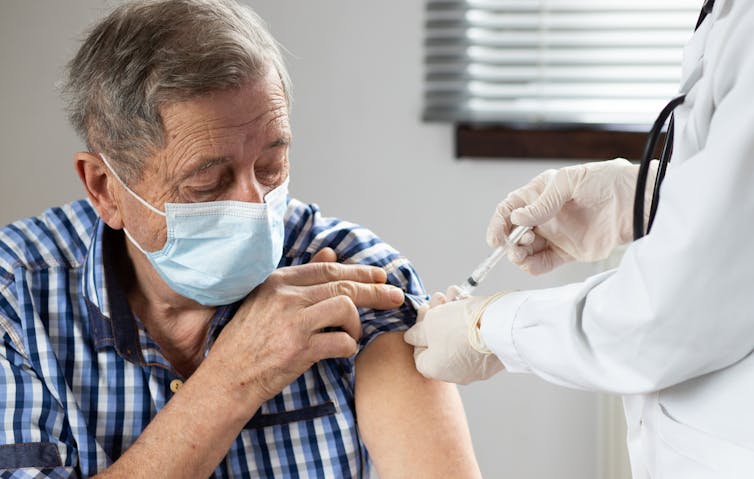
Most groups generated strong antibody responses and were protected against symptomatic COVID-19 after being vaccinated. But in the immunocompromised, antibody levels were lower after two doses, and after their first dose they were less well protected against symptomatic COVID-19 than the other groups. However, after having had both doses, the immunocompromised group appeared to be well protected against the disease, even though their antibody levels were lower.
Have you read?
It’s encouraging that even in the face of a compromised immune system, for some people, two doses of vaccine can still bestow considerable protection against COVID-19. Yet the variation across these studies shows that immunity can differ greatly between immunocompromised individuals. It’s likely that the different causes of low immunity determine how well COVID-19 vaccines work – though we’re only starting to confirm this.
So what hampers immunity?
Compromised immunity exists in two broad categories. There are those with medical conditions that directly affect the immune response, causing it to underperform. And there are also those whose medical conditions are managed using immunosuppressive drugs.
The former group of conditions are called immunodeficiencies. These can exist from birth as a result of genetic alterations, though they are very rare. They can also be acquired later in life through many different causes. These include malnutrition, obesity, diabetes and HIV infection.
The ways in which some of these factors negatively affect the immune system are well known. For example, HIV infects white blood cells know as helper T cells. As a result, patients have fewer of these cells available to fight off other infections.
But in many cases we don’t fully understand why a condition leads to immunodeficiency. For example, diabetes is a risk factor not just for COVID-19 but also other viral and bacterial infections, including hepatitis B and tuberculosis. However, studies are beginning to reveal how uncontrolled blood sugar in diabetic patients makes their immune systems less effective. Signalling between immune cells is impaired, as is their ability to kill disease-causing microorganisms.
Then, there are immunosuppressive drugs, which patients receive for many different reasons. These range from having organ transplants to asthma to blood cancers or autoimmune conditions. There are many types of these drugs, with different ones used for different conditions. The extent to which a drug may affect the COVID-19 vaccine response will vary depending on how the drug works.
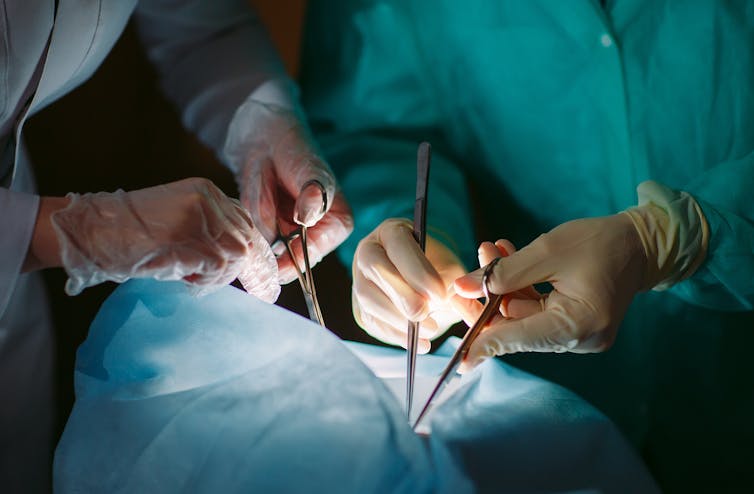
Antimetabolites, for instance, are drugs that interfere with some of the most basic aspects of cell function. To take an example, one such drug – mycophenolate – affects the ability of immune cells to create new DNA and divide properly. Antimetabolites have wide-ranging effects – being used in chemotherapy and to stop the body rejecting organ transplants – and are associated with poorer COVID-19 vaccine responses.
Another class of immunosuppressive drug are what are known as “targeted biologics”. These can block specific parts of the immune system while leaving others unaffected. For example, drugs that block an immune-signalling molecule called TNF work in a very focused way, and so have been shown to have less of an effect on the COVID-19 vaccine response compared to antimetabolites.
However, other targeted biologics – for example rituximab, a type of artificially created (or “monoclonal”) antibody – affect COVID-19 vaccine responses more significantly. Rituximab targets a specific molecule on the surface of immune cells that produce antibodies, reducing their productive ability. For this reason, patients should avoid receiving rituximab for a period before and after COVID-19 vaccination.
At the moment, much of what we know about how well COVID-19 vaccines work in immunocompromised groups comes from smaller studies. It’s vital that data is gathered from larger groups to help us fully understand the barriers to getting people to create effective vaccine responses. In the meantime, people with conditions or taking medications that are known to lower the effectiveness of the immune system should be aware that their level of vaccine protection could be below average.![]()
Authors
Steven Smith, Senior Lecturer in Biomedical Sciences, Brunel University London

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Steven Smith does not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
Partners

Brunel University London provides funding as a member of The Conversation UK.








