Seen by a physician, but still not vaccinated: uncovering missed opportunities in Pakistan
An unnecessary disconnect between curative and preventive healthcare is leaving too many of Pakistan’s children at risk.
- 15 May 2026
- 4 min read
- by Akhter Hameed Khan Foundation

Saima still remembers the night Hasan would not stop crying.
It was past midnight in Dhoke Hassu, Rawalpindi, in the family’s modest two-bedroom home in a densely populated urban slum. The child’s tiny body burned with fever; his cries were weakening and punctuated by a slight hacking cough. Saima had tried every home remedy her mother-in-law recommended – cooling his forehead, placing black cloves near his nose, holding him close, whispering prayers – but nothing worked.
At dawn, she and her husband rushed him to the nearest local GP clinic. The doctor examined the baby, asking questions casually. “It’s a common illness,” he said, scribbling a short prescription. “He’ll be fine.” The parents nodded, unsure but reassured. They had been through similar cycles several times over the past three years. Each visit ended the same way: a diagnosis, a prescription and reassurance.
To Saima, this meant she was doing things right.
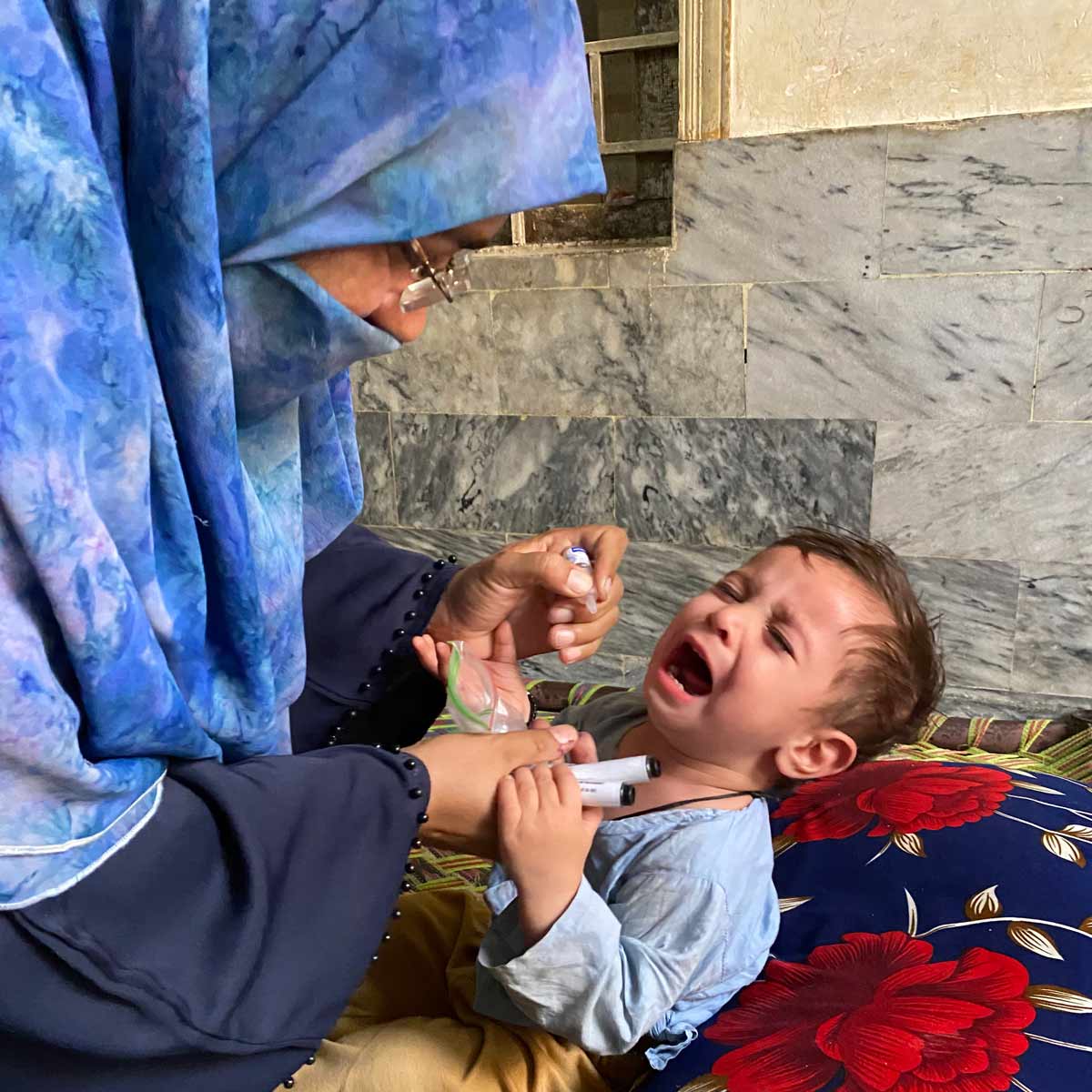
Three months later, at Hasan’s fourth birthday, he fell sick again, this time with symptoms she had never seen before. The clinic visit led to a hospital admission. There, she finally learned that a missed booster shot, skipped when the family visited their village, could have prevented his illness.
Looked over, and overlooked
Five healthcare interactions, and at none of them had a doctor or nurse checked his vaccination status.
Hasan’s story is not unique. It plays out across urban settlements and rural communities throughout Pakistan. It is a story of missed opportunities, gaps in provider practices and weak systems for tracking children who fall behind on immunisation.
Pakistan continues to have one of the highest numbers of under-vaccinated children globally, and vaccine-preventable diseases remain a major contributor to child mortality. However, the issue is not simply one of access.
Analysis of large-scale household data shows that nearly one in four children misses at least one essential vaccine dose, including the basic pentavalent jab, which includes vaccines against diphtheria, pertussis, tetanus, Hib and hepatitis B, and the measles vaccine. More strikingly, over 90% of these children had already interacted with a healthcare provider at least once.
This points to a critical gap: children are reaching the health system, but the system is not consistently delivering vaccination when it has the chance.

These instances are known as missed opportunities for vaccination (MOVs) – situations in which a child eligible for vaccination encounters health services, but leaves without receiving it.
Have you read?
Locating the cracks
In Pakistan, part of the explanation lies in how healthcare is organised.
Vaccination services are largely delivered through the public sector, yet a significant share of care-seeking, particularly in urban areas, takes place in the private sector. Small private clinics are often the first point of contact for families, offering quick and accessible treatment for common illnesses. However, these clinics are not integrated into public sector tracking systems or immunisation networks.
The burden of missed vaccinations is not evenly distributed. Children from poorer households, those living in remote areas, and those with less educated mothers are significantly more likely to miss essential doses. Missed vaccination rates are particularly high in districts of Balochistan, such as Khuzdar, which are sparsely populated, and much of the population is very remote. At the same time, data reveals a less intuitive pattern: missed opportunities are often more frequent in urban settings.

This reflects differences in care-seeking behaviour. Urban families are more likely to rely on private providers, where consultations are efficient but narrowly focused on treatment. Preventive checks, such as reviewing vaccination status, are rarely part of routine care.
Reform, not revolution
For mothers like Saima, who may lack access to information or formal education, navigating immunisation schedules without guidance becomes extremely difficult. Research also suggests that broader issues in service quality such as long waiting times, limited provider engagement and inconsistent service availability can further increase the likelihood of missed vaccinations by shaping where and how families seek care.





