New study: HPV and measles vaccines top vaccine impact list
Researchers compared 14 vaccine programmes across 117 countries to estimate how many deaths and illnesses they prevent per 1,000 vaccinations.
- 15 May 2026
- 4 min read
- by Linda Geddes

For decades, the public health message around vaccines has been relatively simple: vaccines save lives.
But as health budgets tighten and countries face a growing menu of vaccines to choose from, policymakers are increasingly confronting an uncomfortable decision: if countries cannot afford every vaccine programme, which ones should they prioritise?
The dilemma is becoming increasingly acute as Gavi, the Vaccine Alliance, and national governments weigh how to allocate limited funding across expanding immunisation programmes.
While the answer varies substantially depending on geography, disease burden and existing health systems, researchers have now attempted to compare 14 vaccines using the same yardstick: how many deaths or disability-adjusted life years (DALYs) they prevent per 1,000 persons vaccinated.
The researchers stressed that the estimates were intended to inform rather than replace other considerations such as cost-effectiveness, outbreak risk and equity.
They found that HPV and measles programmes delivered the highest overall health impact per person fully vaccinated, although for other vaccines the estimates often overlapped substantially and varied between regions and vaccination strategies.
The researchers stressed that the estimates were intended to inform rather than replace other considerations such as cost-effectiveness, outbreak risk and equity.
Taken together, these considerations could help countries compare vaccine programmes as they take on a greater role in deciding which vaccines to prioritise.
How much difference can vaccines make?
The Vaccine Impact Modelling Consortium (VIMC), an international network of scientists that models the health impact of vaccines, compared 14 Gavi-supported vaccine programmes across 117 low-and middle-income countries, estimating how many deaths or DALYs each prevented per 1,000 vaccinations delivered. DALYs represent years of healthy life saved because vaccines prevented early death, illness or disability.
Unlike previous VIMC analyses, which reported on the overall lives saved by vaccination programmes, the new study focused on comparing the relative impact of different vaccines as countries face increasingly difficult decisions about how to prioritise limited immunisation budgets. It also incorporates estimates for malaria and COVID-19 vaccine programmes for the first time.

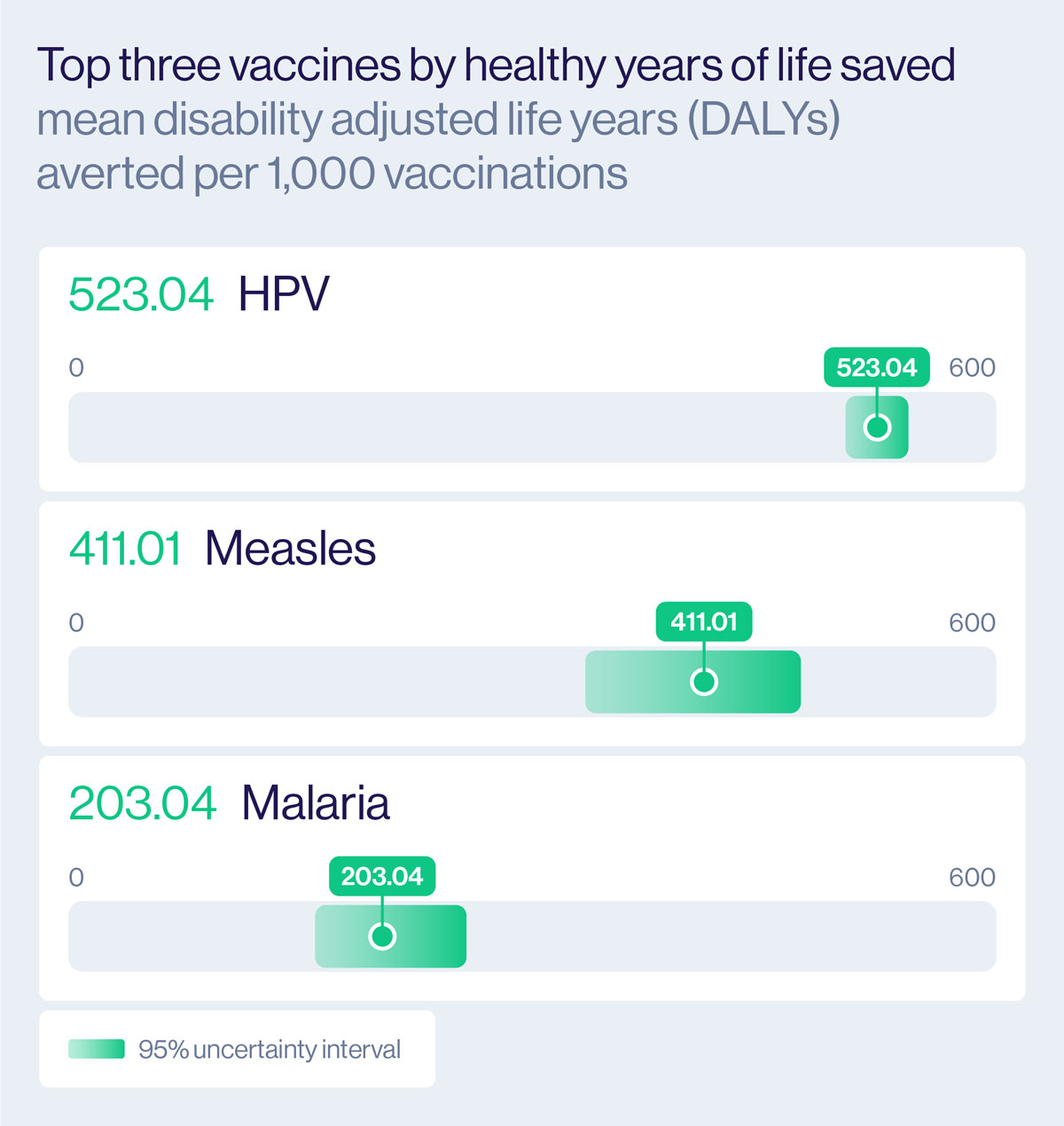
The research, published in The Lancet, found that human papillomavirus (HPV) and measles vaccines delivered the greatest impact on deaths and healthy years of life saved for every 1000 vaccinations given.
Globally, HPV vaccination prevented an estimated 11.2 deaths per 1,000 vaccinations, while measles prevented about 6.1. The two vaccines also ranked highest for disability-adjusted life years (DALYs) – a broader measure of disease burden that includes years lived with disability.
Hepatitis B ranked third for deaths averted, while malaria ranked third for DALYs averted.
Beyond those headline findings, however, the picture became more complex. The estimated impact of many vaccines varied substantially between regions and vaccination strategies, while uncertainty ranges frequently overlapped, meaning the results should not be interpreted as a simple league table of “best” and “worst” vaccines.
Globally, HPV vaccination prevented an estimated 11.2 deaths per 1,000 vaccinations, while measles prevented about 6.1. The two vaccines also ranked highest for disability-adjusted life years (DALYs) – a broader measure of disease burden that includes years lived with disability.
For example, cholera vaccines appeared to have a relatively modest impact globally, but the analysis examined only preventive vaccination campaigns rather than emergency outbreak responses.
The researchers also said their effectiveness could rise substantially when campaigns are geographically targeted towards high-burden or outbreak-prone areas.
Comparisons involving malaria vaccines were also more complicated, because malaria control depends heavily on interventions such as bed-nets and seasonal malaria chemoprevention alongside vaccination.
“There is a whole suite of established interventions that are being used and will have hugely influential effects on malaria vaccine impact,” said Dr Katy Gaythorpe of Imperial College London, who led the analysis on behalf of the consortium.
The COVID-19 findings similarly came with important caveats. COVID-19 vaccines ranked relatively low in the analysis compared with vaccines such as HPV and measles, but Gaythorpe cautioned against overinterpreting the comparison.
She noted that the study focused mainly on low- and middle-income countries and therefore did not capture much of the enormous early COVID-19 burden seen in wealthier nations.
COVID-19 vaccination programmes also differed substantially from many routine childhood immunisation campaigns because they targeted older age groups and evolved rapidly as the pandemic changed.
Some vaccines also showed markedly different impact ratios between regions, reflecting differences in disease burden, vaccination coverage and how programmes are delivered.
Have you read?
How could these vaccine impact estimates be used?
Rather than viewing the analysis as a league table, Gaythorpe said the estimates were intended to help countries weigh vaccine decisions alongside other considerations such as cost, equity and local disease burden.
The team deliberately presented uncertainty ranges alongside the estimates so that policymakers could see where differences between vaccines were meaningful, and where they were not, said Gaythorpe.
To support that process, the consortium has developed an interactive visualisation tool, to be released alongside the paper, allowing policymakers and researchers to explore vaccine impact estimates at global, regional and national levels.
Todi Mengistu, a Senior Programme Officer on the Measurement, Evaluation and Learning team at Gavi, the Vaccine Alliance, said the estimates were already being used to help guide some of the Alliance’s strategic investment decisions.
“Because the estimates cover the full portfolio of Gavi‑supported vaccines and are generated using a consistent approach across diseases, they can be used as one input into prioritisation decisions,” she said.









