In Kenya, the fight against cervical cancer gains ground at long last
Opportunities for the detection and treatment of the human papillomavirus-linked cancer are increasing, but vaccination – which can prevent the vast majority of cases – lags WHO targets.
- 21 March 2024
- 9 min read
- by Claudia Lacave

"When I first learned about my cancer diagnosis, I was utterly shocked. With no parents, no job, and two children to care for, the stress was overwhelming. At times, I found myself pleading with God to end my suffering," recounts Philis Mastili, 43, seated on her friend's makeshift wooden pallet couch on the outskirts of Nairobi one balmy January morning.
A cervical cancer diagnosis sounds like a death sentence to many in Kenya, though the cancer is among the most treatable. It's crucially also almost totally vaccine-preventable. The fourth most common cancer among women worldwide, cervical cancer is the second most prevalent in Kenya, trailing only behind breast cancer. However, with 5,200 fatalities annually, it's the primary cause of cancer-related deaths in the country, claiming approximately nine Kenyan women's lives each day.
“I vividly remember a day when our doctor friend encountered a young woman with advanced cervical cancer. She scheduled her for an appointment the following year, nearly 18 months away, because at the time, we only had one national hospital for radiotherapy. What were the odds that the patient would still be alive by then?”
- Catherine Wachira, Women4Cancer
Africa, in particular, bears a significant burden, contributing 21% of global cervical cancer deaths in 2020, largely due to the prevalence of HIV, which compromises patients' immune systems, leaving them more vulnerable to the cancer-causing human papillomavirus (HPV).
Efforts to change those grim statistics are afoot. One new initiative, led by the World Health Organization (WHO) and the Swiss biotechnology company Roche, and launched at the end of 2023, is aiming to level up the detection, diagnosis and treatment of breast and cervical cancers in Kenya, Zimbabwe and Côte d'Ivoire over the next three years.
Living with cancer
In the cosy, green-walled living room, a thermos of milky tea and plate of boiled arrow roots on the table before her, Mastili recalls the beginning of her battle in June 2023.
"At times, I noticed symptoms like vaginal discharge, abdominal pain, unusual odours, and intimate itching." Two screenings at Nairobi's Kenyatta Hospital confirmed stage 1 cervical cancer. Typically, symptoms only surface much later, often at stages 3 or 4, leading to delayed screenings and significantly diminishing patients' survival prospects.
HPV is the world's most widespread sexually transmitted infection, affecting 80% of people worldwide at least once in their lives. Typically, the body naturally clears the infection, which can target the cervix, anus, vulva, vagina, penis, oropharynx, oral cavity and larynx. However, in some cases, the infection becomes persistent. "When you contract HPV, it takes 10 to 15 years to develop into cancer, but during this period, precancerous lesions may appear. That's why, if identified and treated early, patients can beat it," explains Emmah Kariuki, programme director of the Kenyan organisation, Women4Cancer.
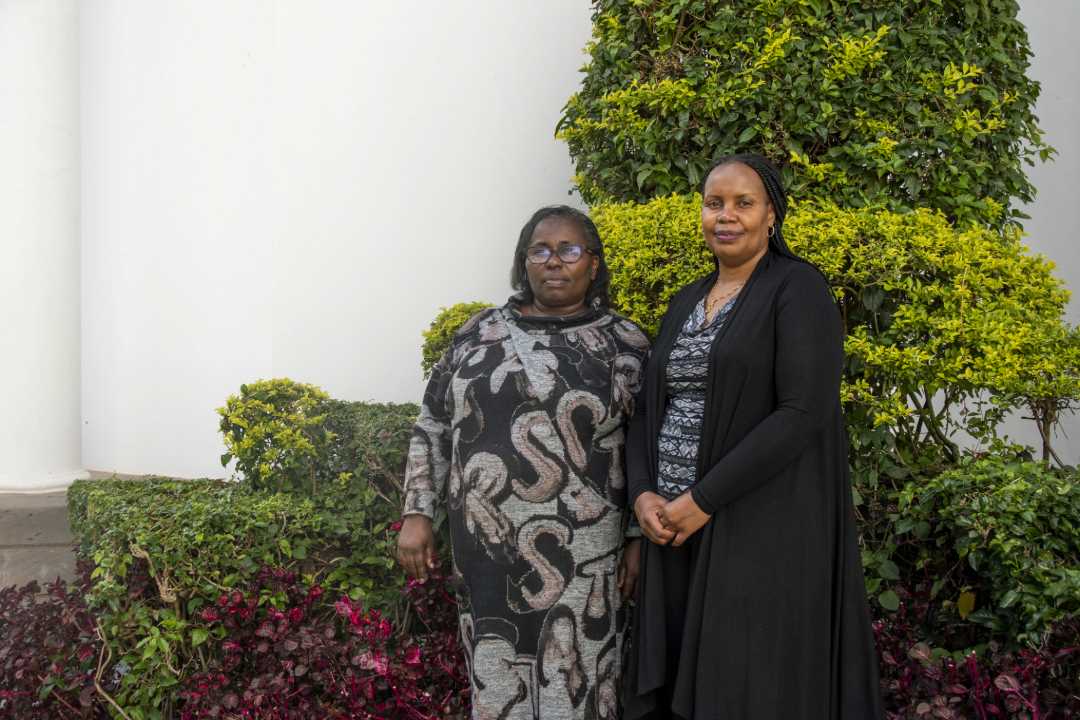
Credit: Claudia Lacave/Hans Lucas
Certain factors increase the risk of virus persistence, such as HIV infection, tobacco use, early onset of sexual activity, multiple sexual partners, long-term use of combined oral contraceptives (oestrogens and progestin), and multiple pregnancies.
Mastili's first response to her diagnosis was resignation. But after that, she says, she managed to turn things around with help from friends who had survived the disease.
Cryotherapy helped her eliminate lesions, and in September, she began an eight-month treatment regimen involving seven daily pills, along with monthly check-ups at the hospital. Her symptoms subsided. Without a job, and therefore lacking health insurance, she had to borrow money from a friend and sell her belongings to afford treatment.
Catherine Wachira, co-founder of Women4Cancer, says, "I'm pleased to say that in Kenya, public services are no longer as costly as they once were. We also have national screening guidelines, including methods like Visual Inspection with Acetic Acid (VIA), Pap tests, and DNA testing. There's talk of improved technology; things are evolving."
Despite initial delays, promising progress
It was during a weekly tea date with three friends that Wachira founded the organisation in 2012, driven by frustration with the status quo. "I vividly remember a day when our doctor friend encountered a young woman with advanced cervical cancer. She scheduled her for an appointment the following year, nearly 18 months away, because at the time, we only had one national hospital for radiotherapy. What were the odds that the patient would still be alive by then?" she says.
During a period when cervical cancer was still a scarcely addressed subject in the country, Wachira, Elizabeth Mbuthia, Dr Njoki Njirain, and Benda Kithaka launched a succession of awareness campaigns, and gradually expanded the organisation to meet evolving needs.
Today, Women4Cancer conducts screening events and supports patients through all stages of recovery, providing financial assistance. They collaborate with county governments to train health care professionals, and develop awareness materials and legislation with the Ministry of Health, all funded by private donations.
Have you read?
Kenya has had policies and clinical guidelines in place since 2009, but these have long remained ineffective. An assessment of the National Cancer Control Program (NCCP) in 2022 found that the majority of measures lacked implementation frameworks and monitoring, and screenings had "not yielded good results in Kenya."
The launch of the HPV vaccine in 2019, though late, triggered rapid progress. "After the 2012 pilot study, Kenya also had to build public trust before moving forward with implementation. Subsequently, agreements were made with Gavi to ensure a steady supply of doses for the coming years until we can take full control. It all took time," Wachira explains.
The COVID-19 pandemic put a temporary damper on this progress, but once the crisis eased, indicators quickly bounced back. The screening rate soared from 11% to 37.5% among women aged 25 to 49 between 2018–2019 and 2022–2023. Now, 59% of health centres offer the test, up from just 25% in 2018.
There are currently six public hospitals offering radiotherapy, with plans for five more facilities in the next five years. While the National Cancer Control Program (NCCP) has trained 7,000 health care workers and provided over 1,000 thermal ablation treatment devices, there is still plenty of room for improvement.
However, vaccination rates have decreased: in 2021, 29% of girls aged 10 to 14 received one dose, and 44% of these completed the second injection. By 2023, only 28% had received the first dose and 24% the second, falling short of WHO's target of 90% complete vaccination. WHO also recommends that 70% of women undergo screening, with 90% of positive cases receiving treatment.
What you don't know could kill you
In Kenya, less than 38% of those screened in 2022–2023 received treatment, highlighting one of the main challenges in battling the disease: the lack of follow-up.
"In the public system, it takes three to six weeks to get cytology results. That's a long time, because cervical cancer can progress during this period," remarks Kariuki, while Wachira adds, "If you tell someone to come back after six weeks, they probably won't, due to the cost and other factors."
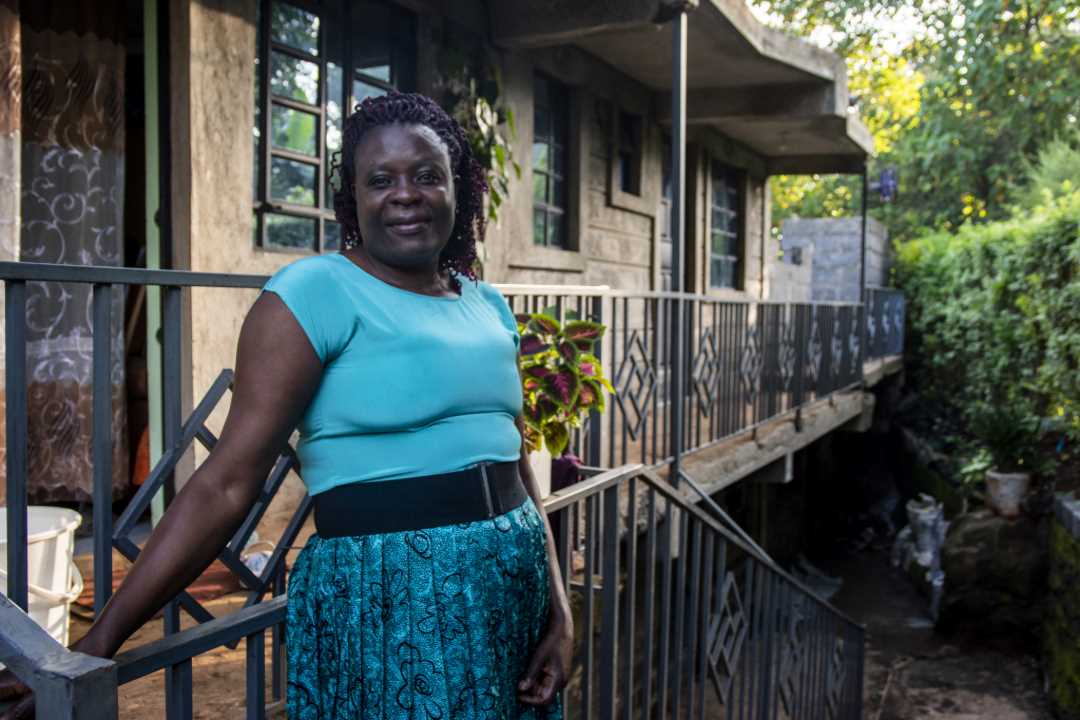
Credit: Claudia Lacave/Hans Lucas
Infrastructure trouble also means longer travel times to hospitals, and many women can't afford the transportation costs, let alone the cost of treatment. Screening and precise diagnostic exams aren't covered by public health insurance, although the public system does cover most treatments.
Pamela Savai, a cancer-survivor-turned-activist, often hears people say, “What you don’t know won’t kill you.”
She participated in a detection event organised by Women4Cancer during the first Kenyan cervical cancer awareness month in 2019. With the organisation's financial support, she completed all tests and underwent a hysterectomy – a surgery to remove the uterus – within two months. Because the screening saved her life, she decided to get involved with Kilele Health, an organisation that works to raise awareness about the cancer. Pamela participates in outdoorsy fundraising events for patients, like climbing Mount Kenya or Kilimanjaro.
Though public information campaigns are paying off in terms of greater public knowledge, prejudice persists. "There's a lot of stigma. When I fell ill, my relatives told me that I was a victim of witchcraft from my in-laws," said Savai.
Philis, too, encounters worrying reactions. "It can't happen to me," people tell her, or else: "Cancer is for rich people." "Let it kill me in silence," say some others.
Churches and vaccination for an STI
Engaging religious leaders who promote abstinence and fidelity within monogamous marriage presents a challenge when it comes to addressing sexually transmitted infections (STIs), including HPV. Initially, spiritual leaders resisted vaccination. Some practitioners, in alliance with the Kenya Catholic Doctors Association, claimed that the doses contained contraceptives, could affect women's fertility, or might encourage sexual activity among children. This resistance occurred amid a backdrop of widespread health misinformation during the COVID-19 pandemic.
However, with time, and after regular invitations to religious leaders to participate in awareness forums about cervical cancer, dissenting voices have begun to diminish. "They understand that the vaccine isn't about promoting abstinence today, but rather about safeguarding the future," explains Emmah Kariuki, programme director of the Kenyan organization Women4Cancer. The organisation is careful to separate the fight against the disease from its sexual causes to ensure broader acceptance of the message. Now, even churches occasionally invite survivors to share their stories and encourage screenings. Kariuki recalls a mission to a Muslim community in Kenya's north-east where, after being educated on the subject, a sheikh himself lectured on the risks and means of prevention of cervical cancer in his mosque.
Follow the writer on X : @C_Lacave









