In Kenya’s West Pokot, a new health centre is nothing short of a health revolution
Kanyarkwat locals in need used to cross the international border into Uganda for healthcare, because Kenyan health centres were even further away. The opening of a local hospital has changed everything.
- 1 May 2026
- 6 min read
- by Pius Sawa

It’s early on a Monday morning, and Nurse Mercyline Chebet is counting out vaccine vials and transferring them from a refrigerator into an insulated carrier box, and already mothers and their children are beginning to arrive.
“Monday and Thursday are market days,” Chebet explains. “We have dedicated those two days for measles-rubella and BCG vaccines, because the turnout is high.”
Just five metres from the Kanyarkwat Hospital’s front gate, an animal market is in full swing: goats, sheep, cows and chickens are bought and sold. Another 200 metres on, the sprawling open air market is noisy with traders hawking vegetables, cereals, household goods, secondhand clothes, electronics and many other things.

Credit: Pius Sawa
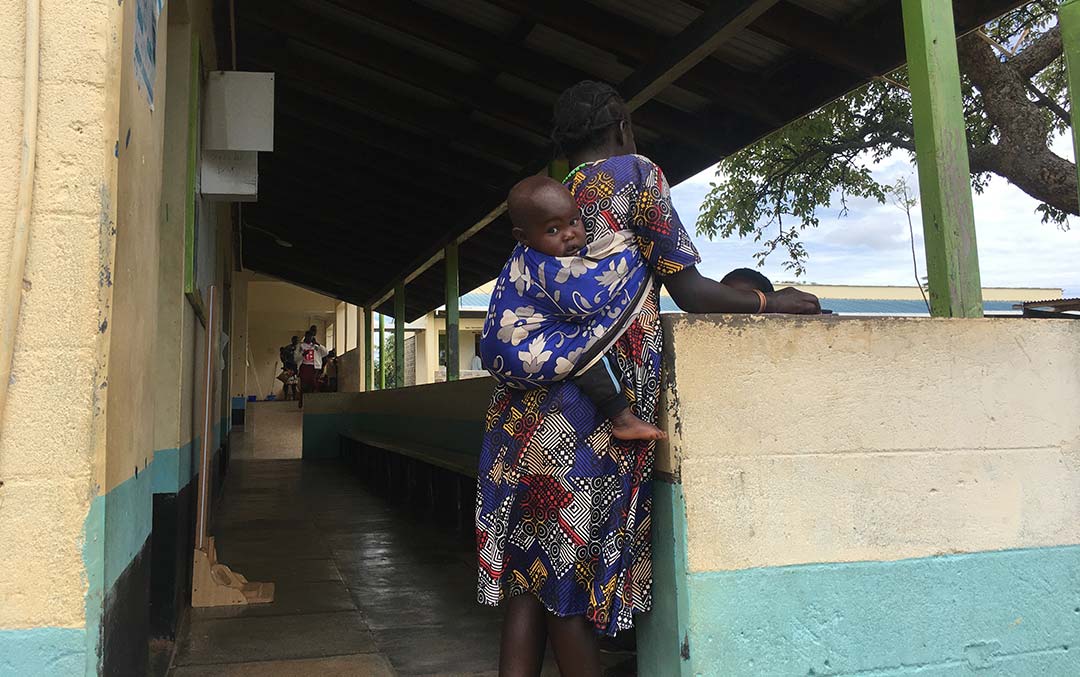
Parents like Cynthia Chebet, aged 20, who arrives on a motorbike with her six-month old baby, can bundle up their trips to market with a visit to the clinic. That equates to less vaccine wastage, nurse Chebet says, because some vaccines come in 20-dose vials, and any unused doses will be discarded at the end of the immunisation session.
Deadly distances
Until recently, the situation here was very different. West Pokot County has few health facilities, and as recently as 2023, local media reported that many Kanyarkwat residents were seeking healthcare in neighbouring Uganda. The great distances people in need were forced to travel in order to receive help, were leading to avoidable fatalities.
Jackline Nelima, a Community Health Promoter (CHP) at Kanyarkwat Hospital, said many mothers were not able to attend any antenatal clinics throughout their pregnancies. When complications started, they looked for motorbikes to rush to any available private clinic, but many died due to complications before reaching the Kapenguria Referral Hospital.
Have you read?
“ [Traditionally] Pokot women go through female genital mutilation, so some of them have very tiny holes for delivering. The baby cannot pass through, so we have to refer them quickly,” Nelima explained.
Traditional birth attendants were being used, but they lacked resources and skills to handle complications. Nelima said many children missed out on vaccination because they simply never connected with the formal health system.
A new hospital
When the government started constructing the new Kanyarkwat Health Centre, which was officially opened in early 2026, electricity was connected, and a refrigerator for storing vaccines was installed. The maternity room is equipped to be capable of handling both daytime and nighttime deliveries. There is clean running tap water, which is rare and vital in a semi-arid area where residents get water from seasonal rivers.

Credit: Pius Sawa
Enough health workers have been employed, and a new ambulance acquired for quick response in case of emergencies. Betty Cheptoo, a newly employed nurse, said the ambulance has responded to cases of mothers who develop precipitate labour, and children with respiratory distress syndrome.
“At times we get up to six deliveries a day, which to us is a very big number compared to years back when the health centre was still just a clinic with no facilities,” said Cheptoo.
The hospital has dedicated every Tuesday for Antenatal Care, while the rest of the days are for family planning and postnatal services. Cheptoo said since January 2026, only one premature delivery resulting in death has been registered.
Outreach
When nurses Chebet and Cheptoo aren’t administering jabs in the health centre’s brand new Immunisation Room, they are often out in the surrounding villages carrying vaccines in a portable cool box.
The health centre’s outreach programme helps include families for whom transport costs and long distance walking are prohibitive. “We have five outreaches: Sengwet, Cheparol, Karinger, Konchie and Katikomor”. Chebet says a single outreach session can record as many as 60 immunisations.
The Katikomor outreach is closest to the Ugandan border, and is held once every month, through support from Rotary Club based in Kacheliba. Action Against Hunger is also helping the team deliver services to other outreaches.
With predictable services made available to the five outreach centers, the Kanyarkwat Health Centre becomes a catchment point for markets day, the nearby communities, deliveries and emergency cases.
Community health promoters and TBAs
Nelima, who has been a CHP since 2014, explains that her major roles are making sure mothers attend antenatal clinics, deliver their babies in a health facility, and take their children for vaccination.
Credit: Pius Sawa
To do that, she often engages traditional birth attendants (TBAs). “We tell them to accompany the mothers to hospital, where we give them trainings on how to monitor the mothers and when to refer them to a hospital for delivery. We discourage any home deliveries under their supervision,” she said.
Nelima, meanwhile, checks immunisation booklets to make sure children in her zone have received all the necessary vaccines, and follows up on those who have defaulted. She says some of the mothers end up conceiving again while their last baby is still very young. This makes them fear to come to the clinic to attend ANC and vaccination.
The children born to one mother at very close intervals tend to be underweight and malnourished. She makes sure they get supplements from the health centre and advice on how to feed them.
Stumbling block
The arrival of Kanyarkwat Health Centre has clearly been a huge leap forward for locals – but there’s a hitch holding up further progress. Kanyarkwat catchment area struggles with exceedingly poor telecommunication signal. Residents struggle to make calls, with their phones referring them to Uganda’s MTN roaming options. That has made life more difficult for both health workers and the communities.
Nelima said she used to distribute treated mosquito nets to mothers in the villages. Because the government requires that all information should be captured on line using a smartphone, she would organise distribution sessions at specific spots where locals said the signal was better.
“We could ask the mothers to converge at this point so that we capture their data and enter them in the system.”
However, registering people in the Social Health Assurance (SHA) system is proving difficult, because registration must be done within the homes. “You can take a whole day trying to register one client, but you fail. Every time you try, it says system failure,” said Nelima.
Nurse Mercyline Chebet echoes the same sentiments. “Many of these mothers have not registered with SHA, while government says we shouldn’t offer services to people not registered with SHA. We are in dilemma. We call for a telecom booster in this area,” she told VaccinesWork.
Under SHA cover, every household is supposed to pay a monthly contribution to allow access to health services. Nelima, said most mothers depend on their husbands to register for SHA cover, but many are reluctant. “We are encouraging them to register using their own national ID cards because most of them have, instead of waiting for their husbands.”
Still, for Nelima, the stumbling blocks are dwarfed by the recent improvements – personally, as well as in terms of public health. “I had stayed for many years without pay, but now am happy that I am being paid,” she said.








