Q&A with Helen Rees
How the African Region is Celebrating the End of Wild Polio while cVDPV Outbreaks Continue
- 28 August 2020
- 6 min read
- by Global Polio Eradication Initiative (GPEI)
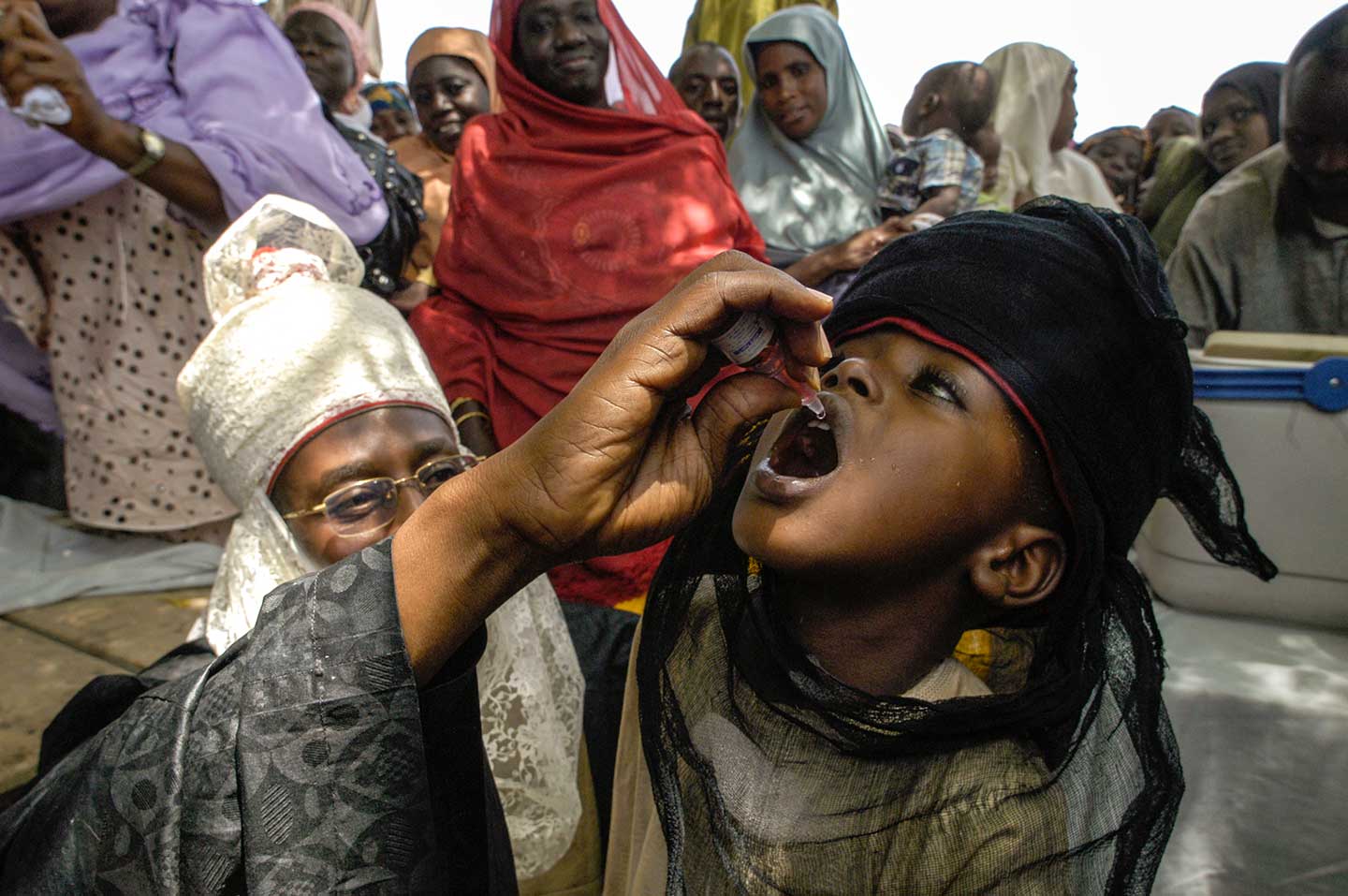
The WHO African Region is expected to be certified free of wild poliovirus on 25 August 2020. Chair of the WHO’s International Health Regulations Emergency Committee and of the AFRO Regional Immunization Technical Advisory Group Helen Rees explains the current cVDPV situation in Africa and its implications ahead of regional wild polio-free certification.
Q. Fifteen countries (as of 14 August 2020) in the World Health Organization’s African region have reported cases of circulating vaccine-derived polio type 2 (cVDPV2) in 2020. The total number of outbreak countries is 16. How does that impact the region’s upcoming wild polio-free certification?
First, it’s important to clarify that cVDPV is a different virus from the wild poliovirus, and will undergo a separate process to validate its absence once wild polio has been eradicated globally.
Second, I want to underscore that the ongoing cVDPV2 outbreaks in Africa do not affect the programme’s confidence that wild polio is gone from the region. Certification is backed by extensive data and a thorough evaluation process that demonstrates wild polio transmission has been interrupted on the continent.
In Africa, an independent body of experts called the African Regional Certification Commission for polio eradication (ARCC) oversees this process by carefully reviewing country documentation and analyzing the quality of surveillance systems and immunization coverage. With this intensive monitoring of polio programmes across the continent, the ARCC is able to confirm with 100% certainty that wild polio is gone from the region.
But for the ARCC, national polio programmes and GPEI partners, the work does not end here. Stopping cVDPVs remains an urgent priority. African countries will need to strengthen their efforts to reach all children with polio vaccines to protect them from cVDPVs and any importation of wild polio from the remaining endemic countries, Pakistan and Afghanistan.
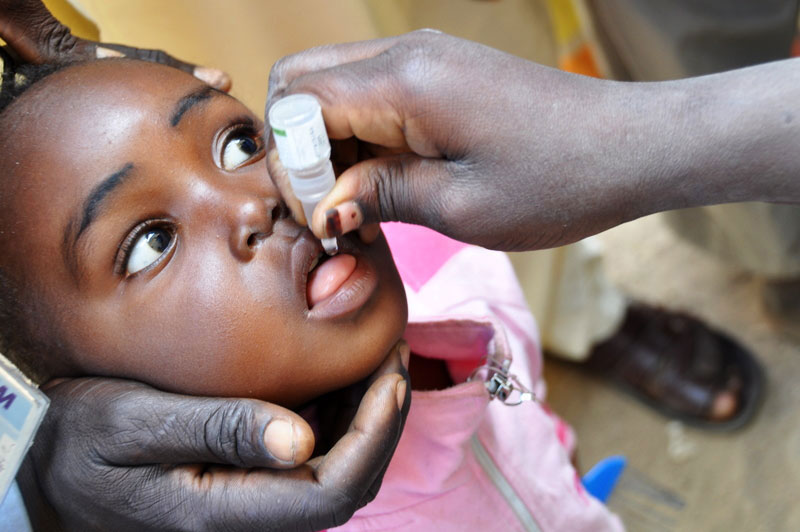
How do cVDPV outbreaks happen? And why has the number of cVDPV cases in Africa increased more rapidly in the past couple years while wild cases have not?
cVDPVs can occur if not enough children receive the polio vaccine. In under-immunized populations, the live weakened virus in the oral polio vaccine (OPV) can pass between individuals and, over time, change to a form that can cause paralysis—resulting in cVDPV cases. This means that the cVDPV outbreaks we’re seeing today are revealing pockets across the continent where immunization rates are too low.
The reason for the increase in cases can be explained by low immunity to type 2 poliovirus, which causes the vast majority of cVDPV cases. This is in part due to a global vaccine switch that occurred in 2016, when countries stopped using the trivalent OPV (which protects against all three forms of polio) and replaced it with the bivalent OPV (which protects against just type 1 and 3).
The GPEI, following the advice of the Strategic Advisory Group of Experts, decided to make this vaccine switch based on extensive evidence that showed it would decrease the number of cVDPV outbreaks. However, immunity to type 2 poliovirus was lower than predicated at the time of the switch and so there were actually more cVDPV2 outbreaks. In response to the cVDPV2 outbreaks monovalent oral polio vaccine type 2 (mOPV2) has been used to interrupt transmission. But with increasing numbers of children who do not have type 2 immunity, mOPV2 vaccines have had to be used longer and in larger quantities than was initially anticipated. This larger and more extensive use of mOPV2 vaccines has seeded new outbreaks especially in areas of low immunization coverage and on the borders of outbreak response zones.
All this said, mOPV2 is an effective tool to stop cVDPV outbreaks if children are properly immunized.
If cVDPV outbreaks can only affect under-immunized communities, doesn’t the increasing number of outbreaks indicate that polio immunity levels are too low across the region? Why were countries able to stop wild polio then?
For years, the wild poliovirus has only existed in a small area on the continent. Nigeria reported its last case of paralysis due to wild polio four years ago, but most other countries haven’t seen a wild polio case in quite some time.
Across the continent, population immunity levels to type 1 polio (the only type of wild polio that remains in the world) and surveillance networks have continued to protect against any wild polio importation from remaining wild polio endemic countries.
However, the increasing number of cVDPV outbreaks across Africa is a reminder that countries cannot afford to let their guard down, and must continue reaching every child with the polio vaccine.

What is the programme doing to address cVDPVs in Africa?
The same tactics that stop wild polio can be used to stop cVDPVs – high vaccination coverage and strong surveillance. The polio programme in Africa has proven experience and strategies to address cVDPV outbreaks. But we know that we cannot rely only on existing tactics, which is why the programme is innovating and adapting its strategies to address the challenge of cVDPVs specifically.
In early 2020, the GPEI released a comprehensive new strategy to stop cVDPV outbreaks currently affecting countries in Africa, Asia and the Middle East.
This includes revising outbreak response standard operating procedures to improve response time, doubling the size of the African Rapid Response Team, forming a global Rapid Response Team and prioritizing the GPEI’s ground presence in high-risk areas.
To raise immunization coverage, the GPEI partners – including Gavi, the Vaccine Alliance – are working to build and strengthen immunization systems in at-risk countries and expand routine immunization with the inactivated polio vaccine (IPV).
The strategy also includes the development of an additional tool to help stop cVDPV2 outbreaks – novel oral polio vaccine type 2 (nOPV2). nOPV2 is a modified version of the existing mOPV2 used to respond to cVDPV2 outbreaks that is less likely to change to a form that can cause paralysis.
The GPEI is confident that with strengthened commitment from country governments and full implementation of the tactics laid out in its strategy, cVDPVs can be wiped out across Africa.
Has COVID-19 affected the programme’s ability to stop cVDPV outbreaks in the region?
The recent pause in house-to-house polio campaigns to help control the spread of COVID-19 is expected to increase cVDPV transmission across affected countries.
The GPEI is taking a number of steps to get back on track. Even while campaigns were paused, surveillance activities continued so that as immunization activities ramp up the programme can target campaigns in areas that are most at risk.
The GPEI recently recommended that all countries with active polio transmission resume vaccination activities as soon as it is safe to do so, in line with WHO and national COVID-19 guidance. Burkina Faso and Angola were among the first countries to start implementing cVDPV outbreak response campaigns after the pause.
These campaigns are closely following safety guidelines and social distancing measures to protect communities and health workers against COVID-19. Measures including the use of masks and gloves, frequent handwashing and no-touch vaccination.
COVID-19 undoubtedly represents a setback for polio eradication, but not the first one the programme has faced. The GPEI and African countries’ national polio programmes are committed to ensuring that countries are ready to tackle the remaining challenge of cVDPVs and to recover lost ground once polio activities can safely ramp up.










